Evidence-Based Approach to Rehabilitation in Hip Osteoarthritis and Hip Fracture
Top Contributors - Ewa Jaraczewska, Jess Bell, Kim Jackson and Lucinda hampton
Introduction[edit | edit source]
Clinical practice guidelines are "systematically developed recommendations for patient care, which are based on scientific research, data or evidence, and are used to guide health care decisions for a defined clinical condition or under specific circumstances" (Segen's Medical Dictionary. 2011.).[1]
When using clinical practice guidelines to guide interventions, clinicians must understand that they are not fixed protocols that must be followed. They are only recommendations and not a replacement for clinical judgment.[2] Clinical practice guidelines establish a standard of care supported by scientific evidence, and their intention is for clinicians to consider the recommended intervention to enhance decision making.[3] These evidence-based tools are developed with a defined methodology and are based on a systematic review of the evidence.[2][4] Because clinical practice guidelines establish standards of care, they can assist clinicians with decision-making.[3]
The American Physical Therapy Association (APTA), which represents physical therapists, physical therapist assistants, and students of physical therapy in the United States, has published a systematic review of evidence in the form of the Clinical Practice Guidelines (CPGs).[5] CPGs are published by APTA sections and are provided to help clinicians choose treatment modalities to achieve the best outcomes.[2]
Quality of Evidence[edit | edit source]
The APTA uses six grades of recommendations based on the strength of the evidence. Each level represents the quality of evidence that supports a specific action:
- A or Strong: based on level I studies. Level I studies include a systematic review or meta-analysis of all relevant randomised controlled trials (RCTs) or evidence-based clinical practice guidelines based on systematic reviews of RCTs or 3 or more RCTs of good quality that have similar results.[6][7]
- B or Moderate: based on level II studies. Level II studies include at least one well-designed RCT.[6][7]
- C or Weak: based on a single-level II study or level III and IV studies. Level III studies are well-designed controlled trials without randomisation. Level IV evidence is from well-designed case-control or cohort studies.[6] [7]
- D or Conflicting evidence: Higher-quality studies conducted on this topic disagree with their conclusions. The recommendation is based on these conflicting studies.[8]
- E or Theoretical/foundational evidence: based on evidence from animal or cadaver studies, from conceptual models/principles, or basic sciences/bench research which support this conclusion.[8]
- F or Expert opinion: A best practice based on the clinical experience of the guideline development group.[8]
RCTs are the gold standard for research. The researcher allocates participants to experimental and placebo groups randomly, taking out any selection bias from the study. Selection bias may change results in a way that benefits a researcher or the body funding the study, damaging scientific integrity.[9]
Hip Osteoarthritis[edit | edit source]
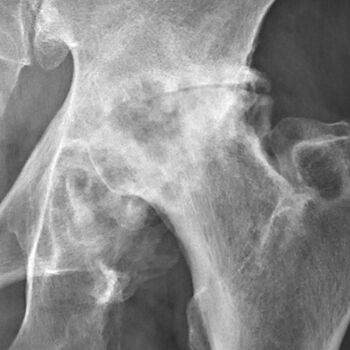
Hip osteoarthritis (OA) is a degenerative joint disease primarily affecting the articular cartilage and surrounding tissues.[10] Primary hip OA is of idiopathic origin whereas secondary hip OA originates from a joint articular surface disorder.[10]
Clinical Practice Guidelines for Hip Osteoarthritis[edit | edit source]
The following are hip osteoarthritis practice guidelines published by the APTA[11][12] and by various medical speciality groups, including:
- The American College of Rheumatology 2012 recommendations[13]
- EULAR evidence-based recommendations were developed by a group of 18 rheumatologists, 4 orthopaedic surgeons, and 1 epidemiologist, representing 14 European countries[14]
- Up-to-date review on hip osteoarthritis by orthopaedic surgeons, a rheumatologist and an immunologist from Cleveland Clinic and Boston Medical Center, USA[10]
Risk Factors[edit | edit source]
- Age: over 50 years[12] (Grade A)
- Sex: higher among men younger than age 50 years and women older than 50 years [10]
- Obesity:[10] every additional 10 pounds (4.5 kg) of body weight can exert an extra 60 pounds (27kg) of pressure upon the hip with each step[10][15]
- Genetics: having a relative who underwent total hip arthroplasty increases a person's risk of having the same procedure[10]
- Occupation: performing high-impact sports activities, repetitive stress and biomechanical overload (eg farmers)[10]
Clinical Presentation and Level of Evidence[edit | edit source]
The most common symptoms of hip osteoarthritis include:
- Anterior or lateral hip pain especially during weight-bearing, including walking, sit-to-stand transition, stair climbing[12](Grade A)
- Pain can be progressive or have a sudden onset[10]
- Morning stiffness[12] (Grade A), or stiffness developing after sitting or resting[10]
- Stiffness lasting for a few minutes, which decreases within 30 minutes[10]
- Limited hip internal rotation and hip extension[12] (Grade A)
- Pain with passive hip internal rotation[12] (Grade A)
- Difficulty putting shoes and socks on[12]
Examination[edit | edit source]
Physiotherapy Assessment[edit | edit source]
Diagnosis of hip osteoarthritis can be made based on clinical presentation. The objective examination should include:
- Lower extremities inspection
- Leg length discrepancy measurement
- Assessment of flexible and fixed hip joint deformity
- Bony prominence palpation for tenderness
- Passive and active range of motion assessment for flexion, extension, adduction, abduction, internal rotation, and external rotation[11][12]
- Neurovascular assessment
- FABER test (Grade A)[12]
Outcome Measures[edit | edit source]
The outcome measures in hip osteoarthritis have grade A evidence and may include:[11][12]
- Western Ontario WOMAC
- Brief Pain Inventory
- Pain Pressure Threshold
- Visual Analogue Scale
- Lower Extremity Functional Scale
- Harris Hip Score
Physical Performance Measures[edit | edit source]
Grade A evidence includes standardised balance tests: Berg Balance, a four-square step test and timed single-leg stance used to assess balance in patients with a long history of hip osteoarthritis and with a history of falls.[11][12]
Other types of Physical Performance Measures in hip osteoarthritis include:
- Six-minute walk test (6MWT)
- 30-second chair stand
- Timed up and go test (TUG)
- Self-paced walk
Physiotherapy Intervention[edit | edit source]
Patient Education[edit | edit source]
- Patient education (Grade B). Research suggests that patient education should include information on healthy weight loss, regular exercise, and activity modification.[11] [12] When discussing activity modification, environment modification must be considered, including, for example, the height of the chair or couch the patient gets up from.[11][12]
- Education reduces pain[14]
- Education on weight reduction have some benefit (Grade C)[14]
- Weight loss (strongly recommended)[13]
Physiotherapy Treatment[edit | edit source]
Physiotherapy provides great benefit during the early stages of hip osteoarthritis. However, little or no benefit was found from physiotherapy interventions during the later stages of hip osteoarthritis.[14] The following activities are recommended:
- Impairment-based functional training, gait training, and balance training (Grade C)[11][12]
- Balance exercises (conditional recommendations)[13]
- Individualised exercise prescription based on the individual's daily life participation and functional activity needs (Grade C)[11][12]
- Tai Chi (strong recommendations)[13]
- Manual therapy including thrust or non-thrust manipulation, and soft tissue releases, performed one to three times a week for over six to twelve weeks (Grade A)[11][12]
- Manual therapy with or without exercises (conditional recommendations against) [13]
- Massage therapy (conditional recommendations against)[13]
- Flexibility, strengthening, and endurance exercises (Grade A)[12] that do not involve high-impact activities.[10] It can include gentle yoga, cycling, or swimming.[10]
- Group-based therapy should be conducted one to five times a week for six to 12 weeks[12]
Modalities[edit | edit source]
- Ultrasound: One megahertz at one Watt per centimetre square for five minutes in all directions, 10 treatments performed for a period of two weeks (Grade B)[11][12]
- Acupuncture (conditional recommendations)[13]
- Thermal interventions (conditional recommendations)[13]
- Transcutaneous Electrical Nerve Stimulation (TENS) (strong recommendations against)[13]
Orthotics[edit | edit source]
- Use of a cane as needed (strong recommendations)[13]
- Lateral and medial wedged insoles (conditional recommendations against)[13]
Evidence-Based Approach to Rehabilitation After Hip Fracture[edit | edit source]
Examination[edit | edit source]
Physiotherapy Assessment[edit | edit source]
Outcome Measures[edit | edit source]
- McDonough et al.[8] recommend the following body functions, body structures, and activities be assessed and documented across all settings (acute and post-acute):
- Knee extension strength (Grade A).
- Verbal rating scale (VRS) for monitoring pain level (Grade A)
- Gait speed test when patients can ambulate without human assistance. Documentation should include comfortable or maximum speed and the use of walking aid (Grade A).
- Basic mobility assessment using the Cumulated Ambulation Score (CAS) (Grade A)
Physical Performance Measures/Patient-Reported Outcome Measures[edit | edit source]
- According to McDonough et al.,[8] the following tests and patient-reported outcome measures should be considered across all settings (acute and post-acute):
- Timed-Up-And-Go test (TUG)(Grade A)
- Short Physical Performance Battery (Grade C)
- New Mobility Score (Grade B)
- Falls Efficacy Scale-International (Grade B)
- A 3-level version of the EuroQol-5 dimensions scale (Grade C)
- The 10-item physical functioning scale of the Medical Outcomes Study 36-Item Short-Form Health Survey (SF-36) (Grade C)
Physiotherapy Intervention[edit | edit source]
- Based on the NICE guidelines[20] for the management of hip fracture in adults, patients should be mobilised on the day after surgery unless medically or surgically contraindicated. Mobilisation should continue at least once a day following regular physiotherapy review.[20]
- Ftouh et al.[21] and Handoll et al.[22] found that progressive resisted training after hip fractures showed a great amount of mobility improvement.[12] (High to Moderate evidence). However, Handoll et al.[22] concluded that there is not sufficient evidence from randomised trials to determine the best strategies for enhancing mobility after hip fracture surgery.[22] According to both authors, there is no evidence that specific treadmill training is better than a control on walking speed or pain.[12] (High Evidence).
- Treadmill training does not change the duration of hospital stay, speed, or pain in the patient.[12] (High evidence).
- Sylliaas et al.[23] proposed strength training including three sets of 15 repetitions of each exercise at 70% of the patient's 1-RM, increased to 80% of the 1-RM, with the number of repetitions reduced from 12 to 10 every third week while maintaining at least eight repetitions.[23] (Strong Evidence).
- There is no statistically significant evidence that ADL, gait and balance testing shows greater improvement after 3 months post-surgery with strength training versus motor training.[12]
- McDonough et al.[8] suggest that physiotherapists must provide structured exercise, based on progressive high-intensity resistive strength, balance, weight-bearing, and functional mobility training (Grade A). Patients with mild to moderate dementia should receive similar interventions and prescriptions as those without dementia (Grade B). During in-hospital care following surgery for a hip fracture, physiotherapy intervention should be high-frequency (daily), with duration as tolerated, and must include instruction in a home programme (Grade B). In the early post-acute phase, physiotherapy care should include upper-body aerobic training, progressive resistive training, balance, and mobility training (Grade C). [8]
- According to Karlsson et al.,[24] patients who are living at home and were admitted for hip surgery showed much better and improved outcomes when compared to the patients who were admitted from assisted living facilities or nursing facilities or dementia care.[12] Patients receiving Geriatric Interdisciplinary Home Rehabilitation showed an ability to ambulate that was similar to those receiving conventional geriatric care and rehabilitation.[24]
- Latham et al.[25] found that a home-based functionally oriented exercise programme led to improved physical functions within six to nine months[12] (Moderate Evidence).
- Diong et al.[26] recommend exercise programmes extending up to 12 months after surgery to obtain an improvement in some outcome measures: knee extension, balance, TUG, “fast” gait speed[12] (Moderate Recommendations).
- Auais et al.[27] suggest a community-based programme to achieve improvement in key areas due to better adherence to the programme[27] (Strong Evidence).
Modalities[edit | edit source]
- Dry needling was not found to be more effective in post-hip surgery recovery than functional movement and functional adaptation to the environment.[12] (Moderate to Low Evidence)
- McDonough et al.[8] recommend the use of electrical stimulation for quadriceps strengthening if other approaches fail (Grade C). In addition, physiotherapists may use electrical stimulation for pain if other strategies were not effective[8] (Grade C).
Discharge and Post-Hospital Care[edit | edit source]
- After reviewing discharge destination post-hip fracture, Ftouh et al.[21] recommend discharge from hospital to home. According to Ftouh et al., home-based care led to a significant increase in functional independence measures.[12] (Strong recommendations).
- Izzaguire et al.[28] concluded that specialised physiotherapy appears to be crucial in the first months after surgery, and becomes less important after four months post-surgery. A review of the literature supports the statement that there is no difference in the type of physiotherapy provided to help the patient achieve the ability to perform daily activities and independence after a hip fracture. [28] (Strong Evidence).
- Ftouh et al.[21] concluded that the first weeks after a hip fracture are critical for recovery.[21]
- McDonough et al.[8] stated that clinicians must provide additional therapies if strength, balance, and functional deficits remain beyond 8 to 16 weeks after fracture. The additional therapies should focus on strength, balance, functional training and gait training to address impairments, activity limitations and fall risk. These services can be provided in the outpatient settings, in the home, or as evidence-based community exercise programmes. (Grade A).
In Summary[edit | edit source]
Physiotherapists working with patients with hip osteoarthritis should consider the following interventions:
- Low impact strengthening, endurance and flexibility exercises
- Group-based therapy
- Tai-Chi
- Patient education
- Use of assistive device for ambulation when needed
Physiotherapy interventions for the treatment of hip fracture should include:
- Early mobilisation
- Progressive resistive training
- Strength training
- Community-based programme
- Home-based functionally oriented exercise programme
Resources[edit | edit source]
- Hip Osteoarthritis: Revision 2017. Clinical Practice Guidelines Linked to the International Classification of Functioning, Disability and Health From the Orthopaedic Section of the American Physical Therapy Association
- The management of hip fracture in adults . NICE.
- Physical Therapy Management of Older Adults With Hip Fracture. Clinical Practice Guidelines Linked to the International Classification of Functioning, Disability and Health From the Academy of Orthopaedic Physical Therapy and the Academy of Geriatric Physical Therapy of the American Physical Therapy Association.
References[edit | edit source]
- ↑ "Clinical practice guidelines." Segen's Medical Dictionary. 2011. Farlex, Inc. 7 Apr. 2022 https://medical-dictionary.thefreedictionary.com/clinical+practice+guidelines
- ↑ 2.0 2.1 2.2 Clinical Practice Guidelines. Available from: https://www.apta.org/patient-care/evidence-based-practice-resources/cpgs [last accessed 10.04.2022]
- ↑ 3.0 3.1 Institute of Medicine (US) Committee on Standards for Developing Trustworthy Clinical Practice Guidelines. Clinical Practice Guidelines We Can Trust. Graham R, Mancher M, Miller Wolman D, Greenfield S, Steinberg E, editors. Washington (DC): National Academies Press (US); 2011. PMID: 24983061.
- ↑ Franco JVA, Arancibia M, Meza N, Madrid E, Kopitowski K. Clinical practice guidelines: Concepts, limitations and challenges. Medwave. 2020 Apr 30;20(3):e7887. Spanish, English.
- ↑ American Physical Therapy Association. Available from: https://www.guidelinecentral.com/guidelines/APTA/# [last accessed 10.04.2022]
- ↑ 6.0 6.1 6.2 Shoemaker MJ, Dias KJ, Lefebvre KM, Heick JD, Collins SM. Physical Therapist Clinical Practice Guideline for the Management of Individuals With Heart Failure. Phys Ther. 2020 Jan 23;100(1):14-43.
- ↑ 7.0 7.1 7.2 Evidence-Based Practice: Levels of Evidence and Study Designs. Available from: https://ascension-wi.libguides.com/ebp/Levels_of_Evidence. Last Updated: Mar 30, 2022 [last accessed 08.04.2022].
- ↑ 8.0 8.1 8.2 8.3 8.4 8.5 8.6 8.7 8.8 8.9 McDonough CM, Harris-Hayes M, Kristensen MT, Overgaard JA, Herring TB, Kenny AM, Mangione KK. Physical Therapy Management of Older Adults With Hip Fracture. J Orthop Sports Phys Ther. 2021 Feb;51(2):CPG1-CPG81.
- ↑ Medical news today What is a RCT? Available:https://www.medicalnewstoday.com/articles/280574#takeaway (accessed 31.10.2022)
- ↑ 10.00 10.01 10.02 10.03 10.04 10.05 10.06 10.07 10.08 10.09 10.10 10.11 10.12 Lespasio MJ, Sultan AA, Piuzzi NS, Khlopas A, Husni ME, Muschler GF, Mont MA. Hip Osteoarthritis: A Primer. Perm J. 2018;22:17-084.
- ↑ 11.0 11.1 11.2 11.3 11.4 11.5 11.6 11.7 11.8 11.9 Cibulka MT, Bloom NJ, Enseki KR, Macdonald CW, Woehrle J, McDonough CM. Hip Pain and Mobility Deficits-Hip Osteoarthritis: Revision 2017. J Orthop Sports Phys Ther. 2017 Jun;47(6):A1-A37.
- ↑ 12.00 12.01 12.02 12.03 12.04 12.05 12.06 12.07 12.08 12.09 12.10 12.11 12.12 12.13 12.14 12.15 12.16 12.17 12.18 12.19 12.20 12.21 12.22 12.23 12.24 12.25 12.26 12.27 Pandya R. Understanding the hip: Rehabilitation Protocols and Treatment Strategies for the Hip. Part 1. Physiopedia Course. 2022
- ↑ 13.00 13.01 13.02 13.03 13.04 13.05 13.06 13.07 13.08 13.09 13.10 Kolasinski SL, Neogi T, Hochberg MC, Oatis C, Guyatt G, Block J, Callahan L, Copenhaver C, Dodge C, Felson D, Gellar K, Harvey WF, Hawker G, Herzig E, Kwoh CK, Nelson AE, Samuels J, Scanzello C, White D, Wise B, Altman RD, DiRenzo D, Fontanarosa J, Giradi G, Ishimori M, Misra D, Shah AA, Shmagel AK, Thoma LM, Turgunbaev M, Turner AS, Reston J. 2019 American College of Rheumatology/Arthritis Foundation Guideline for the Management of Osteoarthritis of the Hand, Hip, and Knee. Arthritis Care Res (Hoboken). 2020 Feb;72(2):149-162.
- ↑ 14.0 14.1 14.2 14.3 Zhang W, Doherty M, Arden N, Bannwarth B, Bijlsma J, Gunther KP, Hauselmann HJ, Herrero-Beaumont G, Jordan K, Kaklamanis P, Leeb B, Lequesne M, Lohmander S, Mazieres B, Martin-Mola E, Pavelka K, Pendleton A, Punzi L, Swoboda B, Varatojo R, Verbruggen G, Zimmermann-Gorska I, Dougados M; EULAR Standing Committee for International Clinical Studies Including Therapeutics (ESCISIT). EULAR evidence-based recommendations for the management of hip osteoarthritis: report of a task force of the EULAR Standing Committee for International Clinical Studies Including Therapeutics (ESCISIT). Ann Rheum Dis. 2005 May;64(5):669-81.
- ↑ Reyes C, Leyland KM, Peat G, Cooper C, Arden NK, Prieto-Alhambra D. Association Between Overweight and Obesity and Risk of Clinically Diagnosed Knee, Hip, and Hand Osteoarthritis: A Population-Based Cohort Study. Arthritis Rheumatol. 2016 Aug;68(8):1869-75.
- ↑ Versus Arthritis. Examination of the hip. Available from: https://www.youtube.com/watch?v=oaIVeMgnpmE [last accessed 14/04/2022]
- ↑ Mission Gait. 2-Minute Walk Test - Setup and Instruction. Available from: https://www.youtube.com/watch?v=qoa0yQBZFs4 [last accessed 14/04/2022]
- ↑ Community Partnership Videos. Short Form (SF-36). 2020. Available from: https://www.youtube.com/watch?v=rSfZ3V1_rbY [last accessed 14/04/2022]
- ↑ EuroQol Research Foundation. EQ-5D-5L Descriptive System.2021. Available from: https://www.youtube.com/watch?v=2plIc9gVs7M[last accessed 14/04/2022]
- ↑ 20.0 20.1 The management of hip fracture in adults. Available from:https://www.nice.org.uk/guidance/cg124/evidence/full-guideline-pdf-183081997. Published: 22 June 2011. Last updated: 10 May 2017 [last accessed 11.04.2022]
- ↑ 21.0 21.1 21.2 21.3 Ftouh S, Morga A, Swift C; Guideline Development Group. Management of hip fracture in adults: summary of NICE guidance. BMJ. 2011 Jun 21;342:d3304.
- ↑ 22.0 22.1 22.2 Handoll HH, Sherrington C, Mak JC. Interventions for improving mobility after hip fracture surgery in adults. Cochrane Database Syst Rev. 2011 Mar 16;(3):CD001704.
- ↑ 23.0 23.1 Sylliaas H, Brovold T, Wyller TB, Bergland A. Progressive strength training in older patients after hip fracture: a randomised controlled trial. Age and Ageing 2011; 40(2)2: 221–227.
- ↑ 24.0 24.1 Karlsson Å, Berggren M, Gustafson Y, Olofsson B, Lindelöf N, Stenvall M. Effects of Geriatric Interdisciplinary Home Rehabilitation on Walking Ability and Length of Hospital Stay After Hip Fracture: A Randomized Controlled Trial. J Am Med Dir Assoc. 2016 May 1;17(5):464.e9-464.e15.
- ↑ Latham NK, Harris BA, Bean JF, Heeren T, Goodyear C, Zawacki S, Heislein DM, Mustafa J, Pardasaney P, Giorgetti M, Holt N, Goehring L, Jette AM. Effect of a home-based exercise program on functional recovery following rehabilitation after hip fracture: a randomized clinical trial. JAMA. 2014 Feb 19;311(7):700-8.
- ↑ Diong J, Allen N, Sherrington C. Structured exercise improve mobility after hip fracture: a meta-analysis with meta-regression. Br J Sports Med. 2016 Mar;50(6):346-55.
- ↑ 27.0 27.1 Auais MA, Eilayyan O, Mayo NE. Extended exercise rehabilitation after hip fracture improves patients' physical function: a systematic review and meta-analysis. Phys Ther. 2012 Nov;92(11):1437-51.
- ↑ 28.0 28.1 Izaguirre A, Delgado I, Mateo-Troncoso C, Sánchez-Nuncio HR, Sánchez-Márquez W, Luque-Ramos A. Rehabilitación de las fracturas de cadera. Revisión sistemática [Rehabilitation of hip fractures. Systematic review]. Acta Ortop Mex. 2018 Jan-Feb;32(1):28-35. Spanish.