Demyelinating Disorders
Original Editor - Lucinda hampton
Top Contributors - Lucinda hampton and Kim Jackson
Introduction[edit | edit source]
The spectrum of “demyelinating disorders” is broad and it includes various disorders with central nervous system (CNS) demyelination, eg multiple sclerosis (MS), Neuromyelitis optica spectrum disorders (NMOSD), Chronic Inflammatory Demyelinating Polyneuropathy (CIDP).[1]
The term demyelination refers to loss of the myelin sheath that surrounds and protects axons in the nervous system. Demyelination occurs as the result of diseases that damage the myelin sheath or the cells that form it. Diseases that are characterized by this loss of myelin are referred to as demyelinating diseases[2].
- Myelin sheaths cover many nerve fibers in the central and peripheral nervous system; they accelerate axonal transmission of neural impulses. Disorders that affect myelin interrupt nerve transmission; symptoms may reflect deficits in any part of the nervous system.
- MS is the most common demyelinating condition. According to the National MS Society, it affects 2.3 million people worldwide.
- Myelin formed by oligodendroglia in the central nervous system (CNS) differs chemically and immunologically from that formed by Schwann cells peripherally. Thus, some myelin disorders (eg, Guillain-Barré syndrome, chronic inflammatory demyelinating polyneuropathy, some other peripheral nerve polyneuropathies) tend to affect primarily the peripheral nerves, and others affect primarily the CNS. The most commonly affected areas in the CNS are the brain, spinal cord, and optic nerves.
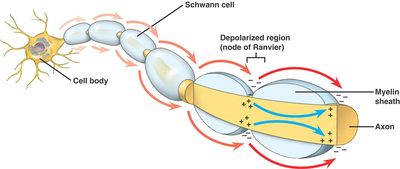
Image 1: Action potential propargation along a myelinated nerve.
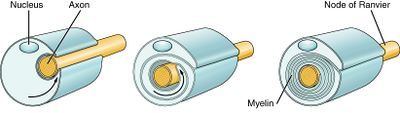
Image 2: Peripheral nerve myelination
Etiology[edit | edit source]
Image 3: Guillain–Barré syndrome (GBS) is a rapid-onset muscle weakness as a result of damage to the peripheral nervous system.
Inflammation is the most common cause of myelin damage. Inflammatory demyelination
- This category includes: multiple sclerosis, Guillain-Barre syndrome, acute‐disseminated encephalomyelitis (ADEM) and acute haemorrhagic leucoencephalitis (AHL). The commonest of these is multiple sclerosis.
- Primary demyelinating disorders may develop after a viral infection or vaccination against a viral infection. A likely explanation is that the virus or another substance somehow triggers the immune system to attack the body’s own tissues (autoimmune reaction). The autoimmune reaction results in inflammation, which damages the myelin sheath and the neurone under it[2].
Other causes include:
Viral demyelination
- The principal viral demyelinating disease in humans is progressive multifocal leucoencephalopathy (PML) caused by the papovavirus, JC virus. Approximately 50% of adolescents and 75% of adults have serological evidence of JC virus infection, but it is usually asymptomatic. The virus establishes latent infection in B cells, kidney and possibly CNS. Reactivation occurs under conditions of impaired cell‐mediated immunity eg after organ transplantation, in patients with leukaemia or lymphoma or in those with AIDS.
- HIV infection and the measles virus (can cause Subacute sclerosing panencephalitis) may cause forms of demyelination disorders.
Acquired metabolic demyelination
- The most common diseases in this category are central pontine myelinolysis (CPM) and extrapontine myelinolysis (EPM). Very rarely, demyelination occurs in association with chronic alcoholism and malnourishment (Marchiafava–Bignami disease).
Hereditary Diseases
- Myelin sheaths do not develop normally in children with certain rare hereditary diseases, eg Tay-Sachs disease, Niemann-Pick disease, Gaucher disease, and Hurler syndrome. These children may have permanent, often extensive, neurologic problems[2].
Hypoxic–ischaemic forms of demyelination
Demyelination caused by focal compression[3]
Clinical Presentation[edit | edit source]
Demyelination should be considered in any patient with unexplained neurologic deficits. Primary demyelinating disorders are suggested by the following:
- Diffuse or multifocal deficits
- Sudden or subacute onset, particularly in young adults
- Onset within weeks of an infection or vaccination
- Deficits that wax and wane
- Symptoms suggesting a specific demyelinating disorder (eg, unexplained optic neuritis or internuclear ophthalmoplegia suggesting multiple sclerosis)
- Specific tests and treatment depend on the specific disorder[2].
Image 4: Monthly multiple sclerosis animation
Treatment[edit | edit source]
No cures exist for demyelinating diseases and their progression, and symptoms are different for everyone. Getting treatment early is important. Treatment focuses on:
- Minimizing the effects of the attacks
- Modifying the course of the disease
- Managing the symptoms
A variety of drug therapies are recommended depending on the specific disorder. Strategies to treat symptoms include physical therapy, muscle relaxing drugs, and medications to reduce pain and fatigue[4].
Physiotherapy may include exercise to help build stamina and keep muscles strong. Over time, client may need braces and splints for weak joints. Each condition has specific needs and a look at the links above to particular condition will guide you in your physiotherapy.
References[edit | edit source]
- ↑ Bernitsas E. Pathophysiology and Imaging Diagnosis of Demyelinating Disorders.2018 Available from:https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5870362/ (last accessed 7.1.2021)
- ↑ 2.0 2.1 2.2 2.3 MSD manual Demyelinating Disorders Available from: https://www.msdmanuals.com/en-au/professional/neurologic-disorders/demyelinating-disorders/overview-of-demyelinating-disorders (accessed 7.1.2021)
- ↑ Love S. Demyelinating diseases. Journal of clinical pathology. 2006 Nov 1;59(11):1151-9.Available from:https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1860500/ Accessed 7.1.2021)
- ↑ Mayo CLINIC DEMYELINATING DISORDERS Available from: https://www.mayoclinic.org/diseases-conditions/multiple-sclerosis/expert-answers/demyelinating-disease/faq-20058521(accessed 7.1.2021)