Cartilage
Top Contributors - Esraa Mohamed Abdullzaher, Lucinda hampton, Kim Jackson, George Prudden, Joao Costa and Sai Kripa
Introduction[edit | edit source]
Cartilage is a non-vascular type of supporting connective tissue that is found throughout the body .
- Cartilage is a flexible connective tissue that differs from bone in several ways; it is avascular and its microarchitecture is less organized than bone.
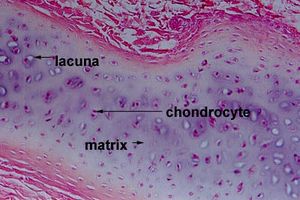
- The cells (chondrocytes) are scattered and lie firmly fixed in matrix supported by collagen and elastic fibres.
- Cartilage is not innervated and therefore relies on diffusion to obtain nutrients. This causes it to heal very slowly.
- The main cell types in cartilage are chondrocytes, the ground substance is chondroitin sulfate, and the fibrous sheath is called perichondrium.
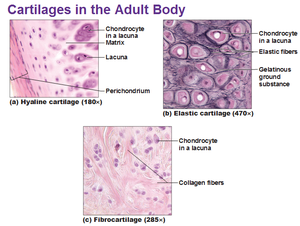
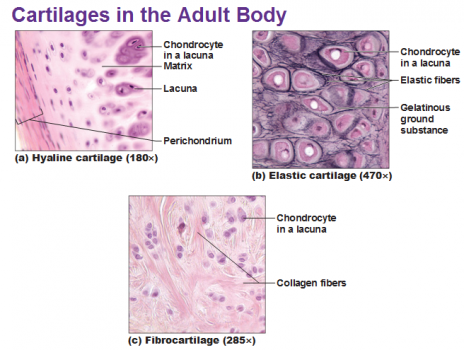
There are three types of cartilage: hyaline, fibrous, and elastic cartilage.
- Hyaline cartilage is the most widespread type and resembles glass. In the embryo, bone begins as hyaline cartilage and later ossifies.
- Fibrous cartilage has many collagen fibers and is found in the intervertebral discs and pubic symphysis.
- Elastic cartilage is springy, yellow, and elastic and is found in the internal support of the external ear and in the epiglottis[1]
Cartilage Structure [edit | edit source]
Cartilage is a dense structure, that resembles a firm gel, made up of collagen and elastic fibres. It contains polysacchride derivaites called chondroitin sulfates which complex with protein in the ground substance forming proteoglycan. The matrix is produced by cells call chrondroblasts which form chrondocytes and can be found in small chambers called lacuna
Cartilage is separated from the surrounding tissues by perichondrium which consist of two layers:
- Outer Fibrous Layer : Which provide protection , mechanical support and attaches the cartilage to other structures.
- Inner Cellular : It Is Important in the growth and maintenance of cartilage .[3]
Types of Cartilage[edit | edit source]
There are three types of cartilage and they all have slightly different structures and function
Hyaline Cartilage[edit | edit source]
Hyaline Cartilage has a smooth surface and is the most common of the three types of cartilage. It has a matrix that contains closely packed collagen fibers, making it tough but slightly flexible. It consists of a bluish-white, shiny ground elastic material, whose matrix contains chondtoitin sulphate, with many fine collagen fibrils and chrondrocytes. The chondrocytes are arranged in small groups within cell nests and the matrix is solid and smooth. Because of its smooth surfaces it allows tissues to slide/glide more easily, as well as providing flexibility and support.
Example : Connection between ribs and sternum, nasal cartilage and articular cartilage (which covers opposing bone surfaces in many joints).
Fibrocartilage[edit | edit source]
Fibrocartilage is the toughest of the three types of cartilage. This consists of dense masses of white collagen fibres in a matrix similar to that of hyaline cartilage with the cells widely dispersed. It has no perichondrium and has a matrix that contains dense bundles of collagen fibers embedded with chrondrocytes, making it durable and tough. This makes it perfect to provide support and rigidity
Example : Intervertebral discs (between spinal vertebrae), Menisci (cartilage pads of the knee joint), the callus (formed at the ends of bones at the site of a fracture), between the Pubic Symphysis and at the junction where tendons insert into bone.
Elastic Cartilage[edit | edit source]
Elastic cartilage provides support. It has a yellowish colour and is surrounded by a perichnodrium. Chrondrocytes are located between a network of threadlike elastic fibres, the abundance of elastic fibres makes it flexible and resilient. It provides support and maintains shape of, e.g. the pinna or lobe of the ear, the epiglottis and blood vessel walls.
- Example : the auricle of the outer ear . [3]
Embryology[edit | edit source]
- Cartilage is formed from the mesoderm germ layer by the process known as chondrogenesis.
- Mesenchyme differentiates into chondroblasts which are the cells that secrete the major components of the extracellular matrix. The most important of these components for cartilage formation being aggrecan and type II collagen.
- Once initial chondrification occurs, the immature cartilage grows mainly by developing into a more mature state since it cannot grow by mitosis.
- There is minimal cell division in cartilage; therefore, the size and mass of cartilage do not change significantly after initially chondrification. The growth of cartilage is a slow process and occurs by the division of cells.[4]
Remodelling of Cartilage[edit | edit source]
- This occurs predominantly by changes and the rearrangement of the collagen matrix in response to load.
- Watch the 1 minute video below.
Mechanical Behaviour of Articular Cartilage[edit | edit source]
The mechanical behaviour depend on interaction of its component : proteoglycan, collagen and interstitial fluid. In an aqueous environment , proteogylcans are polyanionic which means the molecule has negatively charged sites that arise from sulfate and carboxyl. In solution, the mutual repulsion of these negative charges causes the aggregated proteogylcan to spread out and occupy a large volume .
In the cartilage matrix, the volume occupied by proteogylcan aggregates is limited by the network of collagen fibres. when the cartilage is commpressed the negatively charged sites are pushed together increasing the mutual repulsion force adding to the compressive stiffness of the cartilage. During this process non-aggregated protoegylcans are not affected by the compressive load since they are not easily trapped in the cartilage matrix .Damage to the collagen framework reduces compressive stiffness .
The mechanical response of the cartilage is strongly tied to the application of pressure differences and the flow of fluid through the tissue as, when deformed, the fluid flows across the cartilage and articular surface .
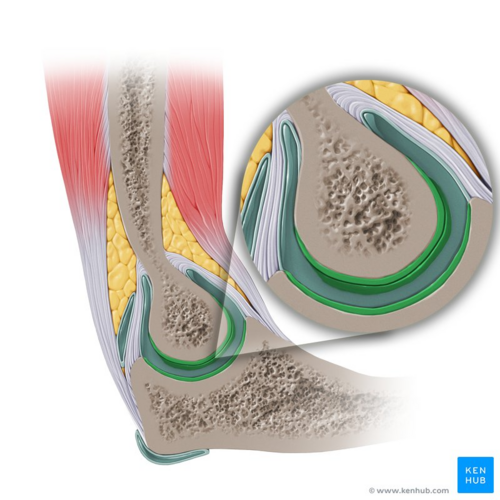
Image: Articular cartilage of the elbow (highlighted in green) - sagittal view [6]
Biphasic Model of Cartilage[edit | edit source]
All of the solid components of the cartilage (lipid, proteogylcans,cells and collagen ) are grouped together to form the solid component of the matrix and the interstitial fluid, that moves freely, forms the fluid component.
Blood Supply and Lymphatics[edit | edit source]
Cartilage is avascular. Since there is no direct blood supply, chondrocytes receive nourishment via diffusion from the surrounding environment. The compressive forces that regularly act on cartilage also increase the diffusion of nutrients. This indirect process of receiving nutrients is a major factor in the slow turnover of the extracellular matrix and lack of repair seen in cartilage.[4]
Nerves[edit | edit source]
Cartilage does not contain nerves; it is a aneural The pain, if any, associated with pathology involving cartilage is most commonly due to irritation of surrounding structures, for example, inflammation of the joint and bone in osteoarthritis.[4]
Muscles[edit | edit source]
Fibrocartilage is a major component of entheses, which is the connective tissue between muscle, tendon or ligament and bone. The fibrocartilaginous enthesis consists of 4 transition zones as it progresses from tendon to bone.
- Longitudinal fibroblasts and a parallel arrangement of collagen fibers are found at the tendinous area
- A fibrocartilaginous region where the main type of cells present transitions from fibroblast to chondrocytes
- A region called the "blue line" or "tide mark" due to an abrupt transition from cartilaginous to calcified fibrocartilage
- Bone[4]
Clinical Significance[edit | edit source]
Many pathology exists involving cartilage, for example, osteoarthritis, spinal disc herniation, traumatic rupture/detachment, achondroplasia, costochondritis, neoplasm, and many others. These result from a variety of degenerative, inflammatory, and congenital causes.
Exercise and Cartilage Health:
- Participation in certain sports appear to increase risk of osteoarthritis resulting from breakdown of joint cartilage. Activities that involve torsional loading , fast acceleration and deceleration , repetitive high impact and high level of participation increase risk of osteoarthritis. Increased risks of osteoarthritis are related to excessive exercise or abnormal joint loading
- Some levels of loading and exercise are beneficial for joint health as exercise enhances production of matrix molecules, which can have a positive effect on joint health.[7]
Current Thinking on Articular Repair and Regeneration[edit | edit source]
A biological approach to cartilage damage is challenging due to its' inherent limited healing potential. Various options have been made available over the years trying to address these issues. New technique have merits and demerits. Stem cells therapy is a strong promise in the treatment of cartilage defects and osteoarthritis.
Stem cells(SC), in particular mesenchymal SCs, are expected to revolutionise the treatment for cartilage defects and osteoarthritis in the near future. It is hoped that the whole cartilage can be repaired not just focal defects.[8]
The below video (4 minutes) delves into the regeneration aspirations
References[edit | edit source]
- ↑ Lumen learning Cartilage Available from:https://courses.lumenlearning.com/boundless-ap/chapter/cartilage/ (last accessed 10.2.2020)
- ↑ https://www.youtube.com/watch?v=mr5JI8Q8dc8
- ↑ 3.0 3.1 Fredric H.Martini ,Judi Nath ,Edwen Bartholomew , Charles M.Seiger ,Damian Hill . Fundamentals of Anatomy and Physiology .9th ed , 2011 .
- ↑ 4.0 4.1 4.2 4.3 Chang IR, Martin A. Anatomy, Cartilage. InStatPearls [Internet] 2018 Dec 13. StatPearls Publishing. Available from:https://www.ncbi.nlm.nih.gov/books/NBK532964/ (last accessed 11.2.2020)
- ↑ https://www.youtube.com/watch?v=tS5S8BoVN-4
- ↑ Articular cartilage of the elbow image - © Kenhub https://www.kenhub.com/en/library/anatomy/cartilage
- ↑ 7.0 7.1 Carol A.Oatis . kinesiology the mechanics and pathomechanics of human movement , 2003 .
- ↑ Karuppal R. Current concepts in the articular cartilage repair and regeneration. J Orthop. 2017;14(2):A1–A3. Published 2017 May 19. doi:10.1016/j.jor.2017.05.001 Available from:https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5440635/ (last accessed 31.5.2019)
- ↑ Sportology Cartilage repair basics Available from: https://www.youtube.com/watch?v=CxhFhidWn6w (last accessed 31.5.2019)