Breast Feeding and Physiotherapy
Original Editor - User Name
Top Contributors - Manisha Shrestha, Rosie Swift, Kim Jackson, Uchechukwu Chukwuemeka, Muskan Rastogi and Carina Therese Magtibay
Introduction[edit | edit source]
Breastfeeding is one of the most effective ways to ensure child health and survival.[1] Breast feeding is linked to decreased mortality and morbidity of infants in developing countries. Other benefits of breast feeding include reduced risk of the child developing obesity or diabetes in later life; and reduced risk of breast and ovarian cancers in women who have breast fed.[1]
Despite many the benefits of breast feeding in both mother and baby, nearly 2 out of 3 infants are not exclusively breastfed for the recommended 6 months—a rate that has not improved in 2 decades.[1] A lack of awareness about breast feeding in mothers and her family, hinder true informed decision making with regards to whether or not to breastfeed. Other issues that lead to decisions to discontinue breastfeeding include challenges with infant positioning and attachment during breastfeeding.[2][3]
Exclusive Breast Feeding[edit | edit source]
According to the World Health Organization (WHO), Exclusive breastfeeding (EBF) is the situation in which an infant receives only breast milk from his/her mother or a wet nurse for the first 6 months and no other solids or liquids with the exception of drops or syrups consisting of vitamins, minerals, supplements, or medicines.[4]
Globally, about 40% of infants were exclusively breastfed and this is expected to rise to 50% by 2025. Worldwide, only 39% of newborns were put to the breast within 1 h of birth, and only 37% of infants were exclusively breastfed. The prevalence of EBP is less in developing countries with 20% Sub-Saharan Africa, 41% in North Africa, 44% in Asia, and 30% in the Latin America.[4]
EBF is an important public health strategy for improving children’s and mother’s health by reducing child morbidity and mortality and helping to control healthcare costs in society.[5] The 2001 WHO EBF-6 recommendation was based on evidence gathered from a systematic review comparing EBF for 6 months to EBF for 3-4 months with continued BF for at least 6 months, examining the impact of these practices on child health, growth, and development, as well as on maternal health. [6]
There were concerns that EBP could result in iron deficiency, other micronutrient deficiencies and growth faltering in susceptible infants. These concerns were directed particularly at populations where maternal nutrition was poor. [7] The risk for iron deficiency in the first 6 months of life can be successfully mitigated by delayed umbilical-cord clamping.[6]
By the age of 6 months, a baby has usually at least doubled his or her birth weight, and is becoming more active. Exclusive breastfeeding is no longer sufficient to meet all energy and nutrient needs by itself, and complementary foods should be introduced to make up the difference. At about 6 months of age, an infant is also developmentally ready for other foods. The digestive system is mature enough to digest the starch, protein and fat in a non-milk diet. Very young infants push foods out with their tongue, but by between 6 and 9 months infants can receive and hold semi-solid food in their mouths more easily. Breastfeeding should continue with complementary feeding up to 2 years of age or beyond, and it should be on demand, as often as the child wants.[8]
Benefits of Breast Feeding[edit | edit source]
The benefits of breastfeeding in baby:
- Strong mother-child relationship,
- Lowers the incidence of many childhood illnesses, such as gastrointestinal infections, middle ear infections, pneumonia, sudden infant death syndrome, diabetes mellitus, malocclusion, and diarrhoea[5]
- Lower malnutrition[4]
- Reduced risk of child being overweight and obesity[1]
- Supports healthy brain development and is associated with higher performance on intelligence tests among children and adolescents[5]
The benefits of breast feeding in mother:
- Decreased frequency of haemorrhage (postpartum haemorrhage), postpartum depression, breast cancer, ovarian and endometrial cancer
- Facilitates weight loss
- The lactation amenorrhea method is an important choice for postpartum family planning [5], provided that certain criteria are met to ensure adequate protection (amenorrhea; fully breastfeeding - no interval of >4–6 hours between breastfeeds; <6 months postpartum)[9]
The benefits of breast feeding in family and society:
- Reduced expenses (formula milk and later treatment cost, if not breastfed)
- Promotes sustainability of environment, due to decreased waste[10]
- Reduced economic burden of the country for milk substitutes
Breast Milk[edit | edit source]
Breastmilk is the ideal food for infants as it is easily digested and efficiently used.. It is a live substance with unparalleled immunological and anti-inflammatory properties that protect against a host of illnesses and diseases for both mothers and children.[11] Breastmilk provides all the energy and nutrients that the infant needs for the first months of life, and it continues to provide up to half or more of a child’s nutritional needs during the second half of the first year, and up to one third during the second year of life. [1]
Constitutes of breast milk[edit | edit source]
It contains fat, carbohydrates, proteins, vitamins, minerals and water. Breast milk also contains bioactive factors that augment the infant's immature immune system, providing protection against infection, and other factors that help digestion and absorption of nutrients.[12]
| Milk contain | Quantity per 100ml |
|---|---|
| Fat | 3.5g |
| Carbohydrate | 7g |
| Protein | 0.9g |
Other important points to be noted are:
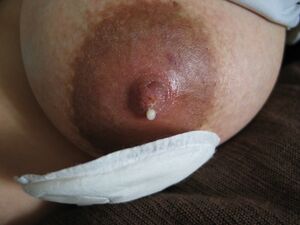
- The fat is secreted in small droplets, and the amount increases as the feed progresses. As a result, the hindmilk secreted towards the end of a feed is rich in fat and looks creamy white which fulfil hunger, while the foremilk at the beginning of a feed contains less fat and looks somewhat bluish-grey in color fulfil thirst. Thus, breastfeeding should be done for at least 15-20 minutes in order to help baby gain the weight.
- The amount of protein is much higher in animal milk than in human. The much higher protein in animal milks can overload the infant's immature kidneys with waste nitrogen products. Animal milk contain high amount of caesin which is hard to digest and make babies to vomit like curd. Along with that, beta-lactoglobulin in cow milk, which is absent from human milk, can become intolerant to infant.[12]
- The breast milk have enough vitamins and minerals need for infants, except for Vitamin D. The infant needs exposure to sunlight to generate endogenous vitamin D – or, if this is not possible, a supplement. The minerals iron and zinc are present in relatively low concentration, but their bioavailability and absorption is high.
- Immunoglobulin and white blood cells help protect child from infections.[12]
Quantity of Breast Milk[edit | edit source]
Milk production is related with a dose-response relationship, meaning there is also a positive effect of the number of breastfeeds in the first 24 hours on milk production on days 3 and 5 after birth. The interventions that promote an adequate milk supply by the first week postpartum are critical. These include skin-to-skin contact and milk removal (breastfeeding or expressing) within an hour of birth and frequent milk removal during the first 24 h after birth, and early initiation of lactation.[13] Milk production is also controlled in the breast by a substance called the feedback inhibitor of lactation, or FIL (a polypeptide), which is present in breast milk. If milk is not removed, the inhibitor collects and stops the cells from secreting any more, helping to protect the breast from the harmful effects of being too full. So if the baby cannot suckle, then milk must be removed by expression.[12]
Colostrum is the special milk that is secreted in the first 2–3 days after delivery. It is produced in small amounts, about 40–50 ml on the first day. On the third day, an infant is normally taking about 300–400 ml per 24 hours, and on the fifth day 500–800 ml.[12]
Reflexes in mother and hormonal control in milk production[edit | edit source]
Oxytocin reflex[edit | edit source]
Oxytocin reflex is also known as 'let-down reflex' or 'milk ejection reflex'.
- Oxytocin reflex stimulates when:
- A mother expects a feed
- When the baby is suckling
- Is conditioned by the mother's sensations and feelings, such as touching, smelling or seeing her baby, or hearing her baby cry, or thinking lovingly about him or her.
- If a mother is in severe pain due to improper positioning, cesarean section, episiotomy ,perineal tear or emotionally upset, the oxytocin reflex may become inhibited.
- Sensory nerve cells in the nipple signal brain to release oxytocin
- Posterior lobe of the pituitary gland secret oxytocin and are released into the bloodstream
- Oxytocin causes myoepithelial cells of alveoli to contract causing squeezing out the milk, pushing it down the ducts towards the nipple
- Oxytocin also makes the milk ducts widen, making it easier for the milk to flow down them.
Mothers may notice one of these signs that show that the oxytocin reflex is active:
- a tingling sensation in the breast before or during a feed;
- milk flowing from her breasts when she thinks of the baby or hears him crying;
- milk flowing from the other breast when the baby is suckling;
- milk flowing from the breast in streams if suckling is interrupted;
- slow deep sucks and swallowing by the baby, which show that milk is flowing into his mouth;
- uterine pain or a flow of blood from the uterus;
- thirst during a feed.[12]
Prolactin reflex[edit | edit source]
Prolactin stimulates the growth and development of the mammary tissue, in preparation for the production of milk. However, milk is not secreted then, because progesterone and oestrogen, the hormones of pregnancy, block this action of prolactin. After delivery, levels of progesterone and oestrogen fall rapidly, prolactin is no longer blocked, and milk secretion begins.[12]
Prolactin reflex is also known as 'milk secretion reflex'. Several factors enhance the prolactin reflex, these include: early initiation of breastfeeds, good attachment and effective suckling, frequent feeds including night feeds and emptying of breast. Other factors inhibit the prolactin reflex, these include: delay in the initiation of breastfeeds, pre-lacteal feeds, bottle feeding, incorrect breast feeding positioning, and painful breasts.
- When a baby suckles at the breast, sensory impulses pass from the nipple to the brain and prolactin hormone is secreted by the anterior lobe of pituitary gland.
- These are released in the bloodstream and travel to the alveoli of mammillary gland
- Milk is produced from the alveoli
Prolactin level is highest about 30 minutes after the beginning of the feed, so its most important effect is to secrete milk for the next feed. More prolactin is produced at night, so breastfeeding at night is especially helpful for keeping up the milk supply. Prolactin seems to make a mother feel relaxed and sleepy, so she usually rests well even if she breastfeeds at night. Suckling affects the release of other pituitary hormones, including gonadotrophin releasing hormone (GnRH), follicle stimulating hormone (FSH), and luteinizing hormone (LH), which results in suppression of ovulation and menstruation. Therefore, frequent breastfeeding can help to delay a new pregnancy. Breastfeeding at night is important to ensure this effect.[12]
Reflexes in baby[edit | edit source]
- Rooting reflex: When something touches a baby's lips or cheek, the baby turns to find the stimulus, and opens his or her mouth, putting his or her tongue down and forward. This is known as the rooting reflex and is present from about the 32nd week of pregnancy.
- Sucking reflex: When something touches a baby's palate, he or she starts to suck it. This is the sucking reflex.
- Swallowing reflex: When the baby's mouth fills with milk, he or she swallows. This is the swallowing reflex.
- Preterm infants can grasp the nipple from about 28 weeks gestational age, and they can suckle and remove some milk from about 31 weeks. Coordination of suckling, swallowing and breathing appears between 32 and 35 weeks of pregnancy. A majority of infants can breastfeed fully at a gestational age of 36 weeks.[12]
- Gag reflex: When something touches the anterior part of tongue, neonate try to vomit. This is known as gag reflex.
- Its purpose is to protect our airway and stop foreign objects and foods from ‘going down the wrong way’, reducing the risk of us choking.
- It is a reflex that is present from birth and remains with us for our whole lives.
- In babies, the gag reflex is further forward in the anterior part of tongue where as in adults in the posterior part of tongue. The gag reflex moves further back in the mouth with age and by around 9 months should be sitting around the back 1/3 of the tongue.
- By the age of 4-6 months baby will begin to have more control of this reflex, which coincides with being ready for weaning at around 6 months. [15]
Positioning and attachment in breastfeeding[edit | edit source]
Proper positioning and attachment is the crucial for a successful breastfeeding. Positioning and attachment are the terms used to describe how you hold your baby at your breast so they can feed.
Attachment[edit | edit source]
A baby needs to be well attached, to stimulate the nipple and remove milk from the breast, and to ensure an adequate supply and a good flow of milk, so that he or she can suckle effectively.
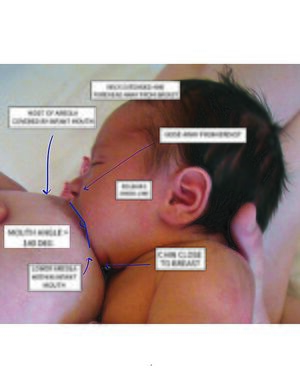
The things that need to be noticed for good latch:
- Hold your baby close with their nose level with your nipple.
- Let your baby’s head tip back so their top lip brushes against your nipple - this should help them open their mouth wide.
- When your baby’s mouth is wide open, bring them to your breast.
- Aim your nipple to the roof of their mouth.
- When they attach, your nipple and most of the areola (the area around your nipple) should be deep in your baby’s mouth.
- When your baby is attached properly, their chin will be pressed into your breast.
- Your baby's nose should be clear for easy breathing. Ideally, the nose should be at a tilt when attached correctly.
- Newborns are nose breathers. If they cannot breathe freely, they will come off the breast.
- In the correct position, your baby will be able to suck, swallow and breathe comfortably.
- If your baby's nose appears to be blocked, move their bottom closer to you. This will create a head tilt and free up their nose.
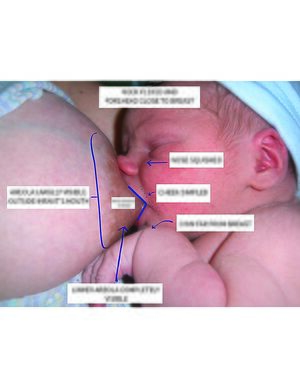
- The deeper the attachment the more comfortable you will feel and the better your baby will feed.
- More of your areola will be visible above their top lip than below their bottom lip.
- Their cheeks will appear fuller.
- They’ll suck quickly at first, followed by longer sucks.
- You will hear them swallowing[16].
When a baby is well attached his mouth and tongue do not rub or traumatise the skin of the nipple and areola. Suckling is comfortable and often pleasurable for the mother. She does not feel pain. Poor attachment may damage the skin of the nipple and areola, causing sore nipples and fissures (or “cracks”). Poor attachment is the commonest and most important cause of sore nipples and may result in inefficient removal of milk and apparent low supply.[12] Causes of poor attachment include: use of a feeding bottle before breastfeeding; functional difficulties such as flat and inverted nipples; or a very small or weak infant; congenital anomalies ( cleft palate, cleft tongue); and first-time mothers.[12]
Positioning[edit | edit source]
A baby and the mother need to be properly positioned for the good attachment of baby at the breast. There are several different positions for them both, but some key points need to be followed in any position.
Position of the mother[edit | edit source]
The mother can be sitting or lying down, or standing, if she wishes. However, she needs to be relaxed and comfortable, and without strain, particularly on her back. If she is sitting, her back needs to be supported, and she should be able to hold the baby at her breast without leaning forward. Considering that WHO recommendations state that exclusive breastfeeding should be done for 6 months and breastfeeding should continue to 2 years, and that breast feeding should be done frequently for at least 15-20 minutes each time, improper positioning can cause musculoskeletal disorders for mothers, particularly affecting the neck, upper back and lower back.[12]
Position of the baby[edit | edit source]
There are four key points about the position of the baby's body that are important:
- The baby's body should be straight, not bent or twisted. The baby's head can be slightly extended at the neck, which helps his or her chin to be close in to the breast.
- He or she should be facing the breast. The nipples usually point slightly downwards, so the baby should not be flat against the mother's chest or abdomen, but turned slightly on his or her back able to see the mother's face.
- The baby's body should be close to the mother which enables the baby to be close to the breast, and to take a large mouthful.
- His or her whole body should be supported. The baby may be supported on the bed or a pillow, or the mother's lap or arm. She should not support only the baby's head and neck. She should not grasp the baby's bottom, as this can pull him or her too far out to the side, and make it difficult for the baby to get his or her chin and tongue under the areola.[12]
Some of the positions that can be used during breastfeeding are:
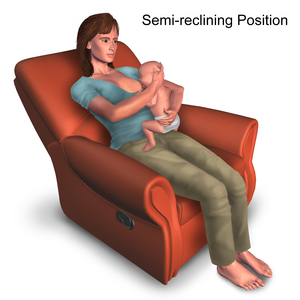
Laid back position: The movement needed to get into this position is from your pelvis. Shift your hips forward in a chair or bed to create a semi-reclined position. Laying your baby down on your semi-reclined body ensures they connect with your body without any gaps. Lay your baby on top of you with their tummy down and their cheek resting near your breast. Mother can also use pillows and cushions to provide support wherever you need it. It is advised to never fall asleep with your baby on a sofa or armchair as this increases the risk of sudden infant death syndrome.[16]
Cradle: Mother hold the head of the baby on the elbow of the same upper extremiy from the breast in which she is feeding, while the buttock of the baby supported on the hand of the mother. In this position, it is recommended that the mother puts pillows behind her back (shoulders and lower back), and under the elbow so that she can keep the child high enough. In this situation, light pressure is exerted on the mother’s neck, shoulders, arm, and back muscles. [17]
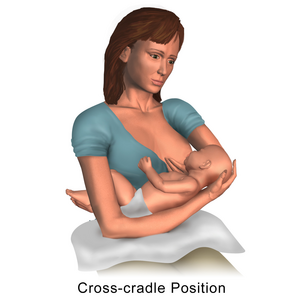
Cross- cradle: In this posture, it is recommended that 1) the mother sits upright and puts pillows behind her back. In this way, she does not have to bend over the infant. 2) The mother holds the infant horizontal or semi-horizontal on the pillow or cushion on her knees and thighs. 3) If the infant is feeding at the left breast, the mother holds the infant with the right hand and vice versa
Football hold: Support your baby’s neck, back and shoulders with your hand and wrist. Let your baby’s back lie along your arm. Your baby should be facing you with their nose near the nipple. Support your breast with your other hand. This position is advisable for caesarean section delivery and for twin-delivery.
Side-lying: Mother and the baby lie down facing each other. Make sure your neck and back are supported and comfortable. Your baby's chest should face your chest. Take the arm that you're lying on and either place it under your head or use it to support your baby by placing it under their head or around their body. You can use a pillow or rolled-up blanket behind your baby's back for support. This position is usually not advisable as milk can enters into the ear, causing frequent acute suppurative otitis media(ASOM).
Breast feeding and Physiotherapy[edit | edit source]
Physiotherapists can help both the mother and baby for the successful breast feeding.
- Prenatal classes can be used to help inform women about the health advantages of breastfeeding, both for babies and mothers, and instructors can explain to women the process and techniques they can use to breastfeed.[3] Proper attachment and positioning can be taught prenatally and postnatally to the mothers and their family.
- Improper positioning of the mother can cause neck, upper back and lower back pain. Postural advice to ensure ergonomic efficiency is recommended; the proper positioning of the mother during a feed, with the back and forearm supported with no forward leaning is advised. The heaviness of the breast during postnatal period can also strain upper back; it is advisable for mothers to wear a suitably supportive bra.
- Simple exercises which incorporate neck, shoulder and scapular muscle stretching exercises, and scapular retractor strengthening exercises during the postnatal period are advisable.
- Since premature babies have difficulty in coordinating suckling, swallowing and breathing, oromotor exercises for the stimulation of sucking and swallowing are beneficial.
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 Breast feeding. World Health Organization. Available from: https://www.who.int/health-topics/breastfeeding#tab=tab_1 lasted assessed: 25th Feb 2022
- ↑ Afshariani R, Kiani M, Zamanian Z. The influence of ergonomic breastfeeding training on some health parameters in infants and mothers: a randomized controlled trial. Archives of Public Health. 2019 Dec;77(1):1-0.
- ↑ 3.0 3.1 Office of the Surgeon General. Breastfeeding from the Public Health Perspective.
- ↑ 4.0 4.1 4.2 Jama A, Gebreyesus H, Wubayehu T, Gebregyorgis T, Teweldemedhin M, Berhe T, Berhe N. Exclusive breastfeeding for the first six months of life and its associated factors among children age 6-24 months in Burao district, Somaliland. International breastfeeding journal. 2020 Dec;15(1):1-8.
- ↑ 5.0 5.1 5.2 5.3 Dukuzumuremyi JP, Acheampong K, Abesig J, Luo J. Knowledge, attitude, and practice of exclusive breastfeeding among mothers in East Africa: a systematic review. International Breastfeeding Journal. 2020 Dec;15(1):1-7.
- ↑ 6.0 6.1 Pérez-Escamilla R, Buccini GS, Segura-Pérez S, Piwoz E. Perspective: should exclusive breastfeeding still be recommended for 6 months?. Advances in Nutrition. 2019 Nov 1;10(6):931-43.
- ↑ Boland M. Exclusive breastfeeding should continue to six months. Paediatrics & child health. 2005 Mar 1;10(3):148-.
- ↑ World Health Organization. Infant and young child feeding: model chapter for textbooks for medical students and allied health professionals. World Health Organization; 2009.
- ↑ CDC. Lactational Amenorrhea Method [online]. 2022
- ↑ Breast feeding for a healthier planet. The Lactation network. Available from: https://lactationnetwork.com/blog/environmental-benefits-breastfeeding/#:~:text=Breastfeeding%20reduces%20the%20release%20of%20methane.&text=According%20to%20the%20EPA%2C%20methane,more%20powerful%20over%2020%20years. lasted accessed: 25th Feb, 2022
- ↑ Office of the Surgeon General. The importance of breastfeeding. The Surgeon General's Call to Action to Support Breastfeeding. US Department of Health and Human Services. https://www. ncbi. nlm. nih. gov/books/NBK52687. 2011.
- ↑ 12.00 12.01 12.02 12.03 12.04 12.05 12.06 12.07 12.08 12.09 12.10 12.11 12.12 World Health Organization. Infant and young child feeding: model chapter for textbooks for medical students and allied health professionals. World Health Organization; 2009. The physiological basis of breastfeeding.
- ↑ Kent JC, Gardner H, Geddes DT. Breastmilk production in the first 4 weeks after birth of term infants. Nutrients. 2016 Dec;8(12):756.
- ↑ Milk Ejection Reflex - Physiology. Available from: https://www.youtube.com/watch?v=kCN9ZHhZkeU
- ↑ Feed Eat Speak. Helping an overactive gag reflex. The gagging reflex. Available from: https://www.feedeatspeak.co.uk/blog/2020/5/21/helping-an-overactive-gag-reflex#:~:text=In%20babies%20the%20gag%20reflex,weaning%20at%20around%206%20months. Lasted accessed: 28th Feb 2022
- ↑ 16.0 16.1 Our Health Services. Positioning and attachment. Available from: https://www2.hse.ie/wellbeing/babies-and-children/breastfeeding/a-good-start/positioning-and-attachment/ lasted accessed: 28th Feb 2022
- ↑ Afshariani R, Kiani M, Zamanian Z. The influence of ergonomic breastfeeding training on some health parameters in infants and mothers: a randomized controlled trial. Archives of Public Health. 2019 Dec;77(1):1-0.
- ↑ 6 Oral Motor Exercises for Babies - Oral Stimulation- Speech Development- Feeding Development. Available from: https://www.youtube.com/watch?v=QOcBCd-4I4c
- ↑ Oral motor stimulation & non nutritive sucking in neonates. Available from: https://www.youtube.com/watch?v=1H0Pc5OU2cY