Biomechanics of the Hip
Original Editor - Ewa Jaraczewska based on course by Rina Pandya
Top Contributors - Ewa Jaraczewska, Jess Bell, Rucha Gadgil, Kim Jackson and Lucinda hampton
Introduction[edit | edit source]
"Biomechanics is simply the physics (mechanics) of motion exhibited or produced by biological systems. More specifically, biomechanics is a highly integrated field of study that examines the forces acting on and within a body as well those produced by a body".[1]
When discussing hip joint biomechanics, one must consider how the bones, ligaments, and muscles transfer the weight of the body from the axial skeleton into the lower limb.[2]
Static Loading[edit | edit source]
Koch’s model[edit | edit source]
Koch first introduced the static model of hip biomechanics. According to his theory, the body lever arm and the abductor muscles lever arm has a ratio of 2:1. This means that in a single-leg stance, gluteus medius needs to generate two times the body weight's force to maintain balance and prevent the body from leaning towards the unsupported side. In this model, gluteus medius is the only muscle that provides resistance to the loads exerted on the femur. Koch proposed that gluteus medius translates these loads into tensile loads on the lateral aspect of the femur below the attachment of the gluteus medius and into compressive loads on the lateral side of the distal third of the femur. It has been noted, however, that Koch's original statement did not explain well how tensile load was converted into a compressive load in the distal part of the femur.[3]
Bilateral Limb Support[edit | edit source]
In newborns and up until the age of four, the neck-shaft angle of the femur has a value of approximately 160-165 degrees.[4] Upright posture continues to reduce this angle until it reaches an angle of 130-135 degrees. It then remains unchanged throughout the process of body development and bone growth despite the amount of time humans spend upright and the fact that body mass continues to increase.[5]
During bilateral limb stance, the centre of gravity is located between the two hips, with an equal force exerted on both hips. The body’s centre of gravity is located approximately one centimetre anterior to the first sacral segment.[5] Gravity affects the lower extremities in the vertical direction. Under these loading conditions, the weight of the body minus the weight of both legs is supported equally on the femoral heads.[5]
Bone tissue responds to various demands, including those influenced by the environment. Specific responses include the development of a hypertrophic or an atrophic bone or an alteration in bone quality in areas of compression (cortical bone) or tensile loading (cancellous bone).[5]
Joint stability in the lower limbs depends on:[5]
- Articular geometry: stability in the hip, knee and the ankle
- Soft tissue integrity: stability of the dynamic (muscle, tendon, fascia) and static elements (ligaments). In response to demands, the dynamic structures adjust their length. The static structures will become taut in extension on one side and, correspondingly, taut in flexion on the other side.[5]
Single Leg Stance[edit | edit source]
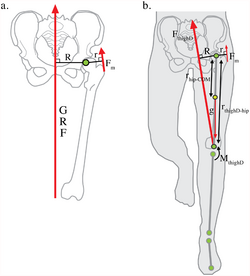
During single-leg stance, the following occur:[7]
- Centre of gravity moves distally and away from the supporting leg
- The non-supporting leg becomes a part of the body mass acting upon the weight-bearing hip
- The downward force exerts a turning motion around the centre of the femoral head
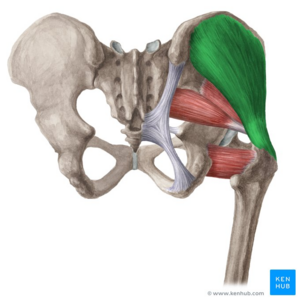
- The abductors, including the upper fibres of the gluteus maximus, the tensor fascia latae, the gluteus medius and minimus, the piriformis and obturator internus, offset the action of the muscles resisting the rotation of the femoral head. This creates a moment around the centre of the femoral head
- The lever of the abductors is shorter than the lever arm of body weight. Therefore, the combined force of the abductors must be multiples of body weight (typically three times body weight), which corresponds to a lever ratio of 2.5
Larger hip forces are required for people who have a wide pelvis and short femoral necks. These people have an increased lever arm ratio, and thus require an increase in abductor muscle force. These individuals tend to be at high risk for hip pathologies, including arthritic conditions.[5] However, a study by Warrener et al.[8] found that pelvic width does not predict hip abductor mechanics or locomotor cost in either women or men.
Examples of postures which indicate an increased lever arm and decreased hip abduction force:[7]
- In supine legs are "falling out"
- In sitting with ankles crossed, a patient's large abdomen forces their hips into abduction and external rotation with their knees "flopped out"
Joint Forces at the Hip[edit | edit source]
The average loads on the hip joint measured in subjects who underwent a total hip replacement were as follows:
- Walking: about 4 km/h, 238% of body weight (BW) (160 to 330% BW)[9][10]
- Stair descending: 108% to 260% BW[11]
- Stair ascending: 251% BW[10]
- During chair rise and bending: 40% BW[11]
- Standing: 32% BW
- Single leg stance: 230 to 290% BW [9]
Note: "stumbling or periods of instability during single-leg stance can generate resultant forces in excess of eight times body weight"[12]
The above numbers indicate that the highest stress on the hip joint occurs during walking and descending stairs. Development of hip pathology, eg. osteoarthritis can be predicted when these activities are performed repetitively and/or under faulty conditions. [11]
Dynamic Model of Hip Biomechanics[edit | edit source]
According to Koch,[3] in order to maintain hip stability, gluteus medius must generate twice the weight of the body force during a single-leg stance. However, based on different data related to hip dynamics and a complete model of stability, it has been concluded that the iliotibial band (ITB) plays a significant role in maintaining hip stability. The following observations support this theory:[5]
- Gluteus medius is less active at the midstance phase of gait
- The iliotibial band serves as a tension band to relieve the metabolic demand and reduce the electrical activity of the gluteus medius during the midstance phase of gait
- Patients with below-knee amputations present with a compromised function of the ITB as a stabiliser of the hip joint due to loss of its distal attachment[5]
Clinical Relevance[edit | edit source]
Painful Hip[edit | edit source]
Management of hip pain should include a reduction of the joint reaction force. It can be accomplished through the following:
- Body mass reduction
- Increasing abductor force
- Decreasing the moment arm by bringing the centre of gravity closer to the centre of the femoral head by:
- Limping (antalgic gait)
- Using a cane in the opposite hand - this reduces the joint reaction force by 50% when approximately 15% of body weight is applied to the cane.[13]
When a person is using a cane for support, the joint reaction force is reduced because the "cane-ground reaction force acts at a much larger distance from the centre of the hip than the abductor's muscles".[13] Even when a small load is applied through the cane, the patient is able to reduce the demand required from the abductor muscles to maintain joint stability during gait.[13]
Stair Climbing[edit | edit source]
When ascending stairs, patients with osteoarthritis demonstrate:[14]
- Limited range of motion in the hip in all three planes: sagittal, transverse and frontal
- Lower hip peak external rotation moment
When descending stairs, these patients demonstrate:
- Increased in ipsilateral trunk lean
- Reduction in sagittal plane range of motion
- Lower external peak extension moment
- Lower external peak rotation moment
- Higher hip adduction moment
- Higher hip adduction moment impulse
- Higher internal rotation moment impulse[14]
The physiotherapy approach to improving stair negotiation for people with osteoarthritis may include:
- TENS as an option for reducing early-stage knee OA-related burden[15]
- Resistance training for improving hip muscle mass. This was found to be positively correlated with performance in stair climbing and chair stand[16]
- Prescribing endurance training for patients with moderate-to-severe hip osteoarthritis. It can improve the endurance capacity of the knee extensors, which play an important role in daily function[17]
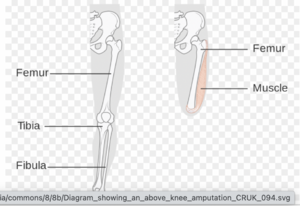
Lower Extremity Amputation[edit | edit source]
Patients with above-knee amputation exhibit a positive Trendelenburg gait pattern despite having intact hip abductors. However, in this patient group, the gluteus medius is not able to provide adequate hip stability during gait due to the loss of the iliotibial band action in providing additional joint stability.
Treatment may include the surgical technique of tenodesis of the ITB and lateral soft tissue structures to the distal femur.[5]
Resources[edit | edit source]
- Zaghloul A, Elalfy MM. Hip Joint: Embryology, Anatomy and Biomechanics. Biomed J Sci & Tech Res, 2018 12(3).
- Hip Biomechanics https://www.orthobullets.com/recon/9064/hip-biomechanics
References[edit | edit source]
- ↑ McLester J, Pierre PS. Applied Biomechanics. Jones & Bartlett Learning; 2019 Mar 8.
- ↑ Van Houcke J, Khanduja V, Pattyn C, Audenaert E. The history of biomechanics in total hip arthroplasty. Indian Journal of Orthopaedics. 2017 Aug;51(4):359-67.
- ↑ 3.0 3.1 Fetto J, Leali A, Moroz A. Evolution of the Koch model of the biomechanics of the hip: a clinical perspective. J Orthop Sci. 2002;7(6):724-30.
- ↑ Feger J. Femoral neck-shaft angle. Reference article, Radiopaedia.org. (accessed on 07 Mar 2022) https://doi.org/10.53347/rID-81120
- ↑ 5.0 5.1 5.2 5.3 5.4 5.5 5.6 5.7 5.8 5.9 Fetto JF. A dynamic model of hip joint biomechanics: The contribution of soft tissues. Advances in Orthopedics. 2019 Jun 4;2019.
- ↑ Mock FRCS Cardiff. Free body diagram hip. 2016. Available from: https://www.youtube.com/watch?v=H0SoMQ_L7-k [last accessed 27/02/2022]
- ↑ 7.0 7.1 Pandya R. Biomechanics of the Hip Course. Plus. 2022.
- ↑ Warrener AG, Lewton KL, Pontzer H, Lieberman DE. A wider pelvis does not increase locomotor cost in humans, with implications for the evolution of childbirth. PLoS One. 2015 Mar 11;10(3):e0118903.
- ↑ 9.0 9.1 Rydell NW. Forces acting on the femoral head prosthesis. A study on strain gauge supplied prostheses in living persons. Acta Orthop Scand. 1966;37:Suppl 88:1-132.
- ↑ 10.0 10.1 Bergmann G, Deuretzbacher G, Heller M, Graichen F, Rohlmann A, Strauss J, Duda GN. Hip contact forces and gait patterns from routine activities. J Biomech. 2001 Jul;34(7):859-71.
- ↑ 11.0 11.1 11.2 Luepongsak N, Amin S, Krebs DE, McGibbon CA, Felson D. The contribution of type of daily activity to loading across the hip and knee joints in the elderly. Osteoarthritis Cartilage. 2002 May;10(5):353-9.
- ↑ Bergmann G, Deuretzbacher G, Heller M, Graichen F, Rohlmann A, Strauss J, Duda GN. Hip contact forces and gait patterns from routine activities. J Biomech. 2001 Jul;34(7):859-71.
- ↑ 13.0 13.1 13.2 Lim LA, Carmichael SW, Cabanela ME. Biomechanics of total hip arthroplasty. The Anatomical Record: An Official Publication of the American Association of Anatomists. 1999 Jun 15;257(3):110-6.
- ↑ 14.0 14.1 Hall M, Wrigley TV, Kean CO, Metcalf BR, Bennell KL. Hip biomechanics during stair ascent and descent in people with and without hip osteoarthritis. Journal of Orthopaedic Research. 2017 Jul;35(7):1505-14.
- ↑ Iijima H, Eguchi R, Shimoura K, Yamada K, Aoyama T, Takahashi M. Transcutaneous electrical nerve stimulation improves stair climbing capacity in people with knee osteoarthritis. Scientific reports. 2020 Apr 29;10(1):1-9.
- ↑ Bieler T, Kristensen AL, Nyberg M, Magnusson SP, Kjaer M, Beyer N. Exercise in patients with hip osteoarthritis–effects on muscle and functional performance: A randomized trial. Physiotherapy Theory and Practice. 2021 May 8:1-2.
- ↑ Burgess LC, Taylor P, Wainwright TW, Swain ID. Strength and endurance deficits in adults with moderate-to-severe hip osteoarthritis, compared to healthy, older adults. Disability and Rehabilitation. 2021 Jun 20:1-8.