Aspiration Pneumonia
Original Editor - Lucinda hampton
Top Contributors - Lucinda hampton
Introduction[edit | edit source]
Aspiration pneumonia (AP) is a common disease that frequently occurs in older patients, with many of these patients having a swallowing disability. Research is limited, but reveals that aspiration pneumonia contributes 5% to 15% of all community-acquired pneumonia. AP is frequently under-diagnosed as although easily diagnosed if overt aspiration events are witnessed, but often silent unobserved aspirations occurs making diagnosis of AP challenging. [1]
In pneumonia, microaspiration is the usual pathogenic mechanism, while “aspiration pneumonia” refers to the aspiration of a large amount of oropharyngeal or upper gastrointestinal content moving through the vocal cords and trachea into the lungs. Put simply AP is an infection of the lungs caused by inhaling saliva, food, liquid, vomit and even small foreign objects.[2]
Pathogenesis[edit | edit source]
In normal healthy people, both the mucociliary mechanism and alveolar macrophages work to defend and protect the respiratory system from micro aspirations of oropharyngeal secretions. The pathological process of AP occurs when the the usual defence mechanisms fail in the predisposed person. Upon entry of fluids into the bronchi and alveolar space an anti-inflammatory reaction is triggered and the release of proinflammatory cytokines, tumor necrosis factor-alpha, and interleukins occur.[3]
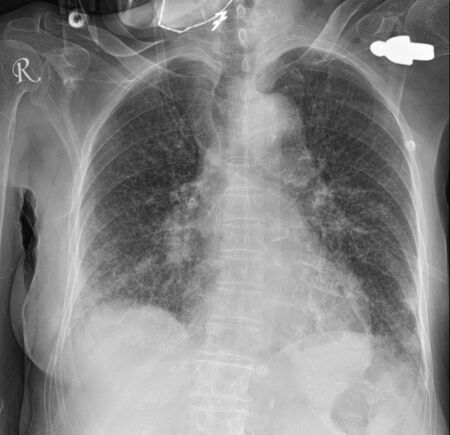
Below: Bilateral inhomogeneous patchy airspace opacities mainly in the lower zones. Effacement of the costophrenic recesses consistent with aspiration.
Risk Factors[edit | edit source]
Include:
- Impaired swallowing (dysphagia, chronic obstructive pulmonary disease, neurological diseases eg stroke, Parkinsons plus, motor neurone disease, dementia, need of mechanical ventilation),
- Weakened cough reflex (medications, stroke, dementia, impaired consciousness and alcohol).
- Reduced consciousness (eg acute stroke, traumatic brain injury, seizures and the effect of some agents that can induce impaired consciousness such as alcohol, drugs, anesthesia or sedatives),
- Greater likely hood of gastric contents reaching the lung (reflux and tube feeding).[2]
Management[edit | edit source]
- Initially the patient's position must be adjusted, then suction of oropharyngeal contents via a nasogastric tube.
- Flexible bronchoscopy may be used to clear large volume aspiration and the secretions and also too obtain of sample for bacteriological studies. Generally, antibiotics are started immediately even though to prevent the progression of the disease.
- Additional treatment might include oxygen therapy or, in life-threatening cases, mechanical ventilation. Close monitoring of the patient's oxygen saturation is critical and swift intubation with mechanical ventilation should be provided if hypoxia occurs.[3]
Physiotherapy[edit | edit source]
Aspiration pneumonia often times occurs in elderly patients, many of whom have patients swallowing disability and develop hospital‐acquired disability. Frequently, patients have difficulty returning home, and they often require long‐term hospitalisation. Therefore physiotherapy for frailty will be appropriate at later stage of treatment.
- Acute‐phase physical rehabilitation programs for AP in the debilitated/older patients includes: early mobilization; pulmonary rehabilitation (positioning, postural drainage, sputum elimination assistance, respiration training guidance); upper limb range-of-motion exercises; functional self‐care exercises; strengthening and endurance exercises; sitting postural education and importance of sit during the daytime; standing, balance and gait training are introduced as required.
- See also page with specifics for physiotherapy in pneumonia here
Other applied health professionals (occupational therapy to help return home are often involved in the management of these clients eg occupational therapy to help return home, dysphagia rehabilitation by speech therapist, and rehabilitation nutrition by dietician.[4]
References[edit | edit source]
- ↑ Almirall J, Boixeda R, de la Torre MC, Torres A. Aspiration pneumonia: A renewed perspective and practical approach. Respiratory Medicine. 2021 Aug 1;185:106485.Available:https://www.resmedjournal.com/article/S0954-6111(21)00191-8/fulltext#secsectitle0050 (accessed 12.11.2023)
- ↑ 2.0 2.1 Niederman MS, Cilloniz C. Aspiration pneumonia. Revista Española de Quimioterapia. 2022;35(Suppl 1):73.Available:https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9106188/ (accessed 12.11.2023)
- ↑ 3.0 3.1 Sanivarapu RR, Gibson J. Aspiration pneumonia.Available:https://www.ncbi.nlm.nih.gov/books/NBK470459/ (accessed 12.11.2023)
- ↑ Momosaki R. Rehabilitative management for aspiration pneumonia in elderly patients. Journal of general and family medicine. 2017 Mar;18(1):12-5.Available:https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5675146/ (12.11.2023)