Ageing and the Locomotor System
Original Editor - Simisola Ajeyalemi
Top Contributors - Simisola Ajeyalemi, Lucinda hampton, Kim Jackson and Rucha Gadgil
Introduction[edit | edit source]
The locomotor system is also known as the musculoskeletal system.
- It is made up of the skeleton, skeletal muscles, ligaments, tendons, joints, cartilage and other connective tissue.
- These parts work together to allow your body to move.
Changes in the locomotor system with ageing can include the issues addressed below.
Posture[edit | edit source]
Age-related hyperkyphosis affects 20-40% of older adults and can be described as an exaggerated anterior curvature of the thoracic spine that is associated with aging.[1]
- Stooped posture, loss of height, and other distortions owing to atrophy and effect of weakness in skeleton and major muscle groups become responsible for posture and antigravity support.
- The result is a more flexed posture with altered biomechanics, muscle imbalance, and slowly decreasing range in joints and overall decrease in safety.
- The therapist may have to provide: exercises for strength, coordination and balance; walking aids; a wheelchair for the person if necessary.
Muscle Changes[edit | edit source]
1.Sarcopenia is defined as being a decline in muscle function (either walking speed or grip strength) associated with loss of muscle mass[2]. Sarcopenia most commonly affects elderly and sedentary populations and patients who have comorbidities that affect the musculoskeletal system or impair physical activity[3]. Sarcopenia leads to disability, falls, and increased mortality. Loss of muscle strength and aerobic function are 2 of the hallmarks of frailty. Sarcopenia has been linked to an increased prevalence of osteoporosis, thus further increasing its propensity to produce fractures.
- If dietary intake of protein is poor, this will increase the problem
2.In aged muscle, satellite cells (act as stem cells and are responsible for the further growth and development of skeletal muscles) that experience prolonged quiescence undergo programmed cellular senescence. This is an irreversible non-dividing state that handicaps the regenerative capabilities of muscle. In the older person, training counteracts the normal decline in satellite cell number seen with ageing[4].
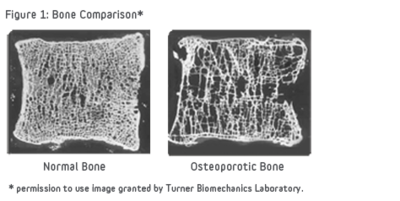
Effects of Ageing on Bone[edit | edit source]
Ageing affects the bones. Osteoporosis is a major public health problem affecting millions of elderly individuals. Besides causing fractures, the disorder leads to severe psychosocial and financial consequences for the patient. The condition has many risk factors and is best managed by an interprofessional team of healthcare workers[5].
By 60–70 years, skeletal mass may be reduced to half of that at age 30.
- If dietary intake of vitamins and calcium is poor, this will increase the problem.
- Osteoporosis increases the risk of insufficiency fractures. This can lead to later issues with range in the joint and mobility of the muscle[6].
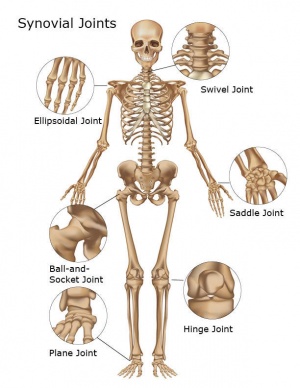
Effects of Ageing on Joints[edit | edit source]
Ageing affects the joints. No matter how healthy an individual is, as they age their joints will show some changes in mobility, due in part to changes in the connective tissues. As joint range of movement has a direct effect on posture and movement, this can result in marked alteration of function.
By age 65, 80% of the population has some articular disorder
- eg Loss of resilience and elasticity in ligaments, cartilage and periarticular tissues; degeneration with erosion, and calcification of cartilage and capsule; gradual reduction in collagen but not in the water content.
- Bunions, subluxation of small joints in hands and feet are common, as are painful feet and other chiropody problems.
- Proprioception and general sensation may be decreased if changes to muscle and joints are compounded by nerve damage.
Loss of muscle bulk, degenerative joint changes and a decline in physical strength cause limitation of range and speed of movement. Disability ensues as a combined effect of muscular weakness, joint stiffness and impaired central mechanism for sensorimotor performance, so there is:
- Less precision in fine movements and in rapid alternating movements
- Irregular timing of action, loss of smooth flow of one form of action into another
- Slowing down to avoid outcome of one action before planning the next. Confidence and reliability of action may be reduced. The individual may experience difficulty with intricate tasks (worse if complicated by uncompensated visual defect).
Balance[edit | edit source]
Decreased balance is attributable to an age-related decline in multiple physiological systems due to to:
- Decreased muscle flexibility and strength
- Reduced central processing of sensory information
- Slowed motor responses.
In addition to an increased risk of falls, diminished balance and mobility may limit:
- Activities of daily living
- Participation in leisure-time activities.
Accordingly, it is essential that balance exercises be incorporated into the physical activity programs of older adults.[7]
Treatment[edit | edit source]
See Physical Activity in Ageing and Falls and Physical Activity in Older Adults
As is commonly known, there are many health benefits of exercise, and this stands true for adults of all ages. Resistance training will improve strength and can reverse or delay the decline in muscle mass and strength that occurs with age. Aerobic exercise can help to improve endurance by increasing the capillary density, mitochondrial and enzyme levels in the skeletal muscles. Together this can help older adults to maintain their participation in ADLs and therefore maintain independence.[8]
The type of exercise and intensity will depend upon the ability of the person. Physical activity for older adults can take many forms (e.g. walking, swimming, stretching, dancing, gardening, hiking, cycling or organised exercise sessions). However, there are several important considerations specific to the older adult population with regard to physical activity recommendations:
- The intensity of aerobic activity takes into account the older adult's aerobic fitness.
- Activities that maintain or increase flexibility are recommended.
- Balance exercises are recommended for older adults at risk of falls.
- Older adults that have medical conditions or disabilities that may affect their capacity to be physically active should seek advice from a doctor.
Resources[edit | edit source]
Ageing and the Locomotor System
References[edit | edit source]
- ↑ Jang et al., H. (2015). Effect of thorax correction exercises on flexed posture and chest function in older women wih age-related hyperkyphosis. J. Phys. Ther. Sci. , 27, 1161-1164.
- ↑ Malmstrom TK, Morley JE. SARC-F: a simple questionnaire to rapidly diagnose sarcopenia. Journal of the American Medical Directors Association. 2013 Aug 1;14(8):531-2.Available from: https://www.researchgate.net/publication/243966215_SARC-
- ↑ Ardeljan AD, Hurezeanu R. Sarcopenia. StatPearls [Internet]. 2020 Jul 10. Available from:https://www.ncbi.nlm.nih.gov/books/NBK560813/ (accessed 9.3.2021)
- ↑ Snijders T, Nederveen JP, McKay BR, Joanisse S, Verdijk LB, van Loon LJ, Parise G. Satellite cells in human skeletal muscle plasticity. Frontiers in physiology. 2015 Oct 21;6:283.Available from: https://www.frontiersin.org/articles/10.3389/fphys.2015.00283/full#h8(accessed 21.3.2021)
- ↑ Joann L. Porter; Matthew Varacallo 19.12.2019 Osteoporosis Available from:https://www.ncbi.nlm.nih.gov/books/NBK441901/ (last accessed 27.2.2020)
- ↑ Locomotor System Available from: Images/1/12/Ageing locomotor system.pdf (accessed 21.3.2021)
- ↑ NeuRa Balance training Available from:https://www.neura.edu.au/health/balance-training/ (Last accessed 17.10.2020)
- ↑ Liu CJ, Latham NK. Progressive resistance strength training for improving physical function in older adults (review). Cochrane database of systematic reviews. 2009 (3)