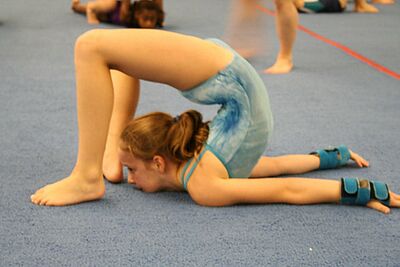Lumbar Spondylolysis in Extension Related Sport
Top Contributors - Lewis Crouch, Melissa Coetsee and Kim Jackson
Introduction[edit | edit source]
Lumbar Spondylolysis refers to a unilateral or bilateral defect of the pars interarticularis of the vertebral arch, which can be accompanied by vertebral displacement in the lumbar region [1]. Spondylolysis derives from the Greek words Spondylo (spine) and Lysis (to dissolve) [2]. Spondylolysis is a common cause of low back pain.
Clinically Relevant Anatomy[edit | edit source]
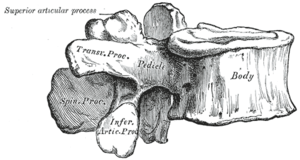
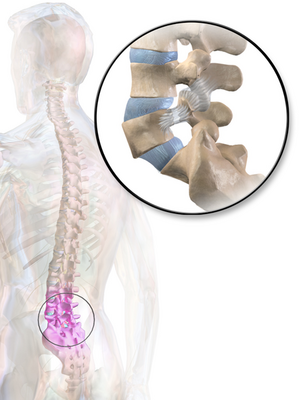
Small structures called vertebrae comprise the vertebral column, otherwise known as the spine. The vertebral column extends from the base of the skull to the coccyx, protecting the length of the spinal cord. In human anatomy, the lumbar vertebrae lie between the rib cage and top of the sacrum. Lumbar vertebrae are the largest of the vertebral column [3]. Together they form the curve of the lower back, known as lordosis. Each lumbar vertebrae consist of the vertebral body and a bony ring or arcus which protects the spinal cord. The arcus is formed by two pedicles which attach to the dorsal side of the vertebral body and two laminae, which complete the arch. The area between the pedicle and the lamina is called the pars interarticularis and is in fact the weakest part of the arcus[4]. It is the pars interarticularis that is affected in spondylolysis.
Epidemiology/Etiology[edit | edit source]
The incidence of lumbar spondylolysis has been estimated to be approximately 6% in the general population[2] and is twice as prevalent in males compared to females[5], with the highest incidence found among adolescent athletes (15-47%)[2][6]. Incidence can also vary in different countries - the incidence in the United States is reported to be 11.5% [7], while the incidence in the Japanese population is predicted to be around 5.9% [8].
Lumbar spondylolysis will typically begin as a stress fracture in one of the two pars interarticularis’ which make up the vertebrae. The unilateral fracture can lead to increased load on the contralateral side which could cause a bilateral pars interarticularis fracture, and eventually spondylolisthesis (slipping of the vertebrae) [9].
One of the main risk factors of lumbar spondylolysis is believed to be repeated hyperextension and is more commonly seen in athletes that repeatedly go into end range lumbar extension, e.g. ballet dancers, gymnasts, cricketers, tennis players etc.[2] [6]. Research has illustrated that extension movements with compression result in more stress on the pars interarticularis than just compression alone[2]. Furthermore, lumbar spondylolysis is more common in adolescents due to differences in trabecular bone density in the developing spine[2]. The pars interarticularis is said to have not achieved full bony remodelling until the age of 25, therefore anyone under this age will be at a high risk of developing lumbar spondylolysis[5].
Lumbar spondylolysis mainly affects the L5 vertebrae which accounts for 85%-95% of all cases [2]. This is thought to be due to the facet joint positioning of the L5/S1 vertebrae. The posterior facing facet of the S1 vertebrae creates anterior shear upon the pars interarticularis of the L5 vertebrae which increases in individuals with excessive anterior pelvic tilt[5]. The enhanced anterior pelvic tilt is a very common movement pattern in extension-related sports such as ballet, gymnastics and tennis, making individuals in these sports more susceptible to the development of spondylolysis.
Spondylolisthesis[edit | edit source]
Spondylolisthesis is the slippage of one vertebral body on top of another. This can occur where bilateral pars defects exist[2]. Spondylolisthesis is graded based on the degree a vertebral body anterior shift [7]. Slippage progression reduces significantly with spinal maturity[2]. There are 6 known types of spondylolisthesis first introduced by Wiltse in 1976 [10]:
- Degenerative: Occurs due to degenerative changes in the vertebra.
- Isthmic: Results from defects in the bilateral pars interarticularis
- Dysplastic: A congenital birth defect that occurs at level L5/S1
- Traumatic: Commonly seen after trauma of the pars interarticularis
- Pathologic: Seen in bone or connective tissue disorders such as Paget’s disease
- Iatrogenic: Commonly seen after the removal of large sections of the spine
Isthmic spondylolisthesis is most commonly seen in athletes primarily due to the frequency of extension and rotation related movements they carry out, particularly in the adolescent population [7].
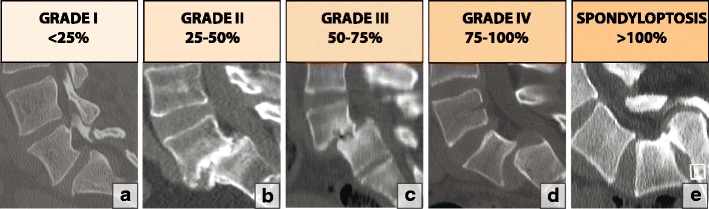
The Meyerding scale is the grading system used in spondylolisthesis. It categorises the degree of vertebral slippage: [11]
Clinical Presentation[edit | edit source]
Spondylolysis sufferers are often asymptomatic, with approximately 10% of affected individuals exhibiting symptoms[5].
Subjective Assessment[edit | edit source]
- Insidious or gradual onset
- Low back pain primarily worsening with extension-related activities[5]
- Pain varies from a dull ache to sharp pain especially upon extension [5]
- Pain may radiate to the buttock [5]
- Pain worsening with sport activity and improves with rest [5]
Objective Assessment[edit | edit source]
- Tenderness and pain on palpation of the spinous process of affected vertebra [5]
- Excessive lordosis in the lumbar spine or flattening of the lumbar spine [5][11]
- Individuals may be excessively hypermobile [5]
- Muscle guarding either unilateral or bilateral of erector spinae [5]
- Weakness in gluteals and abdominals [5]
- Pain on extension [5]
- Positive single-leg hyperextension test - not very sensitive or specific [5]
- Hamstring and hip flexor tightness [5]
Differential Diagnosis[edit | edit source]
For a list of differential diagnoses, please see the Spondylolysis page.
Diagnostic Procedures[edit | edit source]
One-Legged Hyperextension Test[edit | edit source]
The one-legged hyperextension manoeuvre is an orthopaedic test used to assist in the diagnosis of spondylolysis. Although one of the very few diagnostic tests used by clinicians, research has found it to have limited value in the diagnosis of spondylolysis [12]. It has very low specificity and moderate sensitivity. It is performed by asking the patient to lean back while standing on one leg. A positive test will reproduce pain, either unilaterally or bilaterally; unilateral lesions will reproduce pain when performed on the ipsilateral leg [13].
Spinous Process Palpation[edit | edit source]
This is regarded as a potentially useful clinical test for lumbar spondylolisthesis, with high sensitivity and specificity[12].
Diagnostic Imaging[edit | edit source]
At times it may be necessary for multiple types of medical imaging in order to make an accurate diagnosis[5]. It is however important to consider the amount of radiation exposure in adolescents.
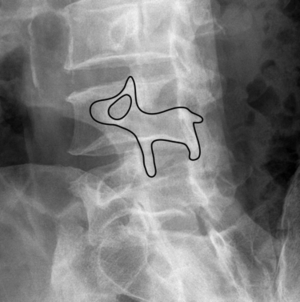
- X-rays are usually the first line of diagnostic testing, but have limited sensitivity when compared to CT scans [5]. Oblique planes provide the best angle to spot pars interarticularis defects [5]. In lumbar spondylolysis, the appearance of a dog like structure can be seen on a plain radiograph when there is a pars interarticularis fracture. This is referred to as the ‘scotty dog’ sign which is seen in oblique planes only [14].
- Single Photon Emission Computerised Tomography (SPECT) is quite sensitive for detecting spondylolysis, but its use in clinical practice has declined[2]
- Computerised Tomography (CT) scan is the most specific imaging for demonstrating a pars defect and the stage of spondylolysis [2]
- Magnetic Resonance Imaging (MRI) can detect the stage of pars defect and thereby assist with clinical decision making regarding conservative or surgical management[2]. MRI's can also detect subtle bone stress reactions, helping with early diagnosis and treatment[2]. MRI has the benefit of avoiding radiation exposure.
It has been argued that imaging may not be necessary as it rarely changes the management of spondylolysis[15].The following patient characteristics can assist with ruling out spondylolysis without imaging (if 2/3 are absent, there is 88% sensitivity to help rule out active spondylolysis[15]:
- Male sex
- Pain with extension
- Difference between active and resting pain
Outcome Measures[edit | edit source]
- Numeric pain rating scale (NPRS)
- Roland Morris disability questionnaire (RMDQ)
- Oswestry disability index (ODI)
- Pain self-efficacy questionnaire (PSEQ)
- The patient-specific functional scale (PSFS)
Lumbar Spondylolysis In Extension Related Sport[edit | edit source]
Cricket[edit | edit source]
A 2019 literature review looking into the incidence of pars interarticularis defects in sporting athletes found that cricket players had the second highest incidence of pars interarticularis abnormalities (31.97%) when compared with other sports, with the majority occurring in the lumbar spine [16].
In cricket, a bowler will throw the ball at least six times to complete an over and will typically be bowling for up to 50 overs throughout a 4 day test match, which involves repeated hyperextension and rotational movements of the lumbar spine. The prevalence of lumbar vertebral stress injuries amongst cricket bowlers is estimated to be between 11%-67%[17]. Injuries can occur bilaterally or unilaterally. Most unilateral lesions occur contralateral to the bowling arm[17] .
Previous research has also focused on the asymmetry of the quadratus lumborum muscle in cricketers. The main role of the quadratus lumborum is to extend, side flex and stabilise the lumbar spine. A study involving English and Welsh professional cricketers found that bowlers with a quadratus lumborum asymmetry of >25% have a 58% probability of developing a pars interarticularis defect compared to a 4% probability in those who had an asymmetry of <5% [18].
Various bowling styles exist in cricket, but the mixed action (a combination of front-on and side-on bowling actions) is associated with 89% of lumbar stress injuries in bowlers[17]. Spikes in training load also increases the likelihood of injury 3-4 weeks after the spike[17].
Gymnastics[edit | edit source]
Gymnastics is a sport that combines dance, speed, the agility of ornamental jumps and the flexibility of ballet [19]. Spinal injuries are accountable for 17.2% of all injuries within Olympic gymnastics, with spondylolysis accounting for a large portion of this percentage although varying between level of participation and gender [19]. In the competitive elite population, larger studies have shown that the prevalence is about 16%, including both male and female athletes [19]. Spondylolysis accounts for 47% of all lumbar pain among gymnasts [19].
Gymnastics utilizes many unique and diverse positions while traveling at high velocities to perform stunts such as somersaults and dismounts, putting large amount of forces through the axial spine. Along with these large forces, athletes are put into positions such as hyperextension which puts a great amount of pressure on the posterior aspects of the lumbar vertebra, e.g. when performing a flip or when trying to maintain a specific pose. Athletes are also forced into hyperextension when vaulting and landing, applying excessive stress on the vertebra [19].
Tennis[edit | edit source]
A 2019 literature review on spondylolysis found that elite tennis players have an incidence rate of 40% in contrast to the 1.1% of the non-athletic population [16]. A retrospective cohort study demonstrated a 12.9% risk of developing a stress fracture during a two year period for elite tennis players with a 16% incidence in the pars interarticularis [20] .
In the youth, another study of young tennis players found that 80% of reported spondylolysis cases were at L5. Amongst the young tennis players the mean age of reported spondylolysis cases was 14.8 years of age [21]. Further support was found in a 2014 study that performed MRI’s on 98 asymptomatic junior elite tennis players with a mean age of 18 years old and found 41 of players had pars defects with 93% occurring at the L5 level [22].
Tennis is a largely one sided sport, with common fast movements of flexion and extension of the trunk in the sagittal and frontal planes in addition to the rotational movements. Competitive adult tennis players spend several years training to reach professional status, which involves repetitive and strenuous training during the developmental stage of the body. As a result it leaves them at an increased risk of developing overuse injuries such as spondylolysis. In tennis, the specific actions that cause overloading of the posterior arch of the vertebrae are hyperextension when serving and the combined movement of extension with rotation when returning with the forehand. These movements are used to generate power to strike the ball. Whilst performing a tennis serve, the lumbar spine experiences lateral flexion forces 8 times greater than those faced during running [23].
During a serve, a player will perform extension of their spine which causes compression of the lumbar spine, however, dependent on the serve other forces can factor in to apply torsion to the lumbar region. For example when performing a topspin serve, lumbar extension is combined with rotation and lateral flexion which puts a greater amount of torsion through the lumbar spine. The coupled movement of lumbar extension, rotation and lateral flexion, combined with the ground reaction force from rear leg drive in the serve, puts up to 10 times body weight through the lower trunk. This has been suggested as a potential mechanism for abdominal tissue strain and low back injuries in adolescent players.
When performing a tennis stroke, the stance of a player can also have an effect on the forces which go through the lower back. An open forehand stance where the trunk is facing the net can lead to increased incidence of spondylolysis in the lower back. This is a result of rapid anteversion (medial hip rotation) and lumbar hyperextension during a stroke [21]. The more open the stance, the more likely the lumbar pars interarticularis is being loaded on all levels rather than other parts of the body such as the knee or thoracic levels of the spine.
Management/Interventions[edit | edit source]
Conservative Management[edit | edit source]
Conservative management typically consists of cessation or modification of sport, combined with bracing and physiotherapy[5]. It has been shown to have good functional outcomes with excellent return to sport rates for athletes at any level.[24]
Cessation from sport consists of complete rest from sport for 2 weeks up to 6 months[5]. During this time bracing can be considered as a complementary treatment technique. Existing literature shows that management that includes bracing, activity modification and cessation from sport may be the best initial therapy[5]. Athletic activities may be gradually resumed as pain subsides, with particular emphasis placed on avoidance of pain eliciting manoeuvres, particularly hyperextension [25].
The main purpose of bracing is to limit spinal mobilisation and stress on the pars interarticularis. Research does however suggest that patients improve clinically with rest, regardless of bracing[5]. The current recommendation is to use bracing when rest alone fails to alleviate symptoms, and bracing should be progressively discontinued once the patient is asymptomatic regardless of radiographic bony union [26].
Surgical Management[edit | edit source]
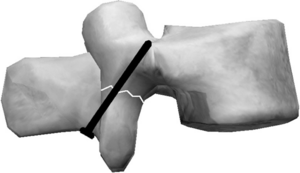
Surgery is usually only considered as an alternative management route to conservative management if there is no progress after at least 6 months[5][27]. For surgical management there are 2 main types of procedures, namely the Buck and Scott procedures. The Buck procedure is designed specifically to repair a defect in the pars interarticularis. The technique involves bone grafts to fill the pars defect followed by screws inserted into the superior articular processes bilaterally. These screws are altered such that they accommodate a hook, which hangs over the lamina, which is later secured by a lock nut. The Buck procedure is the predominant operative method with the Scott procedure, as well as modifications of this procedure, used less often [25].
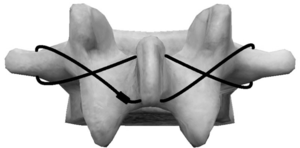
The Scott technique involves a wire passing through the transverse processes of the vertebrae which is tightened around the spinous processes to supplement autologous bone graft repair by providing compression and stabilization of the bony defect [25].
Postoperative rehabilitative care would include protection of the surgical site until wound closure (bracing is typically surgeon dependent) and analgesia. Physiotherapy and re-education on proper biomechanics with an emphasis on posture and sleeping positioning are also given once the surgical wound is healed. An integral part of the postoperative rehabilitative care of athletes is a graded return to sports protocol consisting of education on proper biomechanics followed by the gradual progression to sport specific activities as tolerated [6].
Physiotherapy Management[edit | edit source]
Physiotherapy management focuses on reducing pain levels as well as optimising physical function through the use of specific stabilisation, strengthening and range of motion exercises. The main goal of physiotherapy management is to promote normal movement patterns which are pain free.
Initially, a period of rest is needed to settle down symptoms and promote additional blood flow in order to speed up pars interarticularis healing. This is usually followed by months of physiotherapy training, incorporating a ‘return to play’ stage towards the end of rehabilitation.
During rehabilitation, introducing exercises which focus on improving pelvic control and stability of the core muscles is important [5]. Exercises should focus on strengthening the stabilisers around the spine (abdominals, gluteal muslces, spinal extensors), while limiting the range of extension movement, as well as hip muscle elongation[5][2]:
- Stretching of the hip flexors and hamstrings
- Dynamic core strengthening focusing on the obliques, transverse abdominis, gluteals and pelvic floor[28]
- Once pain free - strengthening of the lumbar spine extensors, multifidus and quadratus lumborum, avoiding end range extension[28]
- Sport specific exercises once bony healing is evident on imaging
Static Stretches[edit | edit source]
Spinal Stabilisation[edit | edit source]
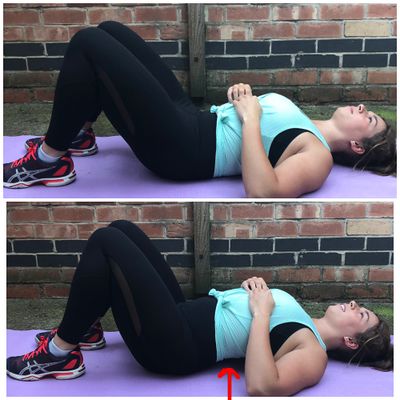
- Rectus abdominis training
- Pelvic tilt control
Complementary Treatments[edit | edit source]
The following treatments can be used throughout rehabilitation to help reduce pain symptoms, although the evidence is lacking [6]:
- Thermotherapy
- NSAIDS
- Epidural Steroid Injections
- Massage
- Cognitive Behavioural Therapy (CBT)
Biopsychosocial Considerations[edit | edit source]
Injuries in athletes can have detrimental effects on their psychological state, particularly with chronic injuries. A lot of athletes will experience the fear of being released by their clubs, especially at an elite level where they have a lot of financial responsibility. This, on top of the frustration of not playing can have adverse effects in which a physiotherapist will try and combat.
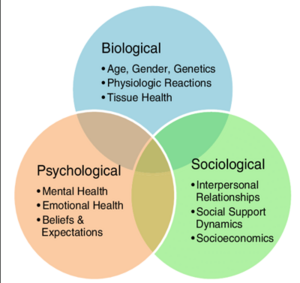
The biopsychosocial model was developed by George Engel in 1977 and is widely recognised as one of the main models used in psychology, medicine and health care today [29]. The model takes into consideration the patient’s biological, psychological and social factors during treatment. A physiotherapist may use this holistic approach to aim to address the mental challenges an athlete faces. Previous research has shown that psychological factors can influence the rehabilitation process of an athlete and can prolong the return to play [30] [31]. Therefore, obtaining as much information from the patient as possible during initial assessment is very important.
Return To Play[edit | edit source]
The time frame for return to play varies depending on the severity of the spondylolysis and the management approach. The mean time period for return to play after conservative management is 4.6 months, and 6.8 months for surgical management[24] This means the return to play time period can last from 2-8 months. Different sports have specific areas to target with regard to rehabilitation, please see below for some considerations.
| Tennis | Cricket | Gymnastics |
|---|---|---|
| Equipment modifications | Video analysis of bowling technique | Monitor technique |
| Technique and movement monitoring | Modifications to reduce trunk side flexion | Monitor load on spine |
| Monitor external load including serve count and training loads | Monitor symptoms | Monitor symptoms |
| Sport specific activites/exercises | Maintain core stability and strength | Maintain core stability and strength |
Clinical Bottom-line[edit | edit source]
Athletes that participate in extension related sports are more at risk of developing Spondylolysis due to the high amount of hyperextension and rotational movements. There is no gold standard for treatment but conservative management should be the first line of action. Moreover, bracing has little effect on outcomes during rehabilitation but can help manage the condition. Surgical treatment is commonly seen as a last resort to help rehabilitation if ineffective after 6 months of conservative treatment.
Despite the poor association between pain and injury, most research on the impact of spondylolysis focuses on pain. It is important to not only rely on pain for clinical decision making, but to consider various other factors, including potential consequences, physical performance, patient's mental health and goals[17].
Also see:
Spondylolysis in Young Athletes
Resources[edit | edit source]
Rehabilitation Guidelines for Lumbar Spondylolysis - UW Health
References[edit | edit source]
- ↑ Lumbar Spondylolysis. Contemporary Spine Surgery. 2012. 13(7), p.8.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 2.12 2.13 Debnath UK. Lumbar spondylolysis-Current concepts review. Journal of Clinical Orthopaedics and Trauma. 2021 Oct 1;21:101535.
- ↑ Gray's Anatomy: Anatomy of the Human Body. Basic Human Anatomy. Annals of Internal Medicine.1967. 66(2), p.462.
- ↑ Chosa, E., Totoribe, K., & Tajima, N. A biomechanical study of lumbar spondylolysis based on a three-dimensional finite element method. Journal of Orthopaedic Research. 2004; 22(1), 158–163
- ↑ 5.00 5.01 5.02 5.03 5.04 5.05 5.06 5.07 5.08 5.09 5.10 5.11 5.12 5.13 5.14 5.15 5.16 5.17 5.18 5.19 5.20 5.21 5.22 5.23 5.24 5.25 Lawrence KJ, Elser T, Stromberg R. Lumbar spondylolysis in the adolescent athlete. Physical Therapy in Sport. 2016 Jul 1;20:56-60.
- ↑ 6.0 6.1 6.2 6.3 McCleary, M. and Congeni, J. Current Concepts in the Diagnosis and Treatment of Spondylolysis in Young Athletes. Current Sports Medicine Reports. 2007; 6(1), pp.62-66.
- ↑ 7.0 7.1 7.2 Kalichman, L., Kim, D., Li, L., Guermazi, A., Berkin, V. and Hunter, D. Spondylolysis and Spondylolisthesis. Spine. 2009; 34(2), pp.199-205.
- ↑ Sakai, T., Sairyo, K., Suzue, N., Kosaka, H. and Yasui, N. Incidence and etiology of lumbar spondylolysis: review of the literature. Journal of Orthopaedic Science. 2010; 15(3), pp.281-288.
- ↑ Sairyo, K., Katoh, S., Sasa, T., Yasui, N., Goel, V., Vadapalli, S., Masuda, A., Biyani, A. and Ebraheim, N. Athletes with Unilateral Spondylolysis are at Risk of Stress Fracture at the Contralateral Pedicle and Pars Interarticularis: A Clinical and Biomechanical Study. The American Journal of Sports Medicine. 2005; 33(4), pp.583-590.
- ↑ Wiltse, L. L., Newman, P., & Macnab, I. Classification of Spondyloisis and Spondylolisthesis. Clinical orthopaedics and related research. 1976; 117, 23–29.
- ↑ 11.0 11.1 Koslosky E, Gendelberg D. Classification in brief: the Meyerding classification system of spondylolisthesis. Clinical orthopaedics and related research. 2020 May;478(5):1125.
- ↑ 12.0 12.1 Alqarni, A., Schneiders, A., Cook, C. and Hendrick, P. Clinical tests to diagnose lumbar spondylolysis and spondylolisthesis: A systematic review. Physical Therapy in Sport. 2015; 16(3), pp.268-275.
- ↑ Masci, L., Pike, J., Malara, F., Phillips, B., Bennell, K., Brukner, P., Standaert, C. and Micheli, L. Use of the one-legged hyperextension test and magnetic resonance imaging in the diagnosis of active spondylolysis. British Journal of Sports Medicine. 2006; 40(11), pp.940-946.
- ↑ Syrmou, E., Tsitsopoulous, P. and Marinopoulos, D. Spondylolysis. Orthopaedic Nursing. 2007; 26(2), pp.112-113.
- ↑ 15.0 15.1 Therriault T, Rospert A, Selhorst M, Fischer A. Development of a preliminary multivariable diagnostic prediction model for identifying active spondylolysis in young athletes with low back pain. Physical Therapy in Sport. 2020 Sep 1;45:1-6.
- ↑ 16.0 16.1 Tawfik, S., Phan, K., Mobbs, R. and Rao, P. The Incidence of Pars Interarticularis Defects in Athletes. Global Spine Journal. 2019; p.219256821882369.
- ↑ 17.0 17.1 17.2 17.3 17.4 Johnson M, Ferreira M, Hush J. Lumbar vertebral stress injuries in fast bowlers: a review of prevalence and risk factors. Physical Therapy in Sport. 2012 Feb 1;13(1):45-52.
- ↑ Ranson, C., Kerslake, R., Burnett, A., Batt, M. and Abdi, S. Magnetic resonance imaging of the lumbar spine in asymptomatic professional fast bowlers in cricket. The Journal of Bone and Joint Surgery. British volume. 2005; 87-B(8), pp.1111-1116.
- ↑ 19.0 19.1 19.2 19.3 19.4 Mohriak, R., Vargas Silva, P., Trandafilov, M., Martins, D., Wajchenberg, M., Cohen, M. and Puertas, E. Spondylolysis and Spondylolisthesis in Young Gymnasts. Revista Brasileira de Ortopedia (English Edition). 2010; 45(1), pp.79-83.
- ↑ Maquirriain, J. The incidence and distribution of stress fractures in elite tennis players * Commentary. British Journal of Sports Medicine. 2006; 40(5), pp.454-459.
- ↑ 21.0 21.1 Ruiz-Cotorro, A. Spondylolysis in young tennis players. British Journal of Sports Medicine. 2006; 40(5), pp.441-446.
- ↑ Rajeswaran, G., Turner, M., Gissane, C. and Healy, J. MRI findings in the lumbar spines of asymptomatic elite junior tennis players. Skeletal Radiology. 2014; 43(7), pp.925-932.
- ↑ Campbell, A., Straker, L., O’Sullivan, P., Elliott, B. and Reid, M. Lumbar Loading in the Elite Adolescent Tennis Serve. Medicine & Science in Sports & Exercise. 2013; 45(8), pp.1562-1568.
- ↑ 24.0 24.1 Grazina R, Andrade R, Santos FL, Marinhas J, Pereira R, Bastos R, Espregueira-Mendes J. Return to play after conservative and surgical treatment in athletes with spondylolysis: A systematic review. Physical Therapy in Sport. 2019 May 1;37:34-43.
- ↑ 25.0 25.1 25.2 Panteliadis, P., Nagra, N., Edwards, K., Behrbalk, E. and Boszczyk, B. Athletic Population with Spondylolysis: Review of Outcomes following Surgical Repair or Conservative Management. Global Spine Journal. 2016; 6(6), pp.615-625.
- ↑ Bouras, T. and Korovessis, P. Management of spondylolysis and low-grade spondylolisthesis in fine athletes. A comprehensive review. European Journal of Orthopaedic Surgery & Traumatology. 2014;25(S1), pp.167-175.
- ↑ Chung CC, Shimer AL. Lumbosacral spondylolysis and spondylolisthesis. Clinics in Sports Medicine. 2021 Jul 1;40(3):471-90.
- ↑ 28.0 28.1 McNeely ML, Torrance G, Magee DJ. A systematic review of physiotherapy for spondylolysis and spondylolisthesis. Manual therapy. 2003 May 1;8(2):80-91.
- ↑ Engel, George L. (8 April 1977). "The need for a new medical model: a challenge for biomedicine". Science. 196(4286): 129–36. doi:10.1126/science.847460. PMID 847460.
- ↑ Ivarsson, A., Tranaeus, U., Johnson, U. and Stenling, A. (2017). Negative psychological responses of injury and rehabilitation adherence effects on return to play in competitive athletes: a systematic review and meta-analysis. Open Access Journal of Sports Medicine, Volume 8, pp.27-32.
- ↑ Putukian, M. (2015). The psychological response to injury in student athletes: a narrative review with a focus on mental health. British Journal of Sports Medicine, 50(3), pp.145-148.