Coma
Original Editor - Lucinda hampton
Top Contributors - Lucinda hampton and Kim Jackson
Introduction[edit | edit source]
Coma is widely encountered throughout health care settings and may occur in the context of a variety of different acute neurological disorders.[1]
A coma is a prolonged state of unconsciousness. During a coma, a person is unresponsive to their environment[2]. The person is alive and looks like they are sleeping, but unlike in a deep sleep, the person cannot be awakened by any stimulation, including pain.
- Causes of coma range from easily correctable metabolic abnormalities to catastrophic life-threatening mass lesions.
- Coma is usually a transitory state though it may last for an indefinite or even prolonged period.[3][2]
- Comas are one of the Disorders of Consciousness
| Wakefulness | Awareness | |
|---|---|---|
| Coma | - | - |
| Vegetative State | + to ++ | - |
| Minimally Conscious State | + to ++ | + |
| Emerged from Minimally Conscious State | ++ | ++ |
Pathophysiology[edit | edit source]
The accepted pathophysiology of a coma involves neuronal dysfunction from a decrease in the supply of glucose or oxygen to the brain. A myriad of etiologies may lead to essential substrate disruption with diffuse central nervous system (CNS) dysfunction and coma as the extreme clinical condition. [3]
Causes[edit | edit source]
More than 50% of comas are related to head trauma or disturbances in the brain's circulatory system.[2]
Causes are many and include:
- Brain injuries caused by an accident or violence. Additionally people can be put into a medically induced coma with medicines. This helps their brain to keep functioning after an injury and saves the patient from feeling extreme pain[4].
- Structural brain disorders eg subdural or epidural traumatic hematomas, stroke, venous thrombosis, tumors, acute hydrocephalus, raised intracranial pressure, anoxic brain injury, or brainstem strokes may all cause altered mental status or coma.
- Common toxic or metabolic causes include hypoglycemia, hyperglycemia, excessive alcohol intake, medication overdose, illicit drug use.
- Less common metabolic causes include hepatic encephalopathy, hyponatremia, hypernatremia, hypercalcemia, endocrine abnormalities.
- Primary central nervous system infections eg meningitis or encephalitis (relatively uncommon)
- Seizure[3][4]
Evaluation[edit | edit source]
Initial evaluation of the comatose patient should always include assessment with intervention as necessary of the airway, breathing, and circulatory conditions (A,B,C's). Recording of the neurologic examination and can be roughly quantified by the Glasgow Coma Scale.
Simplistically, the treatment of a coma is treatment of conditions that lead to coma. These patients may require care of many organ systems and an interprofessional team approach is essential[3].
Neurological examination is the most commonly used management tool for patients with prolonged coma, followed by EEG (either intermittent or continuous monitoring), and neuroimaging (head computed tomography,magnetic resonance imaging [MRI]).[1]
Functional MRI shows promise as a candidate prognostication method in acutely comatose patients following severe brain injury. However, further research is needed before this technique becomes appropriate for clinical practice[5].
Treatment[edit | edit source]
Determination of the serum glucose is recommended for all patients with altered mental status.
Naloxone should be considered in patients with elements of a narcotic overdose eg respiratory rate, small pupils, or altered mental status.
If a readily reversible of coma is not discovered, further evaluation is needed. Further neuroimaging is encouraged if history, physical, and stat laboratory results do not determine a treatment path.
Thiamine should be administered to individuals at risk for poor nutrition eg alcoholics, patients with chronic malabsorptive states.
Cerebral perfusion pressure maintenance (by preserving the mean arterial pressure) is the key to the management strategy. Continuation of supportive supportive care with airway protection and blood pressure is necessary.[3]
Needs[edit | edit source]
A person in coma require complex care and some of the needs might include:
- Postural management programme preventing deformities, contractures and pressure sores including muscle tone management through positioning, splinting, mobilising, sitting in alternative seating systems
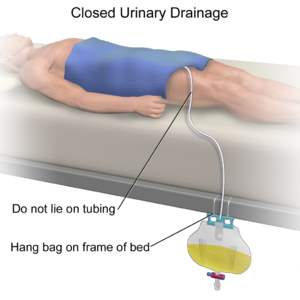
- Bladder and bowel management
- Respiratory care including secretion management, like suctioning, tracheostomy management
- PEG Feeding
- Management of infections like urinary tract infection, chest infection
- Management or prevention of medical and neurological complications like seizures[6].
After the acute period in emergency and intensive care, treatments is not that high-tech. To be kept alive the person requires good basic care (eg turning and changing position to manage skin integrity), a feeding tube, intermittent antibiotics for infections, joint and muscle range of movements to prevent contractures. and perhaps some ongoing mechanical ventilation support (such as oxygen at night)[4].
Physiotherapy[edit | edit source]
Physiotherapy is an important intervention that prevents and mitigates the adverse effects of prolonged bed rest and mechanical ventilation during critical illness. Rehabilitation delivered by the physiotherapist is tailored to patient needs and depends on the conscious state, psychological status and physical strength of the patient. It incorporates any active and passive therapy that promotes movement and includes mobilisation. Early progressive physiotherapy, with a focus on mobility and walking whilst ventilated, is essential in minimising functional decline. [7]
Prognosis[edit | edit source]
In some instances, a person who comes out of a coma can remember what happened to them and are able to resume their normal activities. Others require therapy to re-learn basic tasks and functions, eg tying their shoes, eating with a fork, talking and learning how to walk again. It is possible for people who have been in a coma to make progress and improve their quality of life
Common discharge options for comatose patients who survive hospitalization are long-term acute care hospitals, skilled nursing facilities and acute rehabilitation facilities, or discharged home with assistive services (the minority).[1]
- Patients with reversible causes of coma, eg hypoglycemia, may be discharged after the appropriate intervention.
- Patients with persistent coma need hospital admission with ongoing monitoring, supportive care, and targeted care to the underlying cause of coma.
- Prognosis is difficult and may become clear only after a period of observation[3].
Time to Rethink?[edit | edit source]
Generally, most patients at a hospital do come out of a coma. Typically, a coma does not last more than a few days or couple of weeks. In some rare cases, a person might stay in a coma for several weeks, months or even years. In many countries it has become routine to deliver life-prolonging treatments indefinitely. The vast majority of comatose patients continue to be kept alive via hydration and nutrition delivered through a feeding tube, often for decades. Is this always in their best interest and why do the majority of these people continue to receive this treatment? Possible reasons include
- Loved ones believe that the patient would have wanted ongoing treatment regardless of their level of consciousness or prognosis.
- Loved ones members may be hoping for a “miracle” recovery or are simply not yet ready to let go of a loved one.
- Beliefs of clinicians or care home staff that determine what happens.
- Inertia and maintenance of the status quo.
In cases where people do not recover quickly, the families must decide whether to keep their loved one on a ventilator and feeding tube indefinitely, or to remove these aids and allow the person to die.
If the person in question has written up an advanced medical directive the decision is much easier, because family members can simply follow his or her wishes. In the absence of such a directive, the family must carefully consult with doctors to determine what's best for the patient[8].
References[edit | edit source]
- ↑ 1.0 1.1 1.2 Helbok R, Rass V, Beghi E, Bodien YG, Citerio G, Giacino JT, Kondziella D, Mayer SA, Menon D, Sharshar T, Stevens RD. The Curing Coma Campaign International Survey on Coma Epidemiology, Evaluation, and Therapy (COME TOGETHER). Neurocritical Care. 2022 Feb 9:1-3.Available: https://link.springer.com/article/10.1007/s12028-021-01425-8(accessed 19.5.2022)
- ↑ 2.0 2.1 2.2 Web md Coma: Types, Causes, Treatments, Prognosis Available: https://www.webmd.com/brain/coma-types-causes-treatments-prognosis(accessed 19.5.2022)
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 Huff JS, Tadi P. Coma.[Updated 8 July 2021]. StatPearls [Internet]; StatPearls Publishing: Treasure Island, FL, USA. 2021. Available: https://www.ncbi.nlm.nih.gov/books/NBK430722/ (accessed 19.5.2022)
- ↑ 4.0 4.1 4.2 health direct Coma Available: https://www.healthdirect.gov.au/coma (accessed 19.5.2022)
- ↑ Bruni T, Graham M, Norton L, et al Informed consent for functional MRI research on comatose patients following severe brain injury: balancing the social benefits of research against patient autonomy Journal of Medical Ethics 2019;45:299-303.Available: https://jme.bmj.com/content/45/5/299 (accessed 19.5.2022)
- ↑ Disorders of Consciousness
- ↑ Physiotherapists role in ICU
- ↑ How stuff works How comas work Available: https://science.howstuffworks.com/life/inside-the-mind/human-brain/coma4.htm (accessed 20.5.2022)