Parkinson's - Clinical Presentation: Difference between revisions
No edit summary |
No edit summary |
||
| Line 40: | Line 40: | ||
|- | |- | ||
|{{#ev:youtube|n_mGGir-NgU|300}}<ref>Jen Rodig. Parkinson's Disease. Available from: http://www.youtube.com/watch?v=n_mGGir-NgU [last accessed 29/09/16] </ref> | |{{#ev:youtube|n_mGGir-NgU|300}}<ref>Jen Rodig. Parkinson's Disease. Available from: http://www.youtube.com/watch?v=n_mGGir-NgU [last accessed 29/09/16] </ref> | ||
|{{#ev:youtube|cxHpFWKIfGw|300}} | |{{#ev:youtube|cxHpFWKIfGw|300}}} | ||
<br> | <br> | ||
Revision as of 09:26, 20 April 2019
Original Editor - Bhanu Ramaswamy as part of the APPDE Project
Top Contributors - Wendy Walker, Kim Jackson, Mariam Hashem, Rachael Lowe, Laura Ritchie, Jess Bell, Tarina van der Stockt, Admin, Tony Lowe, Evan Thomas and Naomi O'Reilly
Basal Ganglia Function[edit | edit source]
- Pre-movement planning and preparation (putting plans into actions )
- Initiation of movement
- Sequencing and timing of movement
- Maintaining cortically selected movement amplitude i.e. the frontal cortex is involved in the choice of movement, after which the basal ganglia takes over and communicates with the other areas of the brain. The scale of a required movement is then calibrated the through sensorimotor integration. For example, a person may start to walk with normal step length but if amplitude is incorrectly executed, their steps soon become shorten, progressing to a shuffling gait.
Basal Ganglia Dysfunction[edit | edit source]
Basal ganglia dysfunction affects the automatic (involuntary) nature of our movements. This includes:
- Impaired performance of well-learnt motor skills and movement sequences
- Problems maintaining sufficient movement amplitude
- Difficulty in performing more than one task simultaneously (dual-tasking)
- Difficulty in shifting motor and cognitive sets
- Slower mental processing
- Perseveration (repetition) in thought and action
For a person to perform activities of daily living, the basal ganglia need to be working properly. Impairment affects both mental and physical agility as described by motor and non-motor symptoms.
Clinical Presentation[edit | edit source]
Parkinson's was primarily thought to have motor symptoms only and the non-motor symptoms symptoms were managed separately.
The main motor (movement) symptoms of Parkinson’s are:
- Tremor (involuntary shaking of parts of the body)
- Rigidity (experienced as muscle stiffness)
- Bradykinesia (experienced as slow movement)
| [1] | }
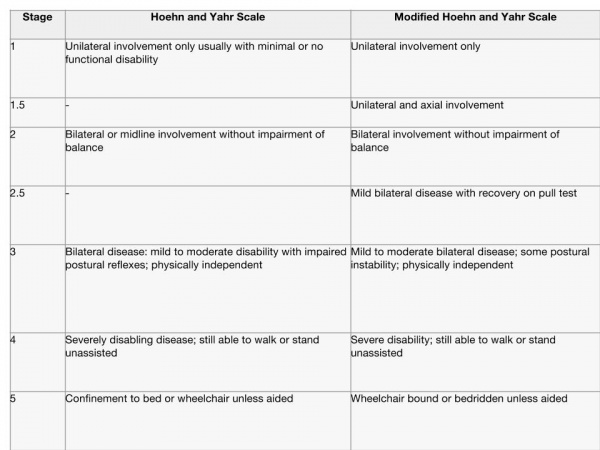
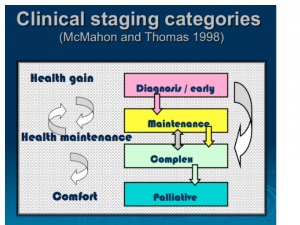
Progression of Parkinson's Disease[edit | edit source]Hoehn and Yahr Scale[edit | edit source]The Hoehn and Yahr scale is commonly used to describe how the motor symptoms of Parkinson’s progress. The original scale was published in a 1967 article by Melvin Yahr and Margaret Hoehn, and included stages 1 to 5[2]. Since then, a modified Hoehn and Yahr scale has been proposed with the addition of stages 1.5 and 2.5 to help describe the intermediate course of the disease. As noted in the H&Y scale, at diagnosis, these signs are usually unilateral, but they become bilateral as the condition progresses. Later in the course of the Parkinson’s additional signs may be present including postural instability (e.g. tendency to fall backwards after a sharp pull from the examiner - the ‘pull test’) and orthostatic hypotension (OH). MacMahon and Thomas Scale[edit | edit source]MacMahon and Thomas (1998) have provided a clinical staging classification[3]. The model is based on four stages of progression from a state of gaining best health, through to the requirement of support and comfort - diagnosis, maintenance, complex and palliative. Unlike the H and Y scale, there is more fluidity with this model, allowing for periods when the person might deteriorate during an illness, whether related to Parkinson’s or not e.g. chest infection, rehabilitation, post fall and fracture, but regains prior ability on recovery.
Non-motor Symptoms[edit | edit source]Non-dopaminergic and non-motor symptoms often present before diagnosis of Parkinson’s, and almost inevitably emerge as the condition progresses. They often dominate the clinical picture of advanced Parkinson's, contributing to disability, impaired quality of life, and shortened life expectancy. Non-motor symptoms are often inadequately treated despite increased attention on the recognition and quantification of symptoms. Commonly experienced non-motor symptoms include:
As these can be improved with available treatments, it is important to elicit from the individual whether they have any such (or other) symptoms; this can be done using the Non-motor symptoms questionnaire Rochester et al (2013) provide an extremely useful table detailing key diagnostic criteria of various movement disorders that help us assess for and recognize and common features in differing conditions. Resources[edit | edit source]
Related pages[edit | edit source]
Read for Credit[edit | edit source]
References[edit | edit source]
|