Hip Dislocation: Difference between revisions
No edit summary |
No edit summary |
||
| Line 6: | Line 6: | ||
== Introduction == | == Introduction == | ||
Hip dislocations are relatively rare, and may be congenital or acquired. Hip dislocation can be classified as: | Hip dislocations are relatively rare, and may be congenital or acquired. The native hip joint (as opposed to prosthetic hip) is inherently stable and needs a huge amount of force to cause dislocation, such as in a motor vehicle accidents.<ref name=":6">Masiewicz S, Mabrouk A, Johnson DE. [https://www.ncbi.nlm.nih.gov/books/NBK459319/ Posterior hip dislocation].Available:https://www.ncbi.nlm.nih.gov/books/NBK459319/ (accessed 7.1.2023)</ref> Hip dislocation can be classified as: | ||
# Posterior dislocation (most common ~85%) | # Posterior dislocation (most common ~85%). Caused by combined forces of: hip flexion, adduction, and internal rotation. | ||
# Anterior dislocation (~10%) | # Anterior dislocation (~10%). Caused by combined forces of : hyper-abduction with the extension.<ref name=":6" /> | ||
# Central dislocation (always occurring with [[Acetabulum Fracture]])<ref name=":5">Radiopedia [https://radiopaedia.org/articles/hip-dislocation Hip dislocation] Available:https://radiopaedia.org/articles/hip-dislocation (accessed 7.1.2023)</ref> | # Central dislocation (always occurring with [[Acetabulum Fracture]])<ref name=":5">Radiopedia [https://radiopaedia.org/articles/hip-dislocation Hip dislocation] Available:https://radiopaedia.org/articles/hip-dislocation (accessed 7.1.2023)</ref> | ||
== Etiology == | == Etiology == | ||
Acquired | '''Acquired Dislocation''': Motor vehicle collisions accounting for >50% of dislocations.<ref name=":5" /> Another common mechanism is falling from a height. Hip dislocations are thus rarely isolated, and often goes together with other injuries or fractures. With hip dislocations, the soft tissue around the hip, such as the muscles, ligaments and labrum are also damaged. Neural injuries may also be present. Fractures to the acetabulum and femur head is most commonly associated with traumatic hip dislocations. | ||
Congenital | [[Total Hip Replacement|Total hip replacement]] (THR) dislocation is a complication of THR usually occurring due to patient noncomplicance with [[Hip Precautions|post-operative precautions]], implant malposition, or soft-tissue deficiency. This type of dislocation normally caused by less trauma, usually falls or turning, moving into the contra-indicated positions, and putting stress on the capsule that was cut to do the replacement surgery..<ref>Orthobullets [https://www.orthobullets.com/recon/5012/tha-dislocation THA Dislocation] Available:https://www.orthobullets.com/recon/5012/tha-dislocation (accessed 7.1.2022)</ref><ref name=":5" /> | ||
'''Congenital Hip Dislocation''' have been appraised and are now viewed as part of the spectrum of [[Developmental dysplasia of the hip (DDH)|developmental dysplasia of the hip.]] See link for information on this. | |||
{| border="0" cellspacing="1" cellpadding="1" | {| border="0" cellspacing="1" cellpadding="1" | ||
|- | |- | ||
| Line 22: | Line 24: | ||
|{{#ev:youtube|watch?v=BLZXlVnqLs0}} | |{{#ev:youtube|watch?v=BLZXlVnqLs0}} | ||
|}<br> | |}<br> | ||
=== Characteristics === | === Characteristics === | ||
The following patients characteristics leads to an increased risk of developing a hip dislocation: <ref name=":0">Van der Grinten M, Verhaar JA. [https://repub.eur.nl/pub/15627/ Luxatie van totaleheupprothese; risicofactoren en behandeling.] Nederlands tijdschrift voor geneeskunde. 2003:286-90.</ref> | The following patients characteristics leads to an increased risk of developing a hip dislocation: <ref name=":0">Van der Grinten M, Verhaar JA. [https://repub.eur.nl/pub/15627/ Luxatie van totaleheupprothese; risicofactoren en behandeling.] Nederlands tijdschrift voor geneeskunde. 2003:286-90.</ref> | ||
| Line 39: | Line 39: | ||
* Chronic hip instability<ref name=":1">Hung NN. [http://chinhhinhnhitw.vn/wp-content/uploads/2018/05/Full-text-5.pdf Traumatic hip dislocation in children.] Journal of Pediatric Orthopaedics B 2012;21(6):542-51.</ref> | * Chronic hip instability<ref name=":1">Hung NN. [http://chinhhinhnhitw.vn/wp-content/uploads/2018/05/Full-text-5.pdf Traumatic hip dislocation in children.] Journal of Pediatric Orthopaedics B 2012;21(6):542-51.</ref> | ||
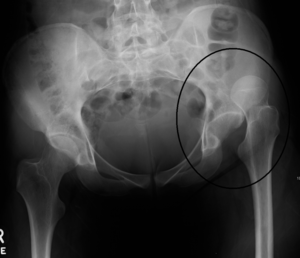
[[File:Hip dislocation.png|none|thumb|A superiorly dislocated hip post trauma]] | [[File:Hip dislocation.png|none|thumb|A superiorly dislocated hip post trauma]] | ||
<br> | <br> | ||
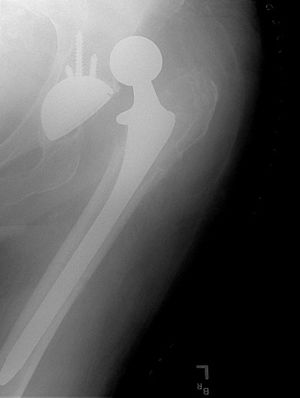
[[File:Dislocated THR.jpg|none|thumb|Dislocated total hip replacement]] | [[File:Dislocated THR.jpg|none|thumb|Dislocated total hip replacement]] | ||
| Line 66: | Line 57: | ||
** Inability to walk as a result of pain and swelling | ** Inability to walk as a result of pain and swelling | ||
* Traumatic hip dislocations:<ref name=":3" /> | * Traumatic hip dislocations:<ref name=":3">Lima LC, Nascimento RA, Almeida VM, Façanha Filho FA. [https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4108698/#:~:text=The%20present%20study%20showed%20that,was%20posterior%20dislocation%20(93.3%25). Epidemiology of traumatic hip dislocation in patients treated in Ceará, Brazil.] Acta ortopedica brasileira 2014;22(3):151-4.</ref> | ||
** Male > female | ** Male > female | ||
** Posterior > anterior | ** Posterior > anterior | ||
| Line 85: | Line 76: | ||
== Complications == | == Complications == | ||
Immediate:<ref name=":4" /> | Immediate:<ref name=":4">Ortho Info. Developmental Dislocation (Dysplasia) of the Hip (DDH). Available from: https://orthoinfo.aaos.org/en/diseases--conditions/developmental-dislocation-dysplasia-of-the-hip-ddh (accessed 08/08/2020).</ref> | ||
* Associated soft tissue injuries | * Associated soft tissue injuries | ||
* Neural injuries, especially to the sciatic nerve in posterior dislocations (present in about 10% of traumatic dislocations) | * Neural injuries, especially to the sciatic nerve in posterior dislocations (present in about 10% of traumatic dislocations) | ||
| Line 102: | Line 93: | ||
== Medical Management == | == Medical Management == | ||
==== Surgery ==== | ==== Surgery ==== | ||
| Line 119: | Line 103: | ||
{{#ev:youtube|watch?v=2dT1r_U7LQ8}} | {{#ev:youtube|watch?v=2dT1r_U7LQ8}} | ||
==== Non-surgical ==== | ==== Non-surgical ==== | ||
Closed relocation of the hip is done by a traction force performed in the opposite direction of the dislocation, with the hip in 90° flexion. This should preferably be done under general or regional anesthesia and muscle relaxation to prevent greater damage to cartilage and soft tissue.<ref name=":2" /> It may also be done in under anaesthetics in theater.<ref name=":4" /> After the relocation, the stability of the hip should be tested very carefully. A period of bed rest might be recommended depending on the stability of the hip and the extent of the soft tissue injuries. | Closed relocation of the hip is done by a traction force performed in the opposite direction of the dislocation, with the hip in 90° flexion. This should preferably be done under general or regional anesthesia and muscle relaxation to prevent greater damage to cartilage and soft tissue.<ref name=":2">Medscape. Hip dislocation. Available from: https://emedicine.medscape.com/article/86930-overview (accessed 09/08/2020).</ref> It may also be done in under anaesthetics in theater.<ref name=":4" /> After the relocation, the stability of the hip should be tested very carefully. A period of bed rest might be recommended depending on the stability of the hip and the extent of the soft tissue injuries. | ||
==== Surgical ==== | ==== Surgical ==== | ||
Revision as of 03:28, 7 January 2023
Original Editor - Annelies Noppe
Top Contributors - Annelies Noppe, Leana Louw, Lucinda hampton, Kim Jackson, Lokiru Paul, WikiSysop, Vidya Acharya, Anas Mohamed and Kirenga Bamurange Liliane
Introduction[edit | edit source]
Hip dislocations are relatively rare, and may be congenital or acquired. The native hip joint (as opposed to prosthetic hip) is inherently stable and needs a huge amount of force to cause dislocation, such as in a motor vehicle accidents.[1] Hip dislocation can be classified as:
- Posterior dislocation (most common ~85%). Caused by combined forces of: hip flexion, adduction, and internal rotation.
- Anterior dislocation (~10%). Caused by combined forces of : hyper-abduction with the extension.[1]
- Central dislocation (always occurring with Acetabulum Fracture)[2]
Etiology[edit | edit source]
Acquired Dislocation: Motor vehicle collisions accounting for >50% of dislocations.[2] Another common mechanism is falling from a height. Hip dislocations are thus rarely isolated, and often goes together with other injuries or fractures. With hip dislocations, the soft tissue around the hip, such as the muscles, ligaments and labrum are also damaged. Neural injuries may also be present. Fractures to the acetabulum and femur head is most commonly associated with traumatic hip dislocations.
Total hip replacement (THR) dislocation is a complication of THR usually occurring due to patient noncomplicance with post-operative precautions, implant malposition, or soft-tissue deficiency. This type of dislocation normally caused by less trauma, usually falls or turning, moving into the contra-indicated positions, and putting stress on the capsule that was cut to do the replacement surgery..[3][2]
Congenital Hip Dislocation have been appraised and are now viewed as part of the spectrum of developmental dysplasia of the hip. See link for information on this.
Characteristics[edit | edit source]
The following patients characteristics leads to an increased risk of developing a hip dislocation: [4]
- Female > male
- Alcohol abuse
- Various pre-operative disorders
- Older age:
- Decreased muscle mass reduces the stress on the hip prosthesis and decreases the natural protection against hip dislocation
- Increased risk of falling due to compromised balance
- Neuromuscular dysfunction associated with old age - e.g. neuropathy or cerebrovascular accident
- Cognitive impairments
- Great dexterity
- Poor follow instructions
- Increased tendency to fall
- Chronic hip instability[5]
Characteristics/Clinical Presentation[edit | edit source]
- Pain:[5]
- Severe pain is the most common symptom. With the separation of the femur head from the acetabulum, surrounding muscles and tendons can be damaged as well. Subsequent knee injuries might also be present.
- Radiating knee pain
- Swelling
- Leg length discrepancy and deformity:
- In most of the cases is the affected leg will appear shortened and the hip joint deformed
- Hip immobility:[5]
- Reduced hip range of motion
- Inability to walk as a result of pain and swelling
- Traumatic hip dislocations:[6]
- Male > female
- Posterior > anterior
- Neurological fallout (mainly in the sciatic nerve distribution) may be present
Differential Diagnosis[edit | edit source]
- Hip dysplasia
- Hip sublaxation
Diagnostic Procedures[edit | edit source]
- X-rays: AP pelvis and lateral
- To confirm dislocation and successful relocation
- Assess for associated fractures
- Progression of hip dysplasia
- CT:
- To rule out concomitant injuries in traumatic dislocations (e.g. acetabulum or femur head fractures)
- Clearance of lumbar spine[7]
Complications[edit | edit source]
Immediate:[8]
- Associated soft tissue injuries
- Neural injuries, especially to the sciatic nerve in posterior dislocations (present in about 10% of traumatic dislocations)
- Fractures, mostly to the femur head or acetabulum (mostly posterior wall)
Long term:[6]
- Avascular necrosis:
- Incidence of 1.7-40% is reducable to 0-10% if relocation is done within 6 hours post traumatic dislocation[9]
- Post-traumatic osteoarthritis
- Chronic dislocations
- Leg length discrepancy
Examination[edit | edit source]
- Observation:
- Hip dislocations can often be diagnosed by just looking at the hip. The hip will be shortenend, in external rotation, slight flexion and adduction in the more common posterior dislocations.
- Imaging (as explained above)
- Neurological assessment (to determine any associated neural injuries)
Medical Management[edit | edit source]
Surgery[edit | edit source]
Surgery is indicated for failed conservative management.
Surgery entails release the of the adductor longus muscle, lengthening the psoas tendon, and insertion of a Kirschner wire. This results in marked improvement in hip function and prevents complications later in life.[5] Total hip replacement surgery is an option later in life, when marked functional limitation and pain is present.
Acquired hip dislocation[edit | edit source]
A dislocated hip should be relocated as soon as possible, as the complication risk of avascular necrosis, neural damage and subsequent dislocations increases with the time between the dislocation and relocation.[6] The Allis maneuver is normally the reduction method of choice for posterior dislocations[6]
Non-surgical[edit | edit source]
Closed relocation of the hip is done by a traction force performed in the opposite direction of the dislocation, with the hip in 90° flexion. This should preferably be done under general or regional anesthesia and muscle relaxation to prevent greater damage to cartilage and soft tissue.[10] It may also be done in under anaesthetics in theater.[8] After the relocation, the stability of the hip should be tested very carefully. A period of bed rest might be recommended depending on the stability of the hip and the extent of the soft tissue injuries.
Surgical[edit | edit source]
Indications:
- Failed conservative relocation
- Instability following conservative relocation
- Associated fractures of the femur head or acetabulum
- Loose bone fragments in joint space after relocation
Hip arthroscopy can be used to evaluate intra-articular fractures and chondral injuries and to remove intra-articular fragments, Hip replacement surgery can also be considered if optimal stability is not achieved with relocation and fixation of the associated injuries.[6] Dislocation following hip replacement surgery might indicate revision surgery to ensure the stability of the hip in the long run.
Open reduction indications:[6]
- Used with challenging relocations or if any obstructions (e.g. loose fragments/soft tissue) is limiting closed reduction
- Deteriorating neurological signs following closed reduction (especially sciatic nerve function following posterior dislocation)
- Cases with proximal femur fractures, where manipulation of the leg is contra-indicated
Physiotherapy Management[edit | edit source]
It is important to take the time frames for soft tissue healing (and bone healing in cases with associated fractures) into consideration with rehabilitation following a hip dislocation. The orthopaedic surgeon will give guidance on weight bearing restrictions that might be present following the medical management of the hip. Full rehabilitation following hip dislocation can take 2-3 months.[8]
- Gait re-education: Initially with mobility assistive devices (walking frame/crutches) to limit weight bearing, and progression thereof
- Improve hip range of motion: Especially extension in children after the use of a brace/splint/harness that kept the hip in flexion
- Strengthening of muscles around the hip, with special focus on hip stabilizers
- Stretching
- Joint mobilization
- Graded return to activity/sport
See rehabilitation resources below.
Resources[edit | edit source]
- Rehabilitation Guidelines for Surgical Hip Dislocation
- Surgical Hip Dislocation Rehabilitation Protocol
- Hip Surgical Dislocation Guidelines
Clinical Bottom Line[edit | edit source]
Hip dislocations are classified into congenial and acquired. Congenital hip dislocations, or developmental hip dysplasia can be successfully managed in children, but might cause problems later in life, when total hip replacement surgery might be indicated to improve function, leg length discrepancies and pain. Acquired, or traumatic hip dislocations are medical emergencies, and treatment should be sought as soon as possible. Relocation should ideally occur within 6 hours from the dislocation, in order to reduce complications. Traumatic dislocations are reduced either open or closed, and open or arthroscopy surgery might be indicated in cases with associated fractures. Physiotherapy plays an important role in the rehabilitation following a hip dislocation, in order to get the patients back to their previous level of function, and to prevent further dislocations.
References[edit | edit source]
- ↑ 1.0 1.1 Masiewicz S, Mabrouk A, Johnson DE. Posterior hip dislocation.Available:https://www.ncbi.nlm.nih.gov/books/NBK459319/ (accessed 7.1.2023)
- ↑ 2.0 2.1 2.2 Radiopedia Hip dislocation Available:https://radiopaedia.org/articles/hip-dislocation (accessed 7.1.2023)
- ↑ Orthobullets THA Dislocation Available:https://www.orthobullets.com/recon/5012/tha-dislocation (accessed 7.1.2022)
- ↑ Van der Grinten M, Verhaar JA. Luxatie van totaleheupprothese; risicofactoren en behandeling. Nederlands tijdschrift voor geneeskunde. 2003:286-90.
- ↑ 5.0 5.1 5.2 5.3 Hung NN. Traumatic hip dislocation in children. Journal of Pediatric Orthopaedics B 2012;21(6):542-51.
- ↑ 6.0 6.1 6.2 6.3 6.4 6.5 Lima LC, Nascimento RA, Almeida VM, Façanha Filho FA. Epidemiology of traumatic hip dislocation in patients treated in Ceará, Brazil. Acta ortopedica brasileira 2014;22(3):151-4.
- ↑ Larson DE. Gezin en gezondheid. Cambium BV:Zeewolde, 1995.
- ↑ 8.0 8.1 8.2 Ortho Info. Developmental Dislocation (Dysplasia) of the Hip (DDH). Available from: https://orthoinfo.aaos.org/en/diseases--conditions/developmental-dislocation-dysplasia-of-the-hip-ddh (accessed 08/08/2020).
- ↑ Bucholz R, Heckman JD. Rockwood e Green fraturas em adultos. In: Rockwood e Green fraturas em adultos, 2006: pp. 2263-2263.
- ↑ Medscape. Hip dislocation. Available from: https://emedicine.medscape.com/article/86930-overview (accessed 09/08/2020).