Spinal Malignancy
Introduction[edit | edit source]
Between one and five percent of all musculoskeletal presentations in primary care are due to serious pathology and these rates are expected to increase as cancer survival rates improve.[1]
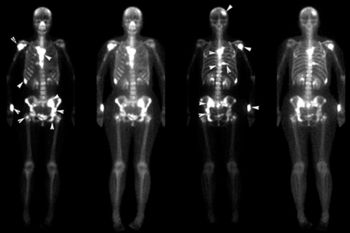
Metastatic bone disease (MBD) is the second most common serious spinal pathology - a vertebral fracture is the most common.[1] Bone is a common location for metastases (i.e. cancers that have spread from primary cancer to a new site in the body).[2]
The spine is often one of the earliest areas affected, particularly in patients who have a history of breast and prostate cancer.[1] Bone metastases can be caused by "most types of malignancies".[3] The five types of cancer that are most likely to spread to the spine are:[4]
- Breast
- Prostate
- Lung
- Renal (Kidney)
- Thyroid
It is not entirely understood how MBD spreads, but its propensity for the spine is considered to be due to haematogenous spread via the venous or arterial pathways.[1]
The distribution of metastases in the spine varies:[1]
- 70% occur in the thoracic spine
- 20% occur in the lumbar spine
- 10% occur in the cervical spine
NB while 70% of metastases occur in the thoracic spine, the patient may not describe thoracic pain.[4]
Identifying Spinal Malignancy[edit | edit source]
Despite relatively low presentation rates, serious pathology, including spinal malignancy, should be considered as a differential diagnosis when a patient presents with back pain.[5]
- Identifying serious pathology as the cause of musculoskeletal pain is highly complex.[2] Symptoms that are caused by spinal metastases are often "non-specific".[6]
- Red flags have traditionally been used to help identify these conditions and a “history of cancer” and “strong clinical suspicion” have empirical evidence of high diagnostic accuracy for malignancy.[7]
- While red flags can indicate serious pathology, red flags signs / symptoms are considered unreliable[8] and generally have poor diagnostic accuracy.[9] There is a lack of consistency in guidelines over which red flags should be used[10] or when health professionals should act.[5] This has led to inconsistency in the management of patients when there is suspicion of serious pathology.[2]
It is vital to identify patients with spinal malignancy as early as possible as this results in much better outcomes.[5] This is discussed in more detail here, but it is known that a patient with a single metastasis or just BMD will do better than a patient with multiple metastases.[4] However, if a patient presents with signs of Metastatic Spinal Cord Compression (MSCC) (eg paralysis, bladder/bowel changes, band-like pain), they will likely have a poor prognosis as this condition indicates late-stage metastatic cancer.[4] Van Tol et al.[11] note that delays in treatment for spinal malignancy are associated with:
- Unfavourable surgical outcomes, such as increased blood loss, longer surgery times, more complications
- Unfavourable clinical outcomes, including poor functional performance, reduced quality of life, and decreased survival
The mnemonic RED FLAGS can be used to detect early warning signs of metastatic spinal cord compression.[12]
- R: Referred back pain that is multi-segmental or band like
- E: Escalating pain that responds poorly to treatment including medication
- D: Different character or site to previous symptoms
- F: Funny feelings, odd sensations or heavy legs
- L: Lying flat increases back pain
- A: Agonising pain-causing anguish or despair
- G: Gait disturbance, unsteadiness especially on stairs (not just a limp)
- S: Sleep grossly disturbed due to pain being worse at night[12]
Risk of Developing Metastatic Bone Disease[edit | edit source]
- While a history of cancer increases the index of suspicion[10][2] of spinal malignancy, not all patients with a history of cancer will go on to develop MBD.
- Approximately 30% of all patients who have one of the 5 primary cancers listed above will go on to have metastases.[2]
- History alone will not necessarily trigger an immediate referral.[4]
- Clinicians should not be reassured just because a patient does not have a history of cancer as MSCC is the first sign of metastases in around 25% of individuals who do not have a primary cancer diagnosis.[2]
Clinical Framework[edit | edit source]
Because of the complexities in identifying patients with serious pathology, Finucane and colleagues (2020) have developed a framework which provides a way for health professionals to screen for spinal pathology that can mimic musculoskeletal spinal conditions.[2]
The Decision Tool for Early Identification of Serious Spinal Pathology has 3 steps which will be discussed in detail below. These are:
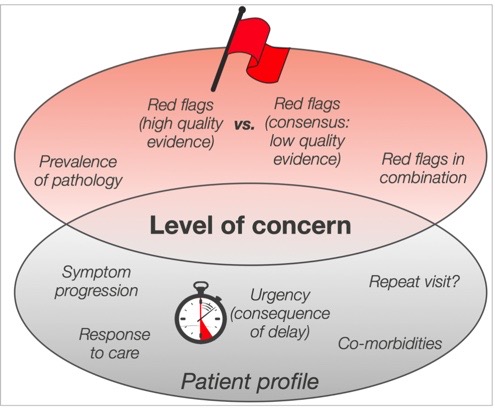
- Determine your level of concern/index of suspicion - this would include considering evidence to support red flags and the patient’s specific health determinants (age, sex etc) (see Figure 1)
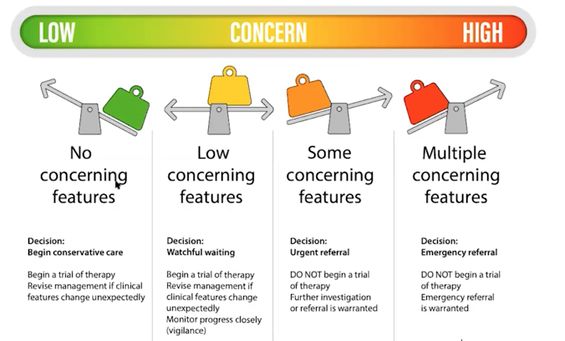
- Decide on clinical action - based on the level of concern (see Figure 2)
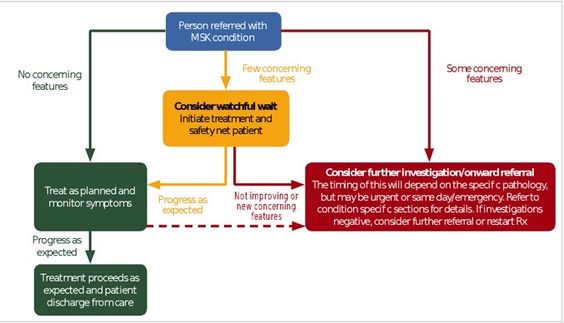
- Consider the pathway for emergency/urgent referral (see Figure 3)
Determine Level of Concern[edit | edit source]
As shown in Figure 1 is important when assessing patients to consider other elements that may or may not be occurring rather than acting on one factor alone (such as a history of cancer alone). Factors to consider include:
- Low-risk tumours
- Ovarian cancer is, for example, less likely to metastasise.
- Tumours with low risk of secondary dissemination
- A low-grade breast cancer (eg grade 1) will have a lower risk of dissemination than a grade 3 or 4 cancer (which refers to a late-stage tumour).
- High-risk tumours, particularly those with a predilection for bone and in patients with high grade or large size, aggressive tumours.
- Type of tumour
- In breast cancer, an oestrogen receptor negative tumour will metastasise in the first 2-5 years of diagnosis whereas an oestrogen positive tumour will more likely metastasise 10-20 years post-diagnosis.[4]
It should be noted that not all patients will know exactly what type of cancer they have had. But they will usually know certain details such as the location (breast, prostate etc) and what surgery they have had (radical, lymph node removal) and which types of treatments (radiotherapy or chemotherapy).[4]
Thus, it can be surmised from this information that if a patient has had radical surgery, lymph node removal and chemotherapy or radiotherapy, they have likely had an aggressive late-stage tumour (grade 3 or 4). This would raise the index of suspicion of metastatic bone disease when exploring the origin of their back pain.[4]
In addition to history, it is important to consider factors such as symptom level and progression. Questions to consider include:
- How is the patient progressing?
- Has s/he responded to treatments?
- Does s/he have any other co-morbidities that are concerning?
These questions will help to determine your level of concern for this patient.[4]
Decide on Clinical Action[edit | edit source]
Based on the level of concern, a management decision will be made. As seen in Figure 2, the framework provides a colour-coded system to help the practitioner decide what management option is best when a patient presents with features that may be suggestive of spinal malignancy. Figure 3 also provides a tool which enables clinicians to consider the pathway for emergency or urgent referral. It is important to note that the pathway is moveable and flexible - a patient can move between pathways.[2]
Use of the pathway may be as follows:
- Green - the patient has a history of cancer, but no concerning features - their back pain is very familiar and they are not concerned about it. Consider conservative treatments, but re-evaluate each session and be cognizant of the fact that things do change.
- Yellow - some concerning features - a history of cancer with that seems to be progressively worsening. Can consider monitoring for 2-3 weeks to see how they respond to treatment. However, metastases tend to wax and wane, so symptoms can also go up and down. Thus, it may appear that a treatment is working, but this will need to be assessed over time to be certain of improvement and aware if symptoms worsen. Worsening symptoms after a period of improvement would heighten suspicion of malignancy. It is important to discuss any concerns you have with your patients so that they also know what signs/symptoms of which to be aware. There needs to be a clear plan for these patients to follow if their symptoms change and they deteriorate.
- Orange - a patient may have a history of cancer and some concerning features - they are reporting that they are experiencing pain unlike their usual back pain. They may be developing neurology. This would indicate the need to arrange an urgent referral for investigation - ie an MRI scan of the whole spine as pain is not always at the level of the metastases.
- Red - Concerning features require immediate action (ie emergency/same day). This would include signs of MSCC. - eg gait disturbance, band-like pain - if the patient loses the ability to walk, they will have a very poor outcome.[4][2]
Other Signs/Symptoms to Consider[edit | edit source]
In addition to history, there are other red flag symptoms that may highlight increased risk, including weight loss and being systematically unwell. These two features often occur in the late stages of metastases, but physiotherapists need to be able to try to pick up concerning features as early as possible. Thus, it is important to explore red flag features in detail.[4]
- Weight loss - is it unexplained or have they been dieting/exercising lately?
- Night pain is common with back pain, so concerning features to look out for include a patient describes pain that prevents them from returning to sleep, pacing at night, sitting up in a chair or being unable to lie flat due to extreme pain
- Patients will report progressively worsening pain and neurology (remembering that symptoms can wax and wane).
- The description of band-like pain is associated with metastatic spinal cord compression
- There is the possibility of spinal tenderness on palpation at the location of the metastasis[4]
Conclusion[edit | edit source]
- It is important to consider a history of cancer when treating musculoskeletal back pain, but this should not be the sole consideration.
- A past history of cancer will raise your index of suspicion, but this in itself is not enough to send them for investigations.
- It is reasonable to consider a trial of therapy first with regular evaluation.
- It is important to inform patents about what signs/symptoms they need to look out for - this will ensure they come back for re-assessment in a timely manner.
- You must follow up with any patient you are concerned about.
- Malignancy should be considered as a differential diagnosis.
- Discuss any concerns you have about a patient with a colleague/support network[4]
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 Finucane L, Greenhalgh S, Selfe J. Which red flags aid the early detection of metastatic bone disease in back pain? Physiotherapy Practice and Research. 2017;38(2): 73-77.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 2.7 2.8 Finucane LM, Mercer C, Greenhalgh SM, Boissonnault WG, Pool-Goudzwaard AL, Beneciuk JM et al. International framework for red flags for potential serious pathologies. J Orthop Sports Phys Ther. 2020; epub: 1-23.
- ↑ Tsukamoto S, Kido A, Tanaka Y, Facchini G, Peta G, Rossi G, Mavrogenis AF. Current overview of treatment for metastatic bone disease. Curr Oncol. 2021 Aug 29;28(5):3347-72.
- ↑ 4.00 4.01 4.02 4.03 4.04 4.05 4.06 4.07 4.08 4.09 4.10 4.11 4.12 Finucane L. Spinal Malignancy Course. Plus 2020.
- ↑ 5.0 5.1 5.2 Finucane L. An Introduction to Red Flags in Serious Pathology. Plus 2020.
- ↑ Van Tol FR, Massier JRA, Frederix GWJ, Öner FC, Verkooijen HM, Verlaan JJ. Costs associated with timely and delayed surgical treatment of spinal metastases. Global Spine J. 2022 Oct;12(8):1661-6.
- ↑ Verhagen AP, Downie A, Maher CG, Koes BW. Most red flags for malignancy in low back pain guidelines lack empirical support: a systematic review. Pain. 2017;158(10):1860-8.
- ↑ Paling C. The complex problem of identifying serious pathology in Musculoskeletal care: Managing clinical risk during the COVID pandemic and beyond. Musculoskelet Sci Pract. 2021 Aug;54:102379.
- ↑ Premkumar A, Godfrey W, Gottschalk MB, Boden SD. Red Flags for Low Back Pain Are Not Always Really Red. J Bone Jt Surg. 2018;100(5):368–74.
- ↑ 10.0 10.1 Verhagen AP, Downie A, Popal N, Maher C, Koes BW. Red flags presented in current low back pain guidelines: a review. European Spine Journal. 2016 Sep 1;25(9):2788-802.
- ↑ Van Tol FR, Versteeg AL, Verkooijen HM, Öner FC, Verlaan JJ. Time to surgical treatment for metastatic spinal disease: Identification of delay intervals. Global Spine J. 2021 Feb 18:2192568221994787.
- ↑ 12.0 12.1 The Christie NHS Foundation Trust. The use of red flags to identify serious spinal pathology. Greater Manchester and Cheshire. 2013. Available from https://www.christie.nhs.uk/media/1121/legacymedia-4941-briefing-paper-use-of-red-flags-to-identify-serious-spinal-pathology-updated-jan-2016.pdf (accessed 18 June 2020).