Sacral Insufficiency Fractures
Introduction[edit | edit source]
Sacral insufficiency fractures (SIFs) are a subtype of stress fractures, resulting from normal stress applied to a bone with reduced elasticity.[1][2] Typically, SIFs are associated with an underlying metabolic bone disease condition such as osteoporosis or Paget's disease and are most common in elderly women. [3]
- During the gait, alternating flexion and extension of the lower limbs would impart alternating twisting forces on the pelvis around its lowest transverse axis.
- This effect can be shown in a pretzel-model. When we hold a pretzel in two hands and twist it around its long axis in alternating directions, the pretzel will snap eventually.
- This is what happens clinically with the sacrum during insufficiency fractures.
- In most cases, these fractures run vertically through the ala of the sacrum parallel to the sacroiliac joint[4] Zone 1 Denis classification see R)
- Most frequently with elderly women, whose sacroiliac joint is relatively ankylosed and whose sacrum has been weakened by osteoporosis.
- Under these conditions, the torsional stress which is normally buffered by the sacroiliac Joint will be transferred to the sacrum. Because of the conditions of the weakened sacrum, it fails to buffer the torsional stress and fractures occur.[4]
Clinically Relevant Anatomy[edit | edit source]
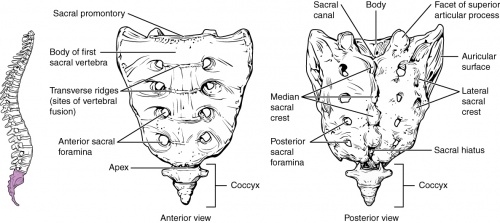
The sacrum is a triangular bone formed by 5 vertebral segments. It is broader on the superior side than on the inferior, and broader on the anterior side than on the posterior side, allowing the sacrum to resist shearing from vertical compression[5] as well as transfer loads from the spinal column to the pelvis. The sacrum articulates superiorly with the fifth lumbar vertebra and inferiorly with the coccyx. The lateral surface of the upper part of the lateral masses (auricular surface) articulates with the ilium.[6]
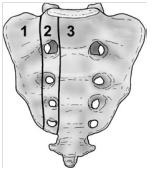
Denis et al classified traumatic sacral fractures by dividing the sacrum into 3 zones.
This classification system is based on the direction, the localisation and the level of the fracture.[5] These traumatic fractures are not directly related to SIFs, but the classification system of Denis is very useful for the description of these SIFs.
- Zone 1: involves the sacral ala (lateral to the sacral foramina). This is the most common area of SIFs.
- Zone 2: involves the sacral (neural) foramina (but the fracture does not enter the central sacral canal). The fractures in this site are associated with unilateral lumbosacral radiculopathies.
- Zone 3: involves the sacral bodies and the transverse central canal.
Epidemiology[edit | edit source]
Current research reports a prevalence rate of approximately 5% of the at-risk patient population. Two-third of patients sustain SIFs atraumatically and frequently both sides are affected.[5] SIF can also occur in the younger population in pregnant women. Other risk factors include:Pelvic radiation
● Steroid-induced osteopenia
● Radiotherapy
● Diabetes mellitus
● Primary biliary cirrhosis
● Rheumatoid arthritis [7]
● Multiple myeloma
● Paget disease
● Renal osteodystrophy [8]
● Hyperparathyroidism
● Corticosteroid medication
● Metastatic disease
● Marrow replacement processes
● Fibrous dysplasia
● Osteogenesis imperfecta
● Osteoporosis
● Osteomalacia
● Development of osteolysis
Clinical Presentation[edit | edit source]
Patients with SIFs usually present reporting vague, non-specific signs and symptoms. Patients will commonly describe problems with walking, pain, and tenderness on palpation over the lower back, hip, groin and/or diffusely over the sacral region, leg weakness and parasymphyseal tenderness [9]. Aggravating factors include weight-bearing activities, especially walking and pain is eased by rest, usually in the supine position. There is no typical 24-hour picture as it is activity-dependent.
On objective examination:
- Slow, antalgic gait
- Trendelenburg test is usually negative
- Sacral tenderness (on lateral compression)
Sacroiliac joint tests are often positive (although not specific for SIFs) - Straight Leg Raise (SLR) is usually normal
- FABER test can be positive indicative of sacroiliac pathology
- A neurological examination is often normal.
Diagnostic investigations to strengthen the diagnosis of SIF are elevated alkaline phosphatase and medical imaging. Plain pelvic radiographs, bone scintigraphy, magnetic resonance imaging (MRI) or computed tomography (CT) can all be used to aid in the diagnosis of SIFs. The research remains unclear for all situations as to which imaging modality is superior to confirm a SIF diagnosis however CT has been shown to be superior to conventional radiography in the assessment of pelvic fractures. [10]
The frequency of undetected sacral fractures is high.[11] SIFs could be considered as a differential diagnosis for osteodegenerative diseases, radiculopathy, spinal stenosis & cauda equina syndrome, particularly if the pathology progression is atypical and/or not responding to treatment.
Medical Management[edit | edit source]
Generally, sacral insufficiency fractures are treated conservatively with relative rest, analgesia and physical therapy. Early ambulation may reduce the complications and significant morbidity and mortality associated with prolonged immobility.
Percutaneous sacroplasty is a variation of percutaneous vertebroplasty. It is an alternative that may provide symptomatic relief and accelerate the recovery. Sacroplasty involves the percutaneous insertion of 1 or more bone needles into the fracture zone of the sacral ala. PMMA (polymethylmethacrylate) cement is then injected in this zone with the aim to treat the lesion and to stabilise the sacrum.[12]
Carina L. Et al. described that CT guidance can improve this procedure.[13] Sacroplasty provides symptom relief including pain relief and functional restoration. The quality of life of the patients is improved and the complications of immobility are avoided. However the longterm results of sacroplasty are not known yet.[14] Further research into the effectiveness of sacroplasty is required.
Physical Therapy Management[edit | edit source]
Early rehabilitation and moderate weight-bearing exercises within the boundaries of pain tolerance are recommended.
- Earlier rehabilitation will stimulate osteoblastic activity and help maintain muscle mass and strength.
- In the early stages of fracture healing, mobilisation can be assisted by the use of support devices such as crutches or walking frames or hydrotherapy which is typically better tolerated by many patients.
- Extracorporal shock wave therapy can also be used. Like the PEMF and the LIPU techniques it stimulates growth factors where the body shock is applied.[6]
References[edit | edit source]
- ↑ Lyders E.M., Whitlow C.T., Baker M.D., Morris P.P., Imaging and treatment of sacral insufficiency fractures (review), Am. J. Neuroradiology 31:201-10, February 2010.
- ↑ Wild A., Jaeger M., Haak H., Mehdian S.H., Sacral insufficiency fracture, an unsuspected cause of low-back pain in elderly women. Arch. Orthop. Trauma. Surg (2002) 122:58-60.
- ↑ Bong-Jin H., Kim J.T., Chung D.S., Sacral insufficiency fracture, most overlooked cause of lumbosacral pain. J. Kor. Neurosurg. Soc. September 2008, 44 (3): 166-169.
- ↑ 4.0 4.1 Cohen, Steven P. MD; Sacroiliac Joint Pain : A Comprehensive Review of Anatomy, Diagnosis and Treatment; Official Journal of the International Anesthesia Research Society; 2005
- ↑ 5.0 5.1 5.2 A. Vleeming; The sacroiliac joint: an overview of its anatomy, function and potential clinical implications; Journal of Anatomy; 221; 537-567; 2012
- ↑ 6.0 6.1 Tsiridis E., Upadhyay N., Giannoudis P.V., Sacral insufficiency fractures: current concepts of management. Osteoporos. Int. (2006) 17: 1716-1725.
- ↑ Dasgupta B., Shah N., Brown H., Gordon T.E., Tanqueray A.B., Mellor J.A., Sacral insufficiency fractures: an unsuspected cause of low back pain. British Journal of Rheumatology 1998; 37: 789-793.
- ↑ Ayhan AŞKIN et al. ; ATYPICAL SACRAL AND ILIAC BONE INSUFFICIENCY FRACTURES IN A PATIENT RECEIVING LONG-TERM BISPHOSPHONATE THERAPY ; 2015, Cilt 18, Sayı 2, Sayfa(lar) 171-175
- ↑ R Watura et al. ; Sacral insufficiency fractures ; Journal of Orthopaedic Surgery 2007;15(3):339-46 (2B)
- ↑ Eriksson T, Claes Olerud PB, Shalabi A & Hänni M. Low-dose CT of postoperative pelvic fractures: a comparison with radiography.Acta Radiologica. April 17, 2018. https://doi.org/10.1177/0284185118770919
- ↑ Hatgis J, Granville M, Jacobson RE, Berti A. Sacral Insufficiency Fractures: Recognition and Treatment in Patients with Concurrent Lumbar Vertebral Compression Fractures. Muacevic A, Adler JR, eds. Cureus. 2017;9(2):e1008. doi:10.7759/cureus.1008.
- ↑ Bayley E. Et al.; Clinical outcomes of sacroplasty in sacral insufficiency fractures: a review of the literature; Eur Spine J;2009; 18:1266-1271
- ↑ Carina L. ;Percutaneous Sacroplasty for the treatment of sacral insufficiency fractures ;American Journal of Roentgenology ;2005 ;184-6
- ↑ William Pommersheim et al. ;Sacroplasty : A Treatment for Sacral Insufficiency Fractures ;American Journal of Neuroradiology ; 2003 ;24 :1003-1007