Pelvic Organ Prolapse
Original Editor - Laura Ritchie, posting on behalf of Lauren Kalvaitis, MPT Class of 2016 at Western University, project for PT9583
Top Contributors - Laura Ritchie, Temitope Olowoyeye, Kim Jackson, Lucinda hampton, WikiSysop, Vidya Acharya, Chelsea Mclene, Kirenga Bamurange Liliane and Evan Thomas
Introduction[edit | edit source]
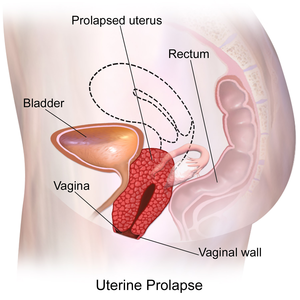
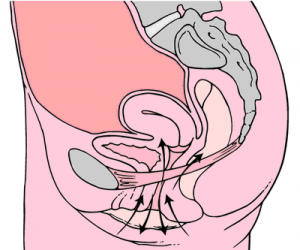
Pelvic organ prolapse (POP) is the herniation of the pelvic organs through the perineum due to weakened pelvic floor muscles and supporting structures. Depending on the pelvic organ involved, POP is further categorized into:
- Anterior compartment containing urinary bladder (cystocele)
- Middle compartment containing uterine or vaginal prolapse (uterus or vagina)
- Posterior compartment containing either the small bowel loops (enterocele) or rectum (rectocele)
POP is a gynecological condition that is very common among multiparous women and mostly postmenopausal women[1] over 50 (affects approximately 50% of women over age 50). Symptoms include fecal or urinary incontinence, uterine prolapse, constipation, or incomplete defecation. POP can negatively impact the patient's body image and sexuality. Although it is generally not life-threatening, it severely impairs an individual's physical and psychological health.[2] Treatments of pelvic prolapse significantly contribute to the healthcare cost in the United States estimated at approximately $300 million from 2005 to 2006.[3] Treatment options vary and are dependent upon the degree of prolapse and symptoms it ranges from non-surgical approaches like Kegel exercise and pessary to various surgical procedures.
Definition/Description[edit | edit source]
Pelvic organ prolapse is the descent of a pelvic organ into or outside of the vaginal canal or anus. It mainly results from pelvic floor dysfunction Pelvic Floor Dysfunction[4] There are several types categorized by the site of descent.
These are:
- Cystocele: prolapse of the bladder into the vagina [5]
- Urethrocele: prolapse of the urethra
- Uterine prolapse [5]
- Vaginal vault prolapse: prolapse of the vagina [6]
- Enterocele: small bowel prolapse
- Rectocele: rectum prolapse [5]
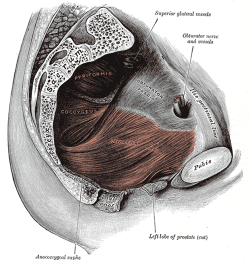
Clinically Relevant Anatomy[edit | edit source]
Please see this page Pelvic Floor Anatomy for a detailed overview of pelvic floor anatomy.
Etiology[edit | edit source]
Pelvic organ prolapse has a multifactorial etiology. It is likely caused by a combination of physiological, anatomical, reproductive, genetic, and lifestyle factors that interact and contribute to dysfunction of the pelvic floor.[6]
Symptoms[edit | edit source]
A variety of symptoms may include:
- Vaginal bulging [7]
- Feeling of pelvic pressure or heaviness [7]
- Pelvic pain [7]
- Urinary Incontinence, fecal incontinence or obstruction [7]
- Altered daily activities, sexual function and quality of life [7]
- Visualization of the prolapsed vaginal[8]
- Bleeding from eroded vaginal mucosa[8][8]
- Constipation[8]
Risk Factors[edit | edit source]
| [9] |
The factors causing pelvic organ prolapse are different between patients.[6] Risk factors include the following:
Primary Pelvic Organ Prolapse
- Pregnancy and labour [5]
- Obesity/BMI [4] [6]
- Respiratory problems involving a chronic, long-term cough [5]
- Cancer of the pelvic organs [5]
- Hysterectomy (surgical removal of the uterus) [5]
- Genetics (possibly) due to weaker connective tissues [5]
- History of vaginal delivery increases the risk 5.56 times [6] [4]
- Hypertension and Diabetes Mellitus combined increase the risk by 1.9 times [4]
- Increased birth weight [4]
- Age [6]
- Parity [6] (i.e. the number of times a woman has given birth to a fetus with a gestational age of greater than or equal to 24 weeks, alive or stillborn) [10]
Pelvic Organ Prolapse Recurrence (after native tissue repair)
- Preoperative stage 3 or 4 pelvic organ prolapse (i.e. a more severe prolapse) [6]
Treatment/Management[edit | edit source]
As prolapse treatment options expand to include more conservative choices, greater awareness and education are needed among women and professionals about these as a first-line treatment and preventive measure (alongside a multi-professional team approach)[11].
Women presenting with prolapse symptoms need to be[11]
- listened to by the health care team
- offered information about treatment choices
- supported to make a decision that is right for them.
Qualitative research developed a conceptual model that explores the experience of living with a POP, and the model indicated that: the physical losses of POP are linked to loss of identity; women conceptualized POP as part of womanhood, and a vicious cycle of taboo, silence, and misunderstanding about POP and its treatment. And further, POP is not taken seriously in healthcare[12].
Treatment for pelvic organ prolapse usually involves either conservative management (for mild prolapse or women who are not good surgical candidates) or surgery. Conservative treatments include pelvic floor muscle training and the use of devices (pessaries). [7]
Physiotherapy[edit | edit source]
Physical therapists play a major role in the nonsurgical management of POP. Along with pessary support, pelvic-floor muscle training (PFMT) is cited in highly credible reviews as a main nonsurgical option for women with POP.[13]
For all the information on retraining these muscles see the physiotherapy section of Pelvic Floor Dysfunction and Kegel's Exercises
In a study by Panman et al in 2016, examining the two-year effects of pelvic floor muscle retraining, it was demonstrated that in women aged 55 and greater with symptomatic mild pelvic organ prolapse, pelvic floor muscle retraining results in a significant decrease in pelvic floor symptoms when compared to watchful waiting (note: statistically significant but below the minimal clinically important difference). Additionally, it was found that pelvic floor muscle retraining was more effective in women who experienced increased pelvic floor symptom distress at baseline. Conversely, the same study found no difference in sexual functioning, quality of life, the function of the pelvic floor muscles, or degree of prolapse.
A randomised control trial[14] compared the effect of intravaginal vibratory stimulation (IVVS) with intravaginal electrical stimulation (IVES) in women with pelvic floor dysfunctions, unable to voluntarily contract the pelvic floor muscles. The results showed improvement with both techniques, with IVVS superior to IVES in improving pelvic floor muscle strength.
Pelvic floor muscle retraining included: (Kegel exercises diagram in illustration)
- Explanation and description of the pelvic floor [7]
- Instruction regarding how to contract and relax pelvic floor muscles [7]
- General exercise program provided, subsequently modified for individual needs [7]
- Taught correct technique for contracting pelvic floor muscles before and during increases in abdominal pressure [7]
- Received information about washroom habits and lifestyle [7]
- If pelvic floor muscles were overactive, focus was on relaxation rather than contraction [7]
- Face-to-face contact with a physiotherapist as well as encouragement to maintain practice at home 3-5 times per week, 2-3 times per day [7]
Differential diagnosis[edit | edit source]
There are some diseases that can mimic the pelvic organ prolapse symptoms that can present as a bulge[15] these are:
- Urogenital atrophy [15]
- Severe irritation of the vaginal mucosa from a Candida or bacterial source[15]
- Large urethral diverticulum [15],[16]
- vaginal wall cyst can present [15], [16]
- Cervical polyps[16]
- Elongation of the cervix[16]
- Tumors of the urethra or bladder[16]
- Skene gland cysts.[16]
Presentations[edit | edit source]
 |
Pelvic Physiotherapy - to Kegel or Not?
This presentation was created by Carolyn Vandyken, a physiotherapist who specializes in the treatment of male and female pelvic dysfunction. She also provides education and mentorship to physiotherapists who are similarly interested in treating these dysfunctions. In the presentation, Carolyn reviews pelvic anatomy, the history of Kegel exercises and what the evidence tells us about when Kegels are and aren't appropriate for our patients. |
References[edit | edit source]
- ↑ Torres-Lacomba, M.; Navarro-Brazález, B.; Yuste-Sánchez, M.J.; Sánchez-Sánchez, B.; Prieto-Gómez, V.; Vergara-Pérez, F. Women’s Experiences with Compliance with Pelvic Floor Home Exercise Therapy and Lifestyle Changes for Pelvic Organ Prolapse Symptoms: A Qualitative Study. J. Pers. Med. 2022, 12, 498. https://doi.org/10.3390/jpm12030498
- ↑ Xicui Long, Yong Hu, Zhenghua Xiong, Chen Li, Wenjiao Jin, Huiming Guo, Juan Zhang, Xuesong Han, Comparison of mood state in severe pelvic organ prolapse patients before and after surgery,Gynecology and Obstetrics ClinicalMedicine,Volume1,Issue4,2021,Pages 220-224,ISSN 2667-1646, https://doi.org/10.1016/j.gocm.2021.11.005.
- ↑ Yoon I, Gupta N. Pelvic Prolapse Imaging. InStatPearls [Internet] 2019 Dec 14. StatPearls Publishing. Available from: https://www.ncbi.nlm.nih.gov/books/NBK551513/ (last accessed 11.1.2020)
- ↑ 4.0 4.1 4.2 4.3 4.4 Isık H, Aynıoglu O, Sahbaz A, Selimoglu R, Timur H, Harma, M. Are hypertension and diabetes mellitus risk factors for pelvic organ prolapse? European Journal of Obstetrics and Gynecology and Reproductive Biology. 2016. 197; 59-62.
- ↑ 5.0 5.1 5.2 5.3 5.4 5.5 5.6 5.7 Iglesia CB, Smithling KR. Pelvic Organ Prolapse. Am Fam Physician. 2017 Aug 1;96(3):179-185. PMID: 28762694.
- ↑ 6.0 6.1 6.2 6.3 6.4 6.5 6.6 6.7 Vergeldt TF, Weemhoff M, Inthout J, and Kluivers KB. Risk factors for pelvic organ prolapse and its recurrence: A systematic review. International Urogynecology Journal Int Urogynecol J. 2015. 26(11); 1559-1573.
- ↑ 7.00 7.01 7.02 7.03 7.04 7.05 7.06 7.07 7.08 7.09 7.10 7.11 7.12 7.13 7.14 Panman C, Wiegersma M, Kollen B, Berger M, Leeuwen YL, Vermeulen K, Dekker J. Two-year effects and cost-effectiveness of pelvic floor muscle training in mild pelvic organ prolapse: A randomised controlled trial in primary care. BJOG: Int J Obstet Gy. 2016 Mar 21. doi: 10.1111/1471-0528.13992.
- ↑ 8.0 8.1 8.2 8.3 Bureau M, Carlson KV. Pelvic organ prolapse: A primer for urologists. Can Urol Assoc J. 2017 Jun;11(6Suppl2):S125-S130. doi: 10.5489/cuaj.4634. PMID: 28616110; PMCID: PMC5461143.
- ↑ the study spot. Uterine Prolapse and Vaginal Prolapse for USMLE. Available from: http://www.youtube.com/watch?v=YBqUV53_QGU [last accessed 02/09/16]
- ↑ Patient. (n.d.). Gravidity and Parity Definitions (Implications in Risk Assessment) | Patient. Retrieved March 30, 2016, from http://patient.info/doctor/gravidity-and-parity-definitions-and-their-implications-in-risk-assessment
- ↑ 11.0 11.1 Abhyankar P, Uny I, Semple K, Wane S, Hagen S, Wilkinson J, Guerrero K, Tincello D, Duncan E, Calveley E, Elders A. Women’s experiences of receiving care for pelvic organ prolapse: a qualitative study. BMC women's health. 2019 Dec;19(1):45. Available from: https://bmcwomenshealth.biomedcentral.com/articles/10.1186/s12905-019-0741-2 (last accessed 11.1.2020)
- ↑ Toye F, Pearl J, Vincent K, Barker K. A qualitative evidence synthesis using meta-ethnography to understand the experience of living with pelvic organ prolapse. International Urogynecology Journal. 2020 Sep 1:1-4.
- ↑ Saunders K. Recent advances in understanding pelvic-floor tissue of women with and without pelvic organ prolapse: considerations for physical therapists. Physical therapy. 2017 Feb 28;97(4):455-63. Available from:https://academic.oup.com/ptj/article/97/4/455/3057463 (last accessed 11.1.2020)
- ↑ Rodrigues MP, Barbosa LJ, Paiva LL, Mallmann S, Sanches PR, Ferreira CF, Ramos JG. Effect of intravaginal vibratory versus electric stimulation on the pelvic floor muscles: A randomized clinical trial. European journal of obstetrics & gynecology and reproductive biology: X. 2019 May 12.
- ↑ 15.0 15.1 15.2 15.3 15.4 Obstetrics and Gynecology Pelvic Organ Prolapse Steve Swift
- ↑ 16.0 16.1 16.2 16.3 16.4 16.5 Aboseif C, Liu P. Pelvic Organ Prolapse. [Updated 2022 Oct 3]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK563229/