Constipation
Definition[edit | edit source]
Chronic constipation is infrequent bowel movements or difficult passage of stools that persists for several weeks or longer.[1]
Etiology[edit | edit source]
The prevalence of chronic constipation in North America 2% to 27%, the percentage varies because of the differing diagnostic criteria used.[2] Constipation may be described as disordered movement of stool through the colon or anorectum. Transit through the proximal gastrointestinal tract is often normal. Slowing of colonic transit may be idiopathic or may be due to secondary causes.
Secondary causes of constipation include:
| Potential causes of Constipation | |
|---|---|
| Neurologic disorders (peripheral) | Diabetes mellitus[3]Aganglionosis (Hirschsprung disease)[4] |
| Neurologic disorders (central) | Multiple Sclerosis[5]
Parkinson's Spinal Cord Injury |
| Non-neurogenic | Anorexia nervosa[6]Pregnancy |
| Idiopathic | Pelvic floor dyssynergia[7][8][9] |
| Other | Irritable Bowel Syndrome[10]
Side-effects of drugs |
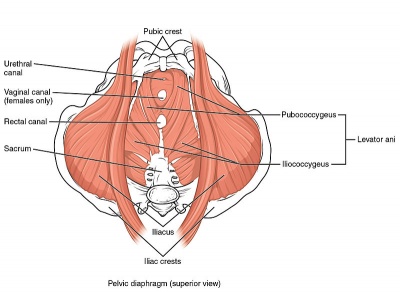
Clinically Relevant Anatomy[edit | edit source]
Please see the page "Pelvic Floor Anatomy," for further details regarding anatomy.
Clinical Presentation[edit | edit source]
An international working committee recommended the following diagnostic criteria (Rome IV) for functional constipation:[11]
- Must include two or more of the following:
- Straining during more than 25 percent of defecations.
- Lumpy or hard stools (Bristol Stool Scale Form 1-2) in more than 25 percent of defecations (figure 1).
- Sensation of incomplete evacuation for more than 25 percent of defecations.
- Sensation of anorectal obstruction/blockage for more than 25 percent of defecations.
- Manual maneuvers to facilitate more than 25 percent of defecations (eg, digital evacuation, support of the pelvic floor).
- Fewer than three spontaneous bowel movements per week.
- Loose stools are rarely present without the use of laxatives
- There are insufficient criteria for IBS. (See "Clinical manifestations and diagnosis of irritable bowel syndrome in adults".)
Although patients with functional constipation may have abdominal pain and/or bloating, they are not the predominant symptoms. - A cross-sectional study in adult women living in a municipality in the interior of northeast Brazil analyzing the relationship between intestinal constipation and functioning showed that women with constipation had reduced cognitive, mobility, self-care, and participation abilities[12].
Management/Interventions[edit | edit source]
Diet[edit | edit source]
A high-fiber diet is a commonly recommended treatment for digestive problems, such as constipation. Most dietary fiber is not digested or absorbed, so it stays within the intestine where it modulates digestion of other foods and affects the consistency of stool. There are two types of fiber that are thought to have benefits: soluble and insoluble fiber.
Soluble fiber consists of a group of substances that is made of carbohydrates and dissolves in water. Examples of foods that contain soluble fiber include fruits, oats, barley, legumes (peas and beans), psyllium, pectin, and wheat dextrin. Insoluble fiber comes from plant cell walls and does not dissolve in water. Examples of foods that contain insoluble fiber include wheat, rye, and other grains.[13] The traditional fiber, wheat bran, is a type of insoluble fiber. Fiber bulks the stool, making it softer and easier to pass. Fiber helps the stool pass regularly, although it is not a laxative.[14]
The recommended amount of dietary fiber is 20 to 35 grams per day. By reading the nutrition label on packaged foods, it is possible to determine the number of grams of dietary fiber per serving.[7] Adding fiber to the diet can have some side effects, such as abdominal bloating or gas. This can sometimes be minimized by starting with a small amount and slowly increasing until stools become softer and more frequent.
Physiotherapist[edit | edit source]
Physiotherapists can implement a "Fiber diary." This can be a useful tool, as it provides both the patient and practitioner with insights into the amount of dietary fiber that is being consumed.
As mentioned above in "Secondary causes of constipation," there can be a number of causes for constipation. Biofeedback can be an extremely useful tool for patients dealing with pelvic floor dyssynergia. Ineffective defecation is associated with a failure to relax, or inappropriate contraction of, the puborectalis and external anal sphincter muscles. This narrows the anorectal angle and increases the pressures of the anal canal so that evacuation is less effective. Relaxation of these muscles involves cortical inhibition of the spinal reflex during defecation; thus, this pattern may represent a conscious or unconscious act. Defecation normally involves the coordinated relaxation of the puborectalis and external anal sphincter muscles, together with increased intra-abdominal pressure and inhibition of colonic segmenting activity. This can be objectively measured through the use of a biofeedback device (ie. electromyography), which the patient can look at to adjust their muscle coordination, and the practitioner can adjust the verbal cueing given.[7][8][9][15][16][17][18]
Physician[edit | edit source]
Physicians may try or prescribe the following options:
Bulk-forming laxatives[edit | edit source]
- Psyllium seed (eg, Metamucil)[19]
- Methylcellulose (eg, Citrucel)
- Calcium polycarbophil (eg, FiberCon)
- Wheat dextrin (eg, Benefiber)
Osmotic agents[edit | edit source]
Stimulant laxatives[edit | edit source]
- Bisacodyl (eg, some forms of Dulcolax)[22]
- Senna (eg, Senokot)
- Sodium picosulfate (eg, Dulcolax drops)
There is no convincing evidence that chronic use of stimulant laxatives causes structural or functional impairment of the colon[23]
In cases of severe constipation or failure of the above options, the following may be prescribed:
- Suppositories
- Disimpaction
Education[edit | edit source]
Patient education involves efforts to reduce dependency on laxatives by emphasizing that daily bowel movements are not the norm or necessary for health, and to increase fluid and fiber intake. Patients should be advised to try to defecate after meals, thereby taking advantage of normal postprandial increases in colonic motility. This is particularly important in the morning when colonic motor activity is highest.
References[edit | edit source]
- ↑ Mayo Clinic. Constipation. Available from: https://www.mayoclinic.org/diseases-conditions/constipation/symptoms-causes/syc-20354253
- ↑ Suares NC, Ford AC. Prevalence of, and risk factors for, chronic idiopathic constipation in the community: systematic review and meta-analysis. The American journal of gastroenterology. 2011 Sep;106(9):1582.
- ↑ He CL, Szurszewski JH, Farrugia G, Soffer EE, Walsh RM, Ferris CD, Program EN. Loss of interstitial cells of cajal and inhibitory innervation in insulin-dependent diabetes. Gastroenterology. 2001 Aug 1;121(2):427-34.
- ↑ Edery P, Lyonnet S, Mulligan LM, Pelet A, Dow E, Abel L, Holder S, Nihoul-Fékété C, Ponder BA, Munnich A. Mutations of the RET proto-oncogene in Hirschsprung's disease. Nature. 1994 Jan;367(6461):378.
- ↑ Hinds JP, Wald A. Colonic and anorectal dysfunction associated with multiple sclerosis. American Journal of Gastroenterology. 1989 Jun 1;84(6).
- ↑ Zipfel S, Sammet I, Rapps N, Herzog W, Herpertz S, Martens U. Gastrointestinal disturbances in eating disorders: clinical and neurobiological aspects. Autonomic Neuroscience. 2006 Oct 30;129(1-2):99-106.
- ↑ 7.0 7.1 7.2 Rao SS, Valestin J, Brown CK, Zimmerman B, Schulze K. Long-term efficacy of biofeedback therapy for dyssynergic defecation: randomized controlled trial. The American journal of gastroenterology. 2010 Apr;105(4):890.
- ↑ 8.0 8.1 Chiarioni G, Whitehead WE, Pezza V, Morelli A, Bassotti G. Biofeedback is superior to laxatives for normal transit constipation due to pelvic floor dyssynergia. Gastroenterology. 2006 Mar 1;130(3):657-64.
- ↑ 9.0 9.1 Rao SS, Valestin JA, Xiang X, Hamdy S, Bradley CS, Zimmerman MB. Home-based versus office-based biofeedback therapy for constipation with dyssynergic defecation: a randomised controlled trial. The Lancet Gastroenterology & Hepatology. 2018 Nov 1;3(11):768-77.
- ↑ Longstreth GF, Thompson WG, Chey WD, Houghton LA, Mearin F, Spiller RC. Functional bowel disorders. Gastroenterology. 2006 Apr 1;130(5):1480-91.
- ↑ Longstreth GF, Thompson WG, Chey WD, Houghton LA, Mearin F, Spiller RC. Functional bowel disorders. Gastroenterology. 2006 Apr 1;130(5):1480-91.
- ↑ Dantas AA, Pereira AR, de Castro SS, de Macedo Dantas TH, Ferreira CW, Barbosa IR, da Câmara SM, de Sousa Dantas D. Is Constipation Associated with Worse Functioning in Adult Women? A Cross-Sectional Study. Journal of Multidisciplinary Healthcare. 2020;13:883.
- ↑ NIH. High-fibre Foods. Available from: https://medlineplus.gov/ency/patientinstructions/000193.htm
- ↑ Suares NC, Ford AC. Systematic review: the effects of fibre in the management of chronic idiopathic constipation. Alimentary pharmacology & therapeutics. 2011 Apr;33(8):895-901.
- ↑ Rao SS, Valestin J, Brown CK, Zimmerman B, Schulze K. Long-term efficacy of biofeedback therapy for dyssynergic defecation: randomized controlled trial. The American journal of gastroenterology. 2010 Apr;105(4):890.
- ↑ Chiarioni G, Whitehead WE, Pezza V, Morelli A, Bassotti G. Biofeedback is superior to laxatives for normal transit constipation due to pelvic floor dyssynergia. Gastroenterology. 2006 Mar 1;130(3):657-64.
- ↑ Rao SS, Valestin JA, Xiang X, Hamdy S, Bradley CS, Zimmerman MB. Home-based versus office-based biofeedback therapy for constipation with dyssynergic defecation: a randomised controlled trial. The Lancet Gastroenterology & Hepatology. 2018 Nov 1;3(11):768-77.
- ↑ Rao SS, Seaton K, Miller M, Brown K, Nygaard I, Stumbo P, Zimmerman B, Schulze K. Randomized controlled trial of biofeedback, sham feedback, and standard therapy for dyssynergic defecation. Clinical Gastroenterology and Hepatology. 2007 Mar 1;5(3):331-8.
- ↑ Ramkumar D, Rao SS. Efficacy and safety of traditional medical therapies for chronic constipation: systematic review. The American journal of gastroenterology. 2005 Apr;100(4):936.
- ↑ DiPalma JA, vB Cleveland M, McGowan J, Herrera JL. A randomized, multicenter, placebo-controlled trial of polyethylene glycol laxative for chronic treatment of chronic constipation. The American journal of gastroenterology. 2007 Jul;102(7):1436.
- ↑ Dupont C, Campagne A, Constant F. Efficacy and safety of a magnesium sulfate–rich natural mineral water for patients with functional constipation. Clinical Gastroenterology and Hepatology. 2014 Aug 1;12(8):1280-7.
- ↑ Kamm MA, Mueller–Lissner S, Wald A, Richter E, Swallow R, Gessner U. Oral bisacodyl is effective and well-tolerated in patients with chronic constipation. Clinical Gastroenterology and Hepatology. 2011 Jul 1;9(7):577-83.
- ↑ Müller-Lissner SA, Kamm MA, Scarpignato C, Wald A. Myths and misconceptions about chronic constipation. The American journal of gastroenterology. 2005 Jan;100(1):232.