Overview of Prostate Cancer
Top Contributors - Stacy Schiurring, Kim Jackson, Lucinda hampton and Jess Bell
Introduction[edit | edit source]
Prostate cancer affects the prostate gland, which is part of the male reproductive system and functions to create seminal fluid.
- In 2020, there were an estimated 1.4 million new cases of prostate cancer and 375,000 prostate cancer-related deaths worldwide[1]
- Prostate cancer was the second most frequent cancer and the fifth leading cause of cancer death among men[1]
- It was the most frequently diagnosed cancer in men in over half of the countries in the world[1]
- Differences in prostate cancer diagnostic practices are most likely the greatest contributor to the worldwide variation in prostate cancer incidence rates[1]
- The majority of men diagnosed with prostate cancer have a slow growing variation of the disease that is non-threatening to their natural life expectancy and can be safely monitored without need for medical intervention[2]
- For those men diagnosed with metastatic prostate cancer, only 28% will survive beyond five years of diagnosis[2]
- The prognosis worsens if the cancer has a chance to spread; metastasis rapidly involves the lymphatic system, lungs, bone marrow, liver or adrenal glands[2]
Providing treatment for prostate cancer is a common entryway into the speciality area of men's health physiotherapy because these patients can be effectively treated without a practitioner having competency in the full scope of men's health skills (i.e. the internal examination and use of real-time ultrasound).[3] Please follow these links to learn more about physiotherapy assessment and treatment of men's health conditions.
Anatomy Review[edit | edit source]
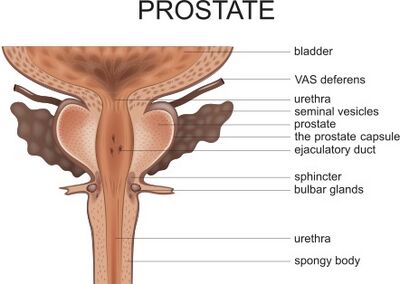
- The prostate gland is situated in the pelvic cavity: below the lower part of the symphysis pubis, above the superior fascia of the urogenital diaphragm, and in front of the rectum.
- The prostate is located below the bladder. It surrounds the urethra. Proximal to the prostate is the internal urethral sphincter, distal to the prostate gland is the external urethral sphincter.[4]
- It can be palpated, especially when enlarged.[4] It is about the size of a walnut.[3]
- The prostate is perforated by both the urethra and the ejaculatory ducts. The ejaculatory ducts open into the prostatic portion of the urethra.[4]
- Arterial supply: internal pudendal, inferior vesical, and middle haemorrhoidal .[4]
- Innervation: receives sympathetic input via the hypogastric nerve and parasympathetic input via the pelvic nerve. The hypogastric and pelvic nerves also provide sensory inputs to the gland.[5]
- The prostate gland is divided into three anatomical lobes: two anterior and one median[2]
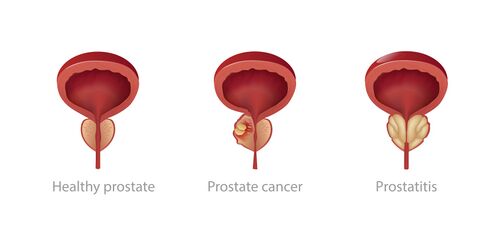
- Knowing the anatomy of the prostate is central to the understanding of both benign and malignant prostatic pathologies; the area in which the pathology originates is a defining characteristic of the three main prostate diseases. The three main diseases of the prostate are:[2]
- Benign prostate hyperplasia (BPH)
- Prostate cancer
- Chronic prostatitis
- Knowing the anatomy of the prostate is central to the understanding of both benign and malignant prostatic pathologies; the area in which the pathology originates is a defining characteristic of the three main prostate diseases. The three main diseases of the prostate are:[2]
Characteristics/Clinical Presentation[edit | edit source]
Early prostate cancer may be asymptomatic. Thus, routine screenings of prostate cancer are commonly done on asymptomatic men.
Clinical signs and symptoms:
- Difficulty starting urination
- Weak or interrupted flow of urine
- Frequent urination, especially at night
- Difficulty emptying the bladder completely
- Pain or burning during urination
- Blood in the urine or semen
- Pain in the back, hips, or pelvis that doesn’t go away
- Painful ejaculation or orgasm[3]
It is important to note that these signs and symptoms may also be present with other non-cancerous prostate-related disease conditions such as BPH or prostatitis. If a patient presents with the above symptoms, referral to a medical doctor or urologist is urgently recommended for proper diagnosis.
Cancer is one condition that can affect the prostate and cause enlargement of the gland. When the prostate enlarges, it can compress the urethra and cause difficulties with urine flow. An enlarged prostate does not always lead to a diagnosis of prostate cancer. Rather, it suggests that further testing in indicated for a proper differential diagnosis.[3]
If a patient reports symptoms of sexual dysfunction, it is important to ask about the timeline of their issues. It is of greater concern if the sexual dysfunction issue involves orgasm and ejaculation, and has occurred within the previous few months. A referral should be made for differential diagnosis.[3]
Tumour Staging[edit | edit source]
- The diagnosis of prostate cancer is established via a biopsy of the prostate gland.
- A small piece of the prostate gland is removed and examined under a microscope for cancer cells. If cancer cells are found, then a Gleason score will be determined from the biopsy. A Gleason score indicates how likely the cancer is to spread. It ranges from 2–10. The lower the score, the less likely it is that the cancer will spread.
- False-negative results often occur; therefore, multiple biopsies may be done before prostate cancer can be detected and confirmed.
What is a Gleason score? Please watch this short video for an explanation of this cancer rating system.
Stage I: Cancer cannot be felt during a digital rectal exam, but it may be found during surgery that is undertaken for another reason. Cancer has not yet spread to other areas.
Stage II: Cancer can be felt during a digital rectal exam or discovered during a biopsy. Cancer has not yet spread.
Stage III :Cancer has spread to nearby tissue.
Stage IV: Cancer has spread to lymph nodes or to other parts of the body.
Prostate Cancer Risk Factors[edit | edit source]
While prostate cancer is common, relatively little is known about its aetiology.[1] There are several known risk factors that have been shown to indicate an increased risk of developing this type of cancer. However, many patients with one or more risk factors never get cancer, while others who get cancer may have had few or no known risk factors.
The following are risk factors for prostate cancer according to the American Cancer Society:
- Age: rare in men under 40 years old, but the chance rises rapidly after age 50. About 6 in 10 cases of prostate cancer are found in men aged older than 65 years.
- Race/ethnicity: develops more often in African American men and in Caribbean men of African ancestry, less often in Asian American and Hispanic/Latino men than in non-Hispanic whites.[8] Black men are twice as likely to die from prostate cancer than White men. A 2022 study found that this disparity is likely due to inherited genetics, modifiable cancer risk factors, and access to healthcare.[9]
- Geography: most common in North America, northwestern Europe, Australia, and on Caribbean islands. It is less common in Asia, Africa, Central America, and South America. The reasons for this are not clear.
- Family history: seems to run in some families, which suggests there may be a genetic factor in some cases. However, most prostate cancers occur in patients without a family history of it.
- Gene changes: several inherited gene mutations seem to raise prostate cancer risk by a small percentage.
Factors with less clear effects on prostate cancer risk:
- Diet: the exact role of diet in prostate cancer is unclear. Some studies suggest that men who consume a lot of dairy or calcium (through food or supplements) may have a higher risk of developing prostate cancer.
- Obesity: there may be a weak link between obesity and the risk of developing a more aggressive prostate cancer. The reasons for this are not clear.
- Smoking: may lead to more aggressive cancers and result in worse treatment outcomes.[10]
- Chemical exposures: the National Academy of Medicine considers there to be “limited/suggestive evidence” of a link between Agent Orange exposure and developing prostate cancer.
- Inflammation of the prostate: there is a possible link between prostatitis and an increased risk of developing prostate cancer. This is an area of ongoing research.
- Sexually transmitted infections: there is a possible link between sexually transmitted infections such as gonorrhea or chlamydia and increased risk of prostate cancer.[8]
Prostate Cancer Tests and Screenings[edit | edit source]
A patient will often receive a routine digital rectal exam and or prostate-specific antigen (PSA) test. If either of these screenings give the medical provider concern about a potential diagnosis of prostate cancer, they will order a biopsy and / or an MRI to confirm the diagnosis. Overall health status is important when making medical decisions. Patients should talk to their healthcare provider about the pros and cons of being tested and treated for prostate cancer.
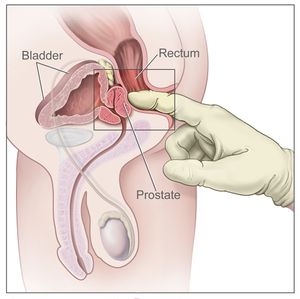
Digital Rectal Examination (DRE)[edit | edit source]
Internal examinations should ONLY be performed by qualified clinicians with advanced training in this skill.
- An examination in which the doctor inserts a finger into the rectum. This enables the doctor to palpate the back of the prostate gland to assess for enlargement or abnormal growths.
- There is a lack of evidence to support the efficacy of DRE. The majority of patients diagnosed with prostate cancer have abnormal PSA levels, but normal DRE results.
- This test may still be included in screening because even though it is less effective than a PSA blood test overall, it may still be able to detect cancer in men that have normal PSA levels.
Prostate-Specific Antigen (PSA) Test[edit | edit source]
- A blood test used to test for elevated levels of PSA, which occurs with any changes in the prostate.
- The risk of disease increases as the PSA level increases; however, a normal level of PSA has not been determined.
- No PSA level guarantees the absence of prostate cancer.
- There are several factors that may increase PSA levels.
- Although PSA remains the gold-standard test for possible prostate cancer diagnosis, it contributes significantly to over-treatment of men with less aggressive prostate cancer. This is a significant issue, as medical treatments for prostate cancer are associated with side effects that can have a significant negative impact on a patient's quality of life,[2] such as sexual dysfunction and urinary incontinence.[3]
Factors that might raise PSA levels include:
- Enlarged prostate
- Prostatitis
- Older age: PSA levels normally increase slowly with age
- Ejaculation: can increase PSA for a short time, therefore some doctors suggest that men abstain from ejaculation for a day or two before testing
- Riding a bicycle: studies suggest that cycling may temporarily raise PSA levels
- Certain medicines: taking male hormones such as testosterone, or other medicines that raise testosterone levels
Factors that might lower PSA levels (even if a man has prostate cancer):
- 5-alpha reductase inhibitors: drugs used to treat BPH or urinary symptoms, such as finasteride (Proscar or Propecia) or dutasteride (Avodart), can lower PSA levels
- Herbal mixtures: some dietary supplements might mask a high PSA level
- Certain medicines: research has suggested that long-term medicine use may lower PSA levels. These medications can include: aspirin, statins, and thiazide diuretics (such as hydrochlorothiazide). More research is needed to confirm these findings.
Biopsy[edit | edit source]
- The diagnosis of prostate cancer is established via a biopsy of the prostate gland and may be indicated for individuals who have elevated PSA levels.
- A small piece of the prostate gland is removed and examined under a microscope for cancer cells. If cancer cells are found, a Gleason score will be determined from the biopsy.
- A biopsy will confirm if a patient has prostate cancer. If prostate cancer is found on a biopsy, this test can also help tell how likely it is that the cancer will grow and spread quickly.[11]
- MRI can also be used to diagnose prostate cancer.[3]
Treatment Options[edit | edit source]
The first decision in managing prostate cancer is determining whether any treatment at all is needed. Prostate cancer, especially low-grade tumors, often grow so slowly that frequently, no treatment is required. This is particularly true in elderly patients and those with comorbidities that would reasonably limit life expectancy to 10 additional years or less.
The interprofessional team can optimise the treatment of these patients through communication and coordination of care. Primary care providers, urologists, oncologists, radiation oncologists, and nurse practitioners provide diagnoses and care plans. The interprofessional team can improve outcomes for patients with prostate cancer through use of the biopsychosocial treatment model.
There are two main options for treatment of prostate cancer: surgical and radiation. However, there are new technologies coming out and research being done continuously. Often, the decision between surgical and radiation treatments comes down to potential side-effects. It is important to discuss these side-effects with patients when making treatment decisions as they have a strong effect on quality of life post-procedure.[3]
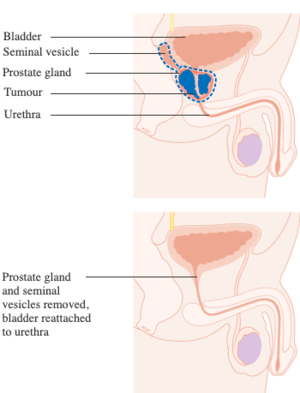
Surgical Interventions[edit | edit source]
Prostatectomy: This involves the removal of the prostate gland. A radical prostatectomy is the removal of the prostate gland and some surrounding tissue. A prostatectomy is a lengthy surgery, lasting 4-6 hours.[3]
Types of prostatectomies:[3]
- Open prostatectomy
- Laparoscopic prostatectomy
- Robot-assisted prostatectomy[12]
Potential side-effects of prostatectomy:[3]
- Post-surgical pain: usually resolves quickly.
- High likelihood of urinary incontinence: most likely stress incontinence. The majority of patients recover their continence with therapy interventions.
- Sexual dysfunction: only 30-40% of patients will regain sexual functioning. Patients will be anejaculate with orgasm (i.e. have an inability to ejaculate) due to the removal of seminal vesicles with prostatectomy. There are also penile changes such as penile shortening and curvature changes. Some patients may lose the ability to achieve an erection if the cavernous nerves could not be sparred during the surgical intervention.
Radiation[edit | edit source]
Use of high-energy radiation to try to destroy the cancer cells. There are two types of radiation therapy that differ by how radiation is applied to a diseased prostate:[3]
- External beam radiation therapy: the radiation is directed into the cancer cells from the outside of the body. Can have more side-effects due to radiation effecting the tissue surrounding the prostate, including the rectum, as it travels through the body.[3] In recent years, there have been improvements in the delivery of radiation therapy, enabling the administration of higher treatment doses with minimal tradeoff in terms tissue toxicity. Complications such as fistulae, bone toxicity, and secondary malignancy are rare, but there is a need for additional high-quality research to assess these side-effects and their management.[13]
- Brachytherapy (internal radiation therapy): Radioactive pellets are surgically implanted into the cancerous area to try to destroy the cells from the inside of the body. Radiation is contained in a specific area to destroy only targeted cells, causing less general tissue damage.
Potential side-effects of radiation treatment:
- Side-effects often do not appear until 2-5 years after treatment due to radiation build-up in tissues surrounding the prostate with gradual tissue decay/destruction. Not all patients who receive radiation treatment will develop side-effects.
- Urinary incontinence: most likely urge incontinence due to development of bladder irritation.
- Sexual dysfunction: changes in ejaculatory function and quantity due to fibrotic tissue changes post-radiation; penile changes such as penile shortening and curvature changes.
The following video compares the pros and cons of prostate surgery and radiation treatment using evidence from recent literature reviews.
Active Surveillance[edit | edit source]
Many low-risk cases can now be followed with active surveillance. Under active surveillance, patients are usually required to have regular, periodic PSA testing and at least one additional biopsy 12 to 18 months after the original diagnosis.
Treatment of Advanced Prostate Cancer[edit | edit source]
Hormone therapy may be used:
- If the cancer has metastasised too far to be cured by surgery or radiation
- If the cancer remains or comes back after surgical or radiation treatment
Types of hormone therapy:
- Androgen Deprivation Therapy: a type of hormone therapy which attempts to reduce the levels of male hormones, i.e. androgens in the body. Androgens stimulate prostate cancer cells to grow. The two main androgens are testosterone and dihydrotestosterone. The majority of androgens are produced by the testicles, but the adrenal glands and prostate cancer itself can also produce these hormones.
- Orchidectomy (surgical castration): surgical removal of the testicles, where the majority of the androgens are produced. This will cause most forms of prostate cancer to stop growing and possibly shrink in size for a time. This is an irreversible procedure, and men may have trouble accepting the removal of their testicles. Because of this, they may choose treatment with drugs that lower hormone levels.
The safety of testosterone therapy after prostate cancer treatment remains controversial. A 2018 study found that the fears of testosterone therapy causing or worsening prostate cancer do not appear to be well supported by available data. More research is warranted to determine the safety of testosterone therapy in men with prostate cancer.[16]
These patients have little to no prospect of sexual function return due to the lack of testosterone production and this can greatly effect a patient's quality of life after treatment and recovery.[3]
Role of Physiotherapy[edit | edit source]
The role of physiotherapy in the treatment of people with prostate cancer focuses on improving the likelihood of successful outcomes following surgical or radiation treatments to provide the highest level of quality life possible. This is done by providing:[3]
- Pre-treatment pelvic floor rehabilitation[12]
- Post-treatment pelvic floor rehabilitation
- Encouraging an active and fit lifestyle
- Behavioural modification
- Lifestyle modification
- Addressing both incontinence and sexual dysfunction issues to achieve the best likelihood of return of function
A 2019 study found that regular leisure-quality physical activity might prevent prostate cancer and improve cancer-related outcomes.[10]
The physiotherapist can play a role in recognising any treatment regret, depression, and or anxiety in this patient population, and guide them to manage "life after prostate cancer" with the interdisciplinary team as part of the biopsychosocial model.[3]
Resources[edit | edit source]
Patient handouts and information:
- American Cancer Society About Prostate Cancer education handout
- American Cancer Society Prostate Cancer Early Detection, Diagnosis, and Staging education handout
Recommended Reading:
- Brookman-May SD, Campi R, Henriquez JD, Klatte T, Langenhuijsen JF, Brausi M, Linares-Espinos E, Volpe A, Marszalek M, Akdogan B, Roll C. Latest evidence on the impact of smoking, sports, and sexual activity as modifiable lifestyle risk factors for prostate cancer incidence, recurrence, and progression: a systematic review of the literature by the European Association of Urology Section of Oncological Urology (ESOU). European urology focus. 2019 Sep 1;5(5):756-87.
- McGillivray HM, Piccolo EE, Wassersug RJ. “Partner”,“Caregiver”, or “Co-Survivor”—Might the Label We Give the Partners of Cancer Patients Affect the Health Outcome of the Patients and Their Partners?. Current Oncology. 2021 Dec 27;29(1):122-9.
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 Sung H, Ferlay J, Siegel RL, Laversanne M, Soerjomataram I, Jemal A, Bray F. Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA: a cancer journal for clinicians. 2021 May;71(3):209-49.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 Tonry C, Finn S, Armstrong J, Pennington SR. Clinical proteomics for prostate cancer: understanding prostate cancer pathology and protein biomarkers for improved disease management. Clinical Proteomics. 2020 Dec;17(1):1-31.
- ↑ 3.00 3.01 3.02 3.03 3.04 3.05 3.06 3.07 3.08 3.09 3.10 3.11 3.12 3.13 3.14 3.15 Roscher, P. Men's Health. Overview of Prostate Cancer. Plus. 2022
- ↑ 4.0 4.1 4.2 4.3 Gray H. Anatomy of the human body. Philadelphia: Lea & Febiger, 1918; Bartleby. com, 2000.
- ↑ White CW, Xie JH, Ventura S. Age-related changes in the innervation of the prostate gland: implications for prostate cancer initiation and progression. Organogenesis. 2013 Jul 1;9(3):206-15.
- ↑ Centers for Disease Control and Prevention. What Are the Symptoms of Prostate Cancer? Available from: https://www.cdc.gov/cancer/prostate/basic_info/symptoms.htm (accessed 14/04/2022).
- ↑ YouTube. Prostate101 | Chapter 2: Gleason Grading. Available from: https://www.youtube.com/watch?v=0XVN8GWH7Ms [last accessed 17/04/2022]
- ↑ 8.0 8.1 8.2 American Cancer Society. Prostate Cancer Risk Factors. Available from: https://www.cancer.org/cancer/prostate-cancer/causes-risks-prevention/risk-factors.html (accessed 16/04/2022).
- ↑ Stopsack KH, Nandakumar S, Arora K, Nguyen B, Vasselman SE, Nweji B, McBride SM, Morris MJ, Rathkopf DE, Slovin SF, Danila DC. Differences in prostate cancer genomes by self-reported race: Contributions of genetic ancestry, modifiable cancer risk factors, and clinical factors. Clinical Cancer Research. 2022 Jan 15;28(2):318-26.
- ↑ 10.0 10.1 Brookman-May SD, Campi R, Henriquez JD, Klatte T, Langenhuijsen JF, Brausi M, Linares-Espinos E, Volpe A, Marszalek M, Akdogan B, Roll C. Latest evidence on the impact of smoking, sports, and sexual activity as modifiable lifestyle risk factors for prostate cancer incidence, recurrence, and progression: a systematic review of the literature by the European Association of Urology Section of Oncological Urology (ESOU). European urology focus. 2019 Sep 1;5(5):756-87.
- ↑ 11.0 11.1 11.2 American Cancer Society. Screening Tests for Prostate Cancer. Available from: https://www.cancer.org/cancer/prostate-cancer/detection-diagnosis-staging/tests.html(accessed 16/04/2022).
- ↑ 12.0 12.1 Goonewardene SS, Gillatt D, Persad R. A systematic review of PFE pre-prostatectomy. Journal of Robotic Surgery. 2018 Sep;12(3):397-400.
- ↑ Matta R, Chapple CR, Fisch M, Heidenreich A, Herschorn S, Kodama RT, Koontz BF, Murphy DG, Nguyen PL, Nam RK. Pelvic complications after prostate cancer radiation therapy and their management: an international collaborative narrative review. European urology. 2019 Mar 1;75(3):464-76.
- ↑ YouTube. Cancer Better | Side Effects of Surgery Vs Radiation for Prostate Cancer. Available from: https://www.youtube.com/watch?v=RuGenDjS950 [last accessed 17/04/2022]
- ↑ American Cancer Society. Hormone Therapy for Prostate Cancer. Available from: https://www.cancer.org/cancer/prostate-cancer/treating/hormone-therapy.html (accessed 17/04/2022).
- ↑ Rodriguez KM, Pastuszak AW, Khera M. The role of testosterone therapy in the setting of prostate cancer. Current urology reports. 2018 Aug;19(8):1-9.