Men's Health Physiotherapy Pelvic Treatment
Top Contributors - Stacy Schiurring, Kim Jackson, Lucinda hampton and Jess Bell
Clinical Reasoning after Assessment[edit | edit source]
Disclaimer: This page aims to provide an introductory discussion of men's health physiotherapy treatment techniques. Please note that further training is required through a reputable pelvic health education company before attempting the techniques discussed in this page. See the Resources section at the bottom of this page for links to pelvic and men's health special interest groups.
The physiotherapy assessment is the most critical part of a therapist's interaction with their patient. Assessment and reassessment should occur every session to develop a detailed clinical picture to guide the creation of the treatment plan. Every patient's clinical picture is unique, therefore comprehensive and ongoing assessment will ensure that the patient receives effective and efficient physiotherapy management.
For a review of men's health physiotherapy pelvic assessment, please read this article.
Male Pelvic Physiotherapy Treatments[edit | edit source]
Pelvic Floor Muscle Rehabilitation[edit | edit source]
Pelvic floor muscle training "is the essence of “functional fitness,” training muscles to help in practical life activities. Because of its simplicity, safety, and noninvasiveness, it should be employed as a first-line approach."[1]
Pelvic floor muscle rehabilitation can encompass a variety of issues: muscle over-utilisation, muscle weakness, muscle dysfunction and or poor coordination.[2] As when training any muscle group, it is important to properly assess the dysfunction prior to beginning treatment to ensure the patient is receiving the proper therapeutic interventions. A muscle must have the appropriate length, strength, and neuromuscular control to function properly.
Please watch the following short video to learn more about the muscle length-strength relationship.
The muscles of the male pelvic floor are all skeletal muscles and are, therefore, adaptable.
- 70% of the pelvic floor muscles are slow-twitch type 1 (fatigue-resistant fibres that maintain static tone)
- 30% are fast-twitch type 2 (fatigue-prone fibres that are capable of active contraction).
This ratio can change with ageing, inactivity, and nerve innervation damage.[1] To learn more about muscle fibre types, please read this article.
Pelvic Floor Strengthening[edit | edit source]
When pelvic floor muscle strengthening is indicated, exercises can be performed to improve muscle endurance and or muscle agility. It is important to match the type of muscle strengthening with the patient's specific issue.[2] Many patients require a combination of the two types of muscle strengthening.
- If a patient with urinary incontinence has urine leaking throughout the day, this is likely a muscle endurance issue.
- However, a patient who only leaks urine with a forced exhalation, such as a cough, likely has a muscle quick fire issue.
Pelvic floor exercises are all about technique. With optimal pelvic floor motor learning, there is more potential for improved continence and erectile function. When performing pelvic floor muscle strengthening, it is helpful to either palpate the muscle or utilise real-time ultrasound to provide the patient with feedback.
Verbal cues can also affect the degree of observable motion in the pelvic floor muscles. Commonly used phrases to help elicit male pelvic floor contractions are “shorten the penis”, “elevate the bladder”, “elevate the scrotum”, “stop the flow of urine” and “tighten the anus.”[4] Stafford et al.[4] conducted a study in asymptomatic participants and in patients with incontinence. The cues “shorten the penis” and “stop the flow of urine” were considered the best to target the specific muscles involved in urinary continence.[4] Rather than "lift your scrotum", men seem to respond well to the popular colloquial cue “nuts to guts.” This cue targets the important lifting action of the pelvic floor.
- Endurance or slow-twitch fibres: Establish a maximum effort contraction of the pelvic floor muscles. Have the patient hold a 20% max contraction for a set amount of time, such as 4 seconds. Gradually increase the 20% max hold to 6 seconds, 10 seconds, et cetera, allowing the patient to gain control and endurance of the pelvic floor muscles.[2]
- Agility or fast-twitch fibres: Establish a maximum effort contraction of the pelvic floor muscles. Have the patient hold a 80% max contraction for a set amount of time, such as 4 seconds then relax. Repeat the 80% max hold for 4 seconds for a set amount of repetitions to perform pelvic floor "flicks."[2]
- Pelvic floor muscle "cross-training": a combination of the above. For example, mix 80% max and 20% max holds for set amounts of time for a set amount of repetitions.[2]
When performing these strengthening exercises, it can be helpful to provide the patient with a chart or graph with the expected %max holds, hold times, and repetitions outlined to serve as a guide during the session.[2] This can also be provided as part of the patient's home exercise programme.
The following videos are examples of male pelvic floor contractions as viewed via real-time ultrasound. The video on the left is a supra-pubic view, the video on the right is transperineal.
Pelvic Floor Inhibition[edit | edit source]
Increased pelvic floor tone can be a cause of pelvic floor pain and sexual dysfunction. There are multiple techniques that can be used to decrease pelvic floor muscle tone or tightness.
- Stretching: by rotating the pelvis, one can stretch the muscles of the pelvic floor. Examples include: lunges, bilateral hip external rotation, squatting. Focus on slow and controlled movements.
- Breathing: slow, deep, diaphragmatic breathing to assist with relaxation.
- Mindfulness: focus on awareness of the pelvic floor activation and training the muscles to relax.
- Internal treatments: trigger point release. Patients can be educated on how to perform releases as part of a home exercise programme.
- Hip joint mobility treatments: Maitland or Mulligan mobilisations to improve hip pain and / or stiffness can have good carry over to address pelvic floor muscle tone or tightness.
The following video is a short example of pelvic floor relaxation utilising breathing and mindfulness.
Pelvic Floor Coordination Training[edit | edit source]
Real-time ultrasound is a useful treatment option for patients who present with good pelvic floor muscle strength and length, but have coordination issues. Biofeedback alone has been shown to be less effective in retraining the pelvic floor muscles than when biofeedback is used as an adjunct to skilled physiotherapy interventions.[8]
Pain Management[edit | edit source]
An accurate and thorough assessment is critical to identify the exact source of pain. Utilise the biopsychosocial model as needed for referrals to gather more information or if findings are outside of a physiotherapy scope of practice.
Potential treatment approaches for pain conditions may include:
- Pelvic floor muscle relaxation or inhibition
- Internal treatments
- Joint mobilisations of the lumbar spine, sacrum, and / or hips
- Neurodynamic treatments, including nerve glides and flossing
- Soft tissue work such as skin rolling, myofascial release, visceral work
- Dry Needling
- Patient education on self management techniques
Urinary Incontinence[edit | edit source]
For more information on male urinary incontinence, please read this article.
When providing treatment for urinary incontinence, the following issues need to be considered and potentially addressed:
- Pelvic floor rehabilitation is not a passive intervention and to see improvements patients need to adhere to the exercises
- Any bowel dysfunction must be managed as this negatively impacts the pelvic floor and bladder
- Any mental health issues must be addressed
- General exercise is very important and has been shown to improve outcomes
- Weight loss is important in overweight men as obesity has been linked to poorer outcomes
Potential treatment approaches for male urinary incontinence may include:
- Pelvic floor work to improve sphincter control (strongly supported by research)[9]
- Use of transperineal ultrasound[10] - provide visual cues of pelvic floor contractions for improved urethral control[11]
- TENS neuromodulation to stimulate the tibial nerve and / or around the sacrum can be a very effective treatment for urge incontinence.[2][11] See next section below for more details.
- Behavioural management: discussing what to wear such as dark pants to hide leaks,[12] limiting fluid intake when away from home, being aware of any foods or drinks that may irritate the bladder
- Bladder training techniques such as stimulating S3-S4 dermatomal levels by: rubbing the inner thighs; squeezing the knees together; pushing toes into the floor. These activities can override the bladder by challenging the micturition reflex[2][11]
- Use of male incontinence pads[11]
- Use of penile clamps
- Use of questionnaires and / or a bladder diary to gather information and track progress[11]
TENS neuromodulation to stimulate the tibial nerve[edit | edit source]
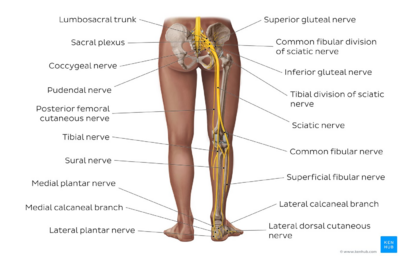
TENS neuromodulation to stimulate the tibial nerve involves the use of electrical impulses to address urinary symptoms, the aim of this stimulation is to target the lower urinary tract innervation system. Stimulation of the posterior tibial nerve will deliver retrograde neuromodulation to the sacral nerve plexus that controls the bladder function and can have positive effects on urinary incontinence.[13]
A 2014 study compared the use of tibial nerve neuromodulation with the use of oxybutynin medication to manage incontinence in women. The study found that while all test groups showed improvement, a combination of treatments was more effective than either treatment alone. In addition the use of neuromodulation, either alone or in combination with medication provided longer lasting results in terms of clinical symptom improvement and quality of life.[13][14]
Bowel Issues[edit | edit source]
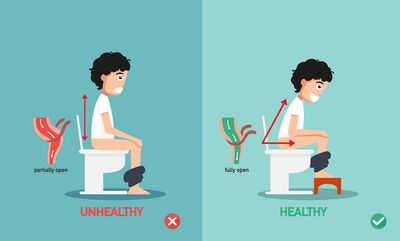
Bowel health can have a strong affect on overall pelvic floor functioning. When assessing a patient's bowel habits, it is important to ask about toileting position, and discuss the use of mindful breathing versus Valsalva during voiding. For more information on toileting position and how male anatomy can be affected by it, please read this article.
Men with pelvic pain commonly have a history of constipation and or haemorroids. This is a common symptom for people who must use a large amount of pressure during voiding. A musculoskeletal and breathing assessment would be beneficial for these patients.
Penile Issues[edit | edit source]
Penile health relies on regular erections (a man will typically have 5-8 nocturnal erections every night). The blood flows into the penis during an erection and encourages mobility of the connective tissue and smooth muscle of the penis.[15]
- Peyronies disease involves a variety of penile symptoms including pain, curvature, shortening, palpable plaque and erectile dysfunction. The development of plaque within the penis results in the curvature. Joanne Milios, a physiotherapist in Australia, has found that the use of therapeutic ultrasound as a treatment for Peyronies disease results in reduced penile pain, improved penile deformity and increased erectile function.[12] Extracorporeal Shock Wave Therapy (ESWT) is also gaining acceptance in the treatment of Peyronies disease. A 2021 meta-analysis found that ESWT failed to improve penile curvature or pain, but that it may reduce plaque size. The authors concluded that further research was indicated to confirm these findings.[16] More recently, a 2022 study found that low-intensity ESWT had a positive impact on patient penile pain, curvature, and plaque size when used during the acute phase of Peyronies disease.[17]
- Penile shortening is common after a prostatectomy and a patient can expect a loss in length of one to two centimetres. Treatment of penile shortening involves patient education on self-stretching, skin rolling, encouragement of erections using either a vacuum therapy device or erection medication, and masturbation.[2]
- Painful orgasm is likely due to increased pelvic floor muscle tone or tightness and / or pelvic floor pain. Treatment may involve pelvic floor muscle inhibition or relaxation, coordination training, and patient self-treatment techniques.
- Erection quality is often affected by impaired muscle coordination and / or endurance. Treatment may involve pelvic floor strengthening and coordination training. Pelvic floor physiotherapy is an excellent alternative to medication use to achieve quality erections.
Resources[edit | edit source]
- Siegel AL. Pelvic floor muscle training in males: practical applications. Urology. 2014 Jul 1;84(1):1-7.
- Nahon, I. Physiotherapy management of incontinence in men. J Physiother. 2021;67(2):87-94.
- Gronski S. Pelvic Pain The Ultimate Cock Block: A no-bullshit guide for men navigating through pelvic pain. Dr. Susie Gronski, Inc., 2020.
Professional Associations and Formal Continuing Education Courses:
- American Physical Therapy Association: Academy of Pelvic Health
- American Physical Therapy Association: On-Demand: Male Pelvic Pain Course
- Australian Physiotherapy Association: Men's Health
- Australian Physiotherapy Association: Male Pelvic Health
References[edit | edit source]
- ↑ 1.0 1.1 Siegel AL. Pelvic floor muscle training in males: practical applications. Urology. 2014 Jul 1;84(1):1-7.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 2.7 2.8 2.9 Roscher, P. Men's Health Physiotherapy Pelvic Treatment. Men's Health Course. Plus. 2022
- ↑ YouTube. Exercise Physiology | Skeletal Muscle Length-Tension Relationship. Available from: https://www.youtube.com/watch?v=n6Flu2szvhk [last accessed 05/04/2022]
- ↑ 4.0 4.1 4.2 Stafford RE, Ashton‐Miller JA, Constantinou C, Coughlin G, Lutton NJ, Hodges PW. Pattern of activation of pelvic floor muscles in men differs with verbal instructions. Neurourology and urodynamics. 2016 Apr;35(4):457-63.
- ↑ YouTube. Contraction of the pelvic floor muscles in ultrasound Available from: https://www.youtube.com/watch?v=4umq_GHvvPg [last accessed 05/04/2022]
- ↑ YouTube. Men's Health Ultrasound - Male Pelvic Floor Contraction Available from: https://www.youtube.com/watch?v=E4dx8f1V1Zs [last accessed 05/04/2022]
- ↑ YouTube. Michelle Kenway | Pelvic Floor Relaxation for Men with Chronic Pelvic Pain. Available from: https://www.youtube.com/watch?v=Fac5ihuQ1Ws [last accessed 05/04/2022]
- ↑ Ladi-Seyedian SS, Sharifi-Rad L, Nabavizadeh B, Kajbafzadeh AM. Traditional biofeedback vs. pelvic floor physical therapy—is one clearly superior?. Current urology reports. 2019 Jul;20(7):1-9.
- ↑ 9.0 9.1 Hodges PW, Stafford RE, Hall L, Neumann P, Morrison S, Frawley H, Doorbar-Baptist S, Nahon I, Crow J, Thompson J, Cameron AP. Reconsideration of pelvic floor muscle training to prevent and treat incontinence after radical prostatectomy.InUrologic Oncology: Seminars and Original Investigations 2020 May 1 (Vol. 38, No. 5, pp. 354-371). Elsevier.
- ↑ Stafford RE, van den Hoorn W, Coughlin G, Hodges PW. Postprostatectomy incontinence is related to pelvic floor displacements observed with trans‐perineal ultrasound imaging. Neurourology and urodynamics. 2018 Feb;37(2):658-65.
- ↑ 11.0 11.1 11.2 11.3 11.4 Nahon I. Physiotherapy management of incontinence in men. Journal of physiotherapy. 2021 Apr 1;67(2):87-94.
- ↑ 12.0 12.1 Milios JE, Ackland TR, Green DJ. Peyronie’s disease and the role of therapeutic ultrasound: A randomized controlled trial. Journal of Rehabilitation Therapy. 2020 Aug 8;2(2).
- ↑ 13.0 13.1 Bhide AA, Tailor V, Fernando R, Khullar V, Digesu GA. Posterior tibial nerve stimulation for overactive bladder—techniques and efficacy. International urogynecology journal. 2020 May;31(5):865-70.
- ↑ Souto SC, Reis LO, Palma T, Palma P, Denardi F. Prospective and randomized comparison of electrical stimulation of the posterior tibial nerve versus oxybutynin versus their combination for treatment of women with overactive bladder syndrome. World journal of urology. 2014 Feb;32(1):179-84.
- ↑ Salonia A, Adaikan G, Buvat J, Carrier S, El-Meliegy A, Hatzimouratidis K, McCullough A, Morgentaler A, Torres LO, Khera M. Sexual rehabilitation after treatment for prostate cancer—part 2: recommendations from the Fourth International Consultation for Sexual Medicine (ICSM 2015). The journal of sexual medicine. 2017 Mar 1;14(3):297-315.
- ↑ Bakr AM, El-Sakka AI. Extracorporeal Shockwave Therapy in Peyronie's Disease: Systematic Review and Meta-Analysis. The Journal of Sexual Medicine. 2021 Oct 1;18(10):1705-14.
- ↑ Abdessater M, Akakpo W, Kanbar A, Parra J, Seisen T, Chartier-Kastler E, Drouin SJ, Roupret M. Low-intensity extracorporeal shock wave therapy for Peyronie's disease: a single-center experience. Asian Journal of Andrology. 2022 Jan;24(1):45.