Osteophyte
Original Editor - Lucinda hampton
Top Contributors -Lucinda hampton, Nupur Smit Shah and Kim Jackson
Introduction[edit | edit source]
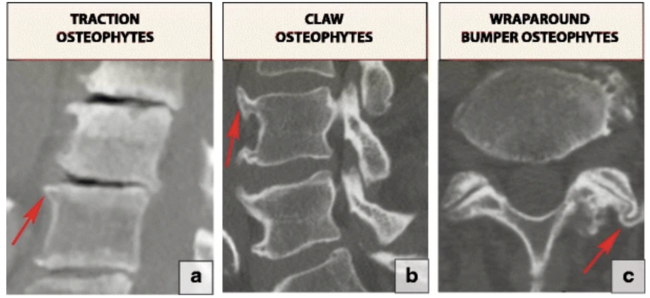
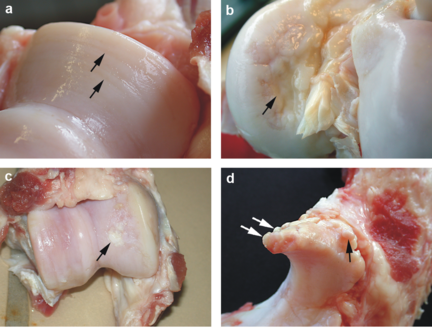
Osteophytes are cartilage-capped bony proliferations (bony spurs) that most commonly develop at the margins of a synovial joint as a response to articular cartilage damage, as seen very commonly in osteoarthritis (OA).[1]
Pathophysiology[edit | edit source]
Osteophytes are formed of fibrocartilage and bone, often forming at the peripheral margins of joints at the interface between cartilage and the periosteum. Osteophytes are thought to develop from chondrogenic differentiation of progenitor cells, commonly from within the periosteum. Osteophytes appear to be a cellular repair response to the altered growth factor environment following joint injury. In some cases osteophytes can contribute to the stability of the joints.[2]
Presentation[edit | edit source]
Osteophytes are most commonly found in the following areas. Neck, shoulder, knee, lower back, fingers or big toe, foot or heel. Osteophytes cause problems for example if they: cause friction if rubbing against footwear; impinge nerves such as an existing spinal root; restrict movement as may occur in hip and knee OA.[3] Following are the pages of conditions where osteophytes are present:
- Hallux Rigidus
- Anterior Ankle Impingement Syndrome
- Osteoarthritis of knee
- Uncovertebral Joints
- Lumbar Spinal Stenosis
- Vertebral osteophytes are a characteristic of disc degeneration. [4]
- Cervical Osteoarthritis
- Lumbar Spondylosis
- Hip Osteoarthritis
- Ankle osteoarthritis
Treatment[edit | edit source]
Osteophytes when causing issues, for example with OA, can be managed along side management of OA, See link here Osteoarthritis. They are not managed specifically.
Removal of an osteophyte is not usual, unless it's irritating a nerve in the spine or restricting a joint's range of movement. If surgery is warranted, a surgeon will explain the procedure's risks and benefits.[3]
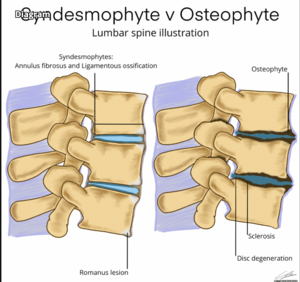
Differential Diagnosis[edit | edit source]
- Syndesmophyte: Thin, vertically oriented ossification of annular ligament (Sharpey fibers) from ankylosing spondylitis[5]
- Enthesophyte: located at an attachment of a ligament, fascia or tendon, not associated with a joint.[1]
- It is difficult to tell the difference between an osteophyte and disc herniation solely by MRI. CT is a helpful adjunct; however, often central canal and foraminal narrowing are caused by a combination of a disc herniation and osteophyte.
References[edit | edit source]
- ↑ 1.0 1.1 Radiopedia Osteophyte Available:https://radiopaedia.org/articles/osteophyte-2 (accessed 7.9.2022)
- ↑ Firestein GS, Budd RC, Gabriel SE, McInnes IB, O'Dell JR. Kelley's Textbook of Rheumatology E-Book. Elsevier Health Sciences; 2012 Aug 31. Available:https://www.sciencedirect.com/topics/medicine-and-dentistry/osteophyte (accessed 7.9.2022)
- ↑ 3.0 3.1 NHS Osteophyte Available:https://www.nhs.uk/conditions/osteophyte/ (accessed 7.9.2022)
- ↑ Czervionke LF, Fenton DS. Imaging Painful Spine Disorders E-Book. Elsevier Health Sciences; 2011 Apr 28.Available:https://www.sciencedirect.com/topics/medicine-and-dentistry/osteophyte (accessed 8.9.2022)
- ↑ Blankenbaker DG, Davis KW. ExpertDDx: Musculoskeletal E-Book. Elsevier Health Sciences; 2017 Oct 13.Available: https://www.sciencedirect.com/topics/medicine-and-dentistry/osteophyte(accessed 8.9.2022)