Mental Health Interventions for People Living With HIV
Original Editor - Uploaded by Khloud Shreif for Melissa Coetsee
Top Contributors - Khloud Shreif, Melissa Coetsee and Kim Jackson
Introduction[edit | edit source]
Since its outbreak in the 1980’s, HIV has resulted in immense global and individual health consequences, and in some African countries, it remains the leading cause of death. The introduction and improved availability of ART (antiretroviral treatment) in recent years, has resulted in fewer people succumbing to the fatal effects of the virus [1]. With more people surviving, the prevalence of HIV has increased significantly. This brings forth the challenge of ensuring that PLWH (people living with HIV) are living good quality, functional lives. Both the effects of the virus and the side effects of ART can have detrimental effects on PLWH’s physical health (pain and energy levels) and mental health (depression and anxiety)[1].
Relationship Between HIV and Mental Health[edit | edit source]
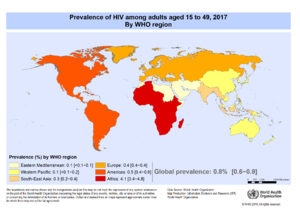
One of the prominent elements contributing to impaired quality of life of PLWH is poor mental health. Mental health problems, such as depression and anxiety, are very common among PLWH. The prevalence rate of depression and mood disorders among PLWH is approximately 33% and the prevalence rate of anxiety disorders is about 20%[2]. This is much higher than the global prevalence of the general population which is 4.7%[3]. It is therefore clear that having HIV poses an increased risk of developing mental health disorders.
Mental health problems have been recognised as a key factor in affecting HIV treatment outcomes[4]. Poor mental health has been shown to negatively affect HIV disease progression as well as adherence to ART[5]. Those who report needing mental health care, but do not receive it, are more likely to not adhere to their ART medication compared to those who do receive mental health care support[6]. Furthermore, evidence also suggests that poor viral suppression (as a result of poor ART adherence) may again lead to an increased risk of mental health problems[6]. High levels of stress and depression have also been associated with poor disease parameters (reduced CD4 and increased viral load) - This could be related to associated poor ART adherence, or attributed to the physiological effects of stress and depression [1].
“PLWH and depression are 42% less likely to achieve good ART adherence, more likely to develop virologic failure and are more likely to have HIV progression, independent of ART adherence, than those without depression” [7]
Mental health in PLWH can be influenced by various biopsychosocial factors, including:
- Isolation
- Stigma
- Discrimination
- Low socio-economic status
- Lack of support
- Disease-related pain
- Neurological damage caused by opportunistic infections
- Neuropsychiatric side effects of some ART (Zidovudine and Abacavir have been associated with mood changes)[4].
- Food insecurity and poverty[8].
- Lack of purpose in society [8].
The World Health Organisation (WHO) describes the concept of quality of life as: “an individual’s perception of their position in life in the context of the culture and value systems in which they live and in relation to their goals, expectations, standards, and concerns”. It is clear that addressing mental health in PLWH should be a priority - not only to improve psychological factors but in order to improve medication adherence and physical health - in order to ultimately improve the quality of life of PLWH.
Mental Health Intervention for PLWH[edit | edit source]
The prevalence of PLWH is much higher in low-mid income settings, but there are significant barriers to providing mental health services in these countries, mostly since there is a lack of trained mental health workers[1]. In Sub-saharan Africa (SSA), there is one mental health professional per 70 000 people. Furthermore, time spent in therapy could be time spent for income generation and could therefore result in poor adherence in low-mid income countries [8]. Thus, the very therapies that are deemed efficacious for HIV-positive populations in resource-rich settings may not be feasible to deliver in SSA settings. It is possible that group-based interventions could have better acceptability than traditional individual mental health therapies[11].
Pharmacological interventions[edit | edit source]
The majority of PLWH, live in low to middle-income countries. It is therefore important to consider results from studies that were done in these settings. In studies conducted in Uganda, full adherence to medication was low (56%)[4] and in Malawi treatment was hindered by low stock of antidepressants nationwide[4]. In addition, the evidence to support the use of antidepressants is inconclusive and it might not have many benefits over psychological interventions alone[4]. Considering the potential issues with adherence and the lack of strong evidence, pharmacological interventions might not be the most practical or cost-effective treatment in PLWH.
Psychotherapeutic interventions[edit | edit source]
Adherence to psychotherapeutic interventions is also important to consider, as this will have an effect on the effectiveness of the treatment. It is therefore important to ensure that the interventions are tailored to the cultural context of the target population[4].
The approach used and the level of qualification of the therapist do not seem to be associated with intervention effectiveness in low-mid income settings [4][1], it can therefore be argued that a group format delivered by lay healthcare workers could be an effective, sustainable and accessible option in poorer countries[4]. Programs aimed at training lay health workers in counseling will be important in narrowing the mental health treatment gap in low- and mid-income (LMICs) countries[4].
Every person’s context will be different, and it’s important to involve the community in the intervention design to ensure good adherence[4]. Some studies have included financial incentives and cultural rituals, others involved spiritual activities during therapy. Recent research indicates that accommodating patient preference in mental health services maximizes treatment uptake and reduces the financial costs of premature dropout and disengagement[4].
The evidence seems to suggest that, when it comes to psychotherapy, it is more important to consider what is available and culturally appropriate, rather than focusing on the content and specifics of the therapeutic method/approach.
Individual therapy
There is good evidence to support the effectiveness of psychotherapy for depression in PLWH in both low and high resource settings [1] [7]. The ‘active ingredients of psychotherapy that were associated with enhanced effectiveness in research studies were:
- Cognitive restructuring
- Positive coping skills
- Venting (sharing personal problems)
- Social support
- Behaviour activation[4].
Group therapy
Group support psychotherapy sessions which are suited to a community, have been shown to be very effective in achieving a long-lasting reduction in depression in PLWH[4]. These group therapy sessions should involve behavioral psychotherapeutic methods (education, sharing, coping skills, etc.), as well as training in basic life skills and planning livelihood activities[11]. A major advantage of a well-designed group intervention is that it does not require ongoing input from expert mental health practitioners. Instead, primary healthcare workers in rural health centers are trained to deliver the sessions. Attending group sessions has also been shown to improve clinical health parameters. This could partially be attributed to associated improved adherence to ART with subsequent suppression of the HIV viral load. This means that affected individuals are less likely to transmit the virus to others. It is also more cost-effective than group HIV education-only sessions[11].
Social and behavioral interventions[edit | edit source]
Interventions such as yoga, meditation, mindfulness, symptoms management strategies, and education, have been shown to be effective in addressing mental health QOL in PLWH, but the quality of evidence is unfortunately poor[12].
There is a known relationship between poverty and mental health, and research has found a correlation between food security and depression in PLWH in sub-saharan Africa[8]. Therefore livelihood programs that aim to improve food security could have potential. A study has shown that providing food hand-outs has little effect on mental health. Therefore the focus should be on interventions that focus on building skills and capital over time, with the aim of restoring productive routines and reducing financial concerns[8]. One study performed in Kenya showed that improved food security resulted in reduced anxiety and depressive symptoms in PLWH. These interventions have the benefit of reducing financial stress but also serve as a means to restore purpose and reduce rumination, as well as improve self-efficacy[8].
“For those who are stigmatized and marginalized, as those with food insecurity and HIV often are, livelihood interventions can contribute powerfully to social reintegration and reversal of status loss —which may be even more important than short-term gains in food security” [8].
Physical activity and exercise interventions[edit | edit source]
The benefits of exercise on the physical health of PLWH are well established and exercise has therefore been advocated for as an important treatment component for PLWH. Various studies have now shown that exercise (aerobic and resistance exercise) can also have positive effects on mental health in PLWH[5][13]. The low cost and ease of implementation of exercise interventions, make it a very feasible treatment approach in all settings [7].
Integrated approach[edit | edit source]
PLWH often has multiple physical barriers to well-being. Pain and lack of energy, as well as recurrent infections, can have a significant influence on mental well-being[1]. Combined medical and psychological interventions are therefore advised to ensure that physical symptoms do not continue to contribute to poor mental health. Collaboration between health care providers or integrated multidisciplinary facilities could assist in addressing the complexity of factors involved in the well-being of PLWH.
Physical therapy Intervention[edit | edit source]
Physios can play a major role in addressing many of the factors that influence the quality of life of PLWH. In high resource settings these interventions might take the form of one on one physio sessions. The reality however is that most people living with HIV live in under resourced settings with little or no access to rehabilitation services. From a public health perspective this poses a big challenge, but also an opportunity.
Physiotherapists often have more time with patients and it is common for patients to share otherwise withheld information with their physiotherapist once a report has been built. Physiotherapists can therefore play a role in identifying patients with mental health concerns and assist with referral where indicated. One study has shown that a good therapeutic relationship can be sufficiently beneficial for pain reduction when compared to education and exercise[14].
Exercise and groups
The proven effectiveness of exercise in improving physical and psychological parameters in PWLH [15][16], makes it a very valuable intervention. Physiotherapists are well trained in designing exercise programs and should play an important role in this facet of HIV management. To improve cost-effectiveness in low resource settings, group exercise classes should be considered. Training of local community members to run such exercises programs could make it more sustainable and has the potential to improve adherence and cultural relevance. Exercise itself has positive physiological effects that can reduce depression, and in addition the group setup could provide a form of support which can further improve mental health.
Pain management
PLWH often present with chronic pain. This could be related to ART side effects, effects of the virus or as a result of deconditioning. Persistent pain can contribute to poor mental health and poor ART adherence[17]- therefore addressing pain should be an important consideration in PLWH. Pain is a multi-faceted phenomenon influenced by various biological, social and psychological factors. Therefore, where possible, physiotherapists should thoroughly assess patients in order to determine the possible underlying mechanisms contributing to pain. In PLWH this is particularly challenging as a multitude of biological, pharmaceutical and psychological factors are present at once. Proper assessment will assist in providing appropriate interventions (exercise, pain neuroscience education, neural mobilisation, strengthening). Various interventions could be successful if designed to target the appropriate underlying mechanisms, but overall exercise and pain education has good evidence to support its effectiveness in HIV patients. A study performed in South Africa proved that a 6-week peer-led exercise program and education interventions are both effective treatments for pain in women living with HIV[18].
Global Health Considerations[edit | edit source]
The highest burden of HIV depression is found in Africa[2], where a lack of resources and infrastructure poses challenges to mental health interventions. Ironically most of the mental health intervention research thus far for this population group has been done in high-resource settings. It is therefore important for further research to be focused on low to mid-income settings, as well as on interventions that are cost-effective and culturally appropriate.
In 2018, UNAIDS made it clear that HIV and mental health is a topic that needs more attention in order to address the HIV epidemic[4]. Mental health conditions can vary from mild to severe, and therefore policies should not only be focused on treatment interventions, but also on promotion and preventive strategies [19].
Conclusion[edit | edit source]
One can almost argue that access to mental health treatment and rehabilitation for PLWH, should be just as important as access to ART. PLWH has the right to improved quality of life, and addressing mental health concerns should therefore be a very important consideration. Physiotherapists have an important role to play in providing effective, holistic interventions for PLWH.
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 van Luenen S, Garnefski N, Spinhoven P, Spaan P, Dusseldorp E, Kraaij V. The benefits of psychosocial interventions for mental health in people living with HIV: a systematic review and meta-analysis. AIDS and Behavior. 2018 Jan;22(1):9-42.
- ↑ 2.0 2.1 Evans DL, Charney DS, Lewis L, Golden RN, Gorman JM, Krishnan KRR, et al. Mood Disorders in the Medically Ill: Scientific Review and Recommendations. Biological Psychiatry. 2005 Aug;58(3):175–89.
- ↑ Ferrari AJ, Somerville AJ, Baxter AJ, Norman R, Patten SB, Vos T, et al. Global variation in the prevalence and incidence of major depressive disorder: a systematic review of the epidemiological literature. Psychological Medicine. 2012 Jul 25;43(3):471–81.
- ↑ 4.00 4.01 4.02 4.03 4.04 4.05 4.06 4.07 4.08 4.09 4.10 4.11 4.12 4.13 Nakimuli‐Mpungu E, Musisi S, Smith CM, Von Isenburg M, Akimana B, Shakarishvili A, et al. Mental health interventions for persons living with HIV in low‐ and middle‐income countries: a systematic review. Journal of the International AIDS Society. 2021 Jun;24(S2).
- ↑ 5.0 5.1 Nosrat S, Whitworth JW, Ciccolo JT. Exercise and mental health of people living with HIV: A systematic review. Chronic illness. 2017 Dec;13(4):299-319.
- ↑ 6.0 6.1 Scroggins S, Schacham E, Renee M. Integrating Mental Health Care Services Into HIV Comprehensive Care. The American Journal of Managed Care. 2020 Aug 1;26(8):357–60.
- ↑ 7.0 7.1 7.2 Lofgren SM, Nakasujja N, Boulware DR. Systematic review of interventions for depression for people living with HIV in Africa. AIDS and Behavior. 2018 Jan;22(1):1-8.
- ↑ 8.0 8.1 8.2 8.3 8.4 8.5 8.6 Hatcher AM, Lemus Hufstedler E, Doria K, Dworkin SL, Weke E, Conroy A, et al. Mechanisms and perceived mental health changes after a livelihood intervention for HIV-positive Kenyans: Longitudinal, qualitative findings. Transcultural Psychiatry. 2019 Jun 26;57(1):124–39.
- ↑ eNCA. Examining mental illness and HIV/Aids. Available from: http://www.youtube.com/watch?v=kJ73fAQ2hQM[last accessed 12/8/2022]
- ↑ Al Jazeera English . The psychological trauma of living with HIV in South Africa. Available from: http://www.youtube.com/watch?v=Pq7ddbQ4zuI[last accessed 12/8/2022]
- ↑ 11.0 11.1 11.2 Nakimuli-Mpungu E, Musisi S, Wamala K, Okello J, Ndyanabangi S, Birungi J, Nanfuka M, Etukoit M, Mayora C, Ssengooba F, Mojtabai R. Effectiveness and cost-effectiveness of group support psychotherapy delivered by trained lay health workers for depression treatment among people with HIV in Uganda: a cluster-randomised trial. The Lancet Global Health. 2020 Mar 1;8(3):e387-98.
- ↑ Bhatta DN, Liabsuetrakul T, McNeil EB. Social and behavioral interventions for improving quality of life of HIV infected people receiving antiretroviral therapy: a systematic review and meta-analysis. Health and quality of life outcomes. 2017 Jan;15(1):1-4.
- ↑ Ibeneme SC, Uwakwe VC, Myezwa H, Irem FO, Ezenwankwo FE, Ajidahun TA, Ezuma AD, Okonkwo UP, Fortwengel G. Effectiveness of Exercise Training on Mental Health, Physical Activity Level and Social Participation in People Living with HIV/AIDS: A Systematic Review and Meta-Analysis.
- ↑ Jackson K, Wadley AL, Parker R. Managing pain in HIV/AIDS: a therapeutic relationship is as effective as an exercise and education intervention for rural amaXhosa women in South Africa. BMC public health. 2021 Dec;21(1):1-4.
- ↑ Heissel A, Zech P, Rapp MA, Schuch FB, Lawrence JB, Kangas M, Heinzel S. Effects of exercise on depression and anxiety in persons living with HIV: A meta-analysis. Journal of psychosomatic research. 2019 Nov 1;126:109823.
- ↑ Gomes-Neto M, Conceição CS, Carvalho VO, Brites C. A systematic review of the effects of different types of therapeutic exercise on physiologic and functional measurements in patients with HIV/AIDS. Clinics. 2013 Aug;68(8):1157–67.
- ↑ Uebelacker LA, Weisberg RB, Herman DS, Bailey GL, Pinkston-Camp MM, Stein MD. Chronic Pain in HIV-Infected Patients: Relationship to Depression, Substance Use, and Mental Health and Pain Treatment. Pain Medicine. 2015 Oct;16(10):1870–81.
- ↑ Parker R, Jelsma J, Stein DJ. Managing Pain in Women Living With HIV/AIDS. Journal of Nervous & Mental Disease. 2016 Sep;204(9):665–72.
- ↑ Remien RH, Stirratt MJ, Nguyen N, Robbins RN, Pala AN, Mellins CA. Mental health and HIV/AIDS: the need for an integrated response. AIDS (London, England). 2019 Jul 7;33(9):1411-20.