Heart Lung Transplant
Original Editor Rachael Lowe
Top Contributors - Andeela Hafeez, Mereena Baby, Kim Jackson, Lucinda hampton, Rachael Lowe, Vidya Acharya, Admin, WikiSysop, Karen Wilson, 127.0.0.1, Laura Ritchie and Evan Thomas
Description[edit | edit source]
A heart-lung transplant is performed for unsalvagable dual cardiac and pulmonary failure. An organ transplant is an established life-saving therapy for these patients. The most common underlying conditions requiring heart-lung transplants are congenital cardiac diseases with Eisenmenger syndrome and certain pulmonary hypertension disorders[1].[2]
Heart transplantation[edit | edit source]
A pioneering heart surgeon, Dr Christiaan Barnard, performed the first successful human-to-human heart transplant operation in 1967 in Cape Town, South Africa. Unfortunately, early operations resulted in problems such as infection and rejection, and heart recipients did not survive very long.
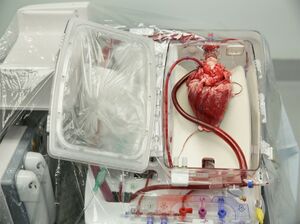
Image: A new method for heart transplantation in Institute for Clinical and Experimental Medicine (IKEM), using a pioneering method of organ retrieval that keeps the heart pumping outside the patient’s body for several hours.[3]
With advances in technique and development of new drugs to suppress the immune system, a majority of transplant recipients currently survive more than 3 years.
- A "bridge" device (assisted device) has been developed that lets certain people live longer while they wait for transplantation. A balloon pump inserted into the aorta, along with battery generator device, that can help the heart to provide blood flow to the body. This “bridge” cannot be used for long and used only in people who are critically ill and very close to getting a new heart.
- A newer procedure involves implanting a mechanical pump into your body to help pump the blood. This pump, called a left ventricular assist device (LVAD), can be used for months or even years. Some devices can be utilized indefinitely.
- Total artificial hearts are now available and have been implanted in a few patients. Besides costs, complications are still present.[4]
Lung transplantation:[edit | edit source]
Successful lung transplantation has been performed since the early 1980s. The first surgeries involved transplanting both lungs and the heart together. Since then, operations have been developed to transplant both lungs, a single lung, and even partial lung (lobes).[4]
Indication[edit | edit source]
A heart-lung transplant is the only treatment available for people who have combined heart and lung failure. It is a treatment that carries high risks but can offer benefits. For this reason, it is only recommended when all other treatment options have failed. If the damage is severe in both organs, replacing the heart or lungs alone may not be possible.
The conditions that most often require a heart-lung transplant are:
- adult congenital heart disease (ACHD) – where an adult has one or more birth defects that affect their heart
- Coronary Artery Disease (CAD), leading to heart attack and permanently damaged heart muscle
- Heart valve disease, such as with damage from rheumatic fever
- Infections of heart tissue, especially heart valves
- Untreated, uncontrolled high blood pressure
- Cardiomyopathies, secondary to multiple causes
- Congenital heart defects (certain heart defects that an individual is born with)
- Certain drugs
- Cystic fibrosis
- Eisenmenger syndrome, which is due to unoperated congenital heart defects
- Idiopathic pulmonary fibrosis
- pulmonary hypertension – where high blood pressure develops inside the blood vessels of the lungs, which can damage both the lungs and the heart.[2]
[edit | edit source]
Acceptable donor criteria are as follows:
- Age younger than 65 years for lung transplantation and younger than 45 years for heart-lung transplantation
- Absence of severe chest trauma or infection
- Absence of prolonged cardiac arrest (heart-lung only)
- Minimal pulmonary secretions
- Negative screens for HIV, hepatitis C, and hepatitis B
- Blood type (ABO) compatibility
- Close match of lung size between donor and recipient
- PaO 2 > 300 mm Hg on 100% fraction of inspired oxygen (FiO2)
- Clear chest radiograph
- No history of malignant neoplasms
Organ rejection:[edit | edit source]
The purpose of your immune system is to protect your health. It recognizes and attacks anything different from the substances normally present in your body, even those only slightly different, like your newly transplanted lung and heart. The immune system does not discriminate between harmful substances, like bacteria, fungi and viruses, and transplanted organs — so to your immune system your new lung and heart appears as a foreign substance that needs to be eliminated.Even with the use of immunosuppressants, your body can at times recognize your transplanted organ as a foreign object and attempt to protect you by attacking it. Rejection is the term used when your body's immune system is attacking your transplanted organ. Nearly all patients will experience at least one episode of rejection. If and when you suffer an episode rejection, remember:
- it does not mean that you will lose your new lung or heart,
- it does not mean your new lung or heart is failing.
Rejection may occur early or late after transplantation. Early rejection occurs most often in the first six months after transplant, and late rejection typically occurs after six months.[5]
Diagnostic Tests[6][edit | edit source]
Heart tests:[edit | edit source]
- echo cardiograph
- cardiac catheterization
- pap test
- mamogram
- prostate exam
- sigmoidoscopy
- bone densitometry
- electrocardiogram
Lung tests:[edit | edit source]
- lung function test
- chest x-ray
- pulmonary function test and arterial blood gas
- blood test
- ABO blood type
- tissue typing
- other blood tests
- ventilation perfusion scan
- ct scan
Pre-Op[edit | edit source]
- Most candidates for transplantation are referred to the program by their primary physician or specialist. Others come to be evaluated at their own initiative. The process begins with a call to the Lung Transplant Office.[7]
- evaluation
- procedure for patient: For some patients, a single lung (one side, "single-lung transplant") is all that is needed. For others, both lungs ("double-lung transplant") or a heart as well as both lungs ("heart-lung transplant") are the best option. Occasionally, the decision about whether a given patient needs one lung or two will be influenced at the time of surgery, by the function of the donor, availability of organs, or the severity illness of the recipient.
- At the end of your pre-transplant evaluation, and after the test results are complete, the Lung Transplant Team will meet to jointly discuss whether or not a lung transplant is an appropriate treatment for you. The transplant coordinator will then notify you of the Team’s decision.
Please understand that abnormal test results might require further investigation. The goal of pre-transplant testing is to ensure that you will be able to undergo the transplant surgery and recover without any significant risk of complications.
If you are approved and are going to be placed on the organ waiting list, the transplant coordinator will tell you what you need to do while you wait for your transplant.[8]
Surgical Technique[edit | edit source]
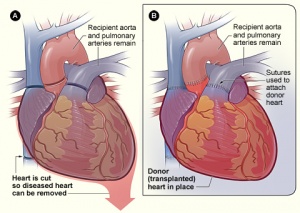
- The recipient's heart is removed but a cuff of right atrium and ascending thoracic aorta distal to semilunar valve is left for anastomosing to the respective parts of the donor's heart. A cuff of the left pulmonary artery is left in its position to protect the integrity of left recurrent laryngeal nerve.
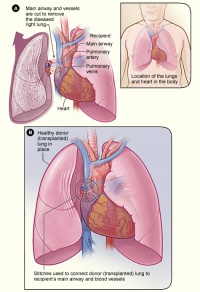
- After this both lungs are dissected, dividing the pulmonary ligament and the hila except the bronchi (intact). The trachea is exposed and just divided above the carina, and the lungs are removed.
- Implantation of donor organs starts with:
- the tracheal anastomosis
- followed by uniting the two aortas
- then the right atrial anastomosis.
- The most crucial and critical part of this procedure is the removal of recipient's heart and lungs without injury to the surrounding nerves like vagus nerve,recurrent laryngeal nerve and phrenic nerve and bronchial arteries.[9]
Post-Op[edit | edit source]
- Monitoring for rejection[10]
- Rejection can frequently be silent and without symptoms, and detected only by lung function testing. This is why we frequently measure your lung function during your hospitalization and at your follow-up clinic visits. In addition, a lung biopsy may be necessary to determine if rejection is actually occurring.
- Pulmonary function tests, a measure of your lung function, will be performed weekly in the 3 months after your transplant, and less frequently thereafter. This test may reveal the first sign of rejection or infection. Your lung function will be followed at home with the measurement of spirometry and peak expiratory flow measurements, which you will record daily at home. Any persistent decrease in these values should be reported to the transplant team.If rejection is suspected, a bronchoscopy, or lung biopsy, will be performed to rule out rejection or see if it is actually occurring.
- Follow-Up Care
- This initially involves returning to the Outpatient Clinic once a week for the first month after leaving the hospital. At this time a series of tests, including blood tests, are conducted to closely monitor the patient's progress. This is a period when medications are precisely adjusted. After this initial period of relatively intensive follow-up, patients are seen periodically as determined by their condition.[7]
- The Patient's Responsibility
- While transplantation can greatly improve the quality of life of the recipients, it also demands much of them. They must become active participants in preserving their health.
- Immunosuppressive Medication
- Transplantation has become so successful in recent years in large part through the development of new drugs, which prevent rejection of donated organs. These drugs inhibit the body's immune system from identifying the new organ as foreign. It is necessary for all patients to take immunosuppressive medication for the rest of their lives following transplant.
Management[11][edit | edit source]
Medical Therapy:[edit | edit source]
- Tacrolimus
- Mycophenolate mofetil
- Cyclosporine
- Azathioprine
Surgical Therapy:[edit | edit source]
- Well-qualified medical and surgical personnel
- Local and readily available support in areas of immunology, pulmonary medicine, infectious diseases, cardiology, and rehabilitation
- Qualified house staff that is available on a 24-h basis
Organ Rejection:[edit | edit source]
We manage a mild rejection episode by making adjustments to your medication dosages. Moderate or severe rejection may require a few days of hospitalization, allowing us to administer alternative immunosuppressants and observe your progress.[10]
Physical Therapy Management:[edit | edit source]
Heart Transplantation:[edit | edit source]
- Breathing Exercises
- Leg and Foot Exercises
Changing Positions in Bed - Sitting, Standing and Walking
Systematic review and meta-analysis showed continuous moderate exercise (CON) or high-intensity interval training improved endothelial function in heart transplant recipients.[12]
DON'Ts:[edit | edit source]
- Do not lift heavier than ten pounds
- Do not push or pull objects heavier than ten pounds unless instructed to do so by your therapist or nurse
- Do not do sit-ups, push-ups, or pull-ups
- Stop any activity that causes pain or pulling across your chest
Lungs transplantation:[13][edit | edit source]
Airway Clearance[edit | edit source]
- The Active Cycle of Breathing
- Breathing Exercises
- Cardiovascular Exercise
- Strengthening Exercises
Lower extremity exercises[edit | edit source]
In bed[edit | edit source]
- Knee to chest
- Hip abduction/adduction (supine)
- Ankle pumps
- Bridging
- Straight leg raise
- Hip abduction in sidelying
In the chair[edit | edit source]
- Hip flexion
- Ankle pumps
- Knee extension
- Sit to stand
In standing[edit | edit source]
- Standing calf lift
- Mini-squat (wall squat)
Upper extremity exercises[edit | edit source]
In bed (on the mat)[edit | edit source]
- Biceps curl
- Triceps curl
- Bench press
- Anterior arm lift
- Strength/Postural Exercises
- Neck and trunk
Shoulder circles;[edit | edit source]
Cervical range of motion; Trunk lateral flexion
Lower extremities[edit | edit source]
- Hamstring stretch
- Calf stretch
6 weeks post surgery[edit | edit source]
- Shoulder flexion overhead
- Shoulder abduction and horizontal abduction standing against wall
- Elbows out into sides with fingers locked behind neck
Case Studies[edit | edit source]
- http://tele.med.ru/book/cardiac_anesthesia/text/ya/ya006.htm
- http://tele.med.ru/book/cardiac_anesthesia/text/ya/ya017.htm
References[edit | edit source]
- ↑ Tully A, Nagalli S. Heart-Lung Transplantation. StatPearls [Internet]. 2020 Jul 5.Available: https://www.statpearls.com/articlelibrary/viewarticle/22669/(accessed 25.4.2021)
- ↑ 2.0 2.1 http://www.nhs.uk/conditions/Heart-lung-transplant/Pages/Introduction.aspxGo to NHS Choices homepageYour health, your choices
- ↑ Pokorná E, Vitko S, Ekberg H. Medical-record review of potential donor pool in the Czech Republic suggests a possible increase to more than double the number of donors. Transplant international. 2003 Sep 1;16(9):633-8.Available:https://english.radio.cz/czech-doctors-perform-first-heart-a-box-transplant-8117525 (accessed 25.4.2021)
- ↑ 4.0 4.1 http://www.emedicinehealth.com/heart_and_lung_transplant/article_em.htm expert for everyday emergancy
- ↑ http://www.columbiasurgery.org/pat/lungtx/guide_immunosuppression.html
- ↑ http://my.clevelandclinic.org/health/treatments_and_procedures/hic-lung-transplant-surgery/hic-lung-transplant-evaluation-required-tests
- ↑ 7.0 7.1 http://umm.edu/programs/transplant/services/lung/what-to-expect
- ↑ http://my.clevelandclinic.org/health/treatments_and_procedures/hic-lung-transplant-surgery/hic-lung-transplant-evaluation-required-tests
- ↑ 7.Cash's Textbook of chest,heart and vascular disorders for physiotherapists,4 th edition,Edited by Patricia A.Downie,Pg No-451
- ↑ 10.0 10.1 http://www.columbiasurgery.org/pat/lungtx/guide_immunosuppression.html
- ↑ http://emedicine.medscape.com/article/429499-treatment
- ↑ de Souza JA, Araújo BT, de Lima GH, de Andrade AD, Campos SL, de Aguiar MI, Carneiro RM, Brandão DC. Effect of exercise on endothelial function in heart transplant recipients: systematic review and meta-analysis. Heart Failure Reviews. 2019 Dec 5:1-8.
- ↑ http://www.columbialungtransplant.org/guide_exercise.html