Cardiomyopathies
Original Editor - Lucinda hampton
Top Contributors - Lucinda hampton, Kim Jackson and Rucha Gadgil
Introduction[edit | edit source]
Cardiomyopathies are abnormalities of the myocardium (heart muscle) with associated cardiac dysfunction, often occurring in families, and can lead to abnormal heart muscle thickening or weakness. Although the majority of these conditions affect adults, changes in the heart can begin in childhood. Some conditions can lead to sudden death, with medical and psychological interventions key to providing the best possible protection and preservation of quality of life. In rare cases, a heart transplant in childhood will be needed[1].[2]
- Cardiomyopathies are a diverse group of cardiac disorders that frequently cause heart failure and death and are now recognized with increasing frequency.
- There has been substantial progress in the clinical recognition and understanding of the natural history of these conditions. Well-established and new techniques of cardiac imaging are helping in this regard. [3]
- Nearly, 50% of patients dying suddenly in childhood or adolescence or undergoing cardiac transplantation are affected by cardiomyopathies.[4]
Cardiomyopathy can be acquired or inherited. Many times, the cause of cardiomyopathy isn’t known. This often is the case when the disease occurs in children[5].
Classification[edit | edit source]
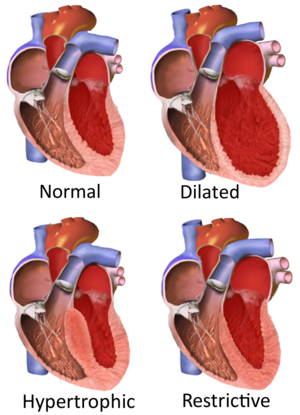
Cardiomyopathy classification separates the various cardiomyopathies into several subtypes. It was classified according to the 1995 World Health Organisation / International Society and Federation of Cardiology (WHO/ISFC) system as follows:
- Dilated cardiomyopathy
- Hypertrophic cardiomyopathy
- Restrictive cardiomyopathy
- Arrhythmogenic right ventricular cardiomyopathy
- Unclassified Cardiomyopathy: Other types of cardiomyopathy are grouped into this category and can include: eg Takotsubo cardiomyopathy/broken heart syndrome.[2]
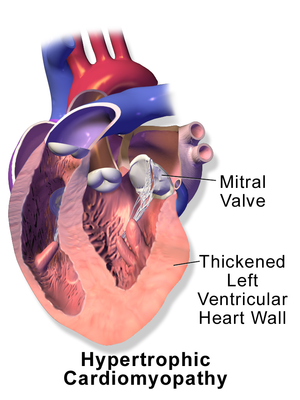
Hypertrophic Cardiomyopathy[edit | edit source]
Hypertrophic cardiomyopathy
- Very common and can affect people of any age.
- Affects men and women equally
- About 1 out of every 500 people has the disease.
- Usually is inherited (caused by a mutation or change in some of the genes in heart muscle proteins).
- Can develop over time because of high blood pressure, aging, or other diseases, such as diabetes or thyroid disease. Sometimes the cause of the disease isn’t known.[5]
Pathophysiology
- Heart muscle enlarges and thickens without an obvious cause.
- Usually the ventricles (the lower chambers of the heart), and septum (wall that separates the left and right side of the heart) thicken.
- The thickened areas create narrowing or blockages in the ventricles, making it harder for the heart to pump blood.
- Hypertrophic cardiomyopathy also can cause stiffness of the ventricles, changes in the mitral valve, and cellular changes in the heart tissue.
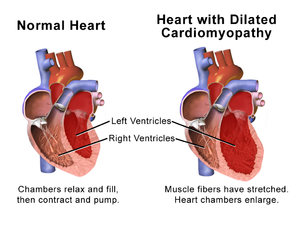
Dilated Cardiomyopathy[edit | edit source]
Dilated cardiomyopathy develops when the ventricles enlarge and weaken. The cause of dilated cardiomyopathy often isn’t known. About one-third of the people who have dilated cardiomyopathy inherit it from their parents.
Pathophysiology:
- Usually starts in the left ventricle and over time can affect the right ventricle.
- Weakened ventricles of the heart don’t pump effectively, causing the heart muscle to work harder.
- Over time, the heart loses the ability to pump blood effectively.
- Dilated cardiomyopathy can lead to heart failure, heart valve disease, irregular heart rate, and blood clots in the heart.
Certain diseases, conditions, and substances also can cause the disease, such as:
- Alcohol, especially combined with a poor diet
- Certain toxins, eg poisons and heavy metals
- Complications during the last months of pregnancy
- Coronary Artery Disease (CAD), heart attack, high blood pressure, diabetes, thyroid disease, viral hepatitis, and HIV
- Illegal drugs, eg cocaine and amphetamines, and some medicines used to treat cancer
- Infections, especially viral infections that inflame the heart muscle
Restrictive Cardiomyopathy[edit | edit source]
Pathophysiology: Restrictive cardiomyopathy develops when the ventricles become stiff and rigid but the walls of the heart do not thicken.
- As a result, the ventricles do not relax and don’t fill with the normal blood volume.
- As the disease progresses, the ventricles do not pump as well and the heart muscle weakens.
- Over time, restrictive cardiomyopathy can lead to heart failure and problems with the heart valves.
Certain diseases, conditions, and factors can cause restrictive cardiomyopathy, including:
- Amyloidosis: A disease in which abnormal proteins build up in the body’s organs, including the heart
- Connective tissue disorders
- Hemochromatosis: too much iron builds up in the body. The extra iron is toxic to the body and can damage the organs, including the heart.
- Sarcoidosis: causes inflammation and can affect various organs in the body. Researchers believe that an abnormal immune response may cause sarcoidosis. This abnormal response causes tiny lumps of cells to form in the body’s organs, including the heart.
- Some cancer treatments, eg radiation and chemotherapy[5]
Arrhythmogenic Right Ventricular Dysplasia[edit | edit source]
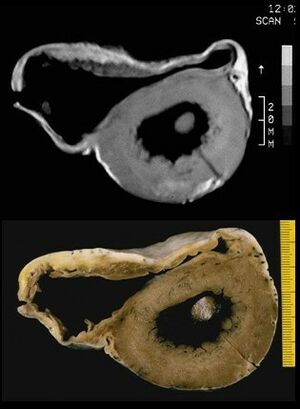
Arrhythmogenic right ventricular dysplasia is a rare type of cardiomyopathy. Researchers think that arrhythmogenic right ventricular dysplasia is an inherited disease.
Image: Arrhythmogenic_right_ventricular_cardiomyopathy. In vitro MRI (c) and corresponding cross section of the heart (d) show RV dilatation with anterior and posterior aneurysms.
Pathophysiology:
- Occurs when the muscle tissue in the right ventricle is replaced with fatty or fibrous tissue.
- Can lead to disruptions in the heart’s electrical signals and causes arrhythmias.
- Arrhythmogenic right ventricular dysplasia usually affects teens or young adults and can cause sudden cardiac arrest in young athletes[5].
Treatment[edit | edit source]
People who have cardiomyopathy but no signs or symptoms may not need treatment whilst other people will need treatment. Treatment depends on the type of cardiomyopathy, severity of symptoms and complications, and age and overall health of person. Treatments may include:
- Heart-healthy lifestyle changes
- Medicines
- Nonsurgical procedure
- Surgery and implanted devices
Surgery and Implanted Devices[edit | edit source]
Doctors use several types of surgery to treat cardiomyopathy, including septal myectomy, surgically implanted devices, and heart transplant.
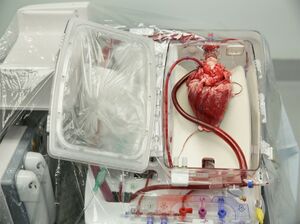
Image: A new method for heart transplantation in Institute for Clinical and Experimental Medicine (IKEM), using a pioneering method of organ retrieval that keeps the heart pumping outside the patient’s body for several hours.[6]
- Septal myectomy is open-heart surgery and is used to treat people who have hypertrophic cardiomyopathy and severe symptoms. This surgery generally is used for younger patients and for people whose medicines aren’t working well. A surgeon removes part of the thickened septum that’s bulging into the left ventricle. This improves blood flow through the heart and out to the body. The removed tissue doesn’t grow back. If needed, the surgeon also can repair or replace the mitral valve at the same time. Septal myectomy often is successful allowing person to return to a normal life with no symptoms.
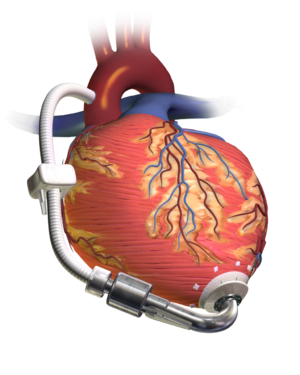
Image: Left Ventricular Assist Device (mechanical pump).
2. Surgeons can place several types of devices in the heart to improve function and symptoms, see Cardiac Implantable Electronic Devices
3.Heart Transplant: A heart transplant is a last resort treatment for people who have end-stage heart failure. ie the condition has become so severe that all treatments, other than heart transplant, have failed[5].
Physiotherapy[edit | edit source]
Advice about exercise is complex. This is because every individual is different in how their condition and exercise affects them, there is little scientific research into the role of exercise in cardiomyopathy and so no definitive advice can be given, and there are legal implications of giving advice.
General recommendations for exercise for people with cardiomyopathy are:
- to participate in 'recreational' (for fun) exercise
- to avoid moderate, intensive or competitive sports
- to avoid exercise that involves sudden bursts of exertion (such as weight lifting, sprinting).
Suitable types of exercise include walking, jogging, easy cycling, swimming, skipping, golf, non-strenuous hiking, tennis, bowling and low-impact aerobics.
Most people with cardiomyopathy will have exercise tests as part of their diagnosis. These tests include:
- Six Minute Walk Test
- Cardiopulmonary Exercise Testing (CPET) In Adults
- Exercise echocardiogram - doing exercise while their heart is being imaged (an 'echo').
- Borg Rating Of Perceived Exertion (Intense exercise on this scale is not recommended for people with cardiomyopathy because it places too much exertion on the heart).
Advice client when exercising that it is important to stop and seek advice from your GP or cardiologist if experiencing:
- Chest pain or tightness.
- Dizzy or light-headedness.
- Breathlessness (dysponea)
- Sudden palpitations (being aware of a change in heart rate or rhythm).
- If any of the symptoms you normally experience become worse when you exercise[7].
Cardiac Rehabilitation has an important role in myopathies. See Link
The Future[edit | edit source]
We look forward to the era when pharmacological and invasive procedures will no longer be the only measures to manage cardiomyopathies, preventing sudden death or cardiac transplantation. It is hoped that further understanding of molecular genetics of cardiomyopathies could well lead to clinical advances[4].
References[edit | edit source]
- ↑ The Conversation Childhood heart disease has a profound impact and is under-recognised Available from:https://theconversation.com/childhood-heart-disease-has-a-profound-impact-and-is-under-recognised-84377 (accessed 24.4.2021)
- ↑ 2.0 2.1 Radiopedia Cardiomyopathies Available from: https://radiopaedia.org/articles/cardiomyopathy-whoisfc-1995-classification(accessed 24.4.2021)
- ↑ Braunwald E. Cardiomyopathies: an overview. Circulation research. 2017 Sep 15;121(7):711-21.Available from:https://www.ahajournals.org/doi/10.1161/CIRCRESAHA.117.311812 (accessed 24.4.2021)
- ↑ 4.0 4.1 McKenna WJ, Maron BJ, Thiene G. Classification, epidemiology, and global burden of cardiomyopathies. Circulation research. 2017 Sep 15;121(7):722-30.Available from: https://www.ahajournals.org/doi/full/10.1161/CIRCRESAHA.117.309711(accessed 24.4.2021)
- ↑ 5.0 5.1 5.2 5.3 5.4 NIH Cardiomyopathies Available: https://www.nhlbi.nih.gov/health-topics/cardiomyopathy (accessed 24.4.2021)
- ↑ Pokorná E, Vitko S, Ekberg H. Medical-record review of potential donor pool in the Czech Republic suggests a possible increase to more than double the number of donors. Transplant international. 2003 Sep 1;16(9):633-8.Available:https://english.radio.cz/czech-doctors-perform-first-heart-a-box-transplant-8117525 (accessed 25.4.2021)
- ↑ Cardiomyopathy UK Available from: https://www.cardiomyopathy.org/physical-health/exercise(accessed 24.4.2021)