Craniocervical Instability in Down Syndrome
Original Editor - Laura Beaman, Beth Potter, Catherine Stanislas, Emily Westwood, as part of the Nottingham University Spinal Rehabilitation Project
Top Contributors - Beth Potter, Angeliki Chorti, Cindy John-Chu, Carina Therese Magtibay, Kim Jackson, Laura Beaman, Naomi O'Reilly and Rucha Gadgil
Introduction[edit | edit source]
Down Syndrome (DS), also known as Trisomy 21, is a condition caused by the presence of an extra chromosome (chromosome 21) which results in atypical physical and cognitive development. It occurs in approximately every 1 in 700 births.[1] Development of secondary health issues such as Craniocervical Instability (CCI) are common within the DS population compared to the general population. Instability of the C0-C1 and C1-C2 joints occur due to malformation of the Axis (C2), specifically the Dens and or laxity of the transverse ligament caused by collagen defects. [2] Both of these structural anomalies allow increased translation of the posterior aspect of the Atlas. The prevalence of CCI in people with DS has been reported to be between 8-63%.[2] CCI can be subdivided in to Occipito-Axial Instability (OAI) also known as Atlanto-Occipital Instability (AOI) and Atlanto-Axial Instability (AAI), affecting 17.5% and between 6.8- 30% of people with DS respectively. [3] [4][5][6] Less than 1-2% of people living with DS who have AAI later develop symptomatic AAI. [5] Symptomatic AAI occurs as a result of excessive cervical movement causing impingement on the spinal cord, with a risk of severe neurological damage if untreated.[4]
Clinically Relevant Anatomy[edit | edit source]
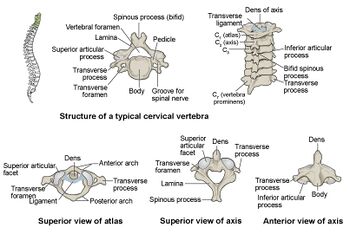
Bones[edit | edit source]
- Occiput (inferior aspect of the skull)
- Atypical Vertebrae:Atlas (C1) & Axis (C2)
- Typical Vertebrae: C3-C7
Joints[edit | edit source]
- Atlanto-occipital (C0/C1)
- Atlanto-axial (C1/C2)
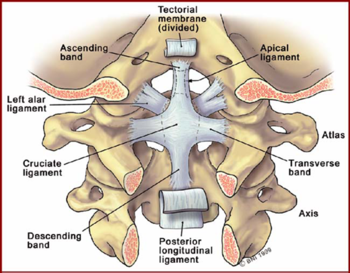
Ligaments[edit | edit source]
- Occipitoatlantoaxial ligaments:Apical, Alar, Transverse & Accessory Atlanto-axial
- Vertebral ligaments:Nuchal, Supraspinous, Interspinous, Anterior Longitudinal, Posterior Longitudinal, Intertransverse & Ligamentum Flavum
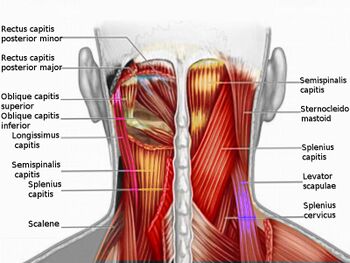
Muscles[edit | edit source]
- Longus Capitis
- Longus Colli
- Rectus Capitis Anterior
- Rectus Capitis Lateralis
- Scalenes
- Splenius Capitis
- Splenius Cervicis
- Upper Trapezius
- Levator Scapulae
See Cervical Anatomy page for more information.
Overview of Pathology[edit | edit source]
Occipito-axial Instability in Down Syndrome[edit | edit source]
Occipito-Axial Instability (OAI) is less researched in the DS population compared to AAI. Bony abnormalities such as undeveloped occipital condyles and superior articular facets of C1 can cause such instability due to decreasing joint congruency.[10]
Ligament laxity has been cited as another explanation for OAI - specifically retropharyngeal ligament laxity.[11]
Atlanto-axial Instability in Down Syndrome[edit | edit source]
Atlanto-axial instability (AAI) is defined as an increased distance between the posterior aspect of the frontal arch of C1 and the anterior aspect of the dens (otherwise known as the odontoid peg) of C2 when measured on radiographs taken in the neutral position.[12] A distance of more than 5mm between the dens and the anterior arch of C2 is considered an abnormality. [3][13][14][15][16]
It can occur as a result of increased movement at the Atlantoaxial joint (the atlas and axis joint articulation).[17] The instability arises from bony abnormalities and ligament laxity of the Atlantoaxial joint.[18]
The causes for such ligament laxity have previously been cited as being due to intrinsic collagen defects and/or a chronic inflammatory state which weakens the ligaments.[2] Lax ligaments allow for more movement between the articulating vertebral bodies. Specifically, the laxity of the transverse ligament, which keeps the dens close to the anterior arch of the atlas, is the primary cause.[16]
In terms of bony abnormalities, those concerning the dens are the most commonly cited. For example, odontoid hypoplasia and the presence of accessory ossicles.[16] Odontoid hypoplasia meaning underdevelopment of the odontoid peg and accessory ossicles implies there are secondary ossification centres that remain separate from the adjacent bone (usually round or ovoid in shape). Odontoid hypoplasia may cause slippage of the transverse ligament over the superior aspect of the shortened odontoid peg.[16]
AAI becomes symptomatic when the displaced dens impinges on the spinal cord. [16]
Signs and Symptoms[edit | edit source]
Symptoms associated with AAI and OAI include:
- Neck pain/discomfort [5][16][19]
- Myelopathy [5][20]
- Abnormal head posture [19][21]
- Abnormal gait[16][19]
- Change in sphincteric control [16]
- Decreased neck range of movement (RoM) [19]
- Frequent falls [19]
- Increased fatigue on walking[19]
Differential Diagnosis[edit | edit source]
A thorough assessment of the cervical spine should be completed in order to distinguish the cause of neck pain and presenting symptoms. Despite the higher prevalence of CCI among the DS population, the signs and symptoms are not unique to this condition, therefore the following should be considered as a potential cause: [22]
- Cervical Trauma
- Cervical Canal Stenosis
- Cervical Ligament Injury
- Cervical Radiculopathy
- Cervical Spondylosis
- Degenerative Disc Disease
- Disc Herniation
- Juvenile Disc Disorder
- Torticollis
Examination and Screening[edit | edit source]
Atlanto-axial Instability Screening[edit | edit source]
Plain Lateral Cervical Radiographs[edit | edit source]
There is limited evidence to support the use of plain radiography as a screening tool for asymptomatic AAI. Lateral cervical radiographs can be conducted with the individual in neck flexion, extension and neutral position. The distance between the posterior surface of the frontal arcus of C1 and the anterior surface of C2 Dens is measured, otherwise known as the anterior atlanto-odontoid distance (AAOD). However, there are large discrepancies in diagnostic criterial for AAI, with AAI being defined by an AAOD ranging from 3mm-4.5mm across studies.[3] [13] [14][15] [16] Several authors have concluded that routine screening using lateral radiographs are not necessary due to the variation in diagnostic criteria, technical difficulties conducting the measurements, [23] the likelihood of AAI decline throughout an individuals' life [24] and the occurrence of symptomatic AAI being extremely rare.[17] Furthermore, Selby et al.[15] found radiographs of the cervical spine was an unreliable and insensitive screening tool in identifying atlantoaxial subluxation in children (aged 6-14 years) with DS.
From a sport participation screening perspective, Cremers et al. [23] studied 91 children and young adults (4-20 years old) with DS presenting with asymptomatic AAI (>4mm). Participants were randomly assigned to one of two groups. Group one continued with usual sport and exercise and the other group avoided sports deemed 'risky' for a year. Results showed no differences between groups in functional motor scale, neurological signs or atlantoaxial distance, concluding that plain radiographic pre-participation screening is unnecessary for asymptomatic AAI. [23]
Non-Radiographic Assessment and Screening[edit | edit source]
British Gymnastics established their own screening criteria for individuals with DS who wish to participate in gymnastics activity (including trampolining).[25] Despite being developed as a screening tool for gymnastics, it has wider application to other sports and physical activity.[18]
A qualified medical practitioner or chartered physiotherapist must complete the following tests: [25]
- Does the person show evidence of progressive Myelopathy? (Yes/No)
- Does the person have poor head/neck muscular control?* (Yes/No)
- Does the person's neck flexion allow the chin to rest on their chest? (Yes/No)
If an individual has a positive test for the first two questions or a negative test for question three, the person should be excluded from participation in gymnastic activity.
- *The neck can be assessed by laying the individual on their back with legs straight, the examiner stands in front of the person and pulls the individual into a sitting position using their hands.
The assessing clinical practitioner should be aware of the signs of progressive Myelopathy and address them during a subjective and objective exam, including: [25]
- Increase in muscle weakness
- Decrease in co-ordination
- Change in gait
- Loss of sensation
- Paraesthesia
- Altered muscle tone
- Recent onset of Urinary Incontinence
Additionally, an in-depth subjective history of a person with DS should be undertaken by a qualified health professional before sport participation; ideally a practitioner familiar with the individual's baseline function.[18][23] Further, Morton et al.[24] have previously recommend a gait assessment and neurological examination including tendon reflexes and plantar responses for AAI screening. Neurological examination is promoted as an alternative to radiographs due to the lack of correlation between X-Ray and neurological findings.[3] [6]
There are manual tests to measure cervical instability, however, there is a paucity of evidence regarding their diagnostic accuracy:
Collectively, after a detailed subjective history, [23] neurological exam, [24] assessment of neck control and use of the British Gymnastics screening tool, [25] an individual will either have unrestricted sport participation or an adapted, more restricted sport participation (if results indicate symptomatic cervical instability). [18]
Atlanto-Occipital Instability Screening[edit | edit source]
Plain Lateral Cervical Radiographs[edit | edit source]
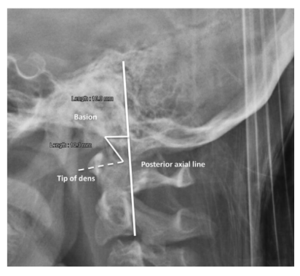
As for AAI, AOI is diagnosed following a lateral cervical X-Ray that must encompass the base of the skull and upper cervical spine (C0-C2). The Rule of 12, otherwise known as the Harris measurement, is used to diagnose AOI. [3]
The Rule of 12 uses the basion-dens interval (BDI) values, with the BDI being the distance from the inferior basion and the superior aspect of the dens. Measurements >12mm indicates AOI or a degree of Atlanto-occipital dissociation.[3]
The consensus statement of the Spine Trauma Study Group concluded that the Rule of 12 is the most sensitive and replicable method in diagnosing AOI in Down Syndrome. [26]
Outcome Measures[edit | edit source]
- Neck Disability Index
- Neck Pain and Disability Scale
- Patient Specific Functional Scale
- Neck Bournemouth Questionnaire
- Measurement of the horizontal displacement and angular displacement of the cervical vertebral body on lateral X‑ray films [27]
Management[edit | edit source]
Surgical Management[edit | edit source]
As many long-term follow-up studies show spontaneous stabilisation of the C1-C2 segment, there is not a demand for the provision of symptom-free stabilisation surgery.[28]
Indications for surgical interventions: [29]
- Neurological manifestations caused by spinal cord compression
- Presence of radiographic signs of obvious AAI. (However, when radiographic signs are present without clinical manifestations, then exclusion of the child's participation in contact sports and annual radiologic examinations are recommended)[28]
- Reduced space around the spinal cord
- Basilar impression
Common surgical fixation strategies are: non-instrumented wiring; wiring with rods; screw fixation; hook and rod fixation; and screw and wire fixation. [30] In addition to fixation, posterior decompression ie. resection of the posterior arch, may be used as a form of surgical management. The goal of these surgeries being to ameliorate symptoms; stabilise the damaged upper cervical segments; and to eliminate spinal stenosis. [31]
Outcomes:
A retrospective study with a population of 131 patients, specifically identifying outcomes of atlantoaxial fusion in paediatric patients found a rate of failed fusion in 11%, instrumentation failure in 2%, and graft failure in 8%. [32] When identifying factors predictive of fusion failure, the singular significant factor was DS. [32]
However, the outcomes of surgical interventions in individuals with marked instability has large complication rates, and rarely leads to amelioration of neurological symptoms. [28]
Conservative Management[edit | edit source]
When management is conservative, routine radiological screening for asymptomatic patients remains imperative, allowing regular reassessment of the management plan.[19]
It is important to ensure education is provided to those with DS, family members and professionals involved with this patient group. Increased awareness of the potential signs and symptoms of symptomatic AAI needs to be raised in these populations.
Physiotherapy Management[edit | edit source]
Strengthening: Neck conditioning exercises should be generally promoted among the DS population. [5]
Proprioceptive Exercises: Proprioceptive exercises play an important role in promoting both dynamic and functional joint stability.[33][34]
Education: Increased awareness of the potential signs and symptoms of symptomatic AAI needs to be raised among patients with DS, family members, and professionals involved with managing this group of patients. [18]
Guidelines for Sport[edit | edit source]
Sport and physical activity are highly beneficial for people with DS in regards to biological, psychological and social spheres. [18] Although the risk of damage to the spinal cord in individuals with AAI during sport is extremely rare, [4] precaution must be taken when advising or prescribing exercise to people with DS with AAI in order to mitigate risk of neurological injury.
At present, special olympics athletes must undergo obligatory X-Ray screening, from which a decision is made whether an athlete can participate. [35] However, Myśliwiec et al. [6] argue the need for a revision in rules to exclude X-Ray screening and introduce neurological examinations instead, as a safer and more cost-effective method of pre-participation sporting assessment.
Overall, pre-participation screening of the neck and neurological exam, as previously outlined, [24][25] is advised before an individual with DS can part take in unrestricted sporting activity.
Sports that are considered high risk of causing symptomatic AAI, and therefore should be avoided or undertaken with extreme caution in the asymptomatic AAI Down Syndrome population, are as follows: [17][18]
- Gymnastics
- Trampolining
- Diving (including diving starts during swimming)
- Butterfly stroke during swimming
- Pentathlon
- Any contact sport such as rugby, football and martial arts
- High jump
Any sport should be undertaken with appropriate supervision in order to facilitate safe sporting participation.[18]
All participants and those involved in the individual's care (such as family, health care and sporting or coaching professionals) should be acutely aware of the aforementioned signs and symptoms of symptomatic AAI. If symptomatic AAI is suspected, the individual's spine should be immobilised and they must be taken to an emergency department for immediate screening. From there, a thorough neurological examination should be commenced by a healthcare professional alongside a radiographic or spinal MRI. [13]
References[edit | edit source]
- ↑ Mai C., Isenburg J., Canfield M., Meyer R., Correa A., Alverson C., Lupo P., Riehle‐Colarusso T., Cho S., Aggarwal D., Kirby R. National population‐based estimates for major birth defects, 2010–2014. Birth defects research. 2019 Nov 1;111(18):1420-35.
- ↑ 2.0 2.1 2.2 Hankinson T., Anderson R. Craniovertebral junction abnormalities in Down syndrome. Neurosurgery. 2010 Mar 1;66(suppl 3):A32-8.
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 3.6 El-Khouri M., Mourao M., Tobo A., Battistella L., Herrero C., Riberto M. Prevalence of atlanto-occipital and atlantoaxial instability in adults with Down syndrome. World neurosurgery. 2014 Jul 1;82(1-2):215-8.
- ↑ 4.0 4.1 4.2 Nakamura N., Inaba Y., Aota Y., Oba M., Machida J., Aida N., Kurosawa K., Saito T. New radiological parameters for the assessment of atlantoaxial instability in children with Down syndrome: the normal values and the risk of spinal cord injury. The Bone & Joint Journal. 2016 Dec;98(12):1704-10.
- ↑ 5.0 5.1 5.2 5.3 5.4 Nader-Sepahi A., Casey A., Hayward R., Crockard H., Thompson D. Symptomatic atlantoaxial instability in Down syndrome. Journal of Neurosurgery: Pediatrics. 2005 Sep 1;103(3):231-7.
- ↑ 6.0 6.1 6.2 Myśliwiec A., Posłuszny A., Saulicz E., Doroniewicz I., Linek P., Wolny T., Knapik A., Rottermund J., Żmijewski P., Cieszczyk P. Atlanto-axial instability in people with Down’s syndrome and its impact on the ability to perform sports activities–a review. Journal of Human Kinetics. 2015 Nov 22;48:17.
- ↑ 'The Vertebral Column'. Lumen Learning. [online]. Available at: https://courses.lumenlearning.com/ap1/chapter/the-vertebral-column/ [Accessed 18 May 2021]
- ↑ Garrett M., Consiglieri G., Kakarla U., Chang S., Dickman C. Occipitoatlantal dislocation. Neurosurgery. 2010 Mar 1;66(suppl_3):A48-55.
- ↑ Stathakios J., Carron M. Anatomy, Head and Neck, Neck Triangle. StatPearls [Internet]. 2020 Jul 31.
- ↑ Rodrigues M., Nunes J., Figueiredo S., de Campos A., Geraldo A. Neuroimaging assessment in Down syndrome: a pictorial review. Insights into Imaging. 2019 Dec;10(1):1-3.
- ↑ Arumugam A., Raja K., Venugopalan M., Chandrasekaran B., Kovanur Sampath K., Muthusamy H., Shanmugam N. Down syndrome—A narrative review with a focus on anatomical features. Clinical Anatomy. 2016 Jul;29(5):568-77.
- ↑ Jusabani M., Rashid S., Massawe H., Howlett W., Dekker M.. A case report of atlanto-axial instability in a Down Syndrome patient. Spinal Cord Series and Cases. 2018 Nov 28;4(1):1-5.
- ↑ 13.0 13.1 13.2 Cohen W. Current dilemmas in Down syndrome clinical care: Celiac disease, thyroid disorders, and atlanto‐axial instability. In: American Journal of Medical Genetics Part C: Seminars in Medical Genetics 2006 Aug 15 (Vol. 142, No. 3, pp. 141-148). Hoboken: Wiley Subscription Services, Inc., A Wiley Company.
- ↑ 14.0 14.1 Roy M., Baxter M., Roy A. Atlantoaxial instability in Down syndrome-guidelines for screening and detection. Journal of the Royal Society of Medicine. 1990 Jul;83(7):433-5.
- ↑ 15.0 15.1 15.2 Selby K., Newton R., Gupta S., Hunt L. Clinical predictors and radiological reliability in atlantoaxial subluxation in Down's syndrome. Archives of Disease in Childhood. 1991 Jul 1;66(7):876-8.
- ↑ 16.0 16.1 16.2 16.3 16.4 16.5 16.6 16.7 16.8 Ali F., Al-Bustan M., Al-Busairi W., Al-Mulla F., Esbaita E. Cervical spine abnormalities associated with Down syndrome. International Orthopaedics. 2006 Aug;30(4):284-9.
- ↑ 17.0 17.1 17.2 Committee on Sports Medicine and Fitness. Atlantoaxial instability in Down syndrome: subject review. Pediatrics. 1995 Jul 1;96(1):151-4.
- ↑ 18.0 18.1 18.2 18.3 18.4 18.5 18.6 18.7 Tomlinson C, Campbell A, Hurley A, Fenton E, Heron N. Sport preparticipation screening for asymptomatic atlantoaxial instability in patients with Down syndrome. Clinical Journal of Sport Medicine. 2020 Jul 1;30(4):293-5.
- ↑ 19.0 19.1 19.2 19.3 19.4 19.5 19.6 Foley C., Killeen O. Musculoskeletal anomalies in children with Down syndrome: an observational study. Archives of Disease in Childhood. 2019 May 1;104(5):482-7.
- ↑ Wadhwa R., Mummaneni P. High cervical instability in adult patients with Down syndrome. World Neurosurgery. 2015 Mar;83(3):332-3.
- ↑ Dumitrescu A., Moga D., Longmuir S., Olson R., Drack A. Prevalence and characteristics of abnormal head posture in children with Down syndrome: a 20-year retrospective, descriptive review. Ophthalmology. 2011 Sep 1;118(9):1859-64.
- ↑ Yang S., Boniello A., Poorman C., Chang A., Wang S., Passias P., A review of the diagnosis and treatment of atlantoaxial dislocations. Global Spine Journal. 2014; 4(3):197–210.
- ↑ 23.0 23.1 23.2 23.3 23.4 Cremers M., Bol E., De Roos F., Van Gijn J. Risk of sports activities in children with Down's syndrome and atlantoaxial instability. The Lancet. 1993 Aug 28;342(8870):511-4.
- ↑ 24.0 24.1 24.2 24.3 Morton R., Khan M., Murray-Leslie C., Elliott S. Atlantoaxial instability in Down's syndrome: a five year follow up study. Archives of Disease in Childhood. 1995 Feb 1;72(2):115-9.
- ↑ 25.0 25.1 25.2 25.3 25.4 British Gymnastics. Atlanto-Axial Instability Information pack. [ebook] Newport: British Gymnastics 2018. Available from: https://www.british-gymnastics.org/technical-information/discipline-updates/disabilities/11985-atlanto-axial-instability-information-pack-2021/file [Accessed 08/03/2023].
- ↑ 26.0 26.1 Bono C., Vaccaro A., Fehlings M., Fisher C., Dvorak M., Ludwig S., Harrop J. Measurement techniques for upper cervical spine injuries: consensus statement of the Spine Trauma Study Group. Spine. 2007 Mar 1;32(5):593-600.
- ↑ Alizada M., Li R., Hayatullah G. Cervical instability in cervical spondylosis patients. Der Orthopäde. 2018 Dec;47(12):977-85.
- ↑ 28.0 28.1 28.2 Khusainov N., Vissarionov S., Kokushin D. Craniocervical instability in children with Down’s syndrome. Pediatric Traumatology, Orthopaedics and Reconstructive Surgery. 2016 Sep 15;4(3):71-7.
- ↑ Pizzutillo P., Herman M. Cervical spine issues in Down syndrome. Journal of Pediatric Orthopaedics. 2005 Mar 1;25(2):253-9.
- ↑ Hofler R., Pecoraro N., Jones G. Outcomes of surgical correction of atlantoaxial instability in patients with Down syndrome: systematic review and meta-analysis. World Neurosurgery. 2019 Jun 1;126:e125-35.
- ↑ Hedequist D., Bekelis K., Emans J., Proctor M. Single stage reduction and stabilization of basilar invagination after failed prior fusion surgery in children with Down's syndrome. Spine. 2010 Feb 15;35(4):E128-33.
- ↑ 32.0 32.1 Brockmeyer D., Sivakumar Ã., Mazur Ã., Sayama C., Goldstein H., Lew S., Hankinson T., Anderson R., Jea A., Aldana P., Proctor M. Identifying Factors Predictive of Atlantoaxial Fusion Failure in Paediatric Patients: Lessons Learned from a Retrospective Paediatric Craniocervical Society Study. Cervical Spine 2018; 43(11):754-60.
- ↑ Lee A., Lin W., Huang C. Impaired proprioception and poor static postural control in subjects with functional instability. Journal of Exercise Science and Fitness. 2006;4(2):117-25.
- ↑ Hagert E. Proprioception of the wrist joint: a review of current concepts and possible implications on the rehabilitation of the wrist. Journal of Hand Therapy. 2010 Jan 1;23(1): 2-17.
- ↑ Special Olympics. Special Olympics Official General Rules. 2015 [ebook] Washington: Special Olympics. Available from: https://media.specialolympics.org/resources/leading-a-program/general-rules/Special-Olympics-General-Rules-Amended-2015-8-17.pdf [Accessed 08/03/2023].