The Effects of Walking on Low Back Pain
Top Contributors - Toby Stowe, Angeliki Chorti, Khloud Shreif and Cindy John-Chu
Introduction[edit | edit source]
Low back pain (LBP) that is not associated with serious or potentially serious causes has been described in the literature as 'non-specific', 'mechanical', 'musculoskeletal', or 'simple' LBP.[1] Non-specific LBP is defined as LBP not attributable to a recognisable specific pathology (eg, infection, tumor, osteoporosis, fracture, structural deformity, inflammatory disorder, radicular syndrome, or cauda equina syndrome).[2]
LBP can be further split into three categories; acute, sub-acute, and chronic.[3]
- Acute is anything that persists for less than 6 weeks.
- Sub-acute is anything persisting between 6-12 weeks.
- Chronic is anything persisting for 12 weeks or more.
LBP is commonly described to be between the anatomical regions of the ribs and gluteal folds.[4]
Anatomy[edit | edit source]
The lumbar spine comprises the lower end of the spinal column between the last thoracic vertebra (T12) and the first sacral vertebra (S1). There is a total of five lumbar vertebrae (L1-L5) that are much larger compared to other regions within the vertebral column. These large facets help support the upper body, as they absorb axial forces (against gravity) delivered from the head, neck, and trunk, and provide protection for the spinal cord from the canal that is formed. The lumbar spine allows for diverse types of trunk motion, including flexion, extension, rotation, and side bending, thus providing further reasons as to why the facets are much larger. Each lumbar segment consists of multiple components; vertebral body, transverse process, super articular process, super articular facet, intervertebral disc, vertebral forearm, the pedicle of the vertebral arch, lamina of the vertebral arch, and a spinous process.[5]
Due to the complex structure of spinal components, discs, intervertebral joints, muscles, and nerves, LBP can present with the same symptoms from different causes.
Epidemiology[edit | edit source]
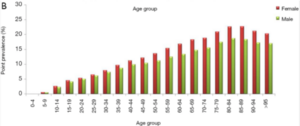
LBP causes more disability than any other condition, affecting 1 in 10 people and becoming more common with increasing age, [1]with rates of 1%–6% in children aged 7–10 years, 18% in adolescents, and a peak prevalence ranging from 28% to 42% in people between 40 years and 69 years.[6] The prevalence of LBP is thought to be increasing due to an increasing and aging population [7] with estimates of life time prevalence being as high as 84% in the adult population. [8]
One study that was carried out in 195 countries assessing the incidence, prevalence, and years lived with disability for 354 medical conditions found LBP to be the leading cause of worldwide productivity loss as measured in years, and the top cause of years lived with disability in 126 countries.[6] In the United Kingdom (UK), it is estimated that LBP is responsible for 37% of all chronic pain in men and 44% in women and the total cost of LBP to the UK economy is reckoned to be over £12 billion per year. [1]
Risk factors for LBP are age, sex, height, weight, sedentary lifestyle, depression, anxiety, insomnia, and smoking.[10] Although muscle strain and imbalance, ligament sprain, and soft tissue damage account for almost all LBP, as it is non-specific, it often has no identifiable underlying condition or origin. [11]
Office workers are usually required to sit for long hours working on a computer while spending most of their time in a sitting position. Approximately 34%- 51% of office workers experienced LBP in the preceding 12 months. Occupational groups exposed to 'poor postures' while sitting for longer than half a day have a considerably increased risk of experiencing LBP. Subjects with LBP are likely to be in sustained postures and have large and infrequent spinal movements. Prolonged postural loading of the spine while sitting can reduce joint lubrication, fluid content of intervertebral discs, and increased stiffness. Additionally to this, prolonged muscle activation in static sitting may lead to localised muscle tension, muscle strains, muscle fatigue, and other soft-tissue damage, causing impairment of motor coordination and control as well as increased mechanical stress on ligaments and intervertebral discs.[12]
Prevalence of walking in the United Kingdom:
- People made an average of 236 walking trips and walked an average of 220 miles.
- People on average have walked less than in 2019, following a fall in short walks.
- People walked 7% farther in 2020 compared to 2019.
- 67% of adults in England reported walking at least once a week.
- 92% of local authorities had at least 60% of their adult population walking at least once a week.
The NHS provides a guide on 'walking for health', to help motivate the population and help them meet the recommended minimum moderate activity guidelines of 150 minutes.
Pedometer Driven Walking[edit | edit source]
Pedometers are devices that work by counting the steps someone takes to estimate the distance they have traveled. [13] Pedometers are usually worn at the hip (on the waistband of clothing) and in alignment with the patella although this may not be the case for all pedometers. There are also other ways of tracking steps - many people now have fitness trackers which are attached to the wrist and will also have the ability to count steps.
Instructions will be included with pedometer devices, and as there are many different types it is important to check these before usage to ensure that the pedometer is being used as accurately as possible. Some pedometers may also be more complex and do a little bit more than just counting steps such as showing calories burned, activity times, and memory logs.
Whilst not a pedometer in the traditional sense, the NHS (National Health Service) also has an application which is free to download called 'Active 10' - this is designed to track walking and will indicate the total amount walked and how much of that was brisk walking. Within the app, there are also options to set goals, achieve milestones, and view progress over the weeks and months. So a pedometer is not the only option to keep a track of walking and daily activity - there are many more apps out there that will do the same thing!
Using an app as a pedometer or walking tracker does rely on the individual having a mobile phone and keeping it in their pocket to ensure it tracks all activity whereas a standard pedometer can be used by a wider number of people and may not be as complex.
Do Pedometers Increase Physical Activity?[edit | edit source]
The NICE (National Institute for Health and Care Excellence) guidelines on LBP and sciatica in over 16s - published in 2016 and last updated in 2020 - advises self-management and exercise as treatments. [1]A pedometer would be an easy way of giving someone a tool to help self-manage their activity levels, as long as this was an appropriate choice of exercise for the individual - those with LBP should be encouraged to continue with their regular activities as well. [1]
A three-arm cluster, randomised control trial (RCT) conducted in 2016 with an eventual number of participants at 956 recruited from primary care settings, found that a pedometer-based walking intervention (regardless of whether there was nurse support) increased the step count and physical activity of generally inactive 45-75 year old at a 12 month follow up. [14]A meta-analysis in 2009 of pedometer-based interventions for activity conducted in 2013 included 32 studies and found using pedometers to have a positive effect on physical activity and this was regardless of age or intervention length.[15] The studies had varying interventions from keeping a daily log of steps, completing 10,000 steps, individualized goals, or a combination of strategies.[15]
Do Pedometers Affect LBP?[edit | edit source]
Acute Low Back Pain (ALBP)[edit | edit source]
There is arguably less research in relation to ALBP and the effects of using a pedometer. However, a study in 2015, focusing on those with ALBP of 48 hours or less looked at whether 'stay active' advice or 'adjusting activities to pain' had different effects. [16] Participants were aged between 18 and 65 and all were provided with a pedometer to track daily steps with the instruction of wearing it at all times during waking hours, they found the pedometer an easily used intervention which increased physical activity, particularly in those with the advice to 'stay active'.[16] This study shows that pedometers could have a useful place in treatment alongside other advice and management techniques for those with ALBP despite the study being over a short period of time, and the study size is relatively small.
Chronic Low Back Pain (CLBP)[edit | edit source]
As previously mentioned, CLBP accounts for a significant amount of chronic pain in individuals of the UK, so interventions that aid in the treatment and management would be beneficial. A recent RCT published in 2021, looked at the effects of a pedometer-driven individualized walking plan compared to standardised care in increasing completion and adherence of physical activity in CLBP management.[17]Whilst no significant difference was noted in disability or pain, there was an indication that using an individualised, guided pedometer program aided in adherence and participation of physical activity - although relevant measures such as step count were not taken from the standardised care group, so it is unclear if there were any increases in physical activity amongst them.[17]
A previous RCT from 2013, of an internet-based pedometer intervention, did find that in the short-term of 6 months back pain disability had decreased, but at 12 months there was no difference between the group with access to the internet support and the ones utilising the pedometer and standard management only.[18]Again, this shows, that whilst pedometer-driven walking can have positive effects in physical activity and adherence, there may need to be further research to explore how positive outcomes can be gained in the long term.
It seems that pedometers can be a relatively cheap and accessibly form of intervention and management in individuals with LBP, and this can have greater positive impacts when included with support in one form or another.[16]
Benefits of Walking on Low Back Pain[edit | edit source]
The lower back muscles play an important role in maintaining its stability and movement; two key aspects that are needed when walking. [19] These muscles can become deconditioned in those with sedentary lifestyles, leading to weakness over time. This prolonged weakness can increase muscular fatigue, and injury, exaggerating the pain already being experienced. [19] Reduced physical activity can also cause these muscles and the joints of the lumbar spine to become stiff, which can increase the pressure on the lower back. [20]
Walking has many positive impacts on the lower back, which can prevent or reduce these changes occurring in the following ways:
- Increased blood flow:
- Small blood vessels and capillaries in the lower back muscles can become constricted following decreased physical activity, reducing the blood flow to these muscles.
- Walking allows for more movement in these muscles, allowing these capillaries and blood vessels to open up again.
- This, in turn, increases the blood supply and nutrients to these muscles, improving muscular health and strength and aiding with the healing process. [20]
- Stretch and contraction of muscles:
- The movement in the lower back during walking increases the stretch and contraction of the lower back muscles and those in the legs, buttocks, and core, allowing for more flexibility and mobility in this area.
- This flexibility increases the overall range of motion in the lower back, also improving the health and strength of the lower back muscles.
Treatment and Management[edit | edit source]
Effect Of Walking On LBP[edit | edit source]
Current evidence supports the use of walking as a treatment option for LBP. A cross-sectional study from 2017 evaluating the relationship between walking and LBP, consisting of 5,982 adults, found that walking was associated with a reduced risk of LBP. [22] The authors also found that the presence of LBP was proportionate to walking frequency, with those who walked more often having reduced LBP. These results are supported by those of a systematic review from 2019 evaluating the effects of walking on those with chronic LBP. [23] Walking was found to be as effective as other non-pharmacological interventions on pain and disability in short-term (<3 months) and intermediate (3-12 months) follow-ups. These findings allowed for walking to be recommended for managing and treating LBP. [23]
The effects of walking have been compared to the effects of exercise for LBP. A systematic review from 2019 comparing the two concluded that walking was as effective as exercise for improving pain, disability, quality of life, and fear-avoidance in those with chronic LBP. [24] Much like the studies by Kim et al. [22] and Sitthipornvorakul et al. [23], Vanti et al. [24] recommend the use of walking as a treatment and management option for LBP.
Interestingly, a systematic review from 2022, found that people with LBP have altered gait patterns compared with healthy individuals. [25] Those with LBP were found to walk slower, have reduced stride lengths, greater lumbar paraspinal activation, and reduced thorax/pelvic coordination. [25] However, the authors were unable to report if these changes were adaptive or maladaptive. Overall, these results indicate that gait re-education may be needed for those with LBP to gain the most benefits from walking.
A systematic review in 2015 included seven randomised controlled trials involving 869 participants adults with chronic LBP. It compared walking to other non-pharmacological management methods such as usual care, specific strength exercises, medical exercise therapy, or supervised exercise classes. It suggested that walking is the same effective as other management methods while having a lower cost. [26]. It could be explained by its high accessibility, but does not require training, supervision, or specialised equipment. [26]
Other research supported that walking is as effective as conventional physiotherapy treatment such as lumbar stabilisation and muscle strengthening exercise. [27][28] A randomised control trial included 48 participants comparing the effect of lumbar stabilisation exercise and walking exercise on LBP. It suggested both interventions significantly reduced LBP, and both interventions show similar results.[28] Another randomised control trial compare strengthening exercise to a combined programme of strengthening exercise and walking exercise on chronic LBP. It suggested that both interventions were beneficial but combined exercise programme was more effective for reducing pain levels than the strength exercise. [27]Another randomised control trial also supported 44 participants comparing conventional physiotherapy to a combination of conventional physiotherapy with walking exercise. It suggested that a combination of conventional physiotherapy with walking exercise is more effective to reduces pain and kinesiophobia, and improved function in patients with subacute and chronic non-specific LBP. [29]
How to Use Walking as a Treatment for LBP[edit | edit source]
1. Combine with conventional physiotherapy treatment[edit | edit source]
Walking is a low-cost intervention, and a combination of physiotherapy with walking is more effective than conventional physiotherapy alone. [26][27][29] Walking exercise could be educated by physiotherapists alongside their exercise prescription. Recommendations support the use of exercise for at least 15 to 30 minutes most days for those with LBP. [30] This can mean gradually building up walking distance and capacity to reduce the risk of injury and allow for the body to adapt to the changes.
2. Goal setting[edit | edit source]
The use of a pedometer means that the patient is able to manage and keep track of their steps whilst walking. The patient might be advised to keep an "activity diary" which keeps track of a daily step count and the patient's step goal. This is achieved by calculating the patient's average step count in the first week of activity, and using this as a baseline when deciding a step goal for the second week. [31] The use of an activity diary can also help establish the patients' baseline in the first week, which is important in informing their individual goals for rehabilitation. [31]
For example, use pedometer/tracking apps (like Active 10) to monitor and then set weekly targets (increase by a certain amount each week/two weeks for example).
3. Postural Control[edit | edit source]
Having the correct walking posture is important to allow for more comfortable walking, helping to reduce pain and discomfort. An optimal posture can be achieved using multiple strategies:
- Stand up straight:
- This can be achieved by making yourself as tall as possible, without leaning forwards or backward.
- Ensuring your chin is kept up and your eyes facing forwards allows for reduced strain on your neck and back.
- These together will allow for a better posture and improved balance. [32]
- Keep shoulders back and relaxed:
- Relaxing your shoulders helps relieve tension and allows for a more neutral spine when walking.
- Engage core muscles and keep a neutral pelvis:
- engaging your core and keeping a neutral pelvis prevents arching of the spine and tilting of the pelvis, allowing for a more neutral spine and better posture. [33]
Outcome measures[edit | edit source]
There are a variety of outcome measures that might be used when advising walking as a management strategy for patients with LBP. These might look at:
- Pain
- Disability
- Physical activity
Pain[edit | edit source]
Visual Analogue Scale (VAS)[edit | edit source]
The VAS (Visual Analogue Scale) is one of the most common outcome measures for LBP. [34]
It is an example of a subjective PROM (Patient Reported Outcome Measure), where the patient records their pain on a 100mm line- from "no pain" at the beginning to the "worst pain imaginable". Some types of VAS also use faces to represent pain from "mild", "moderate" to "severe", as shown below.

Previous studies have found that the VAS is a "reliable and valid" outcome measure for use in a LBP population. [36] It has also shown reliability in predicting disability due to LBP. [37]
Disability[edit | edit source]
Roland-Morris Disability Questionnaire (RMDQ)[edit | edit source]
The Roland-Morris Disability questionnaire (RMDQ) is a commonly used PROM, designed to assess a patient's disability in relation to their LBP. It is a 24-item questionnaire that looks at physical functions that the patient feels have been affected, and a higher score represents a higher level of disability due to LBP. [38]

A study from 2020 found that the RMDQ had good test-retest reliability and internal consistency reliability in capturing the "everyday functional impact of low back pain". [40]
Oswestry Disability Index (ODI)[edit | edit source]
The Oswestry Disability Index (ODI) is also commonly used to assess functional disability in patients with LBP. [41] It consists of 10 items which are detailed below, as well as the interpretation of the scores.


The ODI has been found to be a "valid and reliable scale suitable for measurement of disability for low back pain", and in particular showing high test-retest reliability. [44]
A study looked at comparing the ODI and the RMDQ to each other. The study found that the ODI appeared to be better at detecting changes in patients with more severe lower back pain, whereas the RMDQ seemed to have an advantage when measuring patients who had more mild disability.[45]
Physical activity[edit | edit source]
International Physical Activity Questionnaire (IPAQ)[edit | edit source]
The International Physical Activity Questionnaire (IPAQ) is formed of two different versions including the IPAQ short-form and the IPAQ long version. Both versions require the patient to recall their physical activity levels in the past 7 days. Based on these scores, they are placed in one of three categories: low activity levels, moderate activity levels, and high activity levels. [46]
The IPAQ short-form consists of 4 categories where the patient reports how much they participated in the following activities in the past 7 days:
- Moderate activity
- Vigorous activity
- Time spent walking
- Time spent sitting
The IPAQ short-form may be more beneficial for use in a clinical setting due to the shorter/more accessible nature of the questionnaire for patients. [47]
The IPAQ long version assesses physical activity across 5 domains:
- Job-related physical activity
- Transportation physical activity
- Housework, house maintenance, and caring for family
- Recreation, sport, and leisure time
- Time spent walking
The IPAQ long version is typically used in research studies or may be used if a more detailed picture of a patient's physical activity levels is preferred. [47]
Overall, the IPAQ has been subject to extensive reliability and validity testing across 12 different countries (14 sites) from 2000 as an outcome measure for physical activity.
Suggestions for Future Clinical Research[edit | edit source]
- Based on the current literature, walking has been shown to be an effective management strategy for patients with LBP. However, more high-quality RCT’s need to be carried out using a variety of outcome measures, including physical activity, to further investigate walking as an effective management strategy for LBP.
- In order to strengthen the current evidence around this topic, further research could be carried out on how to ensure the long term effects of pedometer-based intervention. It would also be valuable to investigate whether added interventions might be necessary in aiding supportive positive outcomes long-term.
- The current NICE guidelines for LBP and sciatica were published in 2016 and updated in 2020 for pharmacological interventions. However, the advice for “non-pharmacological interventions” last had an evidence review in 2016. Therefore, it may be beneficial for a reassessment based on new evidence, in which guidelines around walking could be evaluated.
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 De Campos TF. Low back pain and sciatica in over 16s: assessment and management NICE Guideline [NG59]. J Physiother. 2017 Apr 1;63(2):120.
- ↑ Balagué F, Mannion AF, Pellisé F, Cedraschi C. Non-specific low back pain. Lancet. 2012 Feb 4;379(9814):482-91.
- ↑ Burton AK, Balagué F, Cardon G, Eriksen HR, Henrotin Y, Lahad A, Leclerc A, Müller G, Van Der Beek AJ, COST B13 Working Group on Guidelines for Prevention in Low Back Pain. European guidelines for prevention in low back pain: November 2004. European Spine Journal. 2006 Mar;15(Suppl 2):s136.
- ↑ Firestein GS, Budd RC, Gabriel SE, McInnes IB, O'Dell JR. Kelley and Firestein's textbook of rheumatology. Elsevier Health Sciences; 2016 Jun 21.
- ↑ Sassack B, Carrier J. Anatomy, Back, Lumbar Spine. [online] StatPerals [Intenet] 2022; August 25. Available from: https://www.ncbi.nlm.nih.gov/books/NBK557616/ [accessed 25/4/2022]
- ↑ 6.0 6.1 Knezevic NN, Candido KD, Vlaeyen JWS, Van Zundert J, Cohen SP. Low back pain. Lancet. 2021 Jul 3;398(10294):78-92.
- ↑ Buchbinder R, van Tulder M, Öberg B, Costa LM, Woolf A, Schoene M, Croft P, Hartvigsen J, Cherkin D, Foster NE, Maher CG. Low back pain: a call for action. Lancet. 2018 Jun 9;391(10137):2384-8.
- ↑ Casiano VE, Sarwan G, Dydyk AM, Varacallo M. Back Pain. StatPearls [Internet]. 2022 Feb 22. Available from: https://www.ncbi.nlm.nih.gov/books/NBK538173/ [accessed 25/4/2023]
- ↑ Wu A, March L, Zheng X, Huang J, Wang X, Zhao J, Blyth F, Smith E, Buchbinder R, Hoy D. Global low back pain prevalence and years lived with disability from 1990 to 2017: estimates from the Global Burden of Disease Study 2017. Ann Transl Med 2020; 8(6): 299.
- ↑ Sharp C. Musculoskeletal conditions and disorders in P.L. Jacobs (Ed) NSCA’s essentials of training special populations. Champaign, IL: Human Kinetics. 2018
- ↑ Soloman J. Low back pain. In: J.S. Skinner, C.X. Bryant, S. Merrill, & D.J. Green (Eds), American Council on Exercise medical exercise specialist manual. San Diego, CA: American Council on Exercise.2015
- ↑ Waongenngarm P, Areerak K, Janwantanakul P. The effects of breaks on low back pain, discomfort, and work productivity in office workers: A systematic review of randomized and non-randomized controlled trials. Applied ergonomics. 2018 Apr 1;68:230-9.
- ↑ Tudor-Locke C, Lutes L. Why do pedometers work?: a reflection upon the factors related to successfully increasing physical activity. Sports Med. 2009;39(12):981-93.
- ↑ Harris T, Kerry SM, Limb ES, Victor CR, Iliffe S, Ussher M, Whincup PH, Ekelund U, Fox-Rushby J, Furness C, Anokye N. Effect of a Primary Care Walking Intervention with and without Nurse Support on Physical Activity Levels in 45-to 75-Year-Olds: The P pedometer A and C consultation E valuation (PACE-UP) Cluster Randomised Clinical Trial. PLoS Medicine. 2017 Jan 3;14(1):e1002210.
- ↑ 15.0 15.1 Kang M, Marshall SJ, Barreira TV, Lee JO. Effect of pedometer-based physical activity interventions: a meta-analysis. Res Q Exerc Sport. 2009 Sep 1;80(3):648-55.
- ↑ 16.0 16.1 16.2 Olaya-Contreras P, Styf J, Arvidsson D, Frennered K, Hansson T. The effect of the stay active advice on physical activity and on the course of acute severe low back pain. BMC Sports Sci Med Rehabil. 2015 Dec;7(1):1-9.
- ↑ 17.0 17.1 Lang AE, Hendrick PA, Clay L, Mondal P, Trask CM, Bath B, Penz ED, Stewart SA, Baxter GD, Hurley DA, McDonough SM. A randomized controlled trial investigating the effects of an individualized pedometer-driven walking program on chronic low back pain. BMC Musculoskelet Disord. 2021 Dec;22(1):1-4.
- ↑ Krein SL, Kadri R, Hughes M, Kerr EA, Piette JD, Holleman R, Kim HM, Richardson CR. Pedometer-based internet-mediated intervention for adults with chronic low back pain: randomized controlled trial. JMIR. 2013 Aug 22;15(8):e2605.
- ↑ 19.0 19.1 Valdivieso P, Franchi MV, Gerber C, Flück M. Does a better perfusion of deconditioned muscle tissue release chronic Low Back pain?. Front Med. 2018 Mar 20;5:77.
- ↑ 20.0 20.1 Gordon R, Bloxham S. A systematic review of the effects of exercise and physical activity on non-specific chronic low back pain. Healthcare 2016 Apr 25; 4(2):22.
- ↑ Tillotson C. How to walk correctly and fix your lower back pain. Take the Five Easy Steps. Available from: http://www.youtube.com/watch?v=B9jt4d_828g [accessed 26/4/2023]
- ↑ 22.0 22.1 Kim H, Min TJ, Kang SH, Kim DK, Seo KM, Lee SY. Association between walking and low back pain in the Korean population: a cross-sectional study. Ann Rehabil Med. 2017 Oct 31;41(5):786-92.
- ↑ 23.0 23.1 23.2 Sitthipornvorakul E, Klinsophon T, Sihawong R, Janwantanakul P. The effects of walking intervention in patients with chronic low back pain: A meta-analysis of randomized controlled trials. Musculoskelet Sci Pract. 2018 Apr 1;34:38-46.
- ↑ 24.0 24.1 Vanti C, Andreatta S, Borghi S, Guccione A, Pillastrini P, Bertozzi L. The effectiveness of walking versus exercise on pain and function in chronic low back pain: a systematic review and meta-analysis of randomized trials. Disabil Rehabil. 2019 Mar 13;41(6):622-32.
- ↑ 25.0 25.1 Smith J, Stabbert H, Bagwell J, Teng H, Wade V, Lee S. Do people with low back pain walk differently? A systematic review and meta-analysis. J Sport Health Sci. 2022 Jul;11(4):450-465.
- ↑ 26.0 26.1 26.2 Lawford BJ, Walters J, Ferrar K. Does walking improve disability status, function, or quality of life in adults with chronic low back pain? A systematic review. Clin Rehabil. 2016 Jun;30(6):523-36.
- ↑ 27.0 27.1 27.2 Lee JS, Kang SJ. The effects of strength exercise and walking on lumbar function, pain level, and body composition in chronic back pain patients. J Exerc Rehabil. 2016 Oct;12(5):463-70.
- ↑ 28.0 28.1 Suh JH, Kim H, Jung GP, Ko JY, Ryu JS. The effect of lumbar stabilization and walking exercises on chronic low back pain: A randomized controlled trial. Medicine (Baltimore). 2019 Jun;98(26):e16173.
- ↑ 29.0 29.1 Yilmaz Yelvar GD, Çırak Y, Dalkılınç M, Parlak Demir Y, Guner Z, Boydak A. Is physiotherapy integrated virtual walking effective on pain, function, and kinesiophobia in patients with non-specific low-back pain? Randomised controlled trial. Eur Spine J. 2017 Feb;26(2):538-45.
- ↑ Norris MK, Fox FS, Lee C, Wang E, Green K, Yan H, Dieli-Conwright CM. Narrowing the gap for minority cancer survivors: exercise oncology in the past, present, and future. Journal of Clinical Exercise Physiology. 2020 Dec;9(4):155-70.
- ↑ 31.0 31.1 Nicolson PJ, Bennell KL, Dobson FL, Van Ginckel A, Holden MA, Hinman RS. Interventions to increase adherence to therapeutic exercise in older adults with low back pain and/or hip/knee osteoarthritis: a systematic review and meta-analysis. Br J Sports Med. 2017 May 1;51(10):791-9.
- ↑ Pickle NT, Grabowski AM, Auyang AG, Silverman AK. The functional roles of muscles during sloped walking. J Biomech. 2016 Oct 3;49(14):3244-51.
- ↑ Jung J, Yu J, Kang H. Differences in trunk muscle activities and ratios between unstable supine and prone bridging exercises in individuals with low back pain. Journal of Physical Therapy Science. 2012;24(9):889-92.
- ↑ Chiarotto A, Maxwell LJ, Ostelo RW, Boers M, Tugwell P, Terwee CB. Measurement properties of visual analogue scale, numeric rating scale, and pain severity subscale of the brief pain inventory in patients with low back pain: a systematic review. J Pain. 2019 Mar 1;20(3):245-63.
- ↑ WeCapable.com. Visual Analogue Scale for pain (VAS): Scoring pain on 100mm line. Disability information. 2022. Available from: https://wecapable.com/vas-pain-scale-100mm-line/ [accessed 27/5/2023]
- ↑ Olaogun MO, Adedoyin RA, Ikem IC, Anifaloba OR. Reliability of rating low back pain with a visual analog scale and a semantic differential scale. Physiotherapy Theory and Practice. 2004 Jan 1;20(2):135-42.
- ↑ Shafshak TS, Elnemr R. The visual analog scale versus numerical rating scale in measuring pain severity and predicting disability in low back pain. J Clin Rheumatol. 2021 Oct 1;27(7):282-5.
- ↑ Chiarotto A, Maxwell LJ, Terwee CB, Wells GA, Tugwell P, Ostelo RW. Roland-Morris Disability Questionnaire and Oswestry Disability Index: which has better measurement properties for measuring physical functioning in nonspecific low back pain? Systematic review and meta-analysis. Phys Ther. 2016 Oct 1;96(10):1620-37.
- ↑ PrimePhysio. Roland-Morris Disability Questionnaire. Orthopaedic manual therapy certificate. Available from: https://www.primephysio.com/forum/_omtc/roland-morris-disability-questionnaire-rmdq [accessed 27/5/ 2023]
- ↑ Burbridge C, Randall J, Abraham L, Bush E. Measuring the impact of chronic low back pain on everyday functioning: content validity of the Roland Morris disability questionnaire. J Patient Rep Outcomes. 2020 Dec;4(1):1-5.
- ↑ Fairbank JC, Pynsent PB. The Oswestry Disability Index. Spine (Phila Pa 1976). 2000 Nov 15;25(22):2940-52
- ↑ Haegg O. Oswestry Disability Index. Encyclopedia of Pain. 2013 Edition. Available from: https://link.springer.com/referenceworkentry/10.1007/978-3-642-28753-4_3021#howtocite [accessed 27/5/2023]
- ↑ Jalil N, Sulaiman Z, Awang M, Omar M. Retrospective Review of Outcomes of a Multimodal Chronic Pain Service in a Major Teaching Hospital: A Preliminary Experience in Universiti Sains Malaysia. Malays J Med Sci. 2009; 16(4): 55-65.
- ↑ Lee CP, Fu TS, Liu CY, Hung CI. Psychometric evaluation of the Oswestry Disability Index in patients with chronic low back pain: factor and Mokken analyses. Health Qual Life Outcomes. 2017 Dec;15(1):1-7.
- ↑ Fairbank J, Pynsent P. The Oswestry Disability Index. Spine 2000; 25(22):2940-53.
- ↑ Forde C. Scoring the International Physical activity questionnaire (IPAQ). Exercise prescription for the prevention and treatment of disease, University of Dublin 2018; 3. Available from: https://ugc.futurelearn.com/uploads/files/bc/c5/bcc53b14-ec1e-4d90-88e3-1568682f32ae/IPAQ_PDF.pdf [accessed 27/5/2023]
- ↑ 47.0 47.1 Craig C, Marshall A, Sjöström M, Bauman A, Booth M, Ainsworth B, Pratt M, Ekelund U, Yngve A, Sallis J, Oja P. International physical activity questionnaire: 12-country reliability and validity. Med Sci Sports Exerc. 2003 Aug 1;35(8):1381-95.