Haemophilia
Original Editors - Alyssa Elliott, Chelsea Reinhart, Alaa Kora
Top Contributors - Chelsea Reinhart, Alyssa Elliott, Tarina van der Stockt, Kim Jackson, Mandy Roscher, Robin Tacchetti, Elaine Lonnemann, Tony Lowe, WikiSysop, Lucinda hampton, Jess Bell, Aminat Abolade and Stacy Schiurring
Introduction[edit | edit source]
Haemophilia is a term that describes a rare (usually inherited) bleeding disorder that leads to haemorrhage in various body parts. It has various types and each type is different according to the factor that is deficient.[1] It is also known as the royal disease.[2]
Definition[edit | edit source]
Haemophilia is the most commonly known haemorrhagic disorder causing bleeding due to defects in the coagulation factors. This leads to delay in the coagulation process post injury. Haemophilia is usually an X linked recessive inherited disease, but in some rare conditions, it has been found to be acquired.[3][4]
History of Haemophilia[edit | edit source]
The observation of bleeding disorders in males happened early in the 2nd century. The Talmud stated that if 2 brothers had bled to death after circumcision then the next brother shouldn’t be circumcised. Also in the 12th century the Arabic physician al-Zahrāwī, known as Albucasis, described the death of male family members due to excessive haemorrhage after an injury.[5]
The first medical description of haemophilia was made by the physician John Conrad Otto in the 19th century. He successfully linked this bleeding disorder to a sex linked inheritance; this was followed by another genetic description of haemophilia by Nasse in 1820. He stated that haemophilia is transmitted from carrier mothers to their male offspring. Finally, the term “haemophilia” appeared in 1928 in the University of Zurich by Hopff.[5]
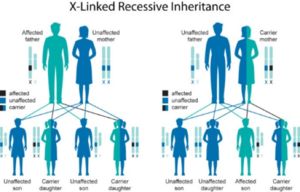
Genetic Inheritance[edit | edit source]
The term sex-linked refers to genes on the Sex chromosomes (usually the larger chromosome “X”)[6].
Genetic inheritance can either be dominant or recessive.
Females (XX) carry two X chromosomes. If a female carries a normal X-chromosome and a mutated X-chromosome. If the gene is recessive the female will be a carrier and will not suffer from the condition.[7] There is a 50% chance she will pass on the mutated x chromosome to her children.
Males (XY) only carry one X chromosome. If a male inherits a mutated X-chromosome he will be affected by the condition whether it is dominant or recessive.
Prevalence of Haemophilia[edit | edit source]
It was estimated that haemophilia was found in 1 in each 5000 male worldwide[8]. In 2019 a meta-analysis found that the number is larger than previously estimated. The researchers found that there is around 1,125,000 males that have bleeding disorders. The study also revealed that in every 100 000 males there are 17.1 with haemophilia A and 3.8 with haemophilia B [9][10]An updated statistic from a 2021 review found a prevalence of 12.8 per 100,000 males for haemophilia A[11].
Types of Haemophilia[edit | edit source]
Haemophilia is usually an inherited disease, but in rare cases, it can be acquired.
Inherited haemophilia[edit | edit source]
The type of haemophilia is determined according to the protein factor that defected[12]. There are three known types of haemophilia:[13][14]
Comparison between types of haemophilia[edit | edit source]
| haemophilia A | haemophilia B | haemophilia C | |
|---|---|---|---|
| Known as | Classical / Standard haemophilia | Christmas haemophilia | Rosenthal’s disease |
| Protein factor affected | Factor VIII | Factor IX | Factor XI |
| Genetic Inheritance | X linked recessive | X linked recessive | Autosomal recessive |
| Gender Affected | Mostly males | Mostly Males | Females & males equally |
| Severity | Mild, Moderate and Severe | Mild, Moderate and Severe | Mild |
Acquired haemophilia[edit | edit source]
Acquired haemophilia is rare and occurs as the result of an autoimmune disease that attacks the protein clotting factors (especially factor VIII) and subsequently leads to manifestations similar to haemophilia A.[13]
The Royal Disease[edit | edit source]
Queen Victoria was a carrier of haemophilia B. She passed the mutated gene to three of her children. Her two daughters became carriers and her son, Prince Leopold, had haemophilia. Queen Victoria’s children married many royals across Europe and Russia. Haemophilia B was spread among royals for many generations with royals being either a carrier or haemophilic.[2][15]
Manifestations of Haemophilia[edit | edit source]
Children with mild haemophilia do not show any manifestation except post-injury or dental extraction. Moderate and severe haemophiliacs may experience the following manifestations:[16]
- Mouth bleeding post-dental extraction or cut.
- Nose bleedings
- Un-stoppable haemorrhage after a small injury or cut
- Blood in urine and stool due to haemorrhage in the kidney / bladder/ intestines or stomach
- Haematoma
- Joint Bleeding
- Muscle Bleeding
Diagnosis of Haemophilia[edit | edit source]
Screening Tests[edit | edit source]
Complete Blood Count[edit | edit source]
Complete Blood Count (CBC) may appear normal in persons with haemophilia. If the patient has already experienced a massive haemorrhage, the CBC count may appear low.[17]
Activated Partial Thromboplastin Time (APTT) Test[edit | edit source]
The APTT test measures the duration of blood clotting by measuring the clotting ability of factor VIII, IX, XI and XIII. In patients with haemophilia, the results will show a prolonged clotting time[17].
Prothrombin Time (PT) Test[edit | edit source]
The PT test measures the duration of blood clotting by measuring the clotting ability of factor I, II, V, VII. In patients with haemophilia, the results are normal.[17]
Clotting Factor Tests[edit | edit source]
Clotting factor tests are used to diagnosis haemophilia and its type and the degree of severity. It measures the levels of factor VIII and IX.[17]
The Severity of Haemophilia[edit | edit source]
The severity of haemophilia is determined by the levels of clotting factor in the blood.[17]
Severity of haemophilia[edit | edit source]
| Severity | Levels of Factor VIII or IX in the blood |
|---|---|
| Normal | 50% to 100% |
| Mild haemophilia | Greater than 5% but less than 50% |
| Moderate haemophilia | 1% to 5% |
| Severe haemophilia | Less than 1% |
Medical Management[edit | edit source]
Replacement Therapy[edit | edit source]
Concentrates of clotting factor VIII (for haemophilia A) or clotting factor IX (for haemophilia B) are slowly injected into a vein to replace the missed clotting factor. These concentrates can be extracted from human blood or synthesized (recombinant clotting factor).[18]
Preventative (prophylactic) therapy[edit | edit source]
Preventative therapy encompasses the usage of replacement therapy on a regular basis to prevent bleeding.[18]
Demand therapy
Demand therapy is a less intensive approach that encompasses the usage of replacement therapy only when the need arises.[18]
Complications of Replacement Therapy[18][edit | edit source]
- May develop antibodies that attack the clotting factor
- Susceptible to viral infections from human clotting factors
- Damage to joints, muscles, or other parts of the body resulting from bleeding as a result of delays in treatment
Other Types of Treatment[edit | edit source]
Other types include Desmopressin (stimulates the production of the clotting factors), Antifibrinolytic Medicines and gene therapy)[18].
Recommended Treatment according to the severity of haemophilia[edit | edit source]
| Severity of haemophilia | Recommended Medical Management |
|---|---|
| Mild haemophilia | Desmopressin
No replacement therapy |
| Moderate haemophilia | Desmopressin
Replacement therapy during bleeding / prevent bleeding prior certain activities or surgeries |
| Severe haemophilia | Replacement therapy |
Physical Therapy Management[edit | edit source]
The National haemophilia Foundation formed a physical therapy working group that created the best physical therapy practice for bleeding disorders including haemophilia.[19]
The Medical and Scientific Advisory Council (MASAC) recommends physical therapy management in haemophilia because the most common manifestation is joint and muscle bleeding.[20]
Joints that have recurrent bleedings in haemophilia are known as “Target Joints”. The most common target joints are knee, elbow, ankle, hip and shoulders.[19]
The physiotherapy management of haemophilia is very similar to the management of Von Willebrand Disease.
Physiotherapy can also play a role in providing support and coaching, and in monitoring the musculoskeletal status of people with haemophilia.[21]
Physical Therapy Evaluation[edit | edit source]
According to the MASAC; the purpose of an evaluation is to detect the musculoskeletal and activities limitations caused by haemophilia.[22]
History and Interview[edit | edit source]
The patient and/or the caregiver is interviewed and the history is taken[22]:
- Personal history.
- Family history.
- Bleeding history.
- Medical and surgical history.
- Pain history.
- ADL concerns.
- Occupational concerns.
Physical Examination[edit | edit source]
- Palpation of joints at rest and during active range of motion to detect crepitus, synovitis, oedema or temperature.
- Girth measurement to assess oedema/ muscle atrophy.
- Atypical Joint End feel detection via the passive range of motion.
- Manual Muscle Testing to assess muscular strength.
- Muscle Flexibility test.
- Sensation and proprioception.
- Balance and fall assessment.
- Posture and alignment assessment.
- Assessment of functional activities.
- Gait analysis.
- Neuromotor assessment.
- Musculoskeletal Ultrasound.
Physical Therapy Treatment[edit | edit source]
The recommended physical therapy program by MASAC for muscles and joints bleeding is different in each recovery phase. There are three recovery phases: Acute, Subacute and Chronic. The management for all muscles follow specific guidelines, except for iliopsoas muscle, and all physical therapy suggested protocols are performed post factor replacement medication as follows:[23]
Physical Therapy Guidelines in Different Recovery Phases of Haemophilia[edit | edit source]
| Acute Phase | Subacute Phase | Chronic | Precautions | |
|---|---|---|---|---|
| Muscles Bleeding except for iliopsoas | Main Problem:
Present pain at rest and with movement |
Main Problem :
Limitations in ADL without increasing pain from baseline |
Main Problem :
ADL limitation but without pain |
|
Physical Therapy Program:
|
Physical Therapy Program:
|
Physical Therapy Program:
| ||
| Iliopsoas Muscle Bleeding | Main Problem:
pain presented at rest and with movement |
Main Problem :
ADL limitation without increase pain from baseline |
Main Problem :
ADL limitation but without pain |
Monitor for femoral nerve palsy |
Physical Therapy Program :
|
Physical Therapy Program:
|
Physical Therapy Program:
| ||
| Joint Bleeding | Main Problem:
pain presented at rest and with movement |
Main Problem :
ADL limitation without increase pain from baseline |
Main Problem :
ADL limitation but without pain |
|
Physical Therapy Program :
|
Physical Therapy Program :
|
Physical Therapy Program :
|
There are also some modalities and physical therapy tools that have been researched across the years to help patients with haemophilia. EMG biofeedback may be helpful with muscle strenthening and relaxation [24]
Kinesio Tape[edit | edit source]
It was shown the Kinesio tape plays a role in haemophilia by supporting the muscles, allowing joint movement with support, decreasing pain and decreasing hematoma.[25]
Transcutaneous Electrical Neurostimulation[edit | edit source]
It was shown that Transcutaneous electrical neurostimulation (TENS) has an impact on reducing pain for patients with haemophilia. It is applied as a low intensity electrical impulse to stimulate peripheral nerves. That inhibits pain information transmission along nerves.[26]
Related update: another treatment modality available to some physiotherapists, laser therapy, is showing promise for improving the functional capacity of patients with haemophilic arthropathy.[27]
Manual Therapy[edit | edit source]
Manual therapy such as fascial therapy, passive mobilization and stretching; manual orthopaedic therapy and proprioception training are recommended for physical therapy management for cases with haemophilia,[28] but joint traction as a manual therapy technique.[29]
haemophilia is a congenital X-linked bleeding disorder in which blood does not properly clot. It is categorized as a disorder of haemostasis. haemostasis, the stopping of bleeding after a blood vessel is injured, normally is divided into two separate processes—primary and secondary haemostasis. In haemophilia, secondary haemostasis (which essentially results in the formation of a fibrin clot) is defected. Thus, deficient clotting is due to an abnormality of the functional plasma-clotting proteins, factors VIII and IX, that are involved in this process. [30]
Differential Diagnosis[edit | edit source]
It is important to ensure haemophilia is properly diagnosed. Below are other medical issues or impairments that may present similarly and if not diagnosed appropriately could lead to a variety of medical issues.
- Nerve impingement: A person with haemophilia may experience bleeding into the iliacus muscle or the psoas. Bleeding in these areas can apply pressure to the femoral nerve branch that supplies the skin of the anterior thigh and a person may have a loss of sensation.
- Appendicitis: A person with haemophilia may have symptoms that mimic appendicitis when they have muscle bleeding on the right side in their lower abdomen.[30]
- Disseminated Intravascular Coagulation (DIC)[31]
- Von Willebrand Disease (VWD)[32]
- Thrombocytopenia[33]
Case Reports/ Case Studies[edit | edit source]
- Girardi D da M, Silva DRA, Villaça PR, Souza CE, Fonseca LG, Bastos DA, Hoffa PMG. Acquired haemophilia A in a patient with advanced prostate cancer. Journal of Autopsy & Case Reports. 2015;5(2):55-59. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC4584669/
- Iioka F, Shimomura D, Nakamura F, Ohno H, Yada K, Nogami K, Shima M. Long-term treatment course of a patient with mild haemophilia A who developed a high titre factor VIII inhibitor. Journal of Haemophilia. 2014;20(6):e402-e404.
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC4232888/ - Janbain M, Leissinger CA, Kruse-Jarres R. Acquired haemophilia A: emerging treatment options. Journal of blood medicine. 2015;6:143-150.
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC4431493/
Resources[edit | edit source]
- National Haemophilia Foundation: https://www.haemophilia.org/
- Genetics Home Reference page for haemophilia: https://ghr.nlm.nih.gov/condition/haemophilia
- CDC page for haemophilia: http://www.cdc.gov/ncbddd/haemophilia/
- Information for people with haemophilia: http://www.cdc.gov/ncbddd/haemophilia/people.html
- haemophilia Federation of America: http://www.haemophiliafed.org/
- Merck Manual Professional Version: haemophilia: http://www.merckmanuals.com/professional/hematology-and-oncology/coagulation-disorders/haemophilia
- Merck Manual Consumer Version: haemophilia: http://www.merckmanuals.com/home/blood-disorders/bleeding-due-to-clotting-disorders/haemophilia
- Steps for Living - haemophilia: https://stepsforliving.haemophilia.org/basics-of-bleeding-disorders
References[edit | edit source]
- ↑ Escobar M, Nguyen T. Hemophilia. In: Reference Module in Biomedical Research [Internet]. 3rd ed. Elsevier Inc.; 2014. p. 1–8.
- ↑ 2.0 2.1 O’Neill C. Royal blood: Queen Victoria and the legacy of hemophilia in European royalty [Internet]. Hekton International. 2020 [cited 2020 Jul 1].
- ↑ Nesterova AP, Klimov EA, Zharkova M, Sozin S, Sobolev V, Ivanikova N V., et al. Diseases of the Blood. In: Disease Pathways [Internet]. Elsevier Inc; 2019. p. 112–9.
- ↑ Marchesini E, Morfini M, Valentino L. Recent advances in the treatment of hemophilia: a review. Biologics: Targets & Therapy. 2021;15:221.
- ↑ 5.0 5.1 Franchini M, Mannucci PM. The History of Hemophilia. Semin Thromb Hemost [Internet]. 2014;40(5):571–6.
- ↑ Easter C. Sex Linked [Internet]. National Human Genome Institude. 2020 [cited 2020 Jul 3].
- ↑ Medline Plus. Sex-linked recessive [Internet]. National Libraray of Medicine. 2020 [cited 2020 Jul 3].
- ↑ National Center on Birth Defects and Developmental Disabilities. What is Hemophilia?. Centers for Disease Control and Prevention. 2020 [cited 2020 Jul 2].
- ↑ Inserro A. Prevalence of Hemophilia Worldwide Is Triple That of Previous Estimates, New Study Says American Journal of Managed Care. 2019 [cited 2020 Jul 2].
- ↑ Iorio A, Stonebraker JS, Chambost H, Makris M, Coffin D, Herr C, et al. Establishing the Prevalence and Prevalence at Birth of Hemophilia in Males. Ann Intern Med [Internet]. 2019 Sep 10;171(8):540–6.
- ↑ Berntorp E, Fischer K, Hart DP, Mancuso ME, Stephensen D, Shapiro AD, Blanchette V. Haemophilia. Nature Reviews Disease Primers. 2021 Jun 24;7(1):1-9.
- ↑ Hemophilia of Georgia. Types of Hemophilia. In: The Hemophilia, von Willebrand Disease & Platelet Disorders Handbook [Internet]. Hemophilia of Georgia; 2020 [cited 2020 Jul 3]
- ↑ 13.0 13.1 Shapiro AD. Hemophilia B [Internet]. National Organization of Rare Diseases. 2020.
- ↑ Bolton-Maggs P. Hemophilia C [Internet]. Medscape. 2019 [cited 2020 Jul 3].
- ↑ Mathew G. Know All About Hemophilia – The Royal Disease [Internet]. Medlife Wellness. 2020 [cited 2020 Jul 3]. Available from:
- ↑ Symptoms of Hemophilia [Internet]. Hemophilia News Today. 2020 [cited 2020 Jul 5].
- ↑ 17.0 17.1 17.2 17.3 17.4 Centers for Disease Control and Prevention. Diagnosis of Hemophilia [Internet]. National Center on Birth Defects and Developmental Disabilities. 2019 [cited 2020 Jul 5]. Available from:
- ↑ 18.0 18.1 18.2 18.3 18.4 National Heart, Lung, and Blood Institute NI of H. How Is Hemophilia Treated? [Internet]. Centers for Cancer Care and Blood Disorders. 2020 [cited 2020 Jul 5].
- ↑ 19.0 19.1 Lowes LP, Alfano L, Orlin MN. Muscloskeltal System: Considerations and Interventions for Specific Pediatric Pathology. In: Effgen SK, editor. Meeting the Physical Therapy Needs of Children. 2nd ed. Philadelphia: F. A. Davis Company; 2013. p. 226–7.
- ↑ Medical and Scientific Advisory Counsil. MASAC Document #238: Recommendations Regarding Physical Therapy Guidelines in Patients with Bleeding Disorders. Natl Hemoph Found. 2015;238.
- ↑ Lobet S, Timmer M, Königs C, Stephensen D, McLaughlin P, Duport G, Hermans C, Mancuso ME. The Role of Physiotherapy in the New Treatment Landscape for Haemophilia. Journal of Clinical Medicine. 2021 Jun 26;10(13):2822.
- ↑ 22.0 22.1 Medical and Scientific Advisory Council. Physical Therapy Evaluation Recommendations. Natl Hemoph Found. 2018;
- ↑ National Hemophilia Foundation. Physical Therapy Practice Guidelines for Persons with Bleeding Disorders: Muscle Bleed. 2018;
- ↑ Culbert T, Banez G. Pediatric Applications. In: Schwartz M, Andrasik F, editors. Biofeedback, Fourth Edition: A Practitioner’s Guide. 4th ed. The Guilford Press; 2017.
- ↑ Zolotnitsky M. The Benefits of Kinesio Taping: Ask The HemoDoc [Internet]. BioMatrix. 2019 [cited 2020 Jul 5].
- ↑ Riley RR, Witkop M, Hellman E, Akins S. Assessment and management of pain in Hemophilia Patients. Hemophilia. 2011;17:839–45.
- ↑ Elshennawy S, Zahreldin AA, Mortada H, Hozien M, Youssef AS, Galal A, Shahien M, Elfeky A, Elaraby A, Hamed M. The efficacy of Physical therapy modalities in patients with haemophilia: a systematic review of randomized controlled trials with meta-analysis. Archives of Physical Medicine and Rehabilitation. 2022 Jul 19.
- ↑ Donoso-Úbeda E, Meroño-Gallut J, López-Pina JA, Cuesta-Barriuso R. Effect of manual therapy in patients with hemophilia and ankle arthropathy: a randomized clinical trial. Clin Rehabil. 2020;34(1):111–9
- ↑ Cuesta-Barriuso R, Trelles-Martínez RO. Manual therapy in the treatment of patients with hemophilia B and inhibitor. BMC Musculoskelet Disord. 2018;19(1):1–5.
- ↑ 30.0 30.1 Goodman CC, Snyder TEK. Differential Diagnosis for Physical Therapists: Screening for Referral. 5th ed. St. Louis: Elsevier Inc, 2013.
- ↑ MedlinePlus. Disseminated intravascular coagulation (DIC). https://www.nlm.nih.gov/medlineplus/ency/article/000573.htm (accessed 8 April 2016).
- ↑ Centers for Disease Control and Prevention. Facts About von Willebrand Disease. http://www.cdc.gov/ncbddd/vwd/facts.html (accessed 8 April 2016).
- ↑ National Heart, Lung, and Blood Institute. What Is Thrombocytopenia?. http://www.nhlbi.nih.gov/health/health-topics/topics/thcp/ (accessed 8 April 2016).