Diastasis Recti Abdominis and Pelvic Floor Dysfunction
Top Contributors - Carin Hunter, Jess Bell, Kim Jackson, Tarina van der Stockt, Momina Masood, Wanda van Niekerk, Vidya Acharya, Lucinda hampton, Khloud Shreif and Matt Huey
Diastasis Recti Abdominis[edit | edit source]
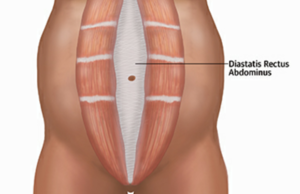
Diastasis recti abdominis (DRA) is an impairment characterised by an increase in midline separation of the rectus abdominis muscles due to the widening and thinning of the linea alba (LA).[1][2] This separation results in an increase in the distance between the two rectus abdominis muscles, commonly referred to as the inter-rectus distance (IRD).[2] DRA is present when the IRD increases and exceeds normal values,[3] which can be measured at 1 or more regions along the LA.[4] It should be noted, that the increase in midline “separation” of the rectus abdominis muscles involves stretching of the LA rather than a true separation.[5]
DRA can occur in both males and females, and across all age groups[6]. In infants, the separation between the rectus abdominis muscles can be congenital due to an abnormal alignment of fibre orientation within the LA or can occur as a result of decreased abdominal muscle activity[6]. In men, increasing age, particularly from middle age, significant weight fluctuations/obesity,[7] weightlifting causing excessive increases in intraabdominal pressure (IAP), and/or inherited muscle weakness are all considered risk factors for the development of DRA.[8] DRA is most commonly recognised as a condition that is highly prevalent in pregnant and postpartum women[1], which can be explained by the expansion of the uterus to accommodate the growing fetus[6]. The expanding uterus causes the rectus abdominis muscles to elongate while altering their angle of attachment, which in conjunction with hormonal elastic changes of connective tissue[9], leads to the stretching of the LA resulting in an increased IRD, displacement of the abdominal organs, and a bulging of the abdominal wall[6]. During pregnancy, 33% of women present with an increased IRD by the second trimester[10], and 100% of these women present with an increased IRD by the end of the third trimester[11].
Clinically relevant anatomy[edit | edit source]
- Rectus abdominis muscles
- External abdominal oblique
- Internal abdominal oblique
- Transverse abdominis
- Linea alba
- Lumbar multifidus
- Pelvic floor
- Diaphragm
Differential Diagnosis[edit | edit source]
The referring diagnosis is often different from DRA.[12] Most commonly these are:
- LBP
- Pelvic Pain/dysfunction
- Hip/Groin pain
Signs and Symptoms[edit | edit source]
- Abdominal doming by umbilicus during rectus abdominis contraction (DRA usually above and/or below umbilicus)[13][14]
- Doming or bulge worsens with
- Excessive pressure in the abdomen, too much effort while breathing
- Activity/Exercise too hard
- Modification should be performed without doming
- Doming or bulge worsens with
- High prevalence of DRA in the patients with urogynaecological conditions, so other symptoms may include:
Testing[edit | edit source]
The most traditionally used diagnostic method in clinical practice is the finger – width method, which primarily functions as a screening tool[15]. This tool is used to detect the presence or absence of DRA. If on palpation, the therapist or patient themself can place two or more finger breaths (≈2cm) in the sulcus between the medial borders of the rectus abdominis muscles, the patient may present with diastasis recti abdominis[16].
In terms of measuring IRD, CT scan and ultrasound imaging (USI) have been titled the gold-standard methods to measure IRD non-invasively[17], displaying good inter-rater[18] and intra-rater reliability in the literature[19]. However, its daily clinical use may be limited due to cost, availability, and training[15]. A more clinically feasible alternative is the use of calipers, whereby the tips of calipers are fitted across the width of the separation[15]. Calipers are considered to be a reliable tool for measuring IRD at and above the umbilicus[15]. This was supported by Chiarello and McAuley (2013), who found that IRD measurements with calipers were similar to those taken with USI above the umbilicus.[20] Additional research is, however, needed to evaluate the potential of calipers relative to ultrasound imaging[15]. Other alternatives include computed tomography (CT scan) and magnetic resonance imaging (MRI), which are considered the method of choice when assessing the abdominal wall. However, neither are clinically feasible and both are expensive[15].
With regards to pathologic interrecti distance (IRD)[21]
- Separation larger than 2 cm,[22] or > 2 finger widths
- 2.5 to 3.4 cm mild
- 5 to 20 cm severe
Treatment[edit | edit source]
- Education to manage patient expectations, limit fear and anxiety
- Postural correction
- Kinesio taping is help helpful in approximation of muscular distance
- Exercises for transverse abdominis, multifidus, diaphragm and pelvic floor muscles[23]
- Preactivation of the transverse abdominis (TA) prior to activity/exercise appears to provide for a “better force transfer between sides of the abdominal wall”[4].
- This changes the clinicians focus from “narrowing the IRD” to creating tension in the linea alba during core strengthening exercises and other activities
- Preactivation of the transverse abdominis (TA) prior to activity/exercise appears to provide for a “better force transfer between sides of the abdominal wall”[4].
- Although researchers suggest that external support, such as abdominal binding, should not be recommended as a primary rehabilitation technique for DRA to avoid reliance, in specific cases there may be benefits to its use when coupled with exercise[1]
- General TA training in neutral spine and functional tasks
- Pelvic floor training
- Tupler technique®
- 18 week programme includes progressive exercise programme, wearing splint, body mechanics, TA activation
- Pilates
- Patient education/body mechanics training
- Breathing strategy
- Diaphragmatic breathing: Fill your belly completely with air, but avoid letting your ribs move up as you inhale. Instead, think as if your belly and rib cage is like an umbrella: open it completely. As you exhale, close the *umbrella* and draw the belly towards the spine. Diaphragmatic breathing is helpful but don't hold down breath deeply because that can be dangerous.
- Hip raises:Lay on your back, with knees bent. Ground your shoulders into the floor and press your weight into your heels. Exhale and squeeze your glutes as you press your hips up, and slowly lower down, bring back slowly because you need to avoid stress. This way glutes along with abdominals activates.
- Avoid stressful movements involving RA early in treatment
- i.e., rolling to get out of bed
Pelvic Floor Dysfunction[edit | edit source]
Anatomy[edit | edit source]
The pelvic floor is made up of a layer of muscles covering the bottom of the pelvis and provide support to the pelvic organs; the bladder and bowel in men[24] and bladder, bowel and uterus in women.[25] The structures that sit on top of the pelvic floor are known as our pelvic organs. These muscles run like a hammock from the front of the pelvis to the coccyx at the back, and side-to-side from one sitting bone to the other.[25]
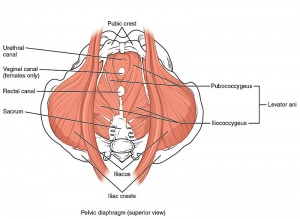
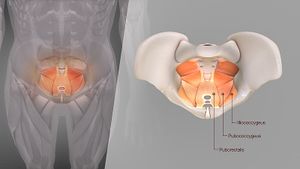
The pelvic floor is a funnel-shaped structure covering the base of the pelvis from the pubic symphysis anteriorly to the coccyx posteriorly and stretches from one ischial tuberosity to the other. It consists of two main muscles, the levator ani, and the coccygeus[26].
- The levator ani muscle is a broad thin muscle that is made up of a group of 3 muscles, pubococcygeus, puborectalis and iliococcygeus. The muscles join in the middle of the pelvis except at the prostrate in males and vagina and urethra in females.
- Pubococcygeus originates from both sides of the body of the pubis lateral to the puborectalis muscle and anterior to the obturator canal at the tendinous arch. It travels posterior and medial to insert onto the perineum, coccyx and anococcygeal ligament.
- Puborectalis is a U-shaped muscle that originates on both sides of the pubic body just lateral to the pubic symphysis. The muscle runs posterior and encircles the rectum so both sides join together. Some fibres join the external anal sphincter. The contraction of this muscle causes the anorectal junction to bend 90 degrees. This maintains faecal continence during contraction and enables defecation on relaxation. Some fibres may extend towards the urethra in both male and females and to the vagina in females, aiding with urinary continence.
- Iliococcygeus originates from the ischial spines and posterior portion of the obturator internus. It travels posterior and medially and inserts onto the anococcygeal ligament and coccyx[27].
- Coccygeus is also known as the ischiococcygeus muscle. It is a small muscle that makes up the posterior portion of the pelvic floor. It originates from the sacrospinous ligament and ischial spine and inserts onto the lateral borders of the inferior sacrum and superior coccyx[28].
- The urogenital diaphragm is a term not recognized any longer by Terminologia Anatomica due to a better understanding of the morphology, but was defined as a triangular sheet of muscle and fascia in the deep peroneal space consisting of the deep transverse perineal muscles and the sphincter urethrae.
- Sphincters and erectile muscles of the urogenital and intestinal tract:
- external anal sphincter,
- bulbospongiosus, ischiocavernosus, superficial transverse perineal.
According to a research study by Migda et al. (2019), the use of high-frequency ultrasound (HFUS) provides an objective assessment of the structures of the vulva, vagina, and cervix[29].
For more information on the anatomy of the pelvic floor please visit: http://teachmeanatomy.info/pelvis/muscles/pelvic-floor/
Types of dysfunction[edit | edit source]
Weakness, elongation of muscles (overstretch)
- Pelvic organ prolapse (POP)
- Uterine prolapse
- Anterior vaginal / cystocele (bladder prolapse)
- Posterior vaginal / rectocele (rectal prolapse)
- Symptoms
- Heaviness, bulging visually, physical see or feel protrusion
- Incontinence, stress urinary incontinence (SUI)
- Leaking with sneezing, coughing, laughing, lifting
- Most common in the 3rd trimester
- Pelvic/low back pain or pressure
Overactive/tightness (pelvic pain, PF is also weak, not able to relax)
- Levator ani syndrome
- Proctalgia
- Vulvodynia
- Dyspareunia
- Coccydynia
- Symptoms
- Pain, pelvic floor, hips, pelvic girdle pain
- Incontinence, leaking, urge or stress urinary incontinence, incomplete bladder emptying
- Painful bowel movements/constipation
- Painful intercourse (dyspareunia)
- Tailbone pain
Signs and Symptoms Review[edit | edit source]
Signs and symptoms of pelvic floor dysfunction include:
- Pain or numbness during intercourse[30][31][32]
- Ongoing pain in your pelvic region, genitals or rectum
- Pain in your lower back that cannot be explained by other causes[30]
- A prolapse – may be felt as a bulge in the vagina (feeling or seeing a bulge or lump in or coming out of your vagina) or a feeling of heaviness, discomfort, pulling, dragging or dropping sensation[30]
- Prolapse is a common condition that can occur due to weak pelvic floor muscles in women. This occurs due to the uterus, bladder, bowel or top of the vagina moving out of their normal positions and pushing into the vagina. This can cause pain and discomfort but can be improved with pelvic floor exercises and lifestyle changes[33]. Urinary incontinence has a direct relationship with pelvic floor muscles. These muscles tighten as a closure mechanism for the tube from the bladder to the exit (urethra) and weakness of these muscles can cause leaking and dribbling[34]
- Accidentally leaking urine when you exercise, laugh, cough or sneeze (stress incontinence)[35][31]
- Feelings of urgency in needing to the bathroom, or not making it there in time[35]
- Frequent need to urinate[35][30]
- Difficulty emptying your bladder (discontinuous urination – stop and start multiple times) and bowels[35][30]
- The feeling of needing to have several bowel movements during a short period of time
- Constipation or bowel strains[32]
- Accidentally passing gas[30]
Risk Factors[edit | edit source]
- Prior pregnancies
- Episiotomies/tears
- Obesity
- Continence status
- Age
- Length of active pushing
- Forceps delivery
Even women who have had a low-risk vaginal birth experience still experience overstretching and muscle “trauma” related to pregnancy and birthing. This usually resolves with time but may need intervention
Other health conditions increasing stress on the pelvic floor musculature:
- Respiratory history
- Excessive coughing (ie, covid, asthma, COPD)
- Gastrointestinal (GI) health
- Irritable bowel syndrome (IBS), constipation
Treatment to consider[edit | edit source]
- Assess and treat pelvic girdle impairments; important considerations:
- Trunk and hip ROM/flexibility/strength; muscle slings
- Core stabilisation exercises including PF contractions if appropriate (not if hypertonic PF)
- Proper breath strategies during exercise and activities of daily living
- Patient education (ie. behavioural, anxiety/fear, bladder diary, fluid intake, avoiding bladder irritants, avoid valsalva manoeuvres)
- Visit pelvic floor Physical therapist after birth, whether you think you have diastasis recti or not. They can provide a plenty of knowledge about muscle imbalances and tips to improve posture that's most important part, alignment, and restore proper function to your entire body.
- Referral to pelvic floor therapist or back to referring provider with recommendation
- Referral to a urogynecologist or back to referring provider with recommendation
References[edit | edit source]
- ↑ 1.0 1.1 1.2 Dufour S, Bernard S, Murray-Davis B, Graham N. Establishing expert-based recommendations for the conservative management of pregnancy-related diastasis rectus abdominis: A Delphi consensus study. Journal of Women’s Health Physical Therapy. 2019 Apr 1;43(2):73-81.
- ↑ 2.0 2.1 Acharry N, Kutty RK. Abdominal Exercise With Bracing, A Therapeutic Efficacy In Reducing Diastasis-Recti Among Postpartal Females. International Journal of Physiotherapy and Research. 2015Nov;3(2):999–1005.
- ↑ Beer GM, Schuster A, Seifert B, Manestar M, Mihic‐Probst D, Weber SA. The normal width of the linea alba in nulliparous women. Clinical anatomy. 2009 Sep;22(6):706-11
- ↑ 4.0 4.1 Lee D, Hodges PW. Behavior of the linea alba during a curl-up task in diastasis rectus abdominis: an observational study. journal of orthopaedic & sports physical therapy. 2016 Jul;46(7):580-9
- ↑ Hickey F, Finch JG, Khanna A. A systematic review on the outcomes of correction of diastasis of the recti. Hernia. 2011;15(6):607–14.
- ↑ 6.0 6.1 6.2 6.3 Michalska A, Rokita W, Wolder D, Pogorzelska J, Kaczmarczyk K. Diastasis recti abdominis — a review of treatment methods. Ginekologia Polska. 2018;89(2):97–101
- ↑ Reinpold W, Köckerling F, Bittner R, Conze J, Fortelny R, Koch A, Kukleta J, et al. Classification of rectus diastasis-a proposal by the German Hernia Society (DHG) and the International Endohernia Society (IEHS). Front Surg. 2019 Jan 28;6:1.
- ↑ Cheesborough JE, Dumanian GA. Simultaneous Prosthetic Mesh Abdominal Wall Reconstruction with Abdominoplasty for Ventral Hernia and Severe Rectus Diastasis Repairs. Plastic and Reconstructive Surgery. 2015;135(1):268–76.
- ↑ Benjamin DR, Van de Water AT, Peiris CL. Effects of exercise on diastasis of the rectus abdominis muscle in the antenatal and postnatal periods: a systematic review. Physiotherapy. 2014 Mar 1;100(1):1-8.
- ↑ Sperstad JB, Tennfjord MK, Hilde G, Ellström-Engh M, Bø K. Diastasis recti abdominis during pregnancy and 12 months after childbirth: prevalence, risk factors and report of lumbopelvic pain. Br J Sports Med. 2016 Jun 20:bjsports-2016
- ↑ Mota PG, Pascoal AG, Carita AI, Bø K. Prevalence and risk factors of diastasis recti abdominis from late pregnancy to 6 months postpartum, and relationship with lumbo-pelvic pain. Manual therapy. 2015 Feb 1;20(1):200-5.
- ↑ Claus CM, Malcher F, Cavazzola LT, Furtado M, Morrell A, Azevedo M, Meirelles LG, Santos H, Garcia R. Subcutaneous onlay laparoscopic approach (SCOLA) for ventral hernia and rectus abdominis diastasis repair: technical description and initial results. ABCD. Arquivos Brasileiros de Cirurgia Digestiva (São Paulo). 2018;31(4).
- ↑ Spitznagle TM, Leong FC, Van Dillen LR. Prevalence of diastasis recti abdominis in a urogynecological patient population. Int Urogynecol J Pelvic Floor Dysfunct. 2007;18(3):321-328. doi:10.1007/s00192-006-0143-5
- ↑ Michalska A, Rokita W, Wolder D, Pogorzelska J, Kaczmarczyk K. Diastasis recti abdominis — a review of treatment methods. Ginekologia Polska. 2018;89(2):97-101. doi:10.5603/GP.a2018.0016
- ↑ 15.0 15.1 15.2 15.3 15.4 15.5 Van de Water AT, Benjamin DR. Measurement methods to assess diastasis of the rectus abdominis muscle (DRAM): a systematic review of their measurement properties and meta-analytic reliability generalisation. Manual therapy. 2016 Feb 1;21:41-53
- ↑ Noble E. Essential Exercises for the Childbearing Year. 2nd edition. Boston, MA: Houghton Miffilin; 1982
- ↑ Benjamin DR, Van de Water AT, Peiris CL. Effects of exercise on diastasis of the rectus abdominis muscle in the antenatal and postnatal periods: a systematic review. Physiotherapy. 2014 Mar 1;100(1):1-8.
- ↑ Keshwani N, Hills N, McLean L. Inter-rectus distance measurement using ultrasound imaging: does the rater matter?. Physiotherapy Canada. 2016;68(3):223-9
- ↑ Mota P, Pascoal AG, Carita AI, Bø K. Normal width of the inter-recti distance in pregnant and postpartum primiparous women. Musculoskeletal Science and Practice. 2018 Jun 1;35:34-7.
- ↑ Chiarello CM, McAuley JA. Concurrent validity of calipers and ultrasound imaging to measure interrecti distance. journal of orthopaedic & sports physical therapy. 2013 Jul;43(7):495-503
- ↑ Litos K. Progressive therapeutic exercise program for successful treatment of a postpartum woman with a severe diastasis recti abdominis. Journal of women’s health physical therapy. 2014 May 1;38(2):58-73.
- ↑ Hernández-Granados P, Henriksen NA, Berrevoet F, Cuccurullo D, López-Cano M, Nienhuijs S, et al. European Hernia Society guidelines on management of rectus diastasis, British Journal of Surgery. 2021;108(10):1189-91.
- ↑ Berg-Poppe, P Hauer M, Jones C, Munger M, Wethor C. Use of exercise in the management of postpartum diastasis recti: a systematic review. Journal of Women's Health Physical Therapy. 2022;46:35-47.
- ↑ Continence Foundation of Australia. 2018. Pelvic Floor Muscles in Men [online] [viewed 28 March 2018] Available from:https://www.continence.org.au/pages/pelvic-floor-men.html
- ↑ 25.0 25.1 Pelvic Floor First. 2016. The Pelvic Floor [online] [viewed 23 March 2018]. Available from:http://www.pelvicfloorfirst.org.au/pages/the-pelvic-floor.html
- ↑ Moore, K.L., Dalley, A.F. and Agur, A.M., 2013. Clinically oriented anatomy. Lippincott Williams & Wilkins
- ↑ Palastanga, N. and Soames, R., 2011. Anatomy and human movement, structure and function. Elsevier Health Sciences.
- ↑ Drake, R., Vogl, A.W. and Mitchell, A.W., 2009. Gray's Anatomy for Students E-Book. Elsevier Health Sciences
- ↑ Migda MS, Migda M, Słapa R, Mlosek RK, Migda B. The use of high-frequency ultrasonography in the assessment of selected female reproductive structures: the vulva, vagina and cervix. J Ultrason. 2019 Dec;19(79):261-8.
- ↑ 30.0 30.1 30.2 30.3 30.4 30.5 Pelvic Floor First. 2017. Pelvic Floor First [online] [viewed 26 March 2018]. Available from: http://www.pelvicfloorfirst.org.au/pages/how-can-i-tellif-i-have-a-pelvic-floor-problem.html
- ↑ 31.0 31.1 Women's and Men's Health Physiotherapy. 2017. Leading the way in pelvic health [online] [viewed 28 March 2018]. Available from: http://www.wmhp.com.au/
- ↑ 32.0 32.1 Healthline. 2017. Pelvic Floor Dysfunction [online] [viewed 26 March 2018]. Available from: https://www.healthline.com/health/pelvic-floor-dysfunction#symptoms
- ↑ NHS Choices. 2018. Pelvic Organ Prolapse Overview [online] [viewed 29 March 2018]. Available from: https://www.nhs.uk/conditions/pelvic-organ-prolapse/
- ↑ Male Pelvic Floor. 2012. Urinary Dysfunction and the Male Pelvic Floor [online] [viewed 29 March 2018]. Available from:http://malepelvicfloor.com/urinary.html
- ↑ 35.0 35.1 35.2 35.3 NHS Choices. 2017. Living with incontinence [online] [viewed 28 March 2018]. Available from: https://www.nhs.uk/Livewell/incontinence/Pages/Livingwithincontinence.aspx