Achilles Tendinopathy Toolkit: Section A - Clinical Evaluation
Original Editor - Kim Jackson for The BC Physical Therapy Tendinopathy Task Force:
Prof. Alex Scott, Dr Joseph Anthony, Dr Allison Ezzat, Prof Angie Fearon, JR Justesen, Dr Allison Ezzat, Dr Angie Fearon, Carol Kennedy, Michael Yates, Paul Blazey and Alison Hoens.
Top Contributors - Kim Jackson, Olajumoke Ogunleye, Cindy John-Chu and Rishika BabburuIntroduction[edit | edit source]
The purpose of this document is to summarize the clinical evaluation of somebody who has been diagnosed with Achilles Tendinopathy.
The first steps involved in assessing a person presenting with Achilles tendinopathy is to carry out a subjective and objective examination, including a detailed history, to confirm the diagnosis. The toolkit leads you through the process of identifying potential risk factors association with Mid-Portion Achilles Tendinopathy, important questions and observations that form part of the subjective and objective assessment, as well as discussing Functional Tests and Differential Diagnosis.
Risk Factors[edit | edit source]
There are potential risk factors associated with mid-portion achilles tendinopathy. These can be further classified as non-modifiable and modifiable risk factors:
- Non-Modifiable Risk Factors
- mid-age 30-60 years[1] [2]
- male>female[3]
- Metabolic Disorders:
- Family history:
- Familial Hypercholesterolemia (HeFH)[1] - New onset of Achilles tendon pain is often the first sign of hypercholesterolemia and should be investigated for serum cholesterol levels.[4] Tendon Xanthomas are fatty deposits from high cholesterol levels and commonly found at the Achilles tendon.
- Genetic variants [1][5] -Certain genetic polymorphisms predispose tendon to altered collagen structure.
- Systemic Inflammatory Disorder:
- Seronegative Spondyloarthropathy (SpA) - 98% of SpAhave at least one enthesis disorder, commonly at the Achilles tendon.[6]. Consider use of SpAscreening tools such as SCREEND’EM [6]
- Modifiable Risk Factors
Assessment[edit | edit source]
Things to look out for when assessing for achilles tendinopathy include taking a thorough history from the patient including a detailed discussion about symptoms, the onset of injury and location of pain, as well as objective signs and biopsychological factors.
Subjective Assessment[edit | edit source]
The subjective assessment allows the patient to share details of the history of the injury, their current status, function, activity level, symptoms as well as any biopsychosocial factors that may have an impact on their treatment and recovery.
- Subjective Symptoms[11]
- Location -described in mid-portion of Achilles tendon.
- Morning pain and stiffness –described on initial weight bearing upon rising from bed or following periods of inactivity.
- History
- Gradual onset of symptoms.
- Pain with loading activity –sport or daily living.
- Biopsychosocial Factors
- Psychological factors, such as fear of movement (kinesiophobia),[12] as well as fears and beliefs about injury, may contribute to pain sensitivity.[13]
- Nervous System Sensitivity is characterized by allodynia and hypersensitivity, and has been considered to be a factor in persistent Achilles tendon pain.[14][15][16]
- Objective Signs/Observations
- Biomechanical Impairments:[2]
- Plantarflexor weakness
- Dorsiflexion stiffness
- Abnormal foot mechanics and lower limb abnormalities
- Palpation tests - Localized tenderness in a zone 2-6 cm above calcaneal insertion in mid-portion of the Achilles tendon. Swelling or thickening may or may not be present. Some studies suggest that only palpation testing was found to be reliable and accurate for diagnosing Achilles tendinosis.[11] [17][18] A combination of palpation tests is recommended in describing mid-portion Achilles tendinopathy.[17] [18] A selection of the palpation tests are listed below:
- Palpation“pinch test” [17][18]- In prone lying, ankle relaxed with foot hanging freely. Most painful site located by pinch pressure applied from proximal to distal along the length of the Achilles tendon. Mid-portion Achilles tendinopathy is identified in a zone 2-6 cm above the calcaneal insertion.
- Arc Sign [17][18] - Prone lying, ankle relaxed with foot hanging freely. Pinch pressure exploring for palpable thickness, swelling or nodule within mid-portion of Achilles tendon. In absence of thickness, a default area 3cm above the calcaneal insertion is located. The client is asked to perform active ankle dorsiflexion/plantarflexion cycles, palpating tendon movement under fingertips. Positive sign when tendon abnormality is felt to move concurrent with active movement. If thickened tissue moves independently or remains stationary, consider lesion to be instead within the para-tendon (synovial sheath) or outside of the tendon structure.
- Royal London Hospital test[17] [18] - In prone lying, ankle relaxed with foot hanging freely. Palpate ‘pinch test’ to locate most tender site of mid-portion of Achilles tendon. Active dorsiflexion results in less tenderness/absence of tenderness at pinch site.
- Biomechanical Impairments:[2]
Functional Tests: Tendon Loading Tests[edit | edit source]
It is important to understand the concept of load and capacity not only when assessing and diagnosing tendon injuries but it is also useful when assessing how they respond and react to mechanical loads that are placed on them. Two popular tests are listed below:
- Heel Rise Test (single leg) - A positive test is the report of pain in Achilles tendon upon repeated active plantar flexion on the symptomatic side during a single leg heel rise[17]
- Hop Test (single leg) - A positive test is the report of pain in Achilles tendon upon hopping or shortly after hopping on the symptomatic side. Test has been described as repeated hopping in place; or performing a single forward hop onto symptomatic side.[17]
Differential Diagnosis[edit | edit source]
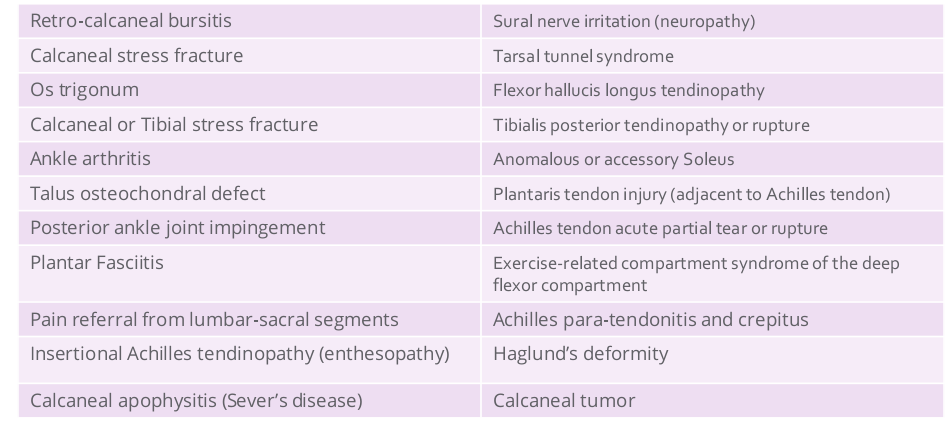
Palpation of surrounding tissue assists to rule out disorders that have alternate locations for tenderness experienced outside the zone of mid-portion Achilles tendinopathy symptoms, but which may be confused due to overlapping or similar pain presentations.[4] [11][17] - See Table 1
Imaging Studies[edit | edit source]
Physical exam using palpation provides comparable accuracy to medical imaging for diagnosis of mid-portion Achilles tendinopathy (Ultrasonography or MRI).[11] Up to 25% of asymptomatic subjects may have structural changes on imaging, highlighting that expensive and often unwarranted imaging should be limited to cases where diagnosis is uncertain.[17]
Resources[edit | edit source]
- Click to go back to the Main Achilles Tendinopathy Toolkit page
- Click to continue to Section B - Outcome Measures
- Click to continue to Section C - Summary of Evidence and Recommendations for Interventions
- Click to continue to Section D - Exercise Programs
- Click to continue to Section E - Low Level Laser Therapy Dosage Calculation
- Click to continue to Section F - Medical and Surgical Interventions
- UBC Achilles Tendinopathy Toolkit
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 Millar NL, Silbernagel KG, Thorborg K, Kirwan PD, Galatz LM, Abrams GD, Murrell GA, McInnes IB, Rodeo SA. Tendinopathy. Nature reviews Disease primers. 2021 Jan 7;7(1):1-21.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 2.7 Bondi M, Rossi N, Magnan B, Renzi Brivio L. The Achilles Tendinopathy: Pathogenesis Review. International Journal of Orthopaedics 2015; 2(3): 289-299
- ↑ Hollander K, Rahlf AL, Wilke J, Edler C, Steib S, Junge A, Zech A. Sex-specific differences in running injuries: a systematic review with meta-analysis and meta-regression. Sports Medicine. 2021 May;51(5):1011-39.
- ↑ 4.0 4.1 4.2 4.3 Abate M, Schiavone C, Salini V, Andia I. Occurrence of tendon pathologies in metabolic disorders. Rheumatology. 2013 Apr 1;52(4):599-608.
- ↑ 5.0 5.1 5.2 5.3 5.4 5.5 5.6 5.7 5.8 5.9 Van Der Vlist AC, Breda SJ, Oei EH, Verhaar JA, de Vos RJ. Clinical risk factors for Achilles tendinopathy: a systematic review. British journal of sports medicine. 2019 Nov 1;53(21):1352-61
- ↑ 6.0 6.1 Kirwan P, March J, Duffy. Screend’em before you treat’em. A clinical tool to help identify spondylarthropathy in patients with tendinopathy. Abstract at the International Scientific Tendinopathy Symposium; 2018; Groningen, the Netherlands
- ↑ Abate M, Vanni D, Pantalone A, Salini V. Cigarette smoking and musculoskeletal disorders. Muscles, ligaments and tendons journal. 2013 Apr;3(2):63.
- ↑ 8.0 8.1 8.2 de Vos RJ, Van Der Vlist AC, Zwerver J, Meuffels DE, Smithuis F, Van Ingen R, Van Der Giesen F, Visser E, Balemans A, Pols M, Veen N. Dutch multidisciplinary guideline on Achilles tendinopathy. British journal of sports medicine. 2021 Oct 1;55(20):1125-34.
- ↑ Spoendlin J, Meier C, Jick SS, Meier CR. Oral and inhaled glucocorticoid use and risk of Achilles or biceps tendon rupture: a population-based case-control study. Annals of medicine. 2015 Aug 18;47(6):492-8.
- ↑ 10.0 10.1 10.2 10.3 Silbernagel KG, Hanlon S, Sprague A. Current clinical concepts: conservative management of Achilles tendinopathy. Journal of athletic training. 2020 May;55(5):438-47.
- ↑ 11.0 11.1 11.2 11.3 Reiman M, Burgi C, Strube E, Prue K, Ray K, Elliott A, Goode A. The utility of clinical measures for the diagnosis of Achilles tendon injuries: a systematic review with meta-analysis. Journal of athletic training. 2014;49(6):820-9.
- ↑ Silbernagel KG, Brorsson A, Lundberg M. The majority of patients with Achilles tendinopathy recover fully when treated with exercise alone: a 5-year follow-up. Am J Sports Med. 2011 Mar;39(3):607-13
- ↑ Stubbs C, Mc Auliffe S, Mallows A, O’sullivan K, Haines T, Malliaras P. The strength of association between psychological factors and clinical outcome in tendinopathy: A systematic review. PloS one. 2020 Nov 30;15(11):e0242568.
- ↑ Eckenrode BJ, Kietrys DM, Stackhouse SK. Pain sensitivity in chronic Achilles tendinopathy. International journal of sports physical therapy. 2019 Dec;14(6):945.
- ↑ Tompra N, van Dieën JH, Coppieters MW. Central pain processing is altered in people with Achilles tendinopathy. British journal of sports medicine. 2016 Aug 1;50(16):1004-7.
- ↑ Debenham J, Butler P, Mallows A, Wand BM. Disrupted tactile acuity in people with achilles tendinopathy: a preliminary case-control investigation. journal of orthopaedic & sports physical therapy. 2016 Dec;46(12):1061-4.
- ↑ 17.0 17.1 17.2 17.3 17.4 17.5 17.6 17.7 17.8 Hutchison AM, Evans R, Bodger O, Pallister I, Topliss C, Williams P, Vannet N, Morris V, Beard D. What is the best clinical test for Achilles tendinopathy?. Foot and ankle surgery. 2013 Jun 1;19(2):112-7.
- ↑ 18.0 18.1 18.2 18.3 18.4 Maffulli N, Kenward MG, Testa V, Capasso G, Regine R, King JB. Clinical diagnosis of Achilles tendinopathy with tendinosis. Clinical Journal of Sport Medicine. 2003 Jan 1;13(1):11-5.
- ↑ CRTechnologies. Achilles Tendon Palpation Test (CR). Available from: https://www.youtube.com/watch?v=a9FI_0HpQ5Y [last accessed 18 May 2022]
- ↑ CRTechnologies. Arc Sign Achilles. Available from: https://www.youtube.com/watch?v=zhP0CAsQr7U [last accessed 18 May 2022]
- ↑ CRTechnologies. Royal London Hospital Test. Available from: https://youtu.be/nM3yu_TR4H8 [last accessed 18 May 2022]