Tendon Load and Capacity
Introduction[edit | edit source]
Understanding the concept of load and capacity is helpful when diagnosing tendon-related problems. Different types of loads, including tensile, compressive, mixed and shear and friction loads, can create various pathologies. Correctly identifying the type of load will help guide treatment.
Capacity[edit | edit source]
Capacity is a tissue's ability to withstand load without incurring damage or dysfunction. "A tissue is at full capacity when the individual can perform functional movements at the volume and frequency required without exacerbating symptoms or causing tissue injury".[1]
Injuries occur when the load placed on a tendon exceeds its capacity.[2][3] Each tendon in the body has a specific capacity, and every individual has a unique level of capacity for their tendons. For example, the patella tendon of an elite athlete tends to have a high capacity. Therefore, high levels of loading can be applied to this tendon without any detrimental effects. Alternatively, the patella tendon of a sedentary person would have a much lower capacity, and a much smaller load could potentially cause an injury to the tendon.[4]
"So the capacity of your tendon or muscle or bone or any tissue in our body, only ever just exceeds the loads that we put on it. So it's truly use it or lose it."[5] -- Ebonie Rio
Load[edit | edit source]
Tendons are subject to a variety of different loads. The cells that are responsible for tendon homeostasis are known as tenocytes. These cells are mechano-sensitive and react to mechanical loads placed on them. When appropriate loads are placed on them, they respond favourably. However, when they are exposed to abnormal loads, they are negatively affected.[6] Optimal, progressive loads result in an increase in tendon integrity. This process happens slowly, and if too much load is placed on a tendon too quickly, it becomes susceptible to injury.[6] Tendons are also slow to heal after an injury. This can make them challenging to treat.
"If you understand loading capacity, you can appreciate how people with all different types of activity levels can actually get into trouble with their tissues."[5] -- Ebonie Rio
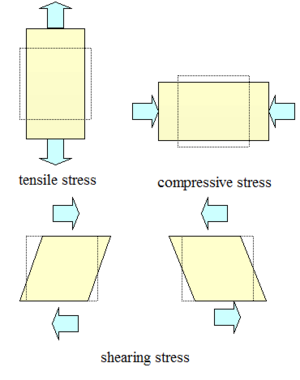
Tendons can be subjected to tensile, compressive, or shearing loads, and each of the loads affects the tendon differently. Please see Figure 1 for a diagram of the different types of loads applied to tendons. It is important to be able to identify the type of load that has resulted in the tendon pathology.
Tensile Load[edit | edit source]
Tensile stress is applied when two forces pull in opposite directions. All tendons are designed to withstand high tensile loads.[6] Tendons store and release energy, similar to a spring.[4] Activities involving speed, such as jumping and changing direction, place high tensile loads on tendons and can make them vulnerable to injury.
Examples of tendons that are subject to tensile load in the lower limb:[5]
- Achilles tendon:
- used as a spring throughout the lifespan
- common in sports with jumping, hopping, fast change of direction (e.g. court and field sports)
- can also occur in more sedentary people
- Patella tendon
- jumping sports (e.g. volleyball)
- change of direction (e.g. lunging at the tennis net)
Compressive Load[edit | edit source]
Compressive forces occur in tendons where the tendons pass bony protuberances. During specific movements, the tendons become compressed against these bony protuberances. This can occur in many areas of the body:
- Achilles tendon is compressed at the superior calcaneus during ankle dorsiflexion
- Gluteus medius and minimus tendons are compressed at the greater trochanter during hip adduction[7]
- Tibialis posterior and the peroneal tendons have permanent pivot points at the medial and lateral malleoli, respectively
Tendons are not only compressed by bony structures. The mid-portion of the Achilles tendon is subject to compressive and shearing loads from the surrounding musculature, tendons, and the posterior retinaculum.[7]
It is necessary to identify compressive load when managing tendinopathies. By reducing compressive load, the tendon can often be successfully rehabilitated with progressive loading.[7]
Combination Loads[edit | edit source]
Compressive forces on the tendon rarely happen in isolation. It is usually a combination of tensile forces with compression that places the tendon in a vulnerable state.[7] This is when the tendon is required to store and release energy while a compressive load is applied over a bony fulcrum.
While tendons are designed to function this way, these are the loads that most commonly cause problems and a clinical presentation of pain.[5] Examples include:[5]
- pushing off in dorsiflexion, where the tendons are compressed, but the tendon is required to spring the body forward
- hamstring tendinopathy in hockey can be caused by players being bent over in flexion while sprinting
Shear and Friction Loads[edit | edit source]
Shear and friction loads can occur when the tendon is subjected to repetitive activities. For example, the Achilles tendon can be affected by shear and friction loads in swimming or cycling when there is repeated dorsiflexion/plantarflexion. There is not the same storage and release of energy as there is in high tensile loads, but rather, the tendon is subjected to repetitive motions. These forces can affect the sheath of the tendon, as well as the structures surrounding the tendon. With shearing forces, the tendon rubs excessively on bony protuberances. This compromises the structures around the tendons (the paratenon) and creates an inflammatory response.[8] Paratenonitis is a different pathology to tendinopathy, so it is essential to recognise the difference between the two in order to select the correct management strategies.[5]
Summary[edit | edit source]
"I would argue that understanding load is really important in changing our treatment direction."[5] -- Ebonie Rio
- Tendons see four loads
- Tensile loads - when we ask our tendon to act like a spring
- Compressive loads - tendon is squashed against the bone
- Combination loads
- Tensile and compressive loads
- Most provocative
- Shear and frictions
"It's important that we can understand what's high tendon load and what isn't for each of our tendons, so that we can really listen in our subjective assessment and decide whether or not our patient is reporting high tensile load for that tendon."[5] -- Ebonie Rio
References[edit | edit source]
- ↑ Cook JL, Docking SI. “Rehabilitation will increase the ‘capacity’of your… insert musculoskeletal tissue here….” Defining ‘tissue capacity’: a core concept for clinicians. British Journal of Sports Medicine Online. 2015
- ↑ Snedeker JG, Foolen J. Tendon injury and repair - A perspective on the basic mechanisms of tendon disease and future clinical therapy. Acta Biomater. 2017;63:18-36.
- ↑ Wiesinger HP, Seynnes OR, Kösters A, Müller E, Rieder F. Mechanical and Material Tendon Properties in Patients With Proximal Patellar Tendinopathy. Front Physiol. 2020;11:704.
- ↑ 4.0 4.1 Rio E. Differential Diagnosis of Tendons Course. Plus. 2019
- ↑ 5.0 5.1 5.2 5.3 5.4 5.5 5.6 5.7 Rio E. Clinical Reasoning in Tendons Course. Plus, 2019.
- ↑ 6.0 6.1 6.2 Galloway MT, Lalley AL, Shearn JT. The role of mechanical loading in tendon development, maintenance, injury, and repair. The Journal of bone and joint surgery. American volume. 2013 Sep 4;95(17):1620-1628.
- ↑ 7.0 7.1 7.2 7.3 Cook JL, Purdam C. Is compressive load a factor in the development of tendinopathy?. Br J Sports Med. 2012 Mar 1;46(3):163-8.
- ↑ Wongsithichai P, Chang KV. Paratenonitis. Journal of Medical Ultrasound. 2014; 22:55e56. DOI:10.1016/j.jmu.2014.01.002