The PGM Method - Pregnancy and Postpartum Considerations
Top Contributors - Wanda van Niekerk, Kim Jackson, Vidya Acharya and Tarina van der Stockt
Introduction[edit | edit source]
During pregnancy the female body undergoes a variety of anatomical and physiological changes. Some of these hormonal and cardiovascular changes are discussed on this page, as well as common conditions during pregnancy and the importance of exercise during pregnancy.
Hormonal Changes[edit | edit source]
Relaxin[edit | edit source]
- Increases during pregnancy so that the body has the ability to stretch
- Often seen as the culprit for problems during pregnancy
- Research indicates that there is no link between pelvic girdle pain and relaxin serum levels during pregnancy[1]
- Relaxin relaxes the uterus and myometrium, as well as cervix
- Also allows for the pubic symphysis area widening during the first trimester
- During first 12 weeks of pregnancy – hormone increases 10 times and then starts to taper off
- Women in early stages of pregnancy already having back pain due to surge of relaxin in the system to prepare for childbirth – decreases to about 50 % of peak value by 20th week[2]
Estrogen[edit | edit source]
- Levels increase during pregnancy
- Responsible for water and sodium retention
- Relaxing effect on muscles and ligaments
- Increases vascularity in the respiratory membrane and signs of this include:
- frequent nosebleeds, nasal stuffiness (congestion), voice changes
Progesterone[edit | edit source]
- Increases body temperature
- Hyperventilation
- Decrease in gastric mobility
- Decrease in smooth muscle tone
Thyroid Hormone[edit | edit source]
- Increases basal metabolic rate (BMT) by 25% during pregnancy [3]
- Thyroid disorders second most common endocrine disorder in pregnancy and postpartum (diabetes is the most common)[4]
- Subclinical hypothyroidism (increased need for thyroxin during pregnancy)
- Symptoms of hypothyroid:
- Difficulty concentrating/ brain fog
- Excessive weight gain
- Cold
- Extreme fatigue
- Muscle cramping
- Constipation
- Symptoms of hyperthyroid:
- Nervousness/anxiety
- Weight loss/low weight gain
- Hot
- Fatigue, difficulty sleeping
- Tremor
- Increased and/or irregular heart rate
- Morning sickness and vomiting
It is very important that the healthcare provider should monitor any thyroid problems and thyroid levels![4]
Gestational Diabetes[edit | edit source]
- Monitored with glucose intolerance test
- Requires medical management
- Can be affected by exercise and education (diet and lifestyle)
- Risk factors linked to diet and lifestyle factors[6]
- Increased risk of:
- Hypertension
- Future diabetes for mother and child
- Caesarean section
- Preeclampsia
- Serious medical condition – life threatening[7]
- Preeclampsia.org (Preeclampsia Foundation)
- Monitor blood pressure and protein in urine
- If blood pressure > 140/90 mmHg and excessive protein in urine
- Symptoms such as:
- Headaches
- Vision changes
- Nausea
- Vomiting
- Rib pain in right side
- Low urine output
- Sudden weight gain
- Swelling, oedema
- Shortness of breath
- Impaired liver function
Other Systems[edit | edit source]
Gastrointestinal System[edit | edit source]
- Gallbladder problems
- Higher risk of gallbladder problems and disorders during pregnancy
- Key sign of gallbladder problems is R upper abdominal quadrant pain
- Pain can also refer to lower back and scapula
- Pain triggered by fatty foods
- Reflux and heartburn[10]
- Nausea and vomiting[10]
- Constipation[10]
Urogenital System[edit | edit source]
During pregnancy women are at higher risk for urinary tract infections (UTI’s). Symptoms of this would include burning and pain.[11]
Integumentary System[edit | edit source]
- Abdominal itching is usually normal
- If during late pregnancy, and experiencing itching in hands and feet with no rash – could possible be symptoms of cholestasis
- If accompanied by right upper quadrant pain, nausea, vomiting, loss of appetite, fatigue – patient needs to be referred to their obstetrician
Cardiovascular Changes[edit | edit source]
Overview of Cardiovascular Considerations[edit | edit source]
- Blood volume increases 35% – 50% during pregnancy[12]
- Venous pressure increases during standing due to uterus size – this may result in increased oedema in the lower extremity
- Heart rate increases 10 to 20 beats per minute and rhythm disturbances are common during pregnancy[12]
- Cardiac output increases 30% – 60% during pregnancy[13]
- Blood pressure decreases early in pregnancy rises during mid-pregnancy but should be similar to pre-pregnancy by the end of the pregnancy – if there are irregularities during pregnancy and if blood pressure is increasing, this may be a sign of preeclampsia.
- Important to monitor blood pressure regularly!
Supine Hypotension[edit | edit source]
- Occurs when a person is supine, but can also occur in standing
- During pregnancy it usually occurs after the 1st trimester, during the 2nd half of pregnancy
- Caused by compression of the vena cava by the enlarged uterus[15]
- Symptoms of supine hypotension[15]:
- Increased foetal movement
- Feeling faint, dizzy
- Shortness of breath (SOB)
- Pallor
- Headaches
- Restless feeling
- Chest pain
- Numbness/Paraesthesia, cold legs, weakness
- Fatigue
- Cyanosis, yawning, convulsions
How to Relief Supine Hypotension?[edit | edit source]
Changing positions increases blood flow to the lower extremities
- Changing from supine or static standing
- Position of choice is to lie on L side – this relieves the pressure on the vena cava and aorta on right side
- Can improve circulation by placing a pillow, towel roll, wedge under right hip
Important to be aware of this, especially during static treatment positions for prolonged periods of time!
Maternal Sleep Position[edit | edit source]
- Education on sleep position during pregnancy is important
- Sleeping in the supine position places stress on the foetus[16]
- Triple risk model for stillbirth[16]:
- High risk or vulnerable foetus
- Maternal comorbidities such as age, obesity, parity, gestational diabetes, gestational hypertension
- Foetal stressor such as supine sleep position
- The foetus cannot adapt to repeated nightly exposure to this stressor and ultimately dies as a result.[16]
Venous Thromboembolism[edit | edit source]
Increased incidence of deep vein thrombosis (DVT) in the prenatal and postpartum population.[17] The risk for DVT’s increases with[18]:
- Smoking
- Hypertension
- Older than 40 years of age
- Obesity
- Varicose veins
- Previous DVT
- Blood type other than O
- Congenital or acquired thrombophilia
- Immobility
- Congestive heart failure
- Malignancy
- Caesarean birth
- Preeclampsia and eclampsia
Pulmonary Embolism[edit | edit source]
A pulmonary embolism is a condition where one or more of the arteries in the lungs become blocked by a blood clot. This is caused by blood clots traveling from the legs or other parts of the body (deep vein thrombosis).
Symptoms of a pulmonary embolism are:
- Shortness of breath or dyspnoea
- Chest pain
- Cough
- Tachycardia
- Syncope
- Haemoptysis (blood in sputum)
Physical signs of DVT are:
- Thigh pain (may be diffuse)
- May be in inguinal region or in calf region
- Skin discoloration
- Swelling/oedema
- Prominent superficial veins
- Positive Homan’s sign may or may not be present
- Sudden increase in pain in calf or popliteal space with passive dorsiflexion
Treatment Positions during Pregnancy[edit | edit source]
The American College of Obstetrics and Gynaecology (ACOG) 2020 position paper on Physical Activity and Exercise during Pregnancy and the Postpartum Period[12] states that women over 20 weeks pregnant may have symptoms in the supine position at rest or during exercise due to aortocaval compression from the gravid uterus, and this should be considered during treatments.[12] Therefore, it is recommended to consider[12]:
- Avoiding supine exercise after 20 weeks of pregnancy
- Avoiding motionless standing due to pooling of blood in lower extremities
- Exercise and assessment modifications[19]
- Sitting
- Standing
- Left side-lying with a pillow between the knees
- Prone over 2 pillows (under chest and hips)
Red Flags[edit | edit source]
Screen for signs and symptoms of:
- Inflammatory disorders
- Infections (i.e., UTI)
- Trauma
- Neoplastic disease (refers to both malignant and benign abnormal growths)
- Degenerative problems
- Metabolic problems
- Unrelenting pain with lack of improvement[1]
- Weight loss
- History of cancer
- Steroid use
- Drug abuse
- HIV
- Neurological symptoms
- Fever
- Systemically unwell
- Placenta abruption
- Uncommon, but can occur in the last trimester of pregnancy
- Symptoms would include:
- Vaginal bleeding (varies widely)
- Sudden onset of abdominal and/or back pain
- Uterine tenderness
- Contractions and firmness in the uterus or abdomen (due to uterine contractions)
- Chronic placenta abruption
- Slow onset, intermittent bleeding, decreased foetal weight gain
Common Conditions during Pregnancy and Postpartum[edit | edit source]
Piriformis Syndrome[edit | edit source]
Symptoms include:
- Buttock pain and/or leg pain with or without low back pain
- Aggravated by sitting and/or prolonged walking
- Area will be painful on palpation
Physiotherapists will often see patients with a referral for piriformis syndrome, but keep in mind that is most likely not just the piriformis muscle that is involved and that assessment of other areas such as low back, the hip, SIJ will be necessary. Commonly seen is hypertonicity or stretch weakness of the piriformis. Stretch weakness of the piriformis indicates that the piriformis can be lengthened and that can lead to the femur on the involved side internally rotating. Stretch weakness of the piriformis occurs with the same side postural leg adduction and internal rotation and anterior pelvic tilt.[20]
It is important to address the muscle imbalances that are present. Some muscle imbalances that may be present:
- Gluteus maximus and medius – weak and/or tender
- Hip flexor tightness/tenderness
- Adductor tightness/tenderness
Targeted stretching and strengthening will be beneficial. Manual therapy techniques may also be beneficial if indicated.
Round Ligament Pain[edit | edit source]
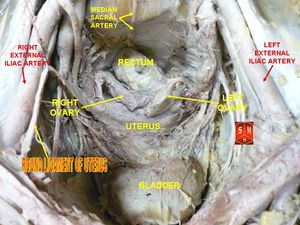
Anatomy of the round ligament
Originates at the uterine horns in the parametrium. The ligament leaves the pelvis via the deep inguinal ring, passes through the inguinal canal, and continues on to the labia majora where its fibres spread and mix with the tissue of the mons pubis (See also The Uterine and Cervical Ligaments)
Symptoms of Round Ligament Pain:
- Sudden pain in the lower abdomen
- Pain is one-sided and usually on the right side of the pelvis/groin
- Ligament stress/pain usually occurs with sudden movements or exercise
- NOT accompanied by the following symptoms:
- Vaginal bleeding
- Discharge
- Fever
- Chills
- Vomiting
If patient presents with lower abdominal pain it is important to rule out an inguinal hernia as there is a higher risk of an inguinal hernia during pregnancy because of the increase intra-abdominal pressure. It can present as a painful or tender groin lump and in some cases surgery is necessary to resolve it.[21]
Interventions for round ligament pain
- Posture and body mechanics education and exercises
- Examples: neutral pelvis, rolling, sit/stand, avoiding fast movements
- Pelvic tilt on side
- Reduce stretch on the ligament
- Assess for muscle imbalances
- Use the PGM Methodsm for screening and the algorithm of exercises in addition to manual muscle testing
- Introduction to the pelvic girdle musculoskeletal method
- The pelvic girdle musculoskeletal method pelvic balancing exercises
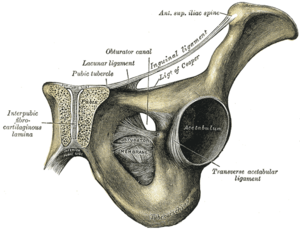
Pubic Symphysis Dysfunction[edit | edit source]
The pubic symphysis has a normal separation between sides of 5 mm or less. A separation is considered pathologic when it is between 6 to 12 mm. This widening of the pubic symphysis usually returns to normal/baseline within 12 weeks after pregnancy.
Separation of the pubic symphysis is rare during pregnancy and more common postpartum.[22] There are however some women who may have pubic symphysis pain during the later stages of pregnancy or who have been injured during a traumatic delivery or as a result of high-velocity trauma such as motor vehicle accident or horseback riding.[23] Separation of the pubic symphysis is usually diagnosed with radiographic documentation. In cases of trauma surgical intervention may be necessary, but during postpartum there is usually no surgery indicated.
Symptoms[22]:
- Pubic or groin pain, with referral to the medial thigh
- Painful with:
- bed mobility
- abducting legs
- walking
- climbing stairs
Differential diagnosis
- Osteitis Pubis
- Periosteal trauma
- Inflammatory process of the symphysis pubis and surrounding structures
- Hernia
- Inguinal/femoral
- Innominate rotation tendency
- Can use PGM method to screen and balance the pelvic girdle muscles
- Introduction to the pelvic girdle musculoskeletal method
- The pelvic girdle musculoskeletal method pelvic balancing exercises
Recommendations[23]
- Limit weight-bearing and ambulation until separation has reduced
- Assess ambulation status
- provide gait training with device
- consider wheelchair if indicated
- Patient education
- Pain management, ice
- Body mechanics education
- in and out of bed, rolling, sit to stand, in/out of a car
- keeping legs together (avoiding hip abduction)
- Holding a pillow between the legs with movement – this can help with engaging the adductors
- Assess for sacroiliac belt/pelvic binder
- Excessive swelling early on may cause compression from the belt to be uncomfortable, reassess at a later stage in such cases
- Respect pain levels
- Stabilising exercises that can be included in management:
- Focus on muscles such as rectus abdominis, transversus abdominis, internal obliques and adductor longus
- Isometric hip muscle strengthening (use pain as a guide)
- Can use physio ball/ theraband
- Hook lying, 4 point, sitting
Coccydynia[edit | edit source]
Pain or deep ache in the coccyx area. Symptoms include:
- Pain with:
- Sitting
- Pressure on the tailbone/coccyx
- Bowel movements
- Intercourse
Differential Diagnosis
- Pelvic girdle imbalances – Screen using the PGM Methodsm
- Screen pelvic floor for hypertonicity/pain/symptoms
- Constipation
Causes of coccydynia
- Idiopathic
- Localised internal or external trauma (childbirth, falls)[24]
- Ligament laxity during pregnancy and postpartum
- Obesity
- Postural issues such as sacral sitting
- Infection or tumor
Assessment
- External palpation of the coccyx[25]
- During pelvic floor contraction coccyx moves normally
- May be a valid and reliable method to assess pelvic floor contraction[25]
- Sidelying or standing
- Physical rectal examination (done by pelvic floor therapists or medical doctor)
- Radiologically diagnosed with X-rays or MRI
Interventions
- Internal soft tissue treatment
- referral to a pelvic health therapist
- Exercises to balance the pelvic girdle in flexibility and strength
- Consider PGM Methodsm
- “Asymmetry of the pelvic girdle has been hypothesized to elicit gluteus maximus, levator ani, and lateral hip rotator muscle overactivity, which can affect both the sacroiliac joints and coccyx.” [26]
- Stool softeners if patient is constipated
- Surgery (coccygectomy)
- Cushion can help with pain with sitting
- Recommended wedge shaped cushions
- thicker part is at back of chair
- results in an anterior pelvic tilt
- clears pressure from the coccyx (avoids “sacral sitting”)
- Recommended wedge shaped cushions
Pregnancy Related Transient Osteoporosis of the Hip[edit | edit source]
Symptoms
- Severe pain – lumbar, groin or hip
- Empty end feels in the hip
- Onset is usually in the 3rd trimester
Risk factors
- Immobility[27]
- Dental problems
- Lack of exercise during childhood
- Corticosteroids
- Heparin use
- Smoking
- Alcohol
- Eating disorders
- Cancer
- Rheumatoid arthritis
- Thyroid disease
Interventions
- Joint protection to decrease the risk of a hip fracture[28]
- Gait training
- Walker, crutches or wheelchair
- Patient education
Caesarean Section and Physiotherapy[edit | edit source]
Caesarean births are prevalent in many countries. Untreated pain associated with caesarean birth may lead to opioid use or depression. Physiotherapists can play a key role in pain management and are well equipped to help women with:
- Early mobilisation
- Progressive functioning
- Early strengthening
- Stress management
- Scar management
Other Common Problems during Childbearing Years[edit | edit source]
- Headaches
- Tension headaches, migraines
- Headache
- Headaches and Dizziness
- Tension-type headache
- Neck and shoulder pain
- Musculoskeletal changes during pregnancy
- Shift in centre of gravity
- Postpartum muscle imbalances
- Wrist pain
- Foot
- Increased weight and hormonal changes (laxity of ligaments)
- Education on proper footwear
Orthotic Supports[edit | edit source]
It is important to accurately assess what type of orthotic support the patient needs. Sacroiliac belts and maternity supports feel very different and support different structures. The sacroiliac belt supports the pelvic ring and sacroiliac joint whereas the maternity supports provide support to the abdominal wall, and a lifting type support.
Read more about Sacroiliac belts here: The PGM Method - Sacroiliac Belt and Patient Education
Maternity supports[edit | edit source]
There are many maternity supports available on the market. Examples of some are:
- FitSplint
- BellyBra
- Compression short
Exercise Guidelines during Pregnancy and Postpartum[edit | edit source]
Regular physical activity during pregnancy and postpartum is advised.
This recent article provides valuable information on exercise during pregnancy and postpartum: Physical Activity and Exercise During Pregnancy and the Postpartum Period.[12] The principles of exercise prescription for pregnant women are similar to those for the general population. The goal is moderate-intensity exercise for 20-30 minutes per day on most or all days of the week. The exercise program should be developed with the patient and adjusted as needed. The Borg ratings of perceived exertion scale or the “talk test” are ways to measure exertion.
There is no evidence that bed rest or activity restrictions reduce the risk for preterm labour or preeclampsia and should not be routinely recommended.
Exercise during the Postpartum Period[edit | edit source]
Women’s level of participation in exercise reduces after childbirth and this often leads to weight gain and obesity. It is important to resume exercise or physical activity routines after childbirth to support lifelong healthy habits. Regular aerobic exercise in lactating women improves maternal cardiovascular fitness and does not affect milk production or infant growth.
Postpartum Care[edit | edit source]
ACOG recommends that postpartum care should be an ongoing process to optimise the health of women and infants. Read more about these recommendations here: Optimising Postpartum Care
See also: Physical Activity and Pregnancy
Depression[edit | edit source]
Prenatal and postpartum depression is unfortunately common. Postpartum depression ranges from blues to depression to psychosis. It is important to screen for depression as it can be difficult to assess without specifically asking certain questions. A recommended screening tool for postpartum depression is the Edinburgh Postnatal Depression Scale. For more discussion and screening tool recommendations see Screening for Perinatal Depression
Lifestyle Issues[edit | edit source]
Lifestyle issues are important to address during pregnancy and postpartum as women are undergoing or have undergone significant changes in mood, sleep, nutrition , stress/anxiety, physical demands, as well as possibly experiencing musculoskeletal problems. In addition women are dealing with many biopsychosocial factors such as fluctuating hormones, adjustment to a different body image, and social changes.
References[edit | edit source]
- ↑ 1.0 1.1 Clinton SC, Newell A, Downey PA, Ferreira K. Pelvic girdle pain in the antepartum population: physical therapy clinical practice guidelines linked to the international classification of functioning, disability, and health from the Section on Women's Health and the Orthopaedic Section of the American Physical Therapy Association. Journal of Women's Health Physical Therapy. 2017 May 1;41(2):102-25.
- ↑ Kristiansson P, Svärdsudd K, von Schoultz B. Serum relaxin, symphyseal pain, and back pain during pregnancy. American journal of obstetrics and gynecology. 1996 Nov 1;175(5):1342- 7
- ↑ Ramprasad M, Bhattacharyya SS, Bhattacharyya A. Thyroid disorders in pregnancy. Indian journal of endocrinology and metabolism. 2012 Dec;16(Suppl 2):S167.
- ↑ 4.0 4.1 Alemu A, Terefe B, Abebe M, Biadgo B. Thyroid hormone dysfunction during pregnancy: A review. International Journal of Reproductive BioMedicine. 2016 Nov;14(11):677
- ↑ That nursing prof. Need to know pregnancy hormones. Available from https://www.youtube.com/watch?v=9dPNI4HnmjY (last accessed 11 June 2021)
- ↑ Ming WK, Ding W, Zhang CJ, Zhong L, Long Y, Li Z, Sun C, Wu Y, Chen H, Chen H, Wang Z. The effect of exercise during pregnancy on gestational diabetes mellitus in normal-weight women: a systematic review and meta-analysis. BMC pregnancy and childbirth. 2018 Dec;18(1):1-9
- ↑ De Kat AC, Hirst J, Woodward M, Kennedy S, Peters SA. Prediction models for preeclampsia: a systematic review. Pregnancy hypertension. 2019 Apr 1;16:48-66
- ↑ Alila Medical Media. Gestational Diabetes, Animation. Available from https://www.youtube.com/watch?v=UIQgolIGQEU (last accessed 3 May 2021)
- ↑ Brigham and Women’s Hospital. Preeclampsia video. Available from https://www.youtube.com/watch?v=Dz8tPyeLvBI&t=254s
- ↑ 10.0 10.1 10.2 Gomes CF, Sousa M, Lourenço I, Martins D, Torres J. Gastrointestinal diseases during pregnancy: what does the gastroenterologist need to know?. Annals of gastroenterology. 2018 Jul;31(4):385
- ↑ Szweda H, Jóźwik M. Urinary tract infections during pregnancy-an updated overview. Dev Period Med. 2016;20(4):263-72
- ↑ 12.0 12.1 12.2 12.3 12.4 12.5 Mota P, Bø K. ACOG Committee Opinion No. 804: Physical Activity and Exercise During Pregnancy and the Postpartum Period. Obstetrics & Gynecology. 2021 Feb 1;137(2):376
- ↑ Soma-Pillay P, Catherine NP, Tolppanen H, Mebazaa A, Tolppanen H, Mebazaa A. Physiological changes in pregnancy. Cardiovascular journal of Africa. 2016 Mar;27(2):89
- ↑ Program for Pregnancy and Postpartum Health. Pregnancy and the Cardiovascular System. Available from https://www.youtube.com/watch?v=RtQyy_K76QY (last accessed 3 May 2021)
- ↑ 15.0 15.1 Humphries A, Mirjalili SA, Tarr GP, Thompson JM, Stone P. Hemodynamic changes in women with symptoms of supine hypotensive syndrome. Acta obstetricia et gynecologica Scandinavica. 2020 May;99(5):631-6.
- ↑ 16.0 16.1 16.2 Warland J. Back to basics: avoiding the supine position in pregnancy. The Journal of physiology. 2017 Feb 15;595(4):1017.
- ↑ Khan F, Vaillancourt C, Bourjeily G. Diagnosis and management of deep vein thrombosis in pregnancy. Bmj. 2017 May 31;357
- ↑ McLendon K, Attia M. Deep Venous Thrombosis (DVT) Risk Factors. InStatPearls [Internet] 2019 Mar 1. StatPearls Publishing
- ↑ Deborah Riczo. The PGM Method- Pregnancy and Postpartum Considerations Course. Plus. 2021
- ↑ Kendall FP, McCreary EK, Provance PG, Rodgers MM, Romani WA. Muscles: Testing and function, with posture and pain (Kendall, Muscles). LWW. 2005
- ↑ Dent BM, Al Samaraee A, Coyne PE, Nice C, Katory M. Varices of the round ligament mimicking an inguinal hernia–an important differential diagnosis during pregnancy. The Annals of the Royal College of Surgeons of England. 2010 Oct;92(7):e10-1.
- ↑ 22.0 22.1 Herren C, Sobottke R, Dadgar A, Ringe MJ, Graf M, Keller K, Eysel P, Mallmann P, Siewe J. Peripartum pubic symphysis separation–Current strategies in diagnosis and therapy and presentation of two cases. Injury. 2015 Jun 1;46(6):1074-80
- ↑ 23.0 23.1 Palmer E, Redavid L. Pelvic Girdle Pain: an Overview. Richman S, ed. CINAHL Rehabilitation Guide. Published online August 2, 2019
- ↑ Lirette LS, Chaiban G, Tolba R, Eissa H. Coccydynia: an overview of the anatomy, etiology, and treatment of coccyx pain. Ochsner Journal. 2014 Mar 20;14(1):84-7
- ↑ 25.0 25.1 Maher RM, Iberle J. Concurrent Validity of Noninvasive Coccygeal Motion Palpation and Transabdominal Ultrasound Imaging in the Assessment of Pelvic Floor Function in Women. Journal of Women's Health Physical Therapy. 2020 Oct 9;44(4):176-81
- ↑ Scott KM, Fisher LW, Bernstein IH, Bradley MH. The treatment of chronic coccydynia and postcoccygectomy pain with pelvic floor physical therapy. PM&R. 2017 Apr 1;9(4):367-76.
- ↑ Hadji P, Boekhoff J, Hahn M, Hellmeyer L, Hars O, Kyvernitakis I. Pregnancy-associated transient osteoporosis of the hip: results of a case-control study. Archives of osteoporosis. 2017 Dec 1;12(1):11.
- ↑ Boissonnault WG, Boissonnault JS. Transient osteoporosis of the hip associated with pregnancy. Journal of Orthopaedic & Sports Physical Therapy. 2001 Jul;31(7):359-67