Sleep: Older People
Original Editor - Lucinda hampton
Top Contributors - Lucinda hampton, Kim Jackson and Cindy John-Chu
Introduction[edit | edit source]
Adults need only one sleep daily. However, many elderly may struggle to obtain those 8 h in one block.[1]
Sleep disturbances pose a significant medical and public health concern for our nation’s aging population. An estimated 50% of persons 55 years and older have some form of sleep problem, including initiating and maintaining sleep. Older adults report the highest prevalence of sleep problems compared with younger age groups when quantified by self-report and by biological assessment. Moderate sleep disturbances in older adults are often associated with deficits in daytime functioning including elevated levels of fatigue; disturbed mood, such as depressive symptoms; and reduced quality of life and lead to the onset of clinical insomnia[2].
Despite the medical consequences of sleep problems, they often go untreated in older adults, especially among those with moderate sleep disturbances.[2]
Assessment[edit | edit source]
Assessment of sleep disorder should include evaluation for secondary causes if any (see aforementioned link).[3]
Many people believe that poor sleep is a normal part of ageing, but it is not. In fact, many healthy older adults report few or no sleep problems. Sleep patterns change as we age, but disturbed sleep and waking up tired every day are not part of normal ageing[4].
Consequences[edit | edit source]
- Poor sleep is associated with increased fatigue, falls, nursing home placement, poor quality of life, and overall mortality. Additionally functional restrictions occur eg lessening of grip strength, reduction of physical activity, and reduction of muscle mass and function[5].
- Bad sleep quality and low sleep efficiency in older people are associated not only with functional restrictions such as lessening of grip strength and reduction of physical activity, but also with muscle mass and function.
- Non-restorative sleep is associated with metabolic (insulin resistance) and hormonal changes[5].
Ageing: Sleep Change[edit | edit source]
After middle age, our body clock gradually changes. With ageing the hormones that help us sleep are released earlier in the day. Some older adults may feel sleepy earlier than they used to and they make wake up in the early hours of the morning. Melatonin is a hormone that is produced naturally in the body at night which promotes sleep, older people make less melatonin making it harder to get to sleep. Other age changes may interfere with sleep eg hot flushes in postmenopausal women, the need to go to the toilet during the night, pain making it difficult to stay in one position for the whole night, day time napping.
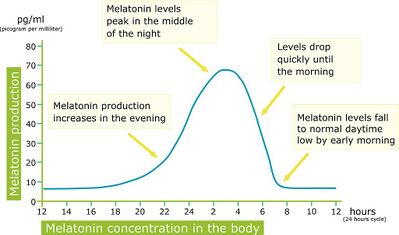
Image 2: Peaks and troughs in the body's Melatonin production during the circadian (sleep) cycle represented in a 24-hour period.
Older Age Health Problems[edit | edit source]
Many conditions can make it harder to sleep for older people eg arthritis, osteoporosis, Parkinson’s, Urinary Incontinence, indigestion, heart disease and lung diseases such as asthma or COPD. Poor sleep may not simply be related to getting older. Stress, depression, anxiety, medications, pain and many other factors may all contribute[6].
- Anxiety and depression can both interfere with getting off to sleep as well as cause wakefulness during the night.
- Dementia or Alzheimer’s disease can make sleep worse. Two-thirds of nursing home residents have problems with their sleep (sleep problems tend to increase when there is not enough exercise or interesting activities during the day or people go to bed too early).
- At least 1 in 4 older people have sleep apnea or periodic limb movement disorder.[6]
See Sleep Deprivation and Sleep Disorders
Treatment[edit | edit source]
Treatment for a sleep problem depends on the cause, so the issue has to be diagnosed before treatment commences. Talking to a doctor about sleeping problems is important. The person might need a referral to see a sleep specialist. There are a variety of effective treatments for snoring, sleep apnoea, restless legs, insomnia and other common sleep problems. Examples of treatments include:
- Education about sleep hygiene and expected changes with aging, stimulus control, decreased daytime sleep and dietary modifications are the first line of treatment for insomnia[3]
- Cognitive behaviour therapy (CBT) is very effective for clinically diagnosed insomnia, however not everyone with milder sleeping difficulties needs such an intensive treatment. CBT helps people to change unhelpful thoughts and behaviours that contribute to poor sleep.
- For some people, sleep quality can be improved by learning relaxation to reduce physical tension and worry.
- Another approach that is showing promise for improving sleep is to learn mindfulness.[7] Formalized mindfulness-based interventions may serve to remediate sleep problems among older adults in the short term, and this effect carries over into reducing sleep-related daytime impairment that has implications for quality of life[2].
- Prescription for melatonin (a synthetic version of the hormone naturally produced by the body and sold as Circadin).
- Medication for short-term relief, should not be used for longer than four weeks (sleeping tablets increase the risk of falls in some older people).[6]
Physiotherapy[edit | edit source]
Physiotherapists can recommend exercise as a treatment plan in order to boost the health and sleep of people and maintain physical well-being of a person.
Exercise can be helpful in improving the sleep quality of people suffering from sleeplessness and has a therapeutic effect on individuals suffering from sleep disorders. It is beneficial in promoting sleep and reduces worry, anxiety and depressive symptoms among patients. And as a bonus, exercise reduces the death and disease rate.[8]
See also Physical Activity in Older Adults
References[edit | edit source]
- ↑ Gulia KK, Kumar VM. Sleep disorders in the elderly: a growing challenge. Psychogeriatrics. 2018 May;18(3):155-65. Available: https://pubmed.ncbi.nlm.nih.gov/29878472/ (accessed 1.10.2021)
- ↑ 2.0 2.1 2.2 Black DS, O’Reilly GA, Olmstead R, Breen EC, Irwin MR. Mindfulness meditation and improvement in sleep quality and daytime impairment among older adults with sleep disturbances: a randomized clinical trial. JAMA internal medicine. 2015 Apr 1;175(4):494-501.Available: https://jamanetwork.com/journals/jamainternalmedicine/fullarticle/2110998(accessed 2.10.2021)
- ↑ 3.0 3.1 Ghimire K, Dahal R. Geriatric Care Special Needs Assessment.Available: https://www.ncbi.nlm.nih.gov/books/NBK570572/(accessed 1.10.2021)
- ↑ AASM Sleeping problems Available: https://sleepeducation.org/sleep-growing-older/ (accessed 2.10,2021)
- ↑ 5.0 5.1 Buchmann N, Spira D, Norman K, Demuth I, Eckardt R, Steinhagen-Thiessen E. Sleep, muscle mass and muscle function in older people: a cross-sectional analysis based on data from the Berlin Aging Study II (BASE-II). Deutsches Ärzteblatt international. 2016 Apr;113(15):253.Available:https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4860870/ (accessed 1.10.2021)
- ↑ 6.0 6.1 6.2 Sleep health foundation Older people and sleeping Available:https://www.sleephealthfoundation.org.au/older-people-and-sleeping.html (accessed 2.10.2021)
- ↑ The Conversation Good sleep gets harder as we age, but mindfulness could help Available: https://theconversation.com/good-sleep-gets-harder-as-we-age-but-mindfulness-could-help-37756 (accessed 2.10.2021)
- ↑ Physiopedia Effects of Exercise on SleepAvailable:https://www.physio-pedia.com/Effects_of_Exercise_on_Sleep?utm_source=physiopedia&utm_medium=related_articles&utm_campaign=ongoing_internal (accessed 2.10.2021)