Reflexes
Original Editor - Lucinda hampton
Top Contributors - Chrysolite Jyothi Kommu, Lucinda hampton, Kim Jackson, Naomi O'Reilly, Rachael Lowe, Vidya Acharya, Rishika Babburu and Ahmed M DiabSpinal Reflex/The Reflex Arc[edit | edit source]
A reflex is an involuntary and nearly instantaneous movement in response to a stimulus. The reflex is an automatic response to a stimulus that does not receive or need conscious thought as it occurs through a reflex arc. Reflex arcs act on an impulse before that impulse reaches the brain.[1]
Reflex arcs can be
- Monosynaptic i.e., contain only two neurons, a sensory and a motor neuron. Examples of monosynaptic reflex arcs in humans include the patellar reflex and the Achilles reflex.
- Polysynaptic i.e., multiple interneurons (also called relay neurons) that interface between the sensory and motor neurons in the reflex pathway.[2]
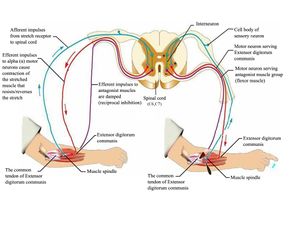 Illustration of the reflex arc.
Illustration of the reflex arc.
Video of reflex arc
Types of Reflexes[edit | edit source]
Reflexes are the body’s intrinsic stimulus-response systems for maintaining homeostasis, and when performed and interpreted correctly are the most objective evidence within the neurological screen to localise the lesion to specific structures within the nervous system. Reflexes may be divided into 4 groups:[3]
Superficial Reflexes[edit | edit source]
Superficial reflexes are usually elicited by stroking the skin or mucous membranes. Abnormal reflex response will show a combination of diminished or absent superficial reflexes with deep reflexes and pathological reflexes indicates upper motor neuron level (UMNL) involvement.
| Type of Reflex | Characteristic | Reflex | Afferent Nerve | Segmental Innervation | Action | Normal Reflex Response |
|---|---|---|---|---|---|---|
| Skin Reflexes | Elicited by stroking the skin. | Interscapular Reflex | Stroke skin of interscapular space | Scapulas draw inward | ||
| Upper and Lower Abdominal Reflexes | Medially stroke each side of abdomen above and below the umbilicus | Umbilical deviation toward the stimulus | ||||
| Gluteal Reflex | Stroke Buttocks | Contraction of Buttocks | ||||
| Anal Reflex | Pudendal | S4-5 | Stroke Perianal Area or Insert Gloved Finger into Rectum | Contraction Sphincter Ani | ||
| Cremasteric Reflex | Stroke Inner Thigh | Testicular Elevation | ||||
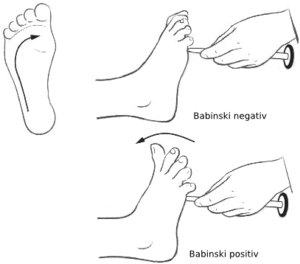
| Plantar Reflex
(Babinski Reflex) |
Tibial | S1-2 | Stroke Sole of Foot | Plantar Flexion of Toes | ||
| Mucous Membrane Reflexes | Elicited by stroking the mucous membranes. | Corneal Reflex | Touch Cornea with Cotton | Blinking | ||
| Gag Reflex | Irritate Pharynx with Tongue Depressor | Gagging | ||||
| Uvular Reflex | Phonation of "Ahh" or Irritation of Posterior Third Tongue with Tongue Depressor | Uvular Elevation | ||||
| Sneeze Reflex | Irritate Nasal Membrane | Sneeze |
Plantar response, abdominal reflex, cremasteric reflex, corneal reflex[4]
- Abdominal reflex-is stimulated by stroking around the abdomen which helps in determining the level of CNS lesion.[5]
- Cremasteric reflex-It is elicited when the inner part of thigh is stroked in males (Geigel reflex is the counterpart in females). This reflex helps in evaluation of acute scrotal pain and assessing for testicular torsion(associated with loss of reflex)[6].
- Corneal reflex-It is elicited by gentle stroking on the cornea with a cotton swab. This reflex mainly helps in knowing the damage peripherally to either the trigeminal nerve (V) or facial nerve (VII) nerve will disrupt the corneal blink circuit. [7]
- Plantar reflex-abnormal reflex indicates metabolic or structural abnormality in the corticospinal system upstream from the segmental reflex.[8]
Deep Tendon Reflexes[edit | edit source]
Evaluates afferent nerves, synaptic connections within the spinal cord, motor nerves, and descending motor pathways. Lower motor neuron lesions (eg affecting the anterior horn cell, spinal root or peripheral nerve) depress reflexes: upper motor neuron lesions increase the reflexes.
Reflexes tested include the following:
- Biceps (innervated by C5 and C6)
- Radial brachialis (by C6)
- Triceps (by C7)
- Distal finger flexors (by C8)
- Quadriceps knee jerk (by L4)
- Ankle jerk (by S1)
- Jaw jerk (by the 5th cranial nerve)
Note any asymmetric increase or decrease. Jendrassik maneuver can be used to augment hypoactive reflexes i.e., the patient locks hands together and pulls vigorously apart as a tendon in the lower extremity is tapped or pushs the knees together against each other, while the upper limb tendon is tested.[9] </section><section></section>
Visceral Reflexes[edit | edit source]
Pathologic Reflexes[edit | edit source]
Pathological or primitive reflexes are considered typical in infants up to about 6 months of age (or even up to 2 years for certain reflexes, such as Babinski’s sign) and disappear. These primitive reflexes are pathological if found in adults, and outside of the realm of what is considered to be normal, and are indicative of an underlying problem with the nervous system. Pathologic reflexes (eg, Babinski, rooting, grasp) are reversions to primitive responses and indicate loss of cortical inhibition.
Visceral Reflexes[edit | edit source]
Reflex Testing[edit | edit source]
- The muscle group to be tested must be in a neutral position (i.e. neither stretched nor contracted).
- The tendon attached to the muscle(s) which is/are to be tested must be clearly identified. Place the extremity in a positioned that allows the tendon to be easily struck with the reflex hammer.
- To easily locate the tendon, ask the patient to contract the muscle to which it is attached. When the muscle shortens, you should be able to both see and feel the cord like tendon, confirming its precise location.
- Strike the tendon with a single, brisk, stroke. You should not elicit pain.
This grading system is rather subjective.
- 0 No evidence of contraction
- 1+ Decreased, but still present (hypo-reflexic). Hyporeflexia is generally associated with a lower motor neuron deficit (at the alpha motor neurons from spinal cord to muscle) eg Guillain–Barré syndrome
- 2+ Normal
- 3+ Super-normal (hyper-reflexic) Hyperreflexia is often attributed to upper motor neuron lesions eg Multiple sclerosis
- 4+ Clonus: Repetitive shortening of the muscle after a single stimulation[10]
Note any asymmetric increase or depression. Jendrassik manoeuvre can be used to augment hypoactive reflexes i.e., the patient locks the hands together and pulls vigorously apart as a tendon in the lower extremity is tapped or can push the knees together against each other, while the upper limb tendon is tested.
The video below illustrates the testing of the deep tendon reflexes
The video below illustrates Jendrassik manoeuvre
Reference[edit | edit source]
- ↑ Wikipedia. Reflex. Available from: https://en.wikipedia.org/wiki/Reflex (last accessed 21.4.2019)
- ↑ Lumen. Reflexes. https://courses.lumenlearning.com/boundless-ap/chapter/reflexes/ (last accessed 21.4.2019)
- ↑ Shibasaki, Hiroshi, and Mark Hallett, 'Tendon Reflexes and Pathological Reflexes', The Neurologic Examination: Scientific Basis for Clinical Diagnosis, 1 edn (New York, 2016; online edn, Oxford Academic, 1 Aug. 2016), https://doi.org/10.1093/med/9780190240974.003.0017, accessed 19 June 2023.
- ↑ http://teachneuro.blogspot.com/2013/01/the-corneal-or-blink-reflex.html?m=1
- ↑ https://en.wikipedia.org/wiki/Abdominal_reflex
- ↑ https://www.ncbi.nlm.nih.gov/books/NBK513348/#
- ↑ https://www.ncbi.nlm.nih.gov/books/NBK534247/
- ↑ https://www.ncbi.nlm.nih.gov/books/NBK397/
- ↑ MDA Maunaul. How to assess reflexes. Available from: https://www.msdmanuals.com/professional/neurologic-disorders/neurologic-examination/how-to-assess-reflexes (last accessed 21.4.2019)
- ↑ University of California. The neurological examination. Available from: https://meded.ucsd.edu/clinicalmed/neuro3.htm (last accessed 21.4.2019)
- ↑ Justin Vaida Deep tendon reflexes. Available from: https://www.youtube.com/watch?v=H1b-iKf2CuY (last accessed 21.4.2019)