Psychological Approaches to Pain Management
Original Editor - Scott Buxton
Top Contributors - Scott Buxton, Admin, Evan Thomas, Lauren Lopez, Kim Jackson, Vidya Acharya, 127.0.0.1, WikiSysop and Tolulope Adeniji
What is Pain Management? [edit | edit source]
Pain management is an area of modern medicine which utilises the multi-disciplinary team to help ease the pain and suffering of patients living with long-term pain to improve their quality of life[1]. Medicine is usually the first port of call to manage pain, however, when pain is not responsive to medication, or resistant to treatment, or persists after healing has occurred and an exact cause of the pain has not been found the alternative treatment or a combined approach can be used[2].
The alternative to medicine or combined approaches to pain management are broad and each of which can be based upon different paradigms of understanding pain. The different approaches come from the wide range of healthcare professionals unique treatments towards pain management, not only limited to Mental-Health or Psychiatrists but can include Physiotherapists, Occupational Therapists, Nurse Practitioners, Medics, Nuse Specialists and Massage Therapists.
Different Types of Management/Treatment[edit | edit source]
The techniques these professionals use can be and not limited to: (This list is not exhaustive and please add more!)
- Patient Education
- Operant Conditioning Approaches
- Cognitive Behavioural Therapy
- Distraction
- Classical Conditioning Approaches
- Social Support Methods
- Relaxation Methods
- Acceptance and Commitment Therapy
- Hypnosis
- Biofeedback
What Is the Psychological Approach to Pain Management[edit | edit source]
As well as the neural interactions and links the brain goes through when a person is in pain, there are multiple layers of complex abstract thoughts and feelings a person goes through which culminates how much pain a person feels and how they deal with pain. Their cognitive constructs, behavioural constructs and environmental influences are all intertwined in a complex web of individuality which need to be considered and incorporated into any treatments for them to be effective and are found out during an initial assessment[3]. It is these personal, individual and holistic areas which make it a psychological approach sitting within the biopsychosocial model of patient treatment. The psychological approach recognizes that pain is not solely a physical sensation, but also involves psychological and social factors.[4] By considering a person's cognitive and behavioural constructs, as well as their environmental influences, healthcare professionals can gain a comprehensive understanding of the individual's pain experience. This holistic approach is crucial in developing effective treatment plans within the biopsychosocial model, as it takes into account the unique needs and circumstances of each patient.
Assessment Considerations[edit | edit source]
According to Asmundson et al[3] an in-depth and thorough assessment is required to discover the root cause of psychological aspects of pain and person specific influence which will be integral to know when it comes to selection and direction of treatment. There are a number of areas which need to be covered in the assessment but arguably the most important is the consideration of the pain intensity, severity and irritability along with location, distribution and duration. This is a useful marker for measuring pain and as a tool for differential diagnosis but asking how the patient is affected functionally is an important consideration but also cruical to confirming the subjective reports of the patient. Tools such as the Visual Analogue Scale, 4-Item Pain Intensity Measure or the Short-form McGill Pain Questionnaire. Another area of consideration are the various "empirically supported and theoretically relevant cognitive, behavioural and environmental influences" which are person specific and can aid in assessment and conclusions relevant for treatment[3].
The idea of looking out for cognitive, behavioural and environmental influences ties with the concept of the Flag System which includes Yellow, Blue, Orange, Black and Red flags as universal indicators of how different psychological, and clinical signs can influence treatment outcomes. Head over to the page to find out more about it.
Psychological Interventions[edit | edit source]
Cognitive Behavioural Therapy[edit | edit source]
Cognitive Behavioural Therapy (CBT) is Cognitive Behavioural Therapy (CBT) is a method that can help manage problems by changing the way patients would think and behave. It is not designed to remove any problems but help manage them in a positive manner[5] [6].
Behaviour therapy (BT) was developed in the 1950’s independently in three countries: South Africa, USA and England [7]. It was further developed to Cognitive Therapy (CT) in the 1970’s by Dr Aaron Beck with its main application on people with depression, anxiety and eating disorders [5] [8]. However, the main evidence today focuses on CBT, after the merging of BT and CT in the late 80’s [9].
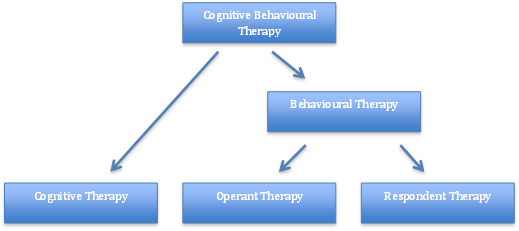
Below is a breakdown of the different aspects of CBT as a concept incorporating its namesake; both cognitive and behavioural elements. These elements can be taken further and take into account two of the most important theories to a behaviourist: operant and classical (respondent) conditioning.
Fig.2 - Breakdown of CBT theory
CBT assumes that changing maladaptive thinking leads to change in behavior. Therapists help individuals challenge their patterns and beliefs and replace "errors in thinking such as overgeneralizing, magnifying negatives, minimizing positives and catastrophizing" with more realistic and effective thoughts, decreasing emotional distress and self-defeating behavior. By challenging an individual's way of thinking and the way that he/she reacts to certain habits or behaviors in a constructive manner can create cognitive dissonance and therefore an opportunity to alter someones thinking patterns and behaviour[10]. Put simply CBT helps you think positively, realistically and rationally about a situation, for example here is a scenario fron the Royal College of Pscyhiatrists (Website)[11]:
You've had a bad day, feel fed up, so go out shopping. As you walk down the road, someone you know walks by and, apparently, ignores you. This starts a cascade of:
| Unhelpful | Helpful | |
| Thoughts: | He/She ignored me - they don't like me | He/She looks wrapped up in themselves - I wonder if there is something wrong? |
| Emotional Feelings: | Low, Sad and Rejected | Concerned for the other person, positive |
| Physical: | Stomach cramps, low energy, feel sick | None- feel comfortable |
| Action: | go home and avoid them | Get in touch to make sure they are ok |
According to the Royal College of Psychiatrists this can be a typical CBT session[11]:
- You will usually meet with a therapist for between 5 and 20, weekly, or fortnightly sessions.
- Each session will last between 30 and 60 minutes.
- You and the therapist will usually start by agreeing on what to discuss that day.
- With the therapist, you break a / each problem down into its separate parts. To help this process, your therapist may ask you to keep a diary. This will help you to identify your individual patterns of thoughts, emotions, bodily feelings and actions.
- Together you will look at your thoughts, feelings and behaviours to work out if they are unrealistic or unhelpful and how they affect you.
- The therapist will then help you to work out how to change unhelpful thoughts and behaviours.
- It's easy to talk about doing something, much harder to actually do it. So, after you have identified what you can change, your therapist will recommend 'homework' - you practise these changes in your everyday life.
CBT has six phases[10]:
- Assessment or psychological assessment;
- Reconceptualization;
- Skills acquisition;
- Skills consolidation and application training;
- Generalization and maintenance;
- Post-treatment assessment follow-up.
The reconceptualization phase makes up much of the "cognitive" portion of CBT.
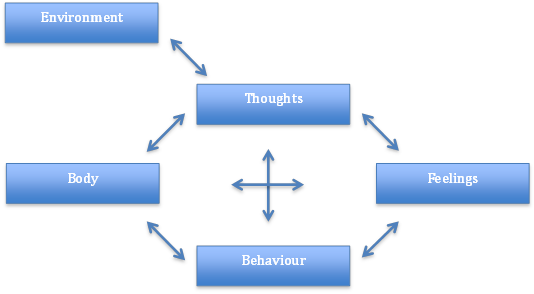
A simplistic and broad understanding of the CBT model and cycle are shown below.
Fig.3 - Factors involved within the Cognitive Behavioural Therapy Model
In terms of clinical relevance CBT has been the subject of many different studies, the majority of which are not within a physiotherapists scope of practice such a substance abuse, child abuse, schizophrenia and personality disorders however as the theory develops and our profession grows it is becoming more clinically relevant. Areas such as musculoskeletal outpatients can use specially trained therapists to treat fibromyalgia[12], low back pain[10] and chronic pain.
Here is a link to a list of Cochrane Reviews including the phrase "Cognitive Behavioural Therapy"
Reconceptualising Pain[edit | edit source]
It is natural to be fearful of pain, after all it is a natural educational tool and vastly unpleasant feeling. When pain persists patients can become fearful of pain and subsequently stop doing things which cause them pain, in main examples this may be movements which is common in osteoarthritis. This fear of pain can become a perpetual cycle towards chronic pain and disability and through the use of education, reconceptualising pain, CBT and the other approaches on this page the cycle can be broken.
Adjunct Interventions[edit | edit source]
Relaxation Therapy[edit | edit source]
Relaxation is usually used in conjunction with other treatment modalities and can take on a number of forms such as spiritual or non-spiritual meditation, progressive relaxation or muscular contraction and relaxation, even imagery[13]. Typically Relaxation would count as an "Alternative" treatment and recommended to be used along side traditional medical management as opposed to on its own. This may be due to a lack of high quality evidence or unproven theoretical fundamentals underpinning the treatment. The National Institutes of Health's National Center for Complementary and Alternative Medicine (NCCAM) defines mind–body medicine as “behavioural, psychologic, social and spiritual approaches to medicine not commonly used[13].”
One way in which relaxation therapy may work is to reduce the effect of stress on the body restoring normal equilibrium within the body systems[14]. At its most basic level, when under stress your body enters a fight or flight mechanism and a number of biochemical changes occur. Heart-rate, blood pressure increases, blood vessels narrow as well as several hormone responses such as adrenaline and cortisol as well as the neurotransmitter serotonin all increasing. These responses are essential in the short term but when these responses (as well as others) prolong and become chronic several damaging consequences occur. These may be fatigue, hypertension, anxiety, suppression of the immune system, reduction of memory and increase in body fat all of which have knock-on consequences elsewhere in the body[15][14].
Regardless of the proposed mechanisms of effect, the effect on the patients psyche can be large enough to prove the treatment worthwhile. It is also important to consider the effect of a placebo treatment on pain. However studies have proven relaxation to reduce pain level more often than not in conjunction with another modality. For example Linton & Gotestam[16] investigated the use of relaxation therapy and relaxation therapy and operant techniques and its effect on chronic arthralgic pain. Relaxation was shown to be effective at reducing pain and that the group with operant conditioning were more effective at taking pain medications[16].
Caution needs to be taken with a large amount of relaxation research as it tends to be older research however there has been some more recent investigation. Spence et al[17] compared the use of relaxation therapy and biofeedback techniques on 48 patients with chronic upper limb pain. Patients were divided into 4 treatment groups (relaxation, biofeedback, combined and 1 control) each receiving treatment twice-a-week for 4 weeks. All 3 treatment groups proved effective initially and at a 3 moth follow up. However the most effective treatment at reducing measures of pain, distress, interference in daily living, depression and anxiety was relaxation therapy (alone). At 6 months there was no difference between treatment groups[17].
Massage[edit | edit source]
Massage therapy, similar to relaxation, is typically used as an adjunct to traditional treatment modalities[18]. It is usually used alongside and compared to relaxation and other psychological treatments so was considered worthwhile to include in this article, relaxation is also considered to be one of the mechanisms of action of massage. According to Massage Today massage is:
"...the application of various techniques to the muscular structure and soft tissues of the body that include applying fixed or movable pressure, holding, vibration, rocking, friction, kneading and compression using primarily the hands..."[19]
Massage therapy has been around since the 2nd Century BC and has since developed a number of different approaches and branches such as Swedish massage, Shiatsu, Rolfing, reflexology and craniosacral therapy[20] .
A Cochrane review appraised the research involving massage and chronic low back pain. The review appraised nine articles (8 RCTs), A large number of studies were excluded from the review as not including massage as a solitary treatment, confirming further that massage is typically an adjunct. Of the eight trials, five were judged to be of high methodological quality and three were low quality[18].
One of the studies compared massage to a placebo treatment and massage was found to be more effective. The other seven studies showed that massage was superior to relaxation, acupuncture and education and no significant difference between corsets and exercises. Massage was less effective than spinal manipulation and transcutaneous electrical nerve stimulation (TENS)[18].
Biofeedback[edit | edit source]
Some of this information is taken from the Physiopedia page on Biofeedback, please visit for further information.
Biofeedback is a multi faceted tool utilising equipment to reveal to human beings some of their internal physiological events, normal and abnormal, in the form of visual and auditory signals in order to teach them to manipulate these otherwise involuntary or unfelt events by manipulating the displayed signals[21]. The concept has developed rapidly in recent years and will continue to as technology develops here is a list of some examples[22][23]:
- Electromyography (EMG) which measures muscle tension
- Thermal biofeedback which measures skin temperature
- Neurofeedback/ electroencephalography (EEG) which measures brain wave activity
- Electrodermography (EDG) which measures skin electrical activity
- Heat Flux which measures the rate at which heat is being dissipated from body
- Pneumography which measures abdominal/chest movement when breathing
- Capnometer which measures end-tidal CO2
- Hemoencephalography which measures the differences in the colour of light reflected back through the scalp based on the relative amount of oxygenated and unoxygenated blood in the brain
- Photoplethysmograph (PPG) which measures peripheral blood flow, heart rate and heart rate variability
Again this is typically a treatment that needs to be used in conjunction with treatments such as postural reeducation, exercise or relaxation to maximise their effectiveness, as demonstrated by a case study by Jepson[24]. The case study involves a 45-year-old female who was involved in 4 car accidents over 15 years. The patient had no obvious pathology on MRI or x-ray but was complaining of chronic pain specifically headaches and soreness in the cervical paraspinal muscles, right morse so than the left which feels tight. VAS score of 2-10 at best and 8 of 10 at worst usually brought on by driving more than 2.5 hours, bending, being in static positions for more than 15 to 20 minutes as well as reaching overhead. The pain has responded to TENS and heat but is now creating disturbances in normal daily life. After assessment it was decided that relaxation, TENS, and stretching would be used initially and then over the following weeks EMG would be used to utilise feedback of relaxation and overactivity of muscles. EMG would then be used during functional tasks to correct any movement abnormalities which could be contributing to the pain. At a 1-year follow up pain had been reduced to VAS 2-3/10 with no pain lasting up to 2 days and 95% reduction in headaches and corrected posture. Additionally the patient reported being able to recognise and correct postural and muscular abnormalities before they became troublesome[25].
This case study is an example of how biofeedback can be used to enhance treatments which would usually be used, in this case exercise and postural reeducation by providing simple targets and practical proof to patients. As this is only a case study this may not be the case with all patients however.
Additional Biopsychosocial Models of Understanding Pain[edit | edit source]
The Behavioural Management of Chronic Pain by Fordyce[26]
A New Clinical Model for the Treatment of Low Back Pain. by Waddell[27].
Pain and Behavioural Medicine: A Cognitive-Behavioural Perspective. By Turk
The Neuromatrix and Pain by Melzack
Related Physiopedia pages[edit | edit source]
References[edit | edit source]
- ↑ Hardy, Paul A. J. (1997). Chronic pain management: the essentials. U.K.: Greenwich Medical Media
- ↑ Butler DS, Moseley GL. Explain pain. Adelaide: Noigroup Publications; 2003
- ↑ 3.0 3.1 3.2 Asmundson,G. Gomez-Perez,L. Richter, A. Carleton, RN. The psychology of pain: models and targets for comprehensive assessment. Chapter 4 in Hubert van Griensven’s Pain: A text book for health care professionals. Elsevier, 2014.
- ↑ Meints SM, Edwards RR. Evaluating psychosocial contributions to chronic pain outcomes. Progress in Neuro-Psychopharmacology and Biological Psychiatry. 2018 Dec 20;87:168-82.
- ↑ 5.0 5.1 Beck, J., 1995. Cognitive Therapy: Basics and Beyond. Guildford Press: New York
- ↑ NHS Choices, 2012. Cognitive behavioural therapy. [online] Available at:http://www.nhs.uk/conditions/cognitive-behavioural-therapy/Pages/Introduction.aspx[Accessed 8th Jan 2014]
- ↑ Öst, L.G., 2008. Efficacy of the third wave of behavioral therapies: a systematic review and meta-analysis. Behaviour research and therapy, 46(3): 296–321
- ↑ Hayes, S.C., 2004. Acceptance and commitment therapy, relational frame theory, and the third wave of behavioral and cognitive therapies. Behavior Therapy, 35: 639–665
- ↑ Roth, A., Fonagy, P. “What works for whom? A critical review of psychotherapy research”. 2nd ed. Guilford Press: New York 2005
- ↑ 10.0 10.1 10.2 Gatchel, Robert J.; Rollings, Kathryn H. (2008). "Evidence-informed management of chronic low back pain with cognitive behavioural therapy". The Spine Journal 8 (1): 40–4.
- ↑ 11.0 11.1 Cognitive Behavioural Therapy. RCPSYCH [ONLINE] Accessed from: https://www.rcpsych.ac.uk/mentalhealthinformation/therapies/cognitivebehaviouraltherapy.aspx 19/03/2014.
- ↑ Hassett, Afton L.; Gevirtz, Richard N. (2009). "Nonpharmacologic Treatment for Fibromyalgia: Patient Education, Cognitive-Behavioral Therapy, Relaxation Techniques, and Complementary and Alternative Medicine". Rheumatic Disease Clinics of North America 35 (2): 393–407.
- ↑ 13.0 13.1 Astin J. Mind–Body Therapies for the Management of Pain. Clinical Journal of Pain. 2004:1;27-32
- ↑ 14.0 14.1 National Centre for Complementary and Alternative Medicine. Relaxation Techniques for Health: An Introduction. [ONLINE] 24/03/2014 http://nccam.nih.gov/health/stress/relaxation.htm
- ↑ Wikipedia. Stress (Biology)[ONLINE] http://en.wikipedia.org/wiki/Stress_(biology) accessed 24/03/2014
- ↑ 16.0 16.1 Linton s. Gotestam k. A controlled study of the effects of applied relaxation and applied relaxation plus operant procedures in the regulation of chronic pain. British Journal of Clinical Psychology. 1984: 23(4)291-299
- ↑ 17.0 17.1 Spence S. Sharpe L. Newton-John t. Champion D. Effect of EMG biofeedback compared to applied relaxation training with chronic, upper extremity cumulative trauma disorders. Pain. 1995 63(2)199-206
- ↑ 18.0 18.1 18.2 Furlan AD, Brosseau L, Imamura M, Irvin E. Massage for low back pain. Cochrane Database Syst Rev 2002:CD001929.
- ↑ Massage Today. All About Massage. [ONLINE] available from http://www.massagetoday.com/aboutmt/ accessed 25/03/2014
- ↑ Tsao J.Effectiveness of Massage Therapy for Chronic, Non-malignant Pain: A Review MEDSCAPE. [ONLINE] Accessed from http://www.medscape.com/viewarticle/559775_1 25/03/2014
- ↑ Basmajian J. (1989), Biofeedback: Principles and Practices for Clinicians, Williams & Wilkins
- ↑ University of Maryland Medical Center (2011), Biofeedback, geraadpleegd op 1/05/2013,[ONLINE] http://www.umm.edu/altmed/articles/biofeedback-000349.htm
- ↑ Lockheed M. (2010), Biofeedback research report, geraadpleegd op 1/05/2013, http://www.etc.cmu.edu/projects/lm-motion/Research/biofeedbackResearch.pdf
- ↑ Jepson NA. Applications of biofeedback for patients with chronic pain. Techniques in Regional Anesthesia and Pain Management (2008) 12, 111-114
- ↑ Jepson NA. Applications of biofeedback for patients with chronic pain. Techniques in Regional Anesthesia and Pain Management (2008) 12, 111-114
- ↑ Fordyce W. Roberts A. Sternbach R. The behavioural management of chronic pain: A response to critics. Pain 22:2;113-25. 1985.
- ↑ Waddell G. 1987 Volvo award in clinical sciences. A new clinical model for the treatment of low-back pain. Spine. 1987 12;7:632-44