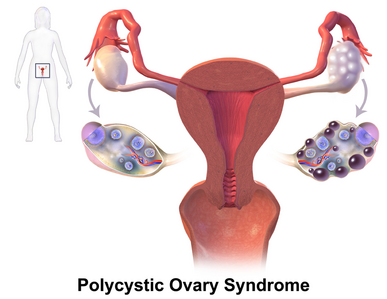
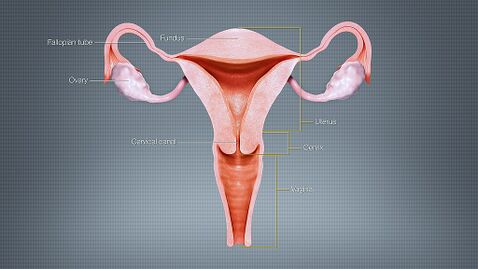
Polycystic Ovarian Syndrome
Original Editors - Amanda Tieken from Bellarmine University's Pathophysiology of Complex Patient Problems project.
Top Contributors - Amanda Tieken, Mudra Shah, Lucinda hampton, Admin, Kim Jackson, Jai Taylor, Aminat Abolade, Safiya Naz, Priyanka Chugh, Kirenga Bamurange Liliane, Rishika Babburu, Tony Varela, 127.0.0.1, Elaine Lonnemann, WikiSysop, Allyson Prieto, Demiana Farag, Macy Purifoy, Wendy Walker and Evan Thomas
Edited April 2023 - by Jai Taylor, Allyson Prieto, and Demiana Farag as part of the Arkansas Colleges of Health Education School of Physical Therapy Musculoskeletal 1 Project
Introduction[edit | edit source]
Polycystic ovarian syndrome (PCOS) is the most common hormonal disorder in females of reproductive age. It is characterized by two or more of the following:
- Irregular menstrual periods
- Hyperandrogenism
- Polycystic ovaries
Unfortunately PCOS is underdiagnosed, frequently taking a long time to be identified, often over a year.
Multiple morbidities are associated with PCOS, including infertility, metabolic syndrome, obesity, insulin resistance, type 2 diabetes mellitus, cardiovascular risk, depression, obstructive sleep apnea, endometrial cancer, and nonalcoholic fatty liver disease . [1][2].
Epidemiology[edit | edit source]
The estimated prevalence of PCOS is 8-13% of women of reproductive age but this varies (up to 20%) depending on the diagnostic criteria used .[3] It is currently recognized as the leading cause of anovulatory infertility and the most prevalent endocrine disorder amongst women of reproductive age. [4]
- 50% of these women have amenorrhea[5]
- 30% of these women have abnormal menstrual bleeding[5]
- 60% of these women are obese[6]
- 40% of women with PCOS have associated insulin resistance and type 2 diabetes mellitus[5]
Pathophysiology[edit | edit source]
Polycystic Ovarian Syndrome PCOS is believed to be a genetically inherited metabolic and gynecological disorder. A repetitive vicious cycle occurs with hormones resulting in the progression of PCOS. To begin with, failure of an ovary to release oocyte results in increased levels of androgen production released from the ovaries as well as the adrenal cortex. The excess androgen hormones in the system have a twofold effect. First, androgens are stored in adipose tissue where they are then converted into estrogen. Excess androgens then result in an increased production of Sex Hormone Binding Globulin (SHGB). This increased SHGB then has the consequence of an even greater fabrication of androgens and estrogens. Thus the cycle begins. The cause of the excess androgen production has been correlated to surplus Luteinizing hormone (LH) stimulation resulting in the presence of cystic changes in the ovaries.[7]
Characteristics/Clinical Presentation[edit | edit source]
Signs and symptoms of PCOS include the following:
- Enlarged polycystic ovaries[7]
- Obesity and central fat distribution[7]
- Hirsutism - male pattern of hair growth primarily on the face, back, chest, lower abdomen, and inner thighs [7]
- Virilization - development of male features including balding of the frontal portion of the scalp, voice deepening, atrophy of breast tissue, increased muscle mass, and clitoromegaly[7]
- Anovulation - failure of the ovaries to release an oocyte[7]
- Amenorrhea - the absence of a menstrual period in women of childbearing age[7]
- Oligomenorrhea - the presence of menstrual cycles greater than 35 days apart[7]
- Dysfunctional uterine bleeding[8]
- Acne related to hyperandrogenism[9]
- Infertility; recurrent first trimester miscarriages[10] PCOS can make it harder to get pregnant and increase the risk for pregnancy complications and miscarriage. Weight loss and other treatments can improve the chances of having a healthy pregnancy.
- Pronounced psychological and psychosocial problems that affect health-related quality of life (HRQL)[11]
- Obstructive Sleep Apnea
Diagnosis[edit | edit source]
There is no single specific test that can be used to accurately diagnose Polycystic Ovarian Syndrome. Rather a comprehensive examination needs to be carried out by a clinician which involves a detailed history, physical examination and investigative procedures. Clinicians should focus on taking a detailed menstrual history for any irregularities, any significant change in the patient's weight and physical appearance (acne, alopecia, terminal hair, acanthuses nigricans, skin tags)[12]. Investigations that could help arrive at a definite diagnosis include:
- Ultrasound - An ultrasonic test allows visualization of any cysts which may be present on the ovaries or if there is any enlargement of one or both ovaries. A transvaginal ultrasound which involves inserting the probe into the vagina is usually done for women who have been sexually active. For women who are not sexually active, an abdominal ultrasound is opted for where the ovaries are viewed from outside the abdominal wall however, a clearer picture is obtained transvaginally compared to a transabdominal ultrasound[13].
- Hormonal Blood Tests[13]
- Hyperandrogenism - Testing for androgen levels and free androgen index (FAI) is best for diagnosis hyperandrogenism which is a key finding in women with PCOS.
- Tests to detect female hormonal levels - Estradiol, Follicle Stimulating Hormone, Luteinizing Hormone levels.
- Tests to exclude other conditions which could present as Polycystic Ovarian Syndrome PCOS - Thyroid Stimulating Hormone, Prolactin, Adrenal hormones.
Criteria for Diagnosis[edit | edit source]
A conclusive diagnosis for PCOS can be made if at least 2 out of 3 of the following is found criteria are met[13]:
- Polycystic ovaries - 12 or more follicles are seen on one ovary or the size of one or both ovaries have enlarged.
- Hyperandrogenism - high levels of androgenous hormones or male pattern of hair growth.
- Menstrual Abnormalities - lack of menses or menstrual cycle irregularities or anovulation.
Treatment[edit | edit source]
Treatment for PCOS usually starts with lifestyle change recommendations; Weight loss - Cornerstone in controlling all derangements seen in PCOS[9]; Regular exercise (30min/day) lowering insulin levels - walking/jogging[9]; Low-carbohydrate diets have been trialed but studies have shown no difference in outcomes.[1]
Medical treatments for menstrual abnormalities, hirsutism, and acne are:
- Hormonal contraceptive, either oral contraceptive, patch, or vaginal rings.
- Metformin and anti-androgens may also help.[1]
- The combined treatment with metformin and progesterone-based oral contraceptives could reverse the early stage endometrial cancer into normal endometria along with improvement of insulin resistance in women with PCOS.[14]
Physical Therapy Management[edit | edit source]
A physiotherapist and dietician are highly recommended as these are considered first-line treatments.
Exercise training has shown great improvement in 50% of the women diagnosed with Polycystic Ovarian Syndrome PCOS, by targeting menstrual irregularities and promoting ovulation. Weight reduction is an important component of the physical therapy program since weight reduction improves glucose intolerance which in turn could resolve the reproductive and metabolic derangements often associated with PCOS. Weight loss may also reduce the pulse amplitude of luteinizing hormone thus reducing androgen production[2].
Physical therapists should also be aware of the clinical presentation of Polycystic Ovarian Syndrome PCOS. Women with PCOS may experience low back pain, sacral pain, and lower quadrant abdominal pain. However, a thorough patient history can provide information about a gynecologic/metabolic connection. The concern of the possible presence of Polycystic Ovarian Syndrome PCOS requires immediate referral to a physician.[5]
In treating patients with a past medical history of Polycystic Ovarian Syndrome PCOS for a non-related condition, be aware of related medical concerns that may affect the patient's ability to participate in activities including glucose intolerance and insulin resistance.[5]
Side effects of medications need to also be taken into account. For example, the side effects of clomiphene citrate, an ovulation inducer, include insomnia, nausea/vomiting, blurry vision, and frequent urination.[5]
Therapeutic Exercise / Activity / Modalities for PCOS[edit | edit source]
Physical therapy interventions seek to decrease the main symptoms of polycystic ovarian syndrome (PCOS) by addressing hormonal imbalances, obesity, and seeking to improve the quality of life for these women. High Intensity Interval Training, Cardiovascular training, and Resistance Training help increase heart rate, which have a positive impact on overall physiological effects on cardiovascular health and hormone regulation, including the androgen hormones and insulin sensitivity that lead to symptoms of PCOS. Physical therapy modalities can also aid in the reduction of experienced symptoms in PCOS.
High Intensity Interval Training (HIIT)[edit | edit source]
High Intensity Interval Training (HIIT) training is a popular style of fitness training that consists of a series of exercises being performed at a fast paced to elicit both an aerobic and anaerobic response. Anaerobic HIIT is a highly desirable workout because it engages all muscle fibers, the fast twitch as well as the slow twitch. This makes anaerobic HIIT good for a complete training effect (Anaerobic Exercise). The benefits of H.I.I.T training for PCOS include improvements of glycemic control,[15] “improvements in aerobic capacity, insulin sensitivity, menstrual regulation and hormonal profiles."[16] HIIT has also been shown to decrease stress, anxiety, and depression level.
A H.I.I.T workout for PCOS would include:
-Warm Up such as walking, jogging, biking to a 50-65% of heart rate’s max. [17]
- 2-3 rounds of 2 minutes of exercises performed at a high speed with low to moderate weight varying in difficulty and heart rate max as low as 65%-90%
Example:
Round 1: Squats and shoulder presses for 2 minutes
Round 2: Mountain climbers and high knees for 2 minutes
Round 3: Side lunges and triceps dips for 2 minutes
-Cool down such as walking, active stretching to lower heart rate max
The kind of exercises can vary depending on the individual's abilities and accessibility to equipment, but the method is consistent. To benefit from aerobic and anaerobic training simultaneously, exercises must be performed at a fast rate in a series of rounds while maintaining 50-90% of the participant’s heart rate max depending on the round of H.I.I.T. To understand target heart rate max, you must first calculate heart rate max prior to training, by subtracting the participants age from 220 and multiplying that value by the percentage you aim to target. During training the participant can use a watch that monitors their heart rate to make sure they are meeting the target heart rate for the corresponding stage in H.I.I.T or they may count their pulse for a minute immediately after exercise and determine if their intensity such as performed speed or resistance needs to be modified.
Aerobic Training[edit | edit source]
Aerobic training can include running, walking, and bike riding. There is no specific method that is superior to the other, each type of aerobic training can help to alleviate the severity of PCOS symptoms. Performing an aerobic activity that will increase your heart rate to sixty to seventy percent can chow improvements in autonomic and inflammatory functions.[18] PCOS can impact each woman differently, and due to this weight and level of perceived intensity will be specific to the individual. The intensity of aerobic training will depend on personal max heart rate. The target heart rate of sixty to seventy percent can be calculated by taking your age and multiplying it by .07 or .06 and then subtracting 220. The sum of this calculation will be the target heart rate. A great way to monitor, to make sure the cardiovascular training is sufficiently reaching the target heart rate that benefits women with PCOS, is to track heart rate manually or with watch devices that report heart rate in real time.
Resistance Training[edit | edit source]
Resistance training (RT) is the “increase in muscle strength by making muscles work against a weight or force”[19] and is another effective way to help improve and decrease PCOS symptoms. RT has been shown to reduce testosterone levels, waist circumference and increase functional capacity.[20] Additionally, it has been found that RT can also help improve “menstrual cyclicity, Ferriman-Gallwey scores [used to score hirsutism], testosterone, DHEA-S, sex hormone binding globulin levels and free androgen index scores”.[21] All these hormones are part of the pathophysiology of PCOS. By improving the hormonal level, RT is helping to address some of the hormonal imbalance caused by PCOS and can improve symptoms and overall health.
A general recommendation for resistance training for women with PCOS includes training 2-3 days per week for 30-60 minutes per session. “Loading for strength training should be between 8 and 15 repetitions with a 1RM percentage between 60% and 85%.”[22] Shrestha et al., n.d. Physiopedia article[19] discusses how you can find your 1RM. Exercises can include dumbbells, barbells, thera-bands, weighted pulley machines, and body weight. Full-body exercises can be squats, pushups, and burpees, while isolated body parts exercises include biceps, triceps, or hamstring curls and single leg raises. Depending on the resources available, a variety of RT exercises can be done. A physical therapist can help assess and evaluate the specific needs of each individual and can create a treatment plan that involves resistance training to help manage PCOS.
Modalities[edit | edit source]
Using patterns in physical therapy can help patients by relieving pain in specific areas. The "Core Four" muscles of the pelvic floor—the diaphragm, multifidus, transverse abdominis, and pelvic floor muscles—painfully contract in PCOS patients. Given their experience with low back pain and pelvic discomfort, women with PCOS frequently experience low back pain and primary dysmenorrhea as a common symptom.
Transcutaneous electrical nerve stimulation (TENS)[edit | edit source]
Transcutaneous electrical nerve stimulation (TENS) is a treatment that utilizes low-voltage electric current to relieve lower back pain and menstrual cramps (primary dysmenorrhea). Women with PCOS often complain of pelvic or lower abdominal discomfort related to menstruation and low back pain. With TENS, electrical pulses can reduce pain and provide short-term pain relief. TENS is essential for PCOS because it alleviates chronic pain associated with the pelvic floor muscles. If the patient experiences severe pain during menstruation, the treatment should last 20-30 minutes [23].
Hot pack/Heat Therapy[edit | edit source]
In areas where women experience PCOS-related discomfort, hot packs, and heat treatments can relax tense muscles, increase blood flow, and alleviate pain. Heat exposure reduces inflammation, which controls PCOS flare-ups. Most HT participants had improved menstrual function and substantially lower serum testosterone levels. The cumulative stress of repeated heat exposure is a potent stimulant that affects both metabolic and ovarian function [24]. Heat therapy also significantly improved PCOS clinical markers. After heat treatment, the clinical indicators of PCOS changed significantly. Heat use resulted in lower serum testosterone and enhanced menstrual function; this demonstrates that repeated exposure to heat is a powerful stimulus that affects both ovarian and metabolic function [24].
Electroacupuncture/Acupuncture[edit | edit source]
Electroacupuncture is a technique for treating conditions by putting an electrical current through a needle. Acupuncture can help people lose weight; this may be a particularly appealing option for those with PCOS because it may also help with other symptoms such as stress, irregular menstrual cycles, and infertility[25]. Participants' health conditions changed with the PCOS symptoms they were experiencing. Acupuncture therapy improvements were linked to variables such as regular menstrual cycles, slower hair growth, improved moods, and less acne [26]. Treatment with acupuncture did have some impact on the PCOS symptoms. More tangible outcomes, such as more regular ovulation and pregnancy, were experienced by some of the women [26].
References[edit | edit source]
- ↑ 1.0 1.1 1.2 Leon LI, Anastasopoulou C, Mayrin JV. Polycystic Ovarian Disease. InStatPearls [Internet] 2021 Jul 21. StatPearls Publishing. Available:https://www.ncbi.nlm.nih.gov/books/NBK459251/ (accessed 21.8.2022)
- ↑ 2.0 2.1 Shetty D, Chandrasekaran B, Singh AW, Oliverraj J. Exercise in polycystic ovarian syndrome: An evidence-based review. Saudi Journal of Sports Medicine. 2017 Sep 1;17(3):123.
- ↑ Radiopedia PCOS Available: https://radiopaedia.org/articles/polycystic-ovarian-syndrome-1 (accessed 21.8.22)
- ↑ Harrison CL, Lombard CB, Moran LJ, Teede HJ. Exercise therapy in polycystic ovary syndrome: a systematic review. Human Reproduction Update. 2010 Sep 10;17(2):171-83.
- ↑ 5.0 5.1 5.2 5.3 5.4 5.5 Goodman CC, Fuller KS, editors. Pathology: implications for the physical therapist. 3rd ed. St Louis: Saunders Elsevier, 2009.
- ↑ Daniilidis A, Dina K. Long term health consequesnces of polycystic ovarian syndrome: a review analysis. Hippokratia 2009; 13:90-92.
- ↑ 7.0 7.1 7.2 7.3 7.4 7.5 7.6 7.7 Callahan TL, Caughey AB, editors. Blueprints: obstetrics & gynecology. 5th ed. Baltimore: Lippincott Williams & Wilkins, 2009.
- ↑ Futterweit W, Diamanti-Kandarakis E, Azziz R. Clinical features of the polycystic ovary syndrome. InAndrogen Excess Disorders in Women 2006 (pp. 155-167). Humana Press.
- ↑ 9.0 9.1 9.2 Merck manual of medical information. 2nd ed. New York: Merck & Co., Inc, 2003. p 1234-35.
- ↑ Sheehan MT. Polycystic ovarian syndrome: diagnosis & management. Clinical Medicine & Research 2004;2:13-27.
- ↑ Elsenbruch S, Hahn S, Kowalsky D, Offner AH, Schedlowski M, Mann K, Janssen OE. Quality of life, psychosocial well-being, and sexual satisfaction in women with polycystic ovary syndrome. J Clin Endocrinol Metab. 2003 Dec;88(12):5801-7. doi: 10.1210/jc.2003-030562. PMID: 14671172.
- ↑ Williams T, Mortada R, Porter S. Diagnosis and Treatment of Polycystic Ovary Syndrome. American family physician. 2016 Jul 15;94(2).
- ↑ 13.0 13.1 13.2 Jean Hailes: How is PCOS diagnosed? Available from: https://jeanhailes.org.au/health-a-z/pcos/how-is-pcos-diagnosed [Accessed 30th June 2018]
- ↑ Shao R, Li X, Billig H. Promising clinical practices of metformin in women with PCOS and early-stage endometrial cancer. BBA Clin. 2014 Jul 25;2:7-9. doi: 10.1016/j.bbacli.2014.07.001. PMID: 26674650; PMCID: PMC4633941.
- ↑ Hiam, D., Patten, R., Gibson-Helm, M., Moreno-Asso, A., McIlvenna, L., Levinger, I., ... & Stepto, N. (2019). The effectiveness of high intensity intermittent training on metabolic, reproductive and mental health in women with polycystic ovary syndrome: study protocol for the iHIT-randomised controlled trial. Trials, 20(1), 1-9.
- ↑ Patten RK, McIlvenna LC, Moreno-Asso A, Hiam D, Stepto NK, Rosenbaum S, et al. Efficacy of high-intensity interval training for improving mental health and health-related quality of life in women with polycystic ovary syndrome. Scientific Reports. 2023 Feb 21;13(1).
- ↑ Philbois SV, Ribeiro VB, Tank J, Maria dos Reis R, Gerlach DA, Souza HCD. Cardiovascular Autonomic Modulation Differences Between Moderate-Intensity Continous and High-Intensity Interval Aerobic Training in Women with PCOS: A Randomized Trial. Frontiers in Endocrinology. 2022 Nov 25;1024844(13):1-12
- ↑ Giallauria F, Palomba S, Maresca L, Vuolo L, Tafuri D, Lombardi G, et al. Exercise training improves autonomic function and inflammatory pattern in women with polycystic ovary syndrome (PCOS). Clinical Endocrinology. 2008 Nov;69(5):792–8.
- ↑ 19.0 19.1 Shrestha M. Strength Training [Internet]. Physiopedia. Available from: https://www.physio-pedia.com/Strength_Training
- ↑ Ramos F, Lara L, Kogure G, Silva R, Ferriani R, Silva de Sá M, et al. Quality of Life in Women with Polycystic Ovary Syndrome after a Program of Resistance Exercise Training. Revista Brasileira de Ginecologia e Obstetrícia / RBGO Gynecology and Obstetrics. 2016 Jul 29;38(07):340–7.
- ↑ Bansal A, Sethi J, Parasher RK. Role of structured exercise programs in polycystic ovary syndrome: a systematic review. Physical Therapy Reviews. 2023 Jan 5;1–11.
- ↑ Cormier T. Resistance Training for Polycystic Ovary Syndrome. ACSM’S Health & Fitness Journal. 2022 Mar;26(2):61–2.
- ↑ Elboim-Gabyzon M, Kalichman L. Transcutaneous Electrical Nerve Stimulation (TENS) for Primary Dysmenorrhea: An Overview. International Journal of Women’s Health. 2020 Jan;Volume 12:1–10.
- ↑ 24.0 24.1 Ely BR, Clayton ZS, McCurdy CE, Pfeiffer J, Needham KW, Comrada LN, et al. Heat therapy improves glucose tolerance and adipose tissue insulin signaling in polycystic ovary syndrome. American Journal of Physiology-Endocrinology and Metabolism. 2019 Jul 1;317(1):E172–82.
- ↑ Yang J, Chon TY, Bauer BA. Use of Acupuncture in Overweight/Obese Women with Polycystic Ovary Syndrome. Medical Acupuncture. 2019 Oct 1;31(5):267–8.:
- ↑ 26.0 26.1 Billhult A, Stener-Victorin E. Acupuncture with manual and low frequency electrical stimulation as experienced by women with polycystic ovary syndrome: a qualitative study. BMC Complementary and Alternative Medicine. 2012 Apr 3;12(1).