Physiotherapy Treatment Approaches for Individuals with Cerebral Palsy
Original Editor - Naomi O'Reilly
Top Contributors - Naomi O'Reilly, Kim Jackson, Vidya Acharya, Simisola Ajeyalemi, Tarina van der Stockt, WikiSysop, Amanda Ager, Jess Bell, Shreya Pavaskar, Cindy John-Chu, Olajumoke Ogunleye and 127.0.0.1
Introduction[edit | edit source]
Cerebral palsy (CP) is one of the most common developmental disabilities. CP is a bracket term given for a set of neurological disorders characterized by disorders of movement and posture causing activity limitation attributed to a static disturbance in the developing brain, often accompanied by associated impairments and secondary health conditions. CP is not a single pathological entity and encompasses disorders in various motor functions including but not limited to body movement, muscle control, muscle coordination, muscle tone, reflex, fine motor skills, gross motor skills, oral motor functioning, posture, and balance. [1]
As highlighted by Gunel (2011) Pediatric Rehabilitation requires a Multidisciplianary (MDT) Approach in order to promote the independence of the child with an impairment, both functionally and psychologically and increase the quality of life of both the child and their family. Physiotherapists, viewed as the 'movement expert', play a key role within this MDT. The main aim of Physiotherapy, as identified by Gunel (2011), is to support the child with Cerebral Palsy to achieve their potential for physical independence and fitness levels within their community, by minimizing the effect of their physical impairments, and to improve the quality of life of the child and their family who have a major role to play in the process. [2]
Physiotherapy focuses on function, movement, and optimal use of the child's potential and uses physical approaches to promote, maintain and restore physical, psychological and social well-being within all environments of the child including home, school, recreation, and community environments. [2]
Gross motor skills, functional mobility in the management for the motor deficits, positioning, sitting, transition from sitting to standing, walking with or without assistive devices and orthoses, wheelchair use and transfers, are all areas that the physiotherapist works on using a wide range of physiotherapeutic approaches to influence functional ability of the child, which we will review. [2] [3]
Treatment Approaches[edit | edit source]
According to Patel (2005) a wide range of therapeutic interventions have been used in the treatment and management of children with cerebral palsy. They show that there is evidence to support the use and effectiveness of neuromuscular electrical stimulation, while evidence in support of the effectiveness of the neurodevelopmental treatment is equivocal at best. The effectiveness of many other interventions, including include: sensory integration, body-weight support treadmill training, conductive education, constraint-induced movement therapy, hyperbaric oxygen therapy used in the treatment of cerebral palsy have not been clearly established based on well-controlled trials. We provides an overview of salient aspects of popular approaches and interventions used in the management of children with Cerebral Palsy. [3] [4]
Antilla (2008) identifies a wide range of choices and availability of various techniques which may vary both between therapists and from country to country. Table 1.7 below lists many of the most common physiotherapy and physiotherapy-related approaches utilized in the management of Cerebral Palsy during the past few decades. [5]
Neurodevelopmental Treatment (NDT) [edit | edit source]
One of the more popular approaches utilised in the management of cerebral palsy, the NDT Approach also know as Bobath Approach, was developed in the 1940's by Berta and Karl Bobath, based on their personal observations working with children with cerebral palsy. The basis of this approach is that motor abnormalities seen in children with Cerebral Palsy are due to atypical development in relation to postural control and reflexes because of the underlying dysfunction of the central nervous system. This approach aims to facilitate typical motor development and function and to prevent development of secondary impairments due to muscle contractures, joint and limb deformities. Although the effectiveness of NDT in Cerebral Palsy has been questioned by some published reports, there are some studies suggesting its effectiveness.[3]
Constraint-Induced Movement Therapy (CIMT)[edit | edit source]
Constraint-induced Movement therapy is used predominantly in the individual with Hemiplegic Cerebral Palsy to improve the use of the affected upper limb. The stronger or non-impaired upper limb is immobilized for a variable duration in order to Force Use of the impaired upper limb over time [3]. Antilla et al (2008) [4] identified one high and one lower-quality trials which measured both body functions and structures, and activity and participation outcomes through use of CIMT. Use of a cast with CIMT showed positive effects in the amount and quality of functional hand use in the impaired limb and new emerging behaviour as compared to the no-therapy group, but no effects were found on QUEST. Use of sling during CIMT also had positive effects on functional hand use on the impaired upper limb, time to complete tasks, and speed and dexterity, but no effects on sensibility, handgrip force, or spasticity. Thus Antilla et al (2005) found there is moderate evidence for the effectiveness of CIMT therapy on functional hand use in the impaired upper limb [4]. According to Patel (2005) the efficacy of this approach has not been established, in particular in relation to the adverse effects of prolonged immobilization of the normally developing upper limb [3].
Patterning[edit | edit source]
The concept of patterning is based on theories developed during the 1950's and 1960's by Fay, Delacato, and Doman. Patterning is based on the principle that typical development of the infant and child progresses through a well-established, pre-determined sequence; with failure to typically complete one stage of development causing inhibition or impairment in the development of subsequent stages. Based on this principal they suggested that in children with Cerebral Palsy typical motor development can be facilitated by passively repeating and putting the child through the sequential steps of typical development, a process called patterning. Parents and other care givers are taught to carry out this patterning process at home but the approach is hugely labour intensive and time consuming as it requires multiple sessions every day. Although Patterning has been utilised for many years its use is now certainly controversial and the effectiveness has not been established. It is a very passive therapy, with little opportunity to encourage the child in their active involvement and its use in children with Cerebral Palsy is not recommended. [3]
Therapeutic Interventions[edit | edit source]
Passive Stretching[edit | edit source]
It is a manual application for spastic muscles to relieve soft tissue tightness. Manual stretching may increase range of movements, reduce spasticity, or improve walking efficiency in children with spasticity. [6] Stretch may be applied in a number of ways during neurological rehabilitation to achieve different effects. The types of stretching used include;
- Fast / Quick
- Prolonged
- Maintained
When we look at the use of a stretch for facilitation, we employ a fast/quick stretch. The fast/quick stretch produces a relatively short-lived contraction of the agonist's muscle and short-lived inhibition of the antagonist muscle which facilitates a muscle contraction. It achieves its effect via stimulation of the muscle spindle primary endings which results in reflex facilitation of the muscle via the monosynaptic reflex arc.
The presence of increased tone can ultimately lead to joint contracture and changes in muscle length. When we look at the use of stretch to normalise tone and maintain soft tissue length we employ a slow, prolonged stretch to maintain or prevent loss of range of motion. While the effects are not entirely clear the prolonged stretch produces inhibition of muscle responses which may help in reducing hypertonus, e.g. Bobath's neuro-developmental technique, inhibitory splinting and casting technique. It appears to have an influence on both the neural components of muscle, via the Golgi Tendon Organs and Muscle Spindles, and the structural components in the long term, via the number and length of sarcomeres.
Muscle Immobilised Shortened Position = Loss of Sarcomeres and Increased Stiffness related to increase in connective tissue
Muscle Immobilised Lengthened Position = Increase Sarcomeres
Studies in Mice show that a stretch of 30 mins daily will prevent the loss of sarcomeres in the connective tissue of an immobilised muscle, although the timescale in humans may not relate directly. The study by Johannes M N Enslin et al. discusses the current literature on possible stretching interventions in children with Cerebral Palsy and highlights additional research that has the potential to improve non-invasive treatment outcomes[7].
Passive stretching may be achieved through a number of methods which include;
Manual Stretching [edit | edit source]
Prolonged manual stretch may be applied manually, using the effect of body weight and gravity or mechanically, using machine or splints. Stretch should provide sufficient force to overcome hypertonicity and passively lengthen the muscle. Unlikely to provide sufficient stretch to cause change in a joint that already has contracture.
Weight Bearing[edit | edit source]
Weight bearing has been reported to reduce contracture in the lower limb through use of Tilt-tables, and standing frames through a prolonged stretch. Angles are key to ensure the knees remain extend during the prolonged stretch as the force exerted on the knee can be quite high. Some research also challenges the assumption of the benefits of prolonged standing.
Splinting[edit | edit source]
Splints and casts are external devices “Splints and casts are external devices designed to apply, distribute or remove forces to or from the body in a controlled manner to perform one or both basic functions of control of body motion and alteration or prevention in the shape of body tissue.” Splinting can be used to produce low-force, long duration stretching although there is a dearth of evidence to support this. A wide range of splint have been used to influence swelling ,resting posture, spasticity, active and passive ROM. A systematic review suggested that Lower Limb Serial Casting improved ankle dorsiflexion passive range of motion, reduced hypertonocity and improved gait in children with Cerebral Palsy[8].
Blackmore (2006) A Systematic Review of the effects of casting on Equinus in Children with Cerebral Palsy An AACPDM Evidence Report
Serial Casting [edit | edit source]
Serial casting is a common technique that is used and most effective in managing spasticity related contracture. Serial casting is a specialized technique to provide an increased range of joint motion. The process involves a joint or joints that are tight, which are immobilized with a semi-rigid, well-padded cast. Serial casting involves repeated applications of casts, typically every one to two weeks as range of motion is restored.
S, Jain et al (2008). Effect of serial casting in spastic cerebral palsy.. Indian J Pediatr. 2008 Oct;75(10):997-1002. doi: 10.1007/s12098- 008-0100-z. Epub 2008 Jun 23.
The duration of the stretch to reduce both spasticity and to prevent contracture are not yet clear from the research and require further research to determine the most appropriate technique and duration to produce the required effect.
Static Weight-bearing Exercises[edit | edit source]
Stimulation of antigravity muscle strength, prevention of hip dislocation, reduction in spasticity and improvements in bone mineral density, self-confidence and motor function have all been achieved through the use of Static Weight-Bearing exercises such as Tilt-Table and Standing Frame. [6]
Muscle Strengthening Exercises[edit | edit source]
It aims to increase the power of weak antagonist muscles and of the corresponding spastic agonists and to provide the functional benefits of strengthening in children with CP. [6]
Functional Exercises[edit | edit source]
Training related to specific functional activities combining aerobic and anaerobic capacity and strength training in ambulatory children, has been shown to significantly improve overall physical fitness, the intensity of activities, and quality of life. Training programs on static bicycles or treadmill have been shown to be beneficial for gait and gross motor development but have not shown to have any impact on spasticity or abnormal movement patterns. [6] A study suggests the application of plyometric exercises to the physical rehabilitation programs of children with unilateral CP could achieve more significant improvement in muscle strength and walking performance[9].
Body Weight Supported Treadmill Training[edit | edit source]
Stepping movements from Reflex Stepping Reactions are normally present in newborns and infants, before the infant starts to bear weight, stand and walk. Body Weight Supported Treadmill Training, is achieved through supporting the child in a harness on the treadmill in an upright posture limiting overall weight bearing, on a slow moving treadmill, eliciting the stepping movements. Treadmill training, thus allows the development of stepping movements needed for ambulation. Studies using 3-4 sessions per week lasting for 3-4 months have shown improvement in lower extremity movements and gait patterns in children with cerebral palsy. [3]
Electrical Stimulation[edit | edit source]
The goal of the electrical stimulation is to increase muscle strength and motor function. Electrical stimulation is provided by Transcutaneous Electrical Nerve Stimulation (TENS) Unit which is portable, non-invasive and can be used in the home-setting by parents or the patient. Neuromuscular Electrical Stimulation (NMES) involves application of transcutaneous electrical current that results in muscle contraction. NMES has been postulated to increase muscle strength by increasing the cross-sectional area of the muscle and by increased recruitment of type 2 muscle fibers. Functional Electrical Stimulation (FES) refers to the application of electrical stimulation during a given task or activity when a specific muscle is expected to be contracting. Patel (2005) has shown there is some evidence to support the use and effectiveness of NMES in children with Cerebral Palsy but found that many of the studies are limited by confounding variables including concomitant use of other therapies, wide variation in methods of application, heterogeneity of subjects, difficulty in measuring functional outcomes and lack of control subjects [3]. Mintaze (2009) proposes that neuromuscular and threshold electrical stimulation as a modality in Cerebral Palsy is used for strengthening the quadriceps muscles in ambulatory diplegic children with Cerebral Palsy, who have difficulty with specific resistive strength training [6].
Hippotherapy[edit | edit source]
Gross Motor Function including Muscle tone, Range of Movement, Balance, Coordination and Postural Control in children with CP have been shown to improve with Hippotherapy - Therapeutic horse-back riding which may reduce the degree of motor disability. Many none physical benefits may also be developed through enjoyment and providing a setting for increased social interaction, cognitive and psychosocial development [3]. Sharan et al (2005) have noted satisfactory results with Hippotherapy in Bangalore, especially in post-surgical rehabilitation [10]. There is limited evidence available with two lower-quality trials on saddle riding on a horse found no between-group differences in muscle symmetry or in any of the seven different outcome measures, except on a sub-item of grasping. [4]
Sensory Integration Training[edit | edit source]
Sensory integration therapy is based on the idea that some kids experience “sensory overload” and are oversensitive to certain types of stimulation. When children have sensory overload, their brains have trouble processing or filtering many sensations at once. Meanwhile, other children are undersensitive to some kinds of stimulation. Children who are undersensitive do not process sensory messages quickly or efficiently. These children may seem disconnected from their environment. In either case, children with sensory integration issues struggle to organize, understand, and respond to the information they take in from their surroundings. Sensory integration therapy exposes children to sensory stimulation in a structured, repetitive manner. The theory behind this treatment approach is that, over time, the brain will adapt and allow them to process and react to sensations more efficiently. In this concept, difficulties in planning and organizing behavior are attributed to problems of processing sensory inputs within the CNS, including vestibular, proprioceptive, tactile, visual, and auditory. Children with sensory integration dysfunction frequently use different sensory combination strategies. Treatment focuses on integration of neurological processing by facilitating the individual to process the type, quality, and intensity of sensation. [11]
Task-oriented approach[edit | edit source]
This treatment is based on the requirements of the child. Today the child is given the possibility to be more of an active problem solver (instead of, as previously, a passive recipient of treatment) in the context of the day-to-day environment. The aim of this therapy for children with CP, as for most children with developmental disabilities, is to facilitate the child’s participation in everyday life situations, e.g., to communicate with parents, siblings, and peers; to move from one place to another; to dress and undress; to eat; and to play. The choice of goals for therapy is dependent on many factors: the child’s likings and the family’s preferences, the society and environment in which the family lives, and the child’s degree of disability. Thus, it is important to integrate principles of motor learning in the treatment concept and adapt the principles to the prerequisites of each specific child. The set goals should be specific, measurable, attainable, relevant, and timed (SMART).[11]
Conductive Exercise[edit | edit source]
Conductive education (CE) is a combined educational and task-oriented approach for children with CP. Specially trained ‘conductors’ give education to homogeneous groups of children with motor disorders. This approach has its origins in learning theory. The conductor who is trained in all aspects of motor and cognitive development structures the activities, especially the self-care activities.. The emphasis of intervention is on independence in attaining goals rather than on quality of movement. [11]
Bimanual Training[edit | edit source]
Bimanual training (BIT) provides bimanual training activities, which focus on improving the coordination of both arms using structured tasks in bimanual play and functional activities with intensive practice. Recently has an intensive bimanual training program, the hand-arm bimanual intensive training (HABIT) been published to substantiate its effectiveness. This approach is based on motor learning theory (practice specificity, types of practice, and feedback), neuroplasticity (i.e., the potential of the brain to change by repetition, increasing movement complexity, motivation, and reward), and focuses on the equal use of both arms in bimanual tasks. Intensive BIT (e.g., HABIT), was developed with recognition that increased functional independence in the child’s environment requires the combined use of both hands. It also focuses on improving coordination of the two hands using structured task practice embedded in bimanual play and functional activities. Hand-arm bimanual intensive therapy including lower extremities (HABIT-ILE) combines upper and lower bilateral extremity training. Frequently used bilateral lower extremity tasks are ball sitting, standing, balance board standing, virtual reality (wii-fit, kinect), walking/running, jumping, cycling, and making scooter. Bimanual activities that require trunk and LE postural adaptations are performed at a table of appropriate height (50% of the time) on unstable supports: sitting on fitness balls or standing on balance boards. Furthermore, 30% of the time is devoted to activities of daily living where standing and/or walking is required (dressing, brushing teeth, doing one’s hair, transporting objects such as a tray, and household chores such as sweeping and washing dishes). Finally, the remaining time (20%) is spent in gross motor physical activities/play, such as bowling, ball playing, jumping rope, street hockey, use of wii-fit, balance bike (without pedals), scooter use, and wall climbing. These are performed in standing, walking, and running (or jumping) with the LE and simultaneously involving bimanual coordination. These activities are graded toward more demanding tasks for the LE.[11]
Robot-assistive therapy[edit | edit source]
Robot-assisted therapy (RAT) is conducted using robotic devices that enable the patients to perform specific limb movements. The main interest in using robots is to allow the patients to achieve a large amount of movement in a limited time. Additionally, the attractive human-machine interface has the capacity to motivate the child to perform his or her therapy through playful games, such as car races, or to perform exercises that mimic ADLs. Moreover, robotic devices allow the patient to receive visual, auditory, or sensory feedbacks. A device specifically developed for the locomotion training is the Lokomat (Hocoma, CH), made of two active orthoses, a weight-bearing system and a treadmill. This robotic rehabilitation has been proposed to improve walking and physical fitness [11]
Virtual reality[edit | edit source]
Virtual reality has been defined as the use of interactive simulations created with computer to perform users in virtual environments that appear, sound, and feel similar to real-world objects and events. Virtual reality can improve the patient’s motivation and achievement in ADLs. Preliminary data suggest that this type of therapy also improves motor function in the upper and lower extremities that are caused by CP.
State of the Evidence[edit | edit source]
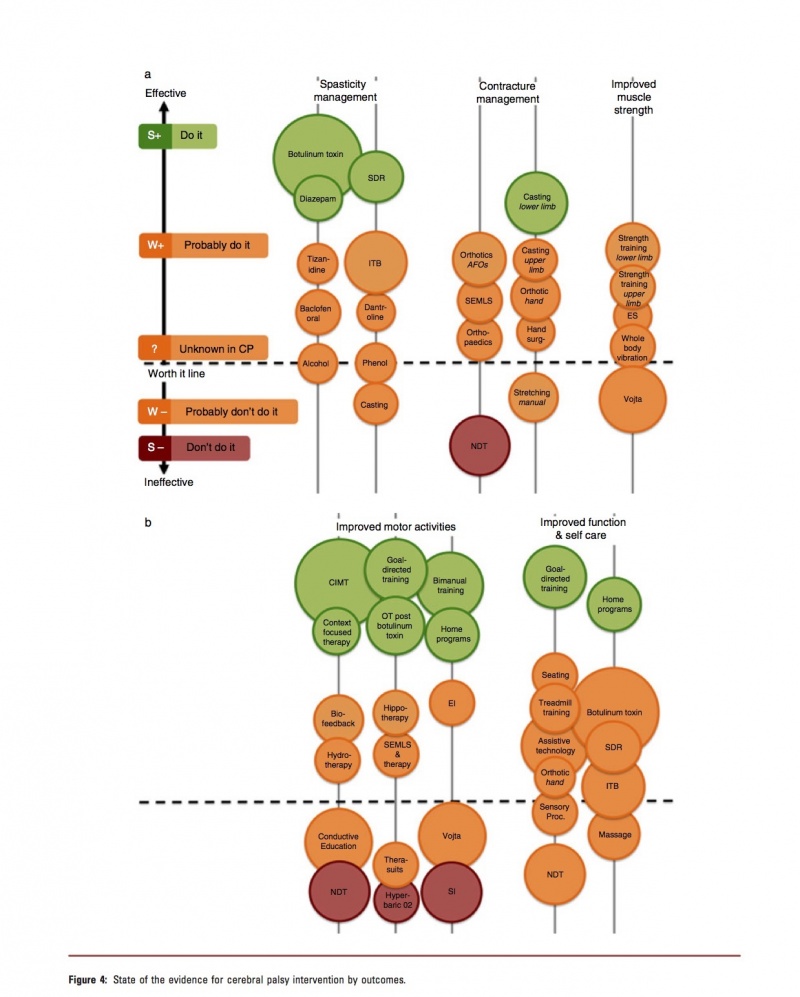
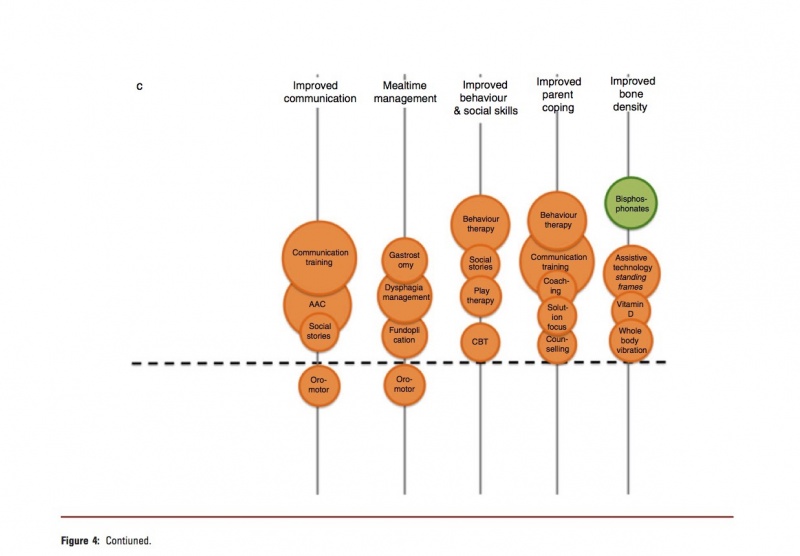
Novak et al. (2013) have developed a chart based on their Systamatic Review, which looked at the State of the Evidence in relation to Interventions for the management of children with Cerebral Palsy, to assist with comparative clinical decision-making amongst intervention options for the same desired outcome. They mapped the interventions using bubble charts, with the size of the circle correlated to the volume of published evidence. [12]
The circle size was calculated using;
- Number of published papers on the topic;
- Total score for the level of evidence (calculated by reverse coding of the Oxford Levels of Evidence, i.e. expert opinion=1, randomized controlled trial [RCT]=5).
- Location of the circle on the Y-Axis of the graph corresponds to the GRADE System Rating.
- Colour of the circle correlates to the Evidence Alert System (Fig. 4). [12]
You can review the article and more detail on their mechanism for rating the interventions at Novak I, Mcintyre S, Morgan C, Campbell L, Dark L, Morton N, Stumbles E, Wilson SA, Goldsmith S. A systematic review of interventions for children with cerebral palsy: state of the evidence. Developmental Medicine & Child Neurology. 2013 Oct 1;55(10):885-910.
References[edit | edit source]
- ↑ Das SP, Ganesh GS. Evidence-based approach to physical therapy in cerebral palsy. Indian journal of orthopaedics. 2019 Jan;53(1):20.
- ↑ 2.0 2.1 2.2 Günel MK. Physiotherapy for children with cerebral palsy. INTECH Open Access Publisher; 2011.
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 3.6 3.7 3.8 Patel DR. Therapeutic interventions in cerebral palsy. The Indian Journal of Pediatrics. 2005 Nov 1;72(11):979-83.
- ↑ 4.0 4.1 4.2 4.3 Anttila H, Autti-Rämö I, Suoranta J, Mäkelä M, Malmivaara A. Effectiveness of physical therapy interventions for children with cerebral palsy: a systematic review. BMC pediatrics. 2008 Apr 24;8(1):1.
- ↑ Anttila H. Evidence-based perspective on CP rehabilitation: Reviews on physiotherapy, physiotherapy-related motor-based interventions and orthotic devices.
- ↑ 6.0 6.1 6.2 6.3 6.4 Mintaze Kerem G. Rehabilitation of children with cerebral palsy from a physiotherapist’s perspective. Acta Orthop Traumatol Turc. 2009;34(2):173-80.
- ↑ Enslin J, Rohlwink UK, Figaji A. Management of Spasticity After Traumatic Brain Injury in Children. Frontiers in Neurology. 2020 Feb 21;11:126.
- ↑ Milne N, Miao M, Beattie E. The effects of serial casting on lower limb function for children with Cerebral Palsy: a systematic review with meta-analysis. BMC pediatrics. 2020 Dec;20(1):1-23.
- ↑ Elnaggar RK, Elbanna MF, Mahmoud WS, Alqahtani BA. Plyometric exercises: subsequent changes of weight-bearing symmetry, muscle strength and walking performance in children with unilateral cerebral palsy. J Musculoskelet Neuronal Interact. 2019 Dec 1;19(4):507-15.
- ↑ Sharan D. Recent advances in management of cerebral palsy. The Indian Journal of Pediatrics. 2005 Nov 1;72(11):969-73.
- ↑ 11.0 11.1 11.2 11.3 11.4 Balcı NÇ. Current rehabilitation methods for Cerebral Palsy. InCerebral Palsy-current steps 2016 Sep 21. IntechOpen.
- ↑ 12.0 12.1 12.2 12.3 Novak I, Mcintyre S, Morgan C, Campbell L, Dark L, Morton N, Stumbles E, Wilson SA, Goldsmith S. A systematic review of interventions for children with cerebral palsy: state of the evidence. Developmental Medicine & Child Neurology. 2013 Oct 1;55(10):885-910.