Introduction to Knee Ankle Foot Orthoses
Original Editors - Rhiannon Clement
Top Contributors - Special:Rhiannon Clement/Introduction to Knee Ankle Foot Orthoses
Introduction[edit | edit source]
Healing[edit | edit source]
- Wedge boot: Often used as conservative treatment or after surgery for Achilles tendon rupture to allow gradual stretching of the tendon as it heals. A heel wedge may also be used in patient's with fixed platar flexion deformity to increased base of support and improve balance.
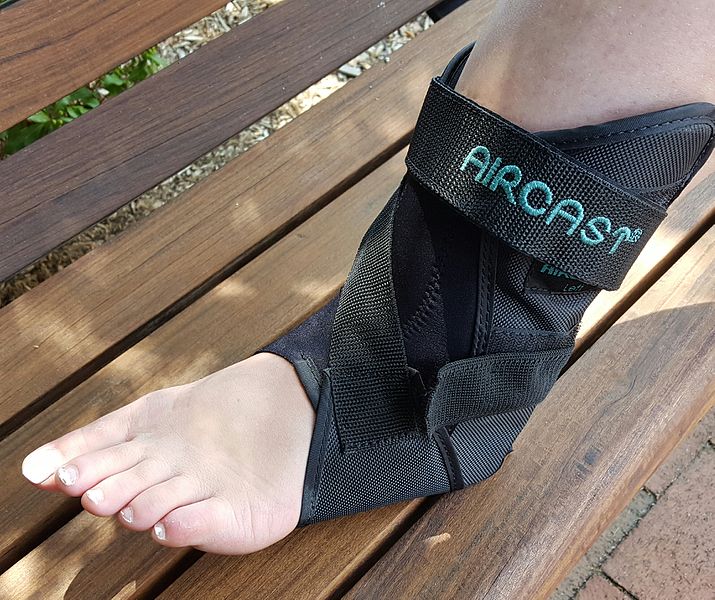
- Aircast boot: Often used after fracture injuries to support and reduce forces through the bone while healing. The air cells can be inflated around the foot and ankle, compressing the injury.
- Hinge-knee brace: Often used to protect knee surgery, such as meniscal repair[1].
- Splints; Patients with increased tone may require a resting splint to maintain optimal positioning of their lower limb and maintain a functional range in affected joints. Positioning and seated and supine positions are very important for these patients
Functional[edit | edit source]
- Ankle- Foot Orthosis (AFO): Correct alignment of the lower foot and ankle, which translates to the alignment of the shin, upper leg and pelvis. AFOs have an influence on both the swing and stance phase of gait[2]. Can also be used to reduce risk of trips and falls as a result of foot drop.
- Lateral support ankle brace: In patient's after ankle injuries, particularly to lateral ligaments, or neuromuscular disorders, a lateral ankle support may be needed. This brace has stiff lateral supports which will prevent excessive pronation or supination at the foot. This reduces the risk of further injury to lower limb structures, or injuries secondary to a fall.
- Functional Electrical Stimulation (FES): In patient's with central nervous system disorders / leisions, it may be possible, and safe, to use FES as a dynamic orthosis[3]. [4]Can be used on a number of muscle groups to simulate electrical impulses in peripheral nerves. It is often used to reduced impact of foot drop or knee hyperextension as a result of muscle weakness. There is also some evidence that it may contribute to strengthening of muscles[5]. In this way, FES may reduce the patient's risk of falls [6] and has been shown to improve quality of life scores [7]
- Foot Orthotics[8] [9]: Custom orthotics can improve foot alignment by affecting muscle activity [10]. Therefore, they improve efficieny in gait and balance, and minimise shock absorption through the lower limb, pelvis and spine[11]. These corrective devices are placed in an individual’s footwear similar to insoles.
A trained health practitioner will complete a detailed assessment of an individual’s gait and foot position in both a static and a dynamic state to identify asymmetries. This information will be combined with a precise imprint of the feet on a foam cast. This will be sent off to a lab where the orthotics will be fabricated and created. Some facilities will also use a gait scan machine in order to analyse where the majority of your weight is dispersed while you heel strike and push off during the gait cycle. The foot specialist may request that the lab add special features to the orthotics based on the patient’s area of pain, the wear patterns in the patient’s shoes and the skin changes on their feet.
Consideration: It seems logical to think that pain in the foot region links directly to dysfunction in the foot region and that orthotics are the intervention of choice. Unfortunately, it is not always that straightforward. For example, could hip weakness or lower back pain be causing disruption to the gait cycle and compensatory strategies that place increased load on foot stuctures? It is important to determine what is “driving” the pain in the foot and to direct treatment to these structures to see if insoles are needed. Also, can the intrinsic muscle of the foot be trained either alongside, or instead of the use of insole orthotics?
Conditions that may require a foot orthosis as an adjunct include:
• Plantar fasciitis
• Morton’s Neuroma
• Flat feet or high arches
• Knee, hip or low back pain and SIJ dysfunction
• Degenerative Disc Disease and scoliosis
• Osteoarthritis
• Patellofemoral pain syndrome
• Femoral acetabular impingment
• Iliotibial band friction syndrome
• Bursitis
• Chronic ankle sprains
• Piriformis syndrome
• Achilles, Patellar, hamstring or gluteal tendinopathy and Snapping Psoas
• Recurrent Calf Strains
Assessment[edit | edit source]
Use of outcome measures will determine the effectiveness of orthotics. This will be based on the patient's initial impairments, but may include:
- Neutral-0
- Passive range
- Active range
- Berg Balance Scale
- Tinetti
- Gait speed
- Timed up and go (TUG)
- Timed Unsupported Stand (TUSS)
- Functional gait assessment
Measurement [edit | edit source]
Add your content to this page here!
Fitting[edit | edit source]
Add your content to this page here!
Troubleshooting [edit | edit source]
Add your content to this page here!
References [edit | edit source]
see adding references tutorial.
- ↑ McDermott, Ian (2010) Meniscal Repair [available from:https://sportsortho.co.uk/treatment/meniscal-repair/] <accessed 29/09/20>
- ↑ NHS. Best Practice Statement: Use of Ankle-Foot Orthoses Following Stroke (2009) [online] <available from: http://www.healthcareimprovementscotland.org/previous_resources/best_practice_statement/use_of_ankle-foot_orthoses_fol.aspx?theme=mobile> [Accessed: 4/10/2020]
- ↑ NICE Functional Electrical Stimulation for Foot Drop of Central Neurological Origin (2009)[Online] <available from: https://www.nice.org.uk/guidance/ipg278> [Accessed 4/10/20]
- ↑ RCP Stroke guidelines , 2016
- ↑ Glinsky, J et al. Efficacy of Electrical Stimulation to increase muscle strength in people with neurological conditions: A systematic review. Physiotherapy Reseach Int. 12(3): 175-194 (2007)
- ↑ Esnouf, J.E. (2010) Impact Activities of Daily Living Using a Functional Stimulator (FES) device to Improve Dropped foot in people with Multiple Sclerosis, measured by the Canadian Occupational Performance Measure. Mult Scler. Sept: 1141-1147
- ↑ Juckes, F., Marceniuk, G., Seary, C., & Stevenson, V. (2019). A cohort study of functional electrical stimulation in people with multiple sclerosis demonstrating improvements in quality of life and cost-effectiveness. Clinical Rehabilitation, 33(7), 1163–1170.
- ↑ The Orthotic Group. Orthotic FAQ. Available from: http://www.theorthoticgroup.com/patientsite/OrthoticFAQ.aspx [last accessed 10/12/14]
- ↑ SBI Orthotic Laboratory. Orthotic FAQ. Available from: http://www.sbiorthoticlab.ca/faq_orthotic.html [last accessed 10/13/14].
- ↑ Roger, Collier. Orthotics work in mysterious ways. CMAJ-Canadian Medical Association Journal. March 8, 2011. Volume 183:p 416-417.
- ↑ Rebalance Sports Medicine. Custom Orthotics. Available from: http://www.rebalancetoronto.com/sports-medicine-services/orthotics-downtown-toronto/ [last accessed 10/13/14].