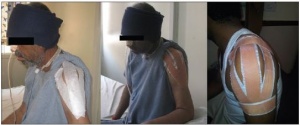
Hemiplegic Shoulder Subluxation
Introduction[edit | edit source]
Shoulder subluxation or Glenohumeral subluxation (GHS) is a common post-stroke complication affecting up to 80% of the stroke subjects[2].
The glenohumeral joint (GHJ) is multi-axial and has a wider range of motion than other joints. To achieve this range of motion, the glenohumeral joint sacrifices a more stable bone structure, which is compensated for by muscular stability. A change in normal muscular function that occurs after a stroke presents a potential risk for subluxation.
- During the initial period following a stroke, the hemiplegic arm is flaccid or hypotonic. The shoulder muscles cannot anchor the humeral head within the glenoid cavity, resulting in a high risk of shoulder subluxation.[3]
- During this period, the affected extremity should be adequately supported; the arm's weight may be enough to cause subluxation.
- Glenohumeral subluxation may also occur as a result of adopting incorrect sleeping postures, lack of support when the patient is in a vertical position or tension on the hemiplegic arm when the patient is being moved from one place to another.[4]
In the long term, GHS may lead to the following complications that may delay the recovery of upper extremity function [5][6]:
- Adhesive Capsulitis
- Reduced Proprioception
Epidemiology[edit | edit source]
The incidence of shoulder subluxation in patients following a stroke varies from 17%–81% and 73% occur in the acute stage[7]. Painful hemiplegic shoulder can occur within the first 2 weeks after the stroke; however, the condition typically presents after 2–3 months.[8][9] In a 10-month follow-up study, shoulder subluxation was shown to be further aggravated in 67% of patients over time.[6] The development of shoulder subluxation occurs mostly during the first 3 weeks of hemiplegia[10].
Pathomechanics and Risk factors[edit | edit source]
Studies have shown that the supraspinatus, and to a lesser extent, the posterior deltoid muscles, played a crucial role in maintaining glenohumeral alignment and preventing downward subluxation of the humerus.[11]
In 1959, Basmajian and Bazant offered a theory to explain the development of GHS:
- During the flaccid stage, the trunk tends to lean or shorten toward the hemiplegic side, which causes the scapula to descend from its normal horizontal level and contribute to the the subluxation of GHJ.
- The trapezius and the serratus anterior also become flaccid, causing the scapula to rotate downward.
- Without a normal tone, the rotator cuff can no longer maintain the integrity of the GHJ.
- During the spastic stage, the pectoralis major and minor, rhomboids, levator scapulae and latissimus dorsi can become hypertonic, further rotating the scapula downward, causing GHS.
On the contrary, other studies had not shown a relationship between scapular orientation and GHS.
Other factors contributing to subluxation include:
- Improper positioning,
- Prolonged downward pull of gravity and lack of counterforce by muscles
- Lack of support in the upright position,
- Pulling on the hemiplegic arm when the patient is transferred,[11]
- Severe loss of motor function and apparent absence of supraspinatus muscle contraction are potential risk factors for GHS. [11]
Assessment[edit | edit source]
Assessment methods of Shoulder subluxation:
Radiographic measurements (X-ray and ultrasound), considered a standard measurement, have been used in several studies to assess the effectiveness of therapy or development of GHS over time. But due to the several problems, such as costs, exposure to radiation, specialized equipments or delayed feedback for therapeutic choices, make measurements difficult to put into practice in many clinical settings.[11]
During the clinical examination or assessment of the the patient, palpate over the glenohumeral joint labrum and head of humerus, if there is gap or feeling of slight depression, known as the 'Sulcus sign'. The Sulcus is an indication of shoulder joint subluxation. it can be graded through Finger breadth palpation method,
So other method commonly used is the Fingerbreadth palpation method[12].
Fingerbreadth Palpation Method[edit | edit source]
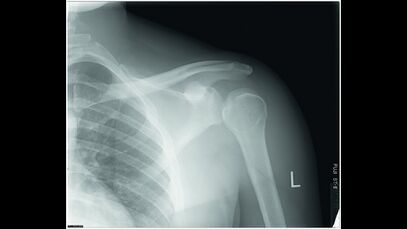
Patients should sit in a chair or wheelchair with both feet flat on the ground or footrest. The physical therapist first assesses the unaffected side to palpate the gap between the acromion and the humerus head and repeat the same on the affected shoulder. Shoulders should be positioned in neutral rotation, with the arm hanging by the side (thumb pointing forward) close to the body with no abduction (As shown in figure below).
Figure. Patient position in fingerbreadth palpation method[13]
Glenohumeral subluxation is defined as a palpable gap between the inferior aspect of the acromion and the superior aspect of the humeral head that is ½ fingerbreadth or more. A 0–5 grading scales are as follow:
| 0 | No subluxation |
|---|---|
| 1 | ½ fingerbreadth gap |
| 2 | 1 fingerbreadth gap |
| 3 | 1½ fingerbreadth gap |
| 4 | 2 fingerbreadth gap |
| 5 | 2½ fingerbreadth gap |
Evidence Based Physical Therapy Management[edit | edit source]
Education[edit | edit source]
Caregivers/Health Professionals/Relatives need to be informed on the importance of proper handling of the arm. Stroke patients who have their arm unsupported and/or handled inappropriately by caregivers (pulling on the arm) are at a higher risk for traction neuropathy and injury. Hence, caregivers of stroke survivors must be adequately trained in handling the hemiplegic arm, especially when shoulder subluxation is present.[14][15][5][16]
Mechanical Approaches[edit | edit source]
Shoulder support or orthosis while in situ could reduce the subluxation temporarily.[17]
Positioning[edit | edit source]
Lap trays, Pillows and foam support help to keep the arm and shoulder supported in the correct position. Good positioning will help reduce strain on your ligaments and prevent frozen shoulder from occurring.[14][15][5][18]
Slings[edit | edit source]
Studies have shown the effectiveness of slings to prevent GHS, but no investigation assessed the efficacy of slings in relation to the duration of their use. Supports from slings have various purposes: realigning scapular symmetry, supporting the forearm in a flexed arm position, improving anatomic alignment with auxiliary support, or supporting the shoulder with a cuff.[11]
The use of slings has been considered a contraindication by some authors because slings can facilitate an increase in flexor tone and synergistic patterns, cause reflex sympathetic dystrophy, restrain functional recovery, obstruct arm swing during walking, and for some, impair body image.[11]
On the other hand, slings are generally simpler for caregivers than functional electrical stimulation (FES) or strapping, and they can be combined with the other treatments. Reviewing the literature and knowing the structural characteristics of slings can help identify the best treatment for preventing and treating GHS.[11]
Strapping/Taping[edit | edit source]
Shoulder strapping is helpful in the first period after stroke. Shoulder strapping is used clinically in patients with stroke, with a various techniques being employed; however, White et al. had brought out two main trends emerging from the literature.
- Longitudinal strapping method
It involves applying two to three strips of strapping with upward tension along the anterior, middle, and posterior deltoid, extending to cover the shoulder complex, occasionally incorporating an anchor strip..[19]
- Circumferential strapping method
It is the application of strapping around the shoulder joint. It originates from the clavicle, wrapping around the deltoid to go under the axilla (over a protective pad) and ending on the spine of the scapula.
The study done by White et al., 2018 shows that longitudinal strapping of the shoulder in patients with stroke seems to positively influence shoulder subluxation and pain.[20]
A study conducted by Chatterjee et al. found the California Tri-pull Taping method to reduces pain, improve active shoulder flexion, and improve distal upper extremity functional ability. This appears to be a promising early adjunctive treatment for clients who have suffered a stroke and demonstrate pain in a subluxed shoulder. This taping method allows the patients to participate in all active UE exercises as well as all ADL's. However, there was no follow-up to determine if the effects demonstrated were maintained.[21]
Another study concluded that a beneficial effect of kinesio taping for reducing shoulder subluxation, improving motor function of the UE and activities of daily living in patients with hemiplegic shoulder pain post-intervention, which could not be interpreted simply as a placebo effect. And it was associated with reduced pain for patients with chronic stroke.[22]
Neuromuscular Approaches: Neuromuscular electrical stimulation[edit | edit source]
Electrical stimulation conventional transcutaneous electrical nerve stimulation(TENS) is given to relieve pain.
Electrical stimulation can prevent shoulder subluxation and decrease shoulder pain in acute phase, but this effect was not maintained after the withdrawal of treatment in later follow-ups.[23][17][24]
| Indication | Patient Position | Electrode Placement | Parameter Recommendations |
|---|---|---|---|
| Prevention or treatment of
shoulder sublux resulting from UE flaccidity poststroke |
Patient sitting with arm support | One channel over the muscle belly of supraspinatus
and posterior deltoid. Avoid upper trapezius fibres and excessive shoulder shrug. Applying a second channel to stimulate the long head of the biceps can be beneficial in correcting humeral head alignment. |
NMES waveform: symmetric or asymmetric biphasic PC
Frequency: 30–35 Hz Pulse duration: 250–350 ms Current amplitude: sufficient to produce a smooth,sustained muscle contraction and reduction of shoulder sublux Work–rest cycle: ON:OFF 10–15 s ON time with progressively shorter rest time (30 s ON time, 2 s OFF time). Rampup time (1–4 s) is set to ensure patient comfort; longer ramp-down time may be required to prevent pain or tissue stretching when the arm sags due to gravity. Treatment schedule: progress to 2–4 h/d on the basis of muscle fatigue Session frequency: 7 d/wk for 4–6 wk or until voluntary control has been restored |
Combination of Long-Duration Electrical Stimulation with External Shoulder Support during Routine Daily Activities is beneficial in reducing shoulder subluxation and improving upper-extremity function while the Fugl Meyer Assesment -Upper Extremity and FMA-hand and finger subscales were significantly improved
Facilitation of Movement[edit | edit source]
Exercises[edit | edit source]
- In the early rehabilitation phase, passive range of motion exercises has been shown to effectively prevent shoulder subluxation among stroke patients. Range-of-motion exercises for the shoulder joint include flexion-extension, abduction-adduction and external-internal rotation. Take care as if improperly carried out, it can cause injury to the shoulder and increase the stroke patient’s risk for shoulder subluxation.[15]
- One of the common therapeutic techniques is Bobath: the method is entered on the idea that patients should be moved and positioned into reflex inhibiting positions "the hemiparetic limb should be away from abnormal increases in muscle tone. [26]
- Weight-bearing exercises on the affected upper extremity proved to be beneficial. From a seated position on your bed or bench, prop yourself up on your affected arm by placing your affected arm about a foot away from your body. Then lean into it. If the patient feels comfortable, this position should last for 10 seconds or so. And if otherwise, it should be stopped immediately.[18]
A study done by Ruthber et al,2020 concluded that Robotic therapy positively influenced in the decrease and annulment of pain and the spasticity degree, reaching a range increase of joint movement and the improvement of muscle tone.[27]
A study done by Jung et al., 2019 has shown that active shoulder exercise with a sling suspension system may effectively reduce shoulder subluxation and improve proprioception and upper extremity function in patients following acute stroke.[6]
The 5-minute video below gives some good exercises to use for the hemiplegic shoulder. In this video, the physiotherapist shows and teachs his patient different types of exercices to prevent or to reduce the pain in the shoulder: Stretch the thumb and the fingers on the affected hand with the unaffected using a ball with different sizes.
The therapist will instruct the patient on how to do stretches, but these are some general guidelines:
- Move the arm through its full range of motion at least three times a day.
- Gently stretch tighter muscles to a point of slight discomfort.
- Then hold the stretch for at least 60 seconds.
Drug Treatment[edit | edit source]
In addition to physiotherapy, electrotherapy and other various methods to reduce pain in Hemiplegic Shoulder Pain (HSP), the use of Analgesic, anti-inflammatory and corticosteroid injections have been used to treat and reduce pain[29].
Resources[edit | edit source]
- Stroke Engine
- Evidence-Based Review of Stroke Rehabilitation
- American Heart Association, Inc.
- Shoulder Subluxation
References[edit | edit source]
- ↑ Lavi C, Elboim-Gabyzon M, Naveh Y, Kalichman L. A Combination of Long-Duration Electrical Stimulation with External Shoulder Support during Routine Daily Activities in Patients with Post-Hemiplegic Shoulder Subluxation: A Randomized Controlled Study. Int J Environ Res Public Health. 2022 Aug 8;19(15):9765. doi: 10.3390/ijerph19159765. PMID: 35955118; PMCID: PMC9368353.
- ↑ Arya KN, Pandian S, Vikas, Puri V. Rehabilitation methods for reducing shoulder subluxation in post-stroke hemiparesis: a systematic review. Topics in stroke rehabilitation. 2018 Jan 2;25(1):68-81.
- ↑ Kim, M.G., Lee, S.A., Park, E.J., Choi, M.K., Kim, J.M., Sohn, M.K., Jee, S.J., Kim, Y.W., Son, J.E., Lee, S.J. and Hwang, K.S., 2022. Elastic Dynamic Sling on Subluxation of Hemiplegic Shoulder in Patients with Subacute Stroke: A Multicenter Randomized Controlled Trial. International Journal of Environmental Research and Public Health, 19(16), p.9975.
- ↑ Murie-Fernández M, Iragui MC, Gnanakumar V, Meyer M, Foley N, Teasell R. Painful hemiplegic shoulder in stroke patients: causes and management. Neurología (English Edition). 2012 May 1;27(4):234-44.
- ↑ 5.0 5.1 5.2 Stroke-rehab.com [Internet]. Shoulder subluxation.
- ↑ 6.0 6.1 6.2 Jung KM, Choi JD. The Effects of Active Shoulder Exercise with a Sling Suspension System on Shoulder Subluxation, Proprioception, and Upper Extremity Function in Patients with Acute Stroke. Medical science monitor: international medical journal of experimental and clinical research. 2019;25:4849.
- ↑ Praveen Kumar, Marianne Mardon, Michael Bradley, Selena Gray, Annette Swinkels, Assessment of Glenohumeral Subluxation in Poststroke Hemiplegia: Comparison Between Ultrasound and Fingerbreadth Palpation Methods, Physical Therapy, Volume 94, Issue 11, 1 November 2014, Pages 1622–1631.
- ↑ Poduri KR. Shoulder pain in stroke patients and its effects on rehabilitation. Journal of Stroke and Cerebrovascular Diseases. 1993 Jan 1;3(4):261-6.
- ↑ Anwer S, Alghadir A. Incidence, prevalence, and risk factors of hemiplegic shoulder pain: a systematic review. International journal of environmental research and public health. 2020 Jul;17(14):4962.
- ↑ . Stolzenberg D, Siu G, Cruz E. Current and future interventions for glenohumeral subluxation in hemiplegia secondary to stroke. Top Stroke Rehabil 2012;19:444-456.
- ↑ 11.0 11.1 11.2 11.3 11.4 11.5 11.6 Paci M, Nannetti L, Rinaldi LA. Glenohumeral subluxation in hemiplegia: An overview. Journal of Rehabilitation Research & Development. 2005 Jul 1;42(4).
- ↑ Kumar P, Mardon M, Bradley M, Gray S, Swinkels A. Assessment of glenohumeral subluxation in poststroke hemiplegia: Comparison between ultrasound and fingerbreadth palpation methods. Physical therapy. 2014 Nov 1;94(11):1622-31.
- ↑ Kumar P, Mardon M, Bradley M, Gray S, Swinkels A. Assessment of glenohumeral subluxation in poststroke hemiplegia: Comparison between ultrasound and fingerbreadth palpation methods. Physical therapy. 2014 Nov 1;94(11):1622-31.
- ↑ 14.0 14.1 Kumar P, Fernando C, Mendoza D, Shah R. Risk and associated factors for hemiplegic shoulder pain in people with stroke: a systematic literature review. Physical Therapy Reviews. 2022;27(3):191–204.
- ↑ 15.0 15.1 15.2 Seneviratne C, Then KL, Reimer M, Then KL, Reimer M. Post-stroke shoulder subluxation: a concern for neuroscience nurses. Axone. 2005 Sep 1;27(1):26.
- ↑ Duncan PW, Zorowitz R, Bates B, Choi JY, Glasberg JJ, Graham GD, Katz RC, Lamberty K, Reker D. Management of adult stroke rehabilitation care: a clinical practice guideline. stroke. 2005 Sep 1;36(9):e100-43.
- ↑ 17.0 17.1 Arya KN, Pandian S, Vikas, Puri V. Rehabilitation methods for reducing shoulder subluxation in post-stroke hemiparesis: a systematic review. Topics in stroke rehabilitation. 2018 Jan 2;25(1):68-81.
- ↑ 18.0 18.1 FlintRehab [Internet]. Shoulder Exercises for Stroke Patients from an Expert Occupational Therapist; 2021 feb 1.
- ↑ Comley-White N, Mudzi W, Musenge E. Effects of shoulder strapping in patients with stroke: A randomised control trial. South African Journal of Physiotherapy. 2018 May 7;74(1):1-1.
- ↑ Comley-White N, Mudzi W, Musenge E. Effects of shoulder strapping in patients with stroke: A randomised control trial. The South African journal of physiotherapy. 2018;74(1).
- ↑ Chatterjee S, Hayner KA, Arumugam N, Goyal M, Midha D, Arora A, Sharma S, Kumar SP. The California tri-pull taping method in the treatment of shoulder subluxation after stroke: a randomized clinical trial. North American journal of medical sciences. 2016 Apr;8(4):175.
- ↑ Deng P, Zhao Z, Zhang S, Xiao T, Li Y. Effect of kinesio taping on hemiplegic shoulder pain: A systematic review and meta-analysis of randomized controlled trials. Clinical Rehabilitation. 2021 Mar;35(3):317-31.
- ↑ Linn SL, Granat MH, Lees KR. Prevention of shoulder subluxation after stroke with electrical stimulation. Stroke. 1999 May;30(5):963-8.
- ↑ Zhou M, Li F, Lu W, Wu J, Pei S. Efficiency of neuromuscular electrical stimulation and transcutaneous nerve stimulation on hemiplegic shoulder pain: a randomized controlled trial. Archives of physical medicine and rehabilitation. 2018 Sep 1;99(9):1730-9.
- ↑ Nussbaum EL, Houghton P, Anthony J, Rennie S, Shay BL, Hoens AM. Neuromuscular electrical stimulation for treatment of muscle impairment: critical review and recommendations for clinical practice. Physiotherapy Canada. 2017;69(5):1-76.
- ↑ Bender L, McKenna K. Hemiplegic shoulder pain: defining the problem and its management. Disabil Rehabil. 2001;23:698–705.
- ↑ Serrezuela RR, Quezada MT, Zayas MH, Pedrón AM, Hermosilla DM, Zamora RS. Robotic therapy for the hemiplegic shoulder pain: a pilot study. Journal of neuroengineering and rehabilitation. 2020 Dec;17(1):1-2.
- ↑ Bob and Brad Top 3 Exercises for Weak Arm after Stroke (Simple Do-it-yourself).
- ↑ Van Ouwenaller C, Laplace P,Chantraine A (1986) Painful shoulder in hemiplegia Arch Phys Med Rehabil 46:23–26.
![Figure. Patient position in fingerbreadth palpation method[13]](/images/thumb/f/f0/Fingerbreadth_Palpation_method.jpg/306px-Fingerbreadth_Palpation_method.jpg)