Dynamic Stabilisers of the Shoulder Complex
Original Editor - Khloud Shreif
Top Contributors - Khloud Shreif, Amanda Ager, Kim Jackson and Rishika Babburu
Introduction[edit | edit source]
The stability of the shoulder joint, like any other joint in the body depends, on both static and dynamic stabilizers. However, because of the vast range of motion of the shoulder complex (the most mobile joint of the human body), dynamic stabilizers are crucial for a strong sense of neuromuscular control throughout all movements and activities involving the upper extremities.
Neuromuscular control in this context, can be understood as the “unconscious activation of dynamic restraints occurring in preparation for, and in response to, joint motion and loading for the purpose of maintaining functional joint stability.”[1] Dynamic restraints result from neuromuscular control over the shoulder muscles, facilitated through motor control and proprioceptive input.
Moreover, the term sensorimotor system describes the sensory, motor, and central integration and processing components involved in maintaining joint homeostasis during bodily movements - more commonly understood to be functional joint stability.[2]
Lastly, proprioception within this context can be understood as an important component of the sensorimotor system; whereby the balance between mobility and stability of the glenohumeral (GH) joint is ensured by a neuromuscular interaction between capsular ligamentous receptors, the central nervous system (CNS), and the stabilizing muscles of the shoulder complex.[3]
Static stabilizers include the joint labrum and capsuloligements components of the glenohumeral joint, as well as fascia tissues throughout the shoulder complex. There is also a theory that the neuromuscular bundle (nerves, veins, arteries) can also contribute to static stability.
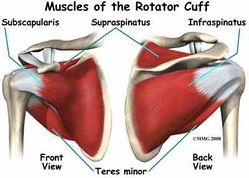
Dynamic stabilizers include the contractile tissues of the shoulder complex (tendons, muscles and tendon-muscular junctions). The most well known are the rotator cuff muscles (supraspinatus, infraspinatus, subscapularis, Teres minor), which collectively control the fine-tuning movement of the humeral head within the glenoid fossa (maintain centralization of the humeral head during static postures and dynamic movements). There are also the periscapsular muscles[4], which are very important for homogeneous shoulder movements while avoiding biomechanical misalignments, such as a shoulder impingement.
Dynamic stabilization during upper extremity movements is obtained by synergetic mechanisms of shoulder muscles’ co-contractions, appropriate positioning, control and coordination of the shoulder as well as the scapula-thoracic complex.[5][6]
The dynamic stability of shoulder complex can be divided into:
- Glenohumeral stability (Local)
- Scapulothoracic stability (Global)
See the Physiopedia page on the Biomechanics of the Shoulder, for an in-depth exploration of accessory movements and the contributions of global movers and fine-tuning muscles of the shoulder complex.
Glenohumeral joint stability[edit | edit source]
Deltoid muscle[edit | edit source]
The deltoid muscle has a significant role as a stabilizer, and is generally accepted as a prime mover for glenohumeral joint during abduction, along with the supraspinatus muscle.
The deltoid is the primary muscle responsible for the abduction of the arm from 15 to 90 degrees. It also serves as a stabilizer of the humeral head, especially in instances of carrying a load.[8]
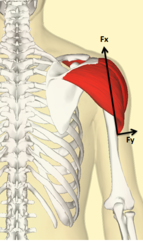
From the biomechanical figure, the line of action (line of pull) of the deltoid with the arm at the side of body, the parallel force component (fx) directed superiorly, is the largest of the three other components; resulting in a superior translation of the humeral head, and a small applied perpendicular force is directed towards rotating the humerus. Also, there is an inferior pull of force (fx), to offset the component of the middle deltoid which is active during arm elevation, as gravity cannot balance the force around the GH joint alone.[9]
Blood supply of the deltoid: The posterior circumflex humeral artery and the deltoid branch of the thoracoacromial artery are the vascular sources for the deltoid.[11]
Innervation of the deltoid: The neural supply of the deltoid is via the axillary nerve (C5, C6) from the posterior cord of the brachial plexus.[11]
Rotator Cuff muscles[edit | edit source]
Rotator cuff (RC) (collectively the following muscles: supraspinatus, subscapularis, infraspinatus, teres minor) not only abduct the shoulder, but also plays an important role as stabilizer muscles.[12] The main role of the rotator cuff is to control the fine-tuning (smaller) movements of the head of the humerus, within the glenoid fossa (often thought of as the accessory movements). The rotator cuff muscles help to maintain a centralized position of the head of the humerus during static postures and dynamic movements. This is crucial with regards to neuromuscular control, as it helps to avoid a biomechanical impingement of the soft tissues, under the subacromial arch during elevation movements.
From Figure 2 we can see three of the RC muscles (teres minor, subscapularis, infraspinatus), in relation to their anatomical position and their muscle fiber direction from origin to insertion. This is important to note, as they tend to have a similar inferior line of pull[10] and with the summation of the three force vectors of rotator cuff, they nearly offset the superior translation of humeral head, created by the deltoid muscle.
Also, the wide range of motion of the shoulder is allowed by the variety of rotational moments of the cuff muscles[13]. The teres minor and infraspinatus muscles are external rotators and participate in the clearing of the greater tubercle underneath the acromion during shoulder movements.
Supraspinatus muscle[edit | edit source]
Supraspinatus abducted the shoulder from (0-15), and has an effective role as a shoulder stabilizer muscle by keeping the humeral head pressed medially against the glenoid cavity this stability function allows supraspinatus to contribute with deltoid in shoulder abduction.
Regarding the location of the supraspinatus muscle, it is more superior than the other three rotator cuff muscles. Therefore, it has a more superior line of pull which cannot offset the line of force emitted from the deltoid muscle.
From Figure 1 and 2, we can consider the deltoid and rotator cuff muscles as a collective force coupling for the movements associated with the glenohumeral joint.
An Imbalance of one or more of these muscles can cause biomechanical misalignments and contribute to shoulder dysfunctions such as: impingement disorders, bursitis, instabilities, scapular dyskinesia or chronic conditions associated with pathological wear and tear.
Blood supply of the supraspinatus: The suprascapular artery delivers blood to the supraspinatus muscle.[11]
Innervation of the supraspinatus: The neural supply of the supraspinatus is by the suprascapular nerve (C5, C6) from the upper trunk of the brachial plexus.[11]
Scapulothoracic joint stability[edit | edit source]
Because the scapulothoracic joint is a floating joint, it solely relies on neuromuscular control (adequate strength and control of the stabilizer muscles, as well as a healthy sense of muscular timing). Agonist, antagonist and synergist muscle control is vital for a normalized and non-pathological scapulothoracic rhythm. During movements in elevation and reaching activities, it is important to consider the force-coupling which acts on the floating joint. Such muscles to consider are the serratus anterior, serratus posterior, the trapezius (upper / middle / lower), the rhomboids, teres major, the levator scapulae, the latissimus dorsi and the flexibility and mobility of the thoracolumbar fascia.
Serratus anterior and Trapezius muscles[14][edit | edit source]
Serratus anterior (SA)[edit | edit source]
During reaching or functional activities that require functional forward length of your upper limb, your scapula will be protracted and upward rotated that is achieved primarily by serratus anterior ms. As the movement of the scapulothoracic occurs in response to the combination of the movement of AC and SC joint. SA produces this movement by acting on the scapula, It can maintain scapulothoracic upward rotation within the entire range of arm elevation, and also contributes to external rotation and post tilting of the scapula. The lower fiber of SA has a longer moment arm to maintain this scapular upward rotation.
Lowe trapezius muscle assists with SA to upwardly rotate the scapula which helps to maintain subacromial space[15].
The strong action of serratus as a protractor/upward rotator needs an apposite force to control this movement (equally strong antagonist). The serratus anterior and trapezius (middle) muscles work as a primary force coupling to upwardly rotate the scapula.
Blood supply of serratus anterior: upper part of the lateral and superior thoracic artery, the lower part of the thoracodorsal artery
Innervation of serratus anterior: long thoracic nerve C5-C7 from brachial plexus
Trapezius[16][edit | edit source]
It's an extensive, superficial muscle subdivided into the upper, middle, and posterior part, each part has different fibers direction that’s why it has different actions. Upper part inserts into the clavicle and has no attachment to the scapula, middle attached to the acromion and spine of the scapula, and the lower part inserts into the medial base of the scapular spine.
It's more active during arm elevation in abduction and has a gradual linear increase in activity with the increase of abduction angle.
Upper trapezius: hence the scapulothoracic movement occurs in response to the combination of the movement of AC and SC joint and the upper trapezius attaches to clavicle it has an indirect weak effect on scapular upward rotation and strong effect on scapular external rotation. When it contracts with a fixed craniocervical region it elevates and retracts the clavicle at the level of the sternoclavicular joint[14]. Clavicle retraction contributes to 100% of scapular external and the clavicle elevation contributes to about 75% of scapular anterior tilt and 25% of scapular upward rotation of the scapula.
Middle and lower fibers: they contribute with serratus anterior to rotate scapula upward, externally rotate the scapula through their torque on AC joint and have a retractor force on scapula that force offsets the protraction of SA muscle
Lower trapezius: along with the serratus anterior muscle, they are a primary upward rotators of the scapula. It contributes to the scapular upward rotation when the axis of elevation reaches the acromioclavicular joint.
Middle trapezius: it has both a downward and upward moment arm arriving from the scapula. Its downward moment arm is stronger (larger moment arm) than upward moment on the scapula plus its retraction force, it contributes to the offset of the strong action of serratus anterior as a protractor and upward rotator (acts as an antagonist)
The serratus anterior and trapezius muscles act as agnostics for scapular upward rotation. and prevent downward rotatory movement created by deltoid (middle/posterior) and are a synergistic muscle with deltoid regards to glenohumeral forces to abduct the G.H joint.
During shoulder extension or when returning your arm beside your body, this movement is associated with scapular downward rotation, internal rotation, and shoulder depression.[edit | edit source]
Latissimus Doris, Pectoralis major.[edit | edit source]
Latissimus dorsi is a muscle of posterior back has an attachment to scapula and humerus. Pectoralis major is a superficial muscle of the pectoral region and has a sternal and clavicular part. The latissimus dorsi contributes to adduct and depress the scapula and shoulder complex with pectoralis major that adduct the shoulder.
They have a stabilization role during arm elevation; latissimus dorsi via its compression force to G.H joint, pectoralis major through higher going reaction force.
Pectoralis minor.[edit | edit source]
It has an attachment to the coracoid process, hence it contributes to scapular downward rotation, internal rotation and anterior tipping. moreover, it is a synergistic with latissimus and pectoralis major to adduct and internally rotate the shoulder as it has a function of adduction and internal rotation of the shoulder.[18]
Rhomboids and teres major muscles[edit | edit source]
Teres major has the same action of latissimus dorsi of adduction, extension, internal rotation. And as it attaches to scapula proximally, humerus distally, for effective adduction and extension it acts to pull humerus to the scapula (stable part), and hence this movement associated with scapula downward rotation and retraction.
Teres major function depends on rhomboids activity as scapular retractor muscles that stabilize the scapula on the thoracic wall during adduction and extension of the GH joint to downward rotate the scapula, and without sufficient stability teres major will upward rotate instead of downward rotation.
Moreover, the rhomboid muscles act eccentrically to control the change in the position of the scapula during arm elevation. Therefore, it acts as a counter to the lateral translation force of the serratus anterior muscle.
Clinical presentation[edit | edit source]
For smooth synchronous movement of the shoulder complex we need the force couplings of the glenohumeral and scapulothoracic joints to work in a synched timing and adequate forces to offset each other.
For example; the deltoid muscle (middle fiber in particular) acts to stabilize the humeral head against the glenoid cavity during arm elevation, while the rotator cuff muscles (specifically the subscapularis, teres minor, infraspinatus muscles) control the fine-tuning movement of the humeral head.
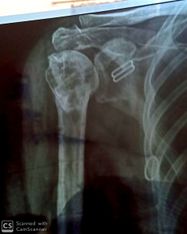
Deficits in these forces, for example, insufficient activation of rotator cuff /deltoid muscles or an over activation of the muscles, can lead to a narrowing of the sub-acromial space (Figure 3). This can compress the tendons and soft tissues within this space, leading to acute or chronic inflammation and dysfunction ( rotator cuff tendinopathy /shoulder impingement)[19].
Also, scapular winging and scapular dyskinesia can occur as a result of scapular muscle imbalances. For example; weakness with the serratus anterior and lower trapezius muscle, and/or an over activation of the upper trapezius muscle, scapular downward rotators overactivity for a long time all affect the scapula upward rotation and you can find scapula on anterior tipping. and adaptive pectoralis minor shorting[18]. This changes the dominant line of pull of the scapula during movements and can cause pathological movement patterns.
Physical therapy interventions[edit | edit source]
Rehabilitation should concentrate on the restoration of the normal biomechanical alignment of the shoulder complex (centralization of the GH joint, proper scapulothoracic gliding of the scapula) as well as restoring the proper force-coupling balance of the stabilizing muscles.
Appropriate strengthening of the shoulder dynamic stabilizer muscles and adequate neuromuscular control-patterns is crucial during rehabilitation as well as the prevention of shoulder injuries.[5][20]
Neuromuscular exercises typically focus on movement quality, as guided by the supervising physical therapists. Neuromuscular exercises typically included strength, coordination, balance, and proprioception components.[21]
Exercises can be performed unilaterally, or bilaterally in unstable conditions involving an increased level of postural control (standing, planking, kneeling and laying on stability ball) and/or with external overload devices challenging motor-coordination (elastics, balls, dumbbells).[22]
Resistance training exercises can promote neural and structural modifications to the shoulder complex[23][24] and can increase the sensory, biomechanical, and motor-processing patterns[25] (such as to the cervico-thoracic spine, the shoulder complex and the upper extremities as a whole).
Kinetic chain exercises for lower limb and trunk during shoulder rehabilitation can reduce the demand on the rotator cuff, improve the recruitment of axioscapular muscles[26].
Overall, to rehabilitate the neuromuscular control of the shoulder complex, the therapist should focus on the following elements:[edit | edit source]
- Full and pain free range of motion of the cervical and thoracic spine.
- No neurological signs or symptoms from the cervical spine, throughout the upper extremities.
- Full and pain free range of motion of all distal joints (digits, thumb, wrist, elbow).
- Postural control (neutral spine, centralization of the GH joint, proper scapular setting) during static and dynamic conditions.
- Proper biomechanical alignment and accessory movements of the 4 shoulder complex joints (GH joint, acromioclavicular joint, sternoclavicular joint, and the floating scapulothoracic joint[27]). Also prudent to verify the overall mobility of the thoracic cage and breathing movements.
- Strengthening of the typically weak / inhibited muscles (Such as the serratus anterior, rotator cuff muscles, lower trapezius, rhomboid muscles)
- Presence of tight muscles due to postural stress and neurological hyperactivity (such as the presence of trigger points).
- Tightness and lack of mobility of surrounding fascia or fascial trains.
- Lack of mobility of the upper extremity, cervical and thoracic neurological tissues (nerve flossing exercises as needed).
- Tension in any static tissues (such as the GH capsule).
- Dynamic stretching of the typically shortened and possibly over-active muscles (Pectorals muscles, upper trapezius, levator scapulae muscles)
- Reeducation of the rotator cuff muscles (working in rotations at various angles of elevation, scaption movements and functional activities).
- Eccentric exercises for rotator cuff muscles in case of a suspected rotator cuff tendinopathy[28][29], to restore collagen alignment of the tendons.
- Strengthening of surrounding supportive musculature (Biceps, triceps, latissimus dorsi, rhomboids, cervical stability muscles, dorsal spine supportive musculature).
- Muscles re-education of the agonist, antagonist, and synergist muscles. Muscular timing (coordinator contractions) is a key component to focus on during shoulder rehabilitation.
Progression factors to consider to challenge the neuromuscular control of the shoulder complex:[edit | edit source]
- Postural control and positioning : static postures towards dynamic movements.
- Strengthening: body weight / rehabilitation bands / free weights / functional strengthening.
- Repetitions: endurance (high repetitions, low load), strength and performance (low repetitions, high load).
- Speed: slow movements towards quicker movements (always under control).
- Joint loading: non-weightbearing towards weight-bearing.
- Surface: stable surface (wall / floor) towards unstable surface (bosu ball, stability disc, movement boards) also incline vs. decline.
- Joint movements: Single joint movements (i.e. GH joint only) towards multi-joint movements (entire shoulder complex and upper extremity).
- Functional movements: throwing, catching, rolling and sport specific movements. Also the use of external perturbations, such as the Water Pipe (training equipment with sand or liquid inside to cause reactionary movements).
For more exercises for the rotator cuff complex:[edit | edit source]
- Selecting exercises-for rotator cuff related shoulder pain interview with hilkka virtapohja
- OrthoInfo
- Systematic review: Exercise rehabilitation for rotator cuff tears (2016)
[edit | edit source]
- Proprioception
- Neuromuscular exercise program
- Neuromuscular adaptations to exercise
- Shoulder instability
- Motor control
- Biomechanics of the shoulder
- Throwing biomechanics
Check out some more resources:[edit | edit source]
References[edit | edit source]
- ↑ Myers, J.B., C.A. Wassinger, and S.M. Lephart. Sensorimotor Contribution to Shoulder Joint Stability, in The Athlete’s Shoulder. 2009, Elsevier. p. 655-669.
- ↑ Lephart SM, Riemann BL, Fu FH. Introduction to the sensorimotor system. In: Lephart SM, Fu FH, eds. Proprioception and Neuromuscular Control in Joint Stability. Champaign, IL: Human Kinetics; 2000:37–51
- ↑ Blasier RB, Carpenter JE, Huston LJ (1994) Shoulder proprioception: effect of joint laxity, joint position and direction of motion. Orthop Rev 23:45–50.
- ↑ Curl LA, Warren RF. Glenohumeral joint stability: selective cutting studies on the static capsular restraints. Clinical Orthopaedics and Related Research®. 1996 Sep 1;330:54-65.
- ↑ 5.0 5.1 Wilk KE, Yenchak AJ, Arrigo CA, Andrews JR. The advanced throwers ten exercise program: a new exercise series for enhanced dynamic shoulder control in the overhead throwing athlete. Phys Sportsmed. 2011;39(4):91–3847. https://doi.org/10.3810/psm.2011.11.1943.
- ↑ Myers JB, Lephart SM. The role of the sensoriomotor system in the athletic shoulder. J Athl Train. 2000;35(3):351–63.
- ↑ GUStrength. What is a Muscle Force Couple?. Available from: http://www.youtube.com/watch?v=mm9_WrrGCEc[last accessed 4/5/2020]
- ↑ Hallock GG. The hemideltoid muscle flap. Ann Plast Surg. 2000 Jan;44(1):18-22.
- ↑ Levangie PK, Norkin CC. Joint Structure and Function; A Comprehensive Analysis. 5th. Philadelphia: Fadavis Company. 2012.
- ↑ 10.0 10.1 Levangie PK, Norkin CC. Joint Structure and Function; A Comprehensive Analysis. 5th. Philadelphia: Fadavis Company. 2012.
- ↑ 11.0 11.1 11.2 11.3 Lam JH, Bordoni B. Anatomy, Shoulder and Upper Limb, Arm Abductor Muscles. [Updated 2020 Mar 31]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK537148/
- ↑ Escamilla RF, Yamashiro K, Paulos L, Andrews JR. Shoulder muscle activity and function in common shoulder rehabilitation exercises. Sports medicine. 2009 Aug 1;39(8):663-85.
- ↑ Longo UG, Berton A, Papapietro N, Maffulli N, Denaro V. Biomechanics of the rotator cuff: European perspective. InRotator Cuff Tear 2012 (Vol. 57, pp. 10-17). Karger Publishers.
- ↑ 14.0 14.1 Ludewig PM, Braman JP. Shoulder impingement: biomechanical considerations in rehabilitation. Manual therapy. 2011 Feb 1;16(1):33-9.
- ↑ Neumann DA, Camargo PR. Kinesiologic considerations for targeting activation of scapulothoracic muscles: part 1: serratus anterior. Brazilian journal of physical therapy. 2019 Feb 2.
- ↑ Camargo PR, Neumann DA. Kinesiologic considerations for targeting activation of scapulothoracic muscles–part 2: trapezius. Brazilian journal of physical therapy. 2019 Feb 3.
- ↑ Muscle and Motion. Force Couple , Scapular Force Couple. Available from: http://www.youtube.com/watch?v=YbbzQs7OBoY[last accessed 12/3/2020]
- ↑ 18.0 18.1 Phadke V, Camargo PR, Ludewig PM. Scapular and rotator cuff muscle activity during arm elevation: a review of normal function and alterations with shoulder impingement. Brazilian Journal of Physical Therapy. 2009 Feb;13(1):1-9.
- ↑ <article> Joseph B. Myers, Ji-Hye Hwang, Maria R. Pasquale, J. Troy Blackburn and Scott M. Lephart. Rotator cuff coactivation ratios in participants with subacromial impingement syndrome. Journal of Science and Medicine in Sport, Volume 12, Issue 6, November 2009, Pages 603-608 </article>
- ↑ Reinold MM, Gill TJ, Wilk KE, Andrews JR. Current concepts in the evaluation and treatment of the shoulder in overhead throwing athletes, part 2: injury prevention and treatment. Sports Health. 2010;2(2):101–15. https://doi.org/10.1177/1941738110362518.
- ↑ Eshoj, H. R., Rasmussen, S., Frich, L. H., Hvass, I., Christensen, R., Boyle, E., Juul-Kristensen, B. (2020). Neuromuscular Exercises Improve Shoulder Function More Than Standard Care Exercises in Patients With a Traumatic Anterior Shoulder Dislocation: A Randomized Controlled Trial. Orthopaedic Journal of Sports Medicine. https://doi.org/10.1177/2325967119896102
- ↑ Baritello, O., Khajooei, M., Engel, T. et al. Neuromuscular shoulder activity during exercises with different combinations of stable and unstable weight mass. BMC Sports Sci Med Rehabil 12, 21 (2020). https://doi.org/10.1186/s13102-020-00168-x.
- ↑ Aagaard P, Simonsen EB, Andersen JL, Magnusson P, Dyhre-Poulsen P. Neural adaptation to resistance training: changes in evoked V-wave and H-reflex responses. J Appl Physiol. 2002;92(6):2309–18. https://doi.org/10.1152/japplphysiol.01185.2001.
- ↑ Behm DG. Neuromuscular implications and applications of resistance training; 1995. p. 264–74.
- ↑ Behm DG, Anderson KG. The role of instability with resistance training. J strength Cond Res. 2006;20:716–22.
- ↑ Richardson E, Lewis JS, Gibson J, Morgan C, Halaki M, Ginn K, Yeowell G. Role of the kinetic chain in shoulder rehabilitation: does incorporating the trunk and lower limb into shoulder exercise regimes influence shoulder muscle recruitment patterns? Systematic review of electromyography studies. BMJ Open Sport & Exercise Medicine. 2020 Apr 1;6(1):e000683.
- ↑ Moghadam AN, Abdi K, Shati M, Dehkordi SN, Keshtkar AA, Mosallanezhad Z. The effectiveness of exercise therapy on scapular position and motion in individuals with scapular dyskinesis: systematic review protocol. JMIR research protocols. 2017;6(12):e240.
- ↑ Larsson R, Bernhardsson S, Nordeman L. Effects of eccentric exercise in patients with subacromial impingement syndrome: a systematic review and meta-analysis. BMC musculoskeletal disorders. 2019 Dec 1;20(1):446.
- ↑ Ortega-Castillo M, Medina-Porqueres I. Effectiveness of the eccentric exercise therapy in physically active adults with symptomatic shoulder impingement or lateral epicondylar tendinopathy: a systematic review. Journal of Science and Medicine in Sport. 2016 Jun 1;19(6):438-53.
- ↑ White Lion Athletics. Resistance Band Exercises: Best Exercises for Shoulder Rehab and Scapular Stabilzation. Available from: http://www.youtube.com/watch?v=Vez6-NTFkS8[last accessed 11/4/2020]