Distal Tibiofibular Syndesmosis
Original Editor - Tarina van der Stockt
Top Contributors - Tarina van der Stockt, Khloud Shreif, WikiSysop, George Prudden and 127.0.0.1
Description[edit | edit source]
A syndesmosis is a complex fibrous joint between two bones and connected by ligaments and a strong membrane[1] with slightly movement allowed.
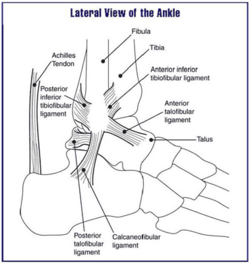
The distal tibiofibular syndesmosis/inferior tibiofibular joint is a syndesmotic joint. It is formed between the distal tibia(concave surface) and fibula(convex surface), with no articular capsule or synovial membrane as a fibrous joint, and attached by the interosseous ligament (IOL), the anterior-inferior tibiofibular ligament (AITFL), the posterior-inferior tibiofibular ligament (PITFL), and the transverse tibiofibular ligament (TTFL)[1][2].
Anatomy[edit | edit source]
Articulating Surfaces[edit | edit source]
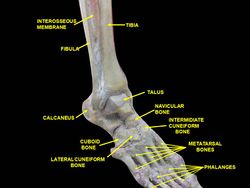
- Distal fibula (rough medial convex surface)
- Distal tibia (the triangular notch of the lateral surface)
The direct contact between the two bones at this site is very limtied, and this forms a mortise for the trochlea of the Talus.
Ligaments & Interosseus membrane[edit | edit source]
INTEROSSEUS MEMBRANE: spanning through the length of the tibia and the fibula.
Function:
- The inferior segment assists in stabilising the tibiofibular syndesmosis.
| LIGAMENTS | DESCRIPTION | PROXIMAL ATTACHMENT | DISTAL ATTACHMENT | ROLE / FUNCTION |
|---|---|---|---|---|
|
Anterior-inferior tibiofibular ligament (AITFL)[3] |
Trapezoid shape (the tibial insertion is wider) The ligament runs obliquely Weaker than the PITFL 20% intra-articular |
Anterior tubercle of the distal tibia | Anterior surface of the distal fibula at the lateral malleolus |
One of the primary stabilisers
|
|
Posterior or posterior-inferior tibiofibular ligament (PITFL) |
Strong compact ligament Known as the Superficial component of the PITFL |
Posterior edge of the lateral malleolus |
Posterior tibial tubercle |
One of the primary stabilisers Limits excessive:
|
|
Transverse ligament or the Transverse tibiofibular ligament (TTFL)
|
Cone shaped Also known as the Deep component of the PTIFL
|
Proximal area of the malleolar fossa | Posterior edge of the tibia -- directly posterior to the cartilaginous covering of the inferior tibial articular surface and may extent up to the medial malleolus |
Forms a true labrum Provides talocrural joint stability. Prevents Posterior translation |
|
Interosseus ligament or the interosseous tibiofibular ligament (IOL) |
Thickened portion of the distal interosseous membrane Dense mass of short fibers with adipose tissue and small branching vessels from the peroneal artery |
Span between the tibia and fibula
The most proximal fibres attach to the apex of the incisura tibialis on the tibia |
Most distal fibres attach to the anterior tubercle of the tibia and descends straight to the talocrural joint of the fibula The length of the fibres increase from proximal to distal |
One of the primary stabilisers Buffer to neutralise forces during weight bearing as it transfers some of the axial compressive load to the fibula 'Spring' action - allowing for minor separation between the distal tibia and fibula during dorsiflexion. Allowing slight wedging of the talus in the mortise |
There exists controversy in the literature if the TTFL and the PITFL are two components of one anatomical structure or two different structures[1].
Blood Supply[edit | edit source]
Anterior syndesmosis: supplied by branches of the tibial and peroneal artery.
Posterior syndesmosis: supplied by the peroneal artery. and in rare cases by branches from the tibial artery.
Function[edit | edit source]
The function of syndesmosis ligament complex:
- Provide strong stabilization and dynamic support to the ankle mortise
- Maintain the integrity between the distal tibia and fibula
- Resist forces (axial, rotational, and translational) that attempt to separate the two bones [2][5][4]
Motions Available[edit | edit source]
- 2° fibula external rotation relative to the tibia
- As the ankle joint moves from end range plantar flexion to end range dorsiflexion the ankle mortise widens only about 1mm[2].
Pathology/Injury[edit | edit source]
Injury to the syndesmotic joint is described in the literature as an injury to the syndesmotic ligaments[1].
Clinical conditions:
- High ankle sprain or syndesmotic ankle sprain (syndesmosis injury)
- AITFL injury is normally combined with a tear of the IOL.[2]
- Tibiofibular Diastasis
- Ankle fracture
- Syndesmotic Impingement (anterolateral soft tissue impingement)
- A fatty synovial fringe (small bundle of adipose tissue) moves during ankle movement. It rises during dorsiflexion and thus retracts between the tibia and the fibula and descends during plantarflexion thus lowering towards the ankle joint.
- May cause chronic pain after an ankle sprain.[4]
Examination[edit | edit source]
Examination of syndesmotic injuries or sprains.
Treatment[edit | edit source]
Treatment of syndesmotic injuries or sprains.
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 Hermans JJ, Beumer A, De Jong TA, Kleinrensink GJ. Anatomy of the distal tibiofibular syndesmosis in adults: a pictorial essay with a multimodality approach. Journal of anatomy. 2010 Dec 1;217(6):633-45.
- ↑ 2.0 2.1 2.2 2.3 2.4 Lin CF, Gross MT, Weinhold P. Ankle syndesmosis injuries: anatomy, biomechanics, mechanism of injury, and clinical guidelines for diagnosis and intervention. Journal of Orthopaedic&Sports Physical Therapy. 2006 Jun;36(6):372-84.
- ↑ Bartoníček J. Anatomy of the tibiofibular syndesmosis and its clinical relevance. Surgical and Radiologic anatomy. 2003 Dec 1;25(5-6):379-86.
- ↑ 4.0 4.1 4.2 4.3 Golanó P, Vega J, De Leeuw PA, Malagelada F, Manzanares MC, Götzens V, Van Dijk CN. Anatomy of the ankle ligaments: a pictorial essay. Knee Surgery, Sports Traumatology, Arthroscopy. 2010 May 1;18(5):557-69.
- ↑ 5.0 5.1 Ebraheim NA, Taser F, Shafiq Q, Yeasting RA. Anatomical evaluation and clinical importance of the tibiofibular syndesmosis ligaments. Surgical and Radiologic Anatomy. 2006 May 1;28(2):142-9.
- ↑ Dr Christoph Agten. MRI Anatomy of ankle ligaments: Syndesmosis. Available from: http://www.youtube.com/watch?v=sNcJfZhH64g[last accessed 6/3/2021]
</div>