Ankle and Foot Fractures
Original Editor - Andrea Nees as part of the Vrije Universiteit Brussel Evidence-Based Practice Project
Top Contributors - George Prudden, Kim Jackson, Andrea Nees, Eta Frida, Rachael Lowe, Rosie Swift, Admin, Aminat Abolade, WikiSysop, Luna Antonis, Scott Cornish, Haddad Yousri, Claire Knott, Wanda van Niekerk, 127.0.0.1, Carina Therese Magtibay, Evan Thomas and Karen Wilson
Description[edit | edit source]
A fracture is an interruption of the continuity of bone. This page will discuss ankle and foot fractures and the role that physiotherapists play in the rehabilitation of such injuries. Fractures of the ankle joint are common amongst adults. Kannus et al. report an incidence of up to 174 cases per 100 000 persons per year in a Finish population.[1] Fractures of the foot are less common.
Fractures of the ankle[edit | edit source]
Ankle fractures are most commonly diagnosed through clinical examination and x-ray. Ottawa rules provide clinicians with a tool to decide whether the joint should be imaged or not. Several classifications exist and are used to determine the severity of injury and management. Examples include the Danis-Weber classification which identifies the level of injury and; the Lauge-Hansen classification which is based on the mechanism of the injury which have predictable patterns and imaging findings.
Complications of ankle fractures can include reduced range of motion at the ankle and foot joints, as a result of peri-articular and intra-articular adhesions or disruption of articular surfaces. Disruption to articular surfaces may lead to the development of osteoarthritis.
Fractures without displacement can be treated with a below knee cast that may be applied for 3-6 weeks. If displaced, a surgeon should reduce the fragments to the normal anatomical position of the joint. If this cannot be achieved by manipulation and plaster cast, an individual may have to undergo an open reduction with internal fixation (ORIF) followed by immobilisation in a plaster cast.[2]
Common ankle fractures include:
Fractures in the foot[edit | edit source]
The bony anatomy of the foot means that a variety of fractures are possible. Fractures of the calcaneum often occur as a result of a fall from height. Such fractures can be very painful and may be accompanied by vertebral fractures. The phalanges and metatarsals are commonly injured by a heavy object falling onto the foot. These fractures do not require reduction or immobilisation. Stress fractures of the metatarsals are known as a 'march' fracture. These are caused by repeated trauma from prolonged walking.[2]
Common fractures of the foot include:
Stress Fractures[edit | edit source]
Stress fractures occur in bones that undergo mechanical fatigue.[3] They are a consequence of exceeding repetitive submaximal loads, which creates an imbalance between bone resorption and bone formation.[4] The fractures usually begin in locations of great stress; this is called “crack initiation”.[4] If this microscopic crack is not able to heal and is subjected to further loading, the microdamage will increase and the crack will enlarge. This increase in damage can cause the bone to break on a macroscopic level.[4]
Clinically Relevant Anatomy[edit | edit source]
The ankle joint[edit | edit source]
The ankle joint, also known as talocrural joint, is made up of three bony structures: the distal ends of the tibia (shinbone) and fibula, proximally and the talus, distally. The tibia and fibula have specific parts that make up the ankle:
- Medial malleolus - inside part of the tibia
- Posterior malleolus - back part of the tibia
- Lateral malleolus – end of the fibula
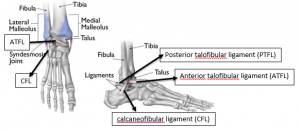
The tibia and fibula form the ankle joint with structure and stability provided by the following connective tissues:
- Interosseous membrane
- Anterior, posterior, and transverse tibiofibular ligaments
The collateral ligaments stabilize the joint against abduction and adduction forces. Laterally, the anterior talofibular ligament (ATFL), calcaneofibular ligament (CFL), and posterior talofibular ligament (PTFL), and, medially, the broad fan of the deltoid ligament and the plantar calcaneonavicular ligament, whose medial border is blended with the forepart of the deltoid ligament.[5]
The foot[edit | edit source]
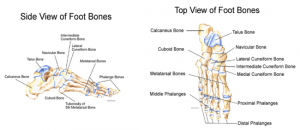
The foot contains 26 bones. The foot is divided into three main parts: hindfoot, midfoot and forefoot.
- Hindfoot is composed of 2 bones: calcaneus and talus. They form the subtalar joint.
- Midfoot is made up of 5 bones: navicular, cuboid and 3 cuneiforms (medial, intermediate and lateral). The bones are connected to the forefoot and the hindfoot by muscles and the plantar fascia (arch ligament).
- Forefoot consists of 19 bones: 5 metatarsals and 14 phalanges.
The Chopart joint is the connection between the hindfoot to the midfoot involving the ‘talonavicular joint’ and the ‘calcaneocuboid joint’; the Lisfranc joint connects the forefoot to the midfoot.
Epidemiology /Etiology[edit | edit source]
Ankle fracture is caused by traumas such as falls, twisting injuries and sports-related injuries[6]. It occurs in both older and younger populations.
There are a number of risk factors associated with an increased risk of sustaining foot and ankle fractures. These are: smoking, diabetes, obesity, previous falls and/or fractures, very high or low levels of physical activity, and low bone mineral density (BMD). For older individuals over an age of 50, additional risk factors include female gender, comorbidities and multiple medications.
The higher level of activity in younger males, particularly in risk taking and sports activities, might explain the high rates of ankle and foot fractures in this age group[7]. Younger females, under the age of 50, although less active than males have a higher tendency to fall, later in life which coincides with postmenopausal bone loss; this results in an increase in fracture risk.[7]
Characteristics/Clinical Presentation[edit | edit source]
- Difficulties or inability to walk/load the ankle (it is possible to walk with less severe breaks, so relying on walking as a test of whether a bone has been fractured is not reliable)
- Pain
- Swelling
- Bruising (soon after the injury)
- Difference in appearance
- Observable differences compared to the unaffected side
When an ankle has been broken, there is not only structural damage to the skeletal structure, but also to the ligaments (deltoid ligament and the anterior and posterior tibiofibular ligaments) and also nervous and musculoskeletal tissue around the ankle complex. This can result in impaired balance capacity, reduced joint position sense, slowed nerve conduction, velocity, impaired cutaneous sensation and decreased dorsal extension range of motion.[6]
Fracture Classifications [edit | edit source]
Ankle fractures can be classified according to either the AO/OTA, Danis-Weber or Lauge-Hansen classification system.
The Lauge-Hansen classification is based on a rotational mechanism of injury. There are 4 categories and 13 subgroups of ankle fractures detailed in the table below.
| Categories | Stage (subgroups) |
| Supination external rotation (SER) | 1. Injury of the anterior inferior tibiofibular ligament 2. Oblique/spiral fracture of the distal fibula 3. Injury of the posterior inferior tibiofibular ligament or avulsion of the posterior malleolus 4. Medial malleolus fracture or injury to the deltoid ligament |
| Supination adduction (SA) | 1. Transverse fracture of the distal fibula 2. Vertical fracture of the medial malleolus |
| Pronation external rotation (PER) | 1. Medial malleolus fracture or injury to the deltoid ligament 2. Injury of the anterior inferior tibiofibular ligament 3. Oblique/spiral fracture of the fibula proximal to the tibial plafond 4. Injury of the posterior inferior tibiofibular ligament or avulsion of the posterior malleolus |
| Pronation abduction (PA) | 1. Medial malleolus fracture or injury to the deltoid ligament 2. Injury of the anterior inferior tibiofibular ligament 3. Transverse or comminuted fracture of the fibula proximal to the tibial plafond |
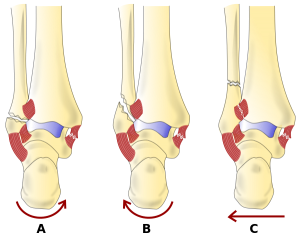
The Danis-Weber classification is based on radiographic criteria. It took into consideration the position of the distal fibular fracture in relation to the syndesmosis of the ankle joint. Three categories were created:
- Type A fracture: below the level of the tibial plafond (syndesmosis) and may be associated with oblique or vertical medial malleolar fractures
- Type B fractures: at the level of the tibial plafond (syndesmosis) and extend proximally in an oblique fashion
- Type C fractures: proximal to the level of the tibial plafond and often have an associated syndesmotic injury. It can be associated with medial malleolus fractures or injury to the deltoid ligament.[5][8]
AO classification/OTA system classifies all long bone fractures with a systematic approach, based on location, topography, and extent of bony lesion. It is based on radiographic criteria and incorporates the mechanism of injury. The fractures are classified as infrasyndesmotic, transsyndesmotic and suprasyndesmotic with further subcategories based on the presence or absence of medial or posterior malleolar injuries.
The AO and Lauge-Hansen classification systems are widely used in the clinical diagnosis of ankle injuries. The AO classification system is simple to understand, and it emphasizes the coordinating role of the fibula and syndesmosis of the ankle joint. The Lauge-Hansen classification system emphasizes the different stages of pathological damage in addition to the fracture pattern, and it insists on the understanding of damage to the ankle ligament system. It can provide an extensive assessment of ankle injuries.
Compared to Lauge-Hansen classification, AO classification system is more reliable and reproducible and thus has more value in clinical practice. Despite this, the Lauge-Hansen classification system stands as the basis for understanding the mechanics of ankle fractures.[9]
The table below compares the Danis-Weber, Lauge-Hansen, and AO/OTA classification systems.
|
Fibular fracture location |
Danis-Weber classification
|
Lauge-Hansen classification SAD I, II
|
AO/OTA classification of tibial malleolar fractures |
| Infrasyndesmotic | Type A | SAD I, II | 44-A1 (isolated lateral) 44-A2 (lateral and medial) 44-A3 (lateral, medial, and posterior) |
| Transsyndesmotic | Type B | SER I, II, III, IV | 44-B1 (isolated lateral) 44-B2 (lateral and medial) 44-B3 (lateral, medial, and Volkmann’s fracture) |
| Suprasyndesmotic | Type C |
PER I, II, III, IV PA I, II, III |
44-C1 (simple diaphyseal) 44-C2 (multifragmentary) 44-C3 (proximal |
OTA = Orthopaedic Trauma Association; SAD = supination adduction; SER = supination external rotation; PER = pronation external rotation; PA = pronation abduction.[8]
Differential Diagnosis[edit | edit source]
- Rheumatoid Arthritis
- Gout and Pseudogout
- Ankle Dislocation
- Ankle Impingement
- Compartment Syndrome of the Foot
- Deep Venous Thrombosis
- Peroneal Tendinopathy
- Sinus Tarsi Syndrome
- Ankle ligament sprains
The clinical presentation of some subtle fractures of the ankle can be similar to that of ankle sprains. This similarity makes that ankle fracture is often mistaken as ankle sprain. These injuries are quite different and need an accurate and early diagnosis.[10]
Diagnostic Procedures[edit | edit source]
Ottawa rules[edit | edit source]
Ankle X-ray is only required if there is any pain in the malleolar zone and any one of the following:
- Bone tenderness along the distal 6 cm of the posterior edge of the tibia or tip of the medial malleolus, OR
- Bone tenderness along the distal 6 cm of the posterior edge of the fibula or tip of the lateral malleolus, OR
- An inability to bear weight both immediately and in the emergency department for four steps.
Additionally, the Ottawa ankle rules indicate whether a foot X-ray series is required. It states that it is indicated if there is any pain in the midfoot zone and any one of the following:
- Bone tenderness at the base of the fifth metatarsal (for foot injuries), OR
- Bone tenderness at the navicular bone (for foot injuries), OR
- An inability to bear weight both immediately and in the emergency department for four steps.
Ankle fractures are initially evaluated by physical examination and then by x-ray.[5]
To reduce the use of x-rays, an infrasound device can be used to detect malleolar fractures even though it cannot be relied upon alone due to an 85% sensitivity and 52% sensitivity.[11]
Ultrasound had good sensitivity and specificity for diagnosing fifth metatarsal, lateral and medial malleolus fractures in patients with foot and/or ankle sprains. However, sensitivity and specificity of ultrasound for navicular fractures were low.[8]
Imaging[edit | edit source]
Outcomes Measures[edit | edit source]
- SF-36 includes 8 categories: Physical functioning, Physical role, Bodily pain, General health, Vitality, Social functioning, Emotional role and Mental health)[12]
- Kerr-Atkins score for pain and function after calcaneal fracture leading to a best score of 100points.[6]
- EuroQol (EQ-5D) to measure the Quality of life and general health status[6]
- American Orthopaedic Foot and Ankle Society score based on 9 items: pain, activity and functional limitations, walking distance, difficulties with different terrains, gait abnormality, sagittal range of motion at the ankle and range of motion at the subtalar joint, stability, and alignment[13]
- Olerud-Molander Ankle Score (OMAS), is an ordinal rating scale from 0 points (totally impaired function) to 100 points (completely unimpaired function) related to 9 different items given different points: pain, stiffness, swelling, stair climbing, running, jumping, squatting, supports and work/activity level.[14]
- FAOS is also a self-administered patient questionnaire and consists of 42 items divided into five subscales: pain, other symptoms, function in daily living (ADL), function in sport + recreation + foot and ankle-related quality of life.[14]
- Global self-rated ankle (GSRF) to evaluate their present ankle function[14]
- The American Orthopaedic Foot and Ankle Society Hindfoot score (AOFAS) score contains 3 components: pain (40 points), function and alignment on a scale of 0- 100 points, 100 best possible score[7]
- Foot Function Index (FFI) consists of 23 questions to measure the impact of foot pathology on function in terms of pain, disability and restriction of activity. The lower the score, the better outcome[7]
Medical Management[edit | edit source]
Most patients with a malleolus fracture require 6 weeks of immobilisation. Patients with an initially non-displaced fracture or who were treated surgically will generally require 4 weeks of non-weight bearing in a short-leg cast or removable walking boot, followed by 2 weeks in a walking cast or boot. The removable boot will allow for earlier range-of-motion exercises.
Surgery is needed for many types of ankle fractures. While not always necessary, surgery for ankle fractures is not uncommon. The need for surgery depends on the appearance of the ankle joint on X-ray and the type of ankle fracture.
The goals of surgery are to achieve the smooth anatomical reconstruction of the joint surface and the protection of the injured ligamentous structures to enable early postoperative functional therapy of the joint. Adequate reduction with congruency of the joint has been reported as one of the most important indications of a good end result. Inadequate reduction may lead to osteoarthritis.
The timing of definitive surgical treatment depends mainly on the soft-tissue finding and is possible only if the soft tissues are not critically vulnerable (few hours after the trauma). The need for surgery depends on the appearance of the ankle joint on X-ray and the type of ankle fracture.
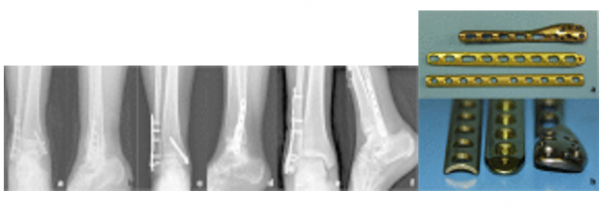
While not always necessary, surgery for ankle fractures can be done with 3 kinds of metal plate and multiple screws: one-third tubular plate; locking compression (LCP) metaphyseal plate for lateral malleolar fracture and Weber B fracture; LCP distal fibula plate Weber A fracture and Weber B fracture.[5][15]
Physical Therapy Management[edit | edit source]
Fractures that are stable with non-displaced or only slightly displaced fragments can be treated conservatively. Type A fractures do not need to be immobilised in a cast, but can rather be treated like external ligament ruptures in a stabilising ankle orthosis for early function with pain-adapted full weight-bearing.[5]
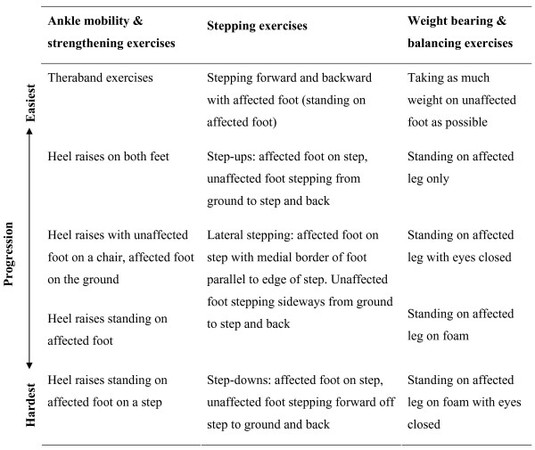
More significant fractures are immobilised and require a rehabilitation program after cast removal. Programs should be patient centred and take into consideration patient goals and aspirations. Programs tend to include ankle mobility, strengthening exercise, weight bearing and balancing exercise. Physiotherapists should empower the patient with home exercises and provide education and advice.[6]
Patients frequently complain of difficulties with activities involving the lower limb, such as stair climbing, walking and reduced participation in work and recreation. Impairments can be pain, swelling, stiffness, muscle atrophy and decreased muscle torque[9], impaired ankle mobility, impaired balance capacity and increased ankle circumference[6]at the ankle after cast removal.
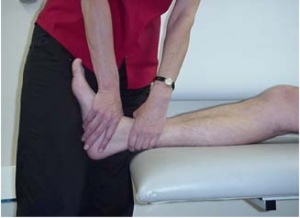
Passive joint mobilisation can be used to work on the problems of pain and joint stiffness, in order to allow an earlier return to activities. For this technique, the physiotherapist manually glides the articular surfaces of a joint to produce oscillatory movements[16] . Manual techniques should be complimentary to a program that includes active exercise.
Strength-training may be beneficial after fracture and should be considered as an important rehabilitation option by physiotherapy. Because strength loss is one of the most common complications by a foot or ankle fracture.[17]
Key Research[edit | edit source]
- Fractures of the Ankle Joint: Investigation and Treatment Options.[5]
- Accuracy of Ottawa ankle rules to exclude fractures of the ankle and mid-foot: systematic review.[18]
Resources[edit | edit source]
- Orthopaedic Surgery ucsf. Ankle Physical Examination. http://orthosurg.ucsf.edu/oti/patient-care/divisions/sports-medicine/physical-examination-info/ankle-physical-examination/ (accessed 24 Aug 2014).
References [edit | edit source]
- ↑ Kannus P, Palvanen M, Niemi S, Parkkari J, Jrvinen M. Increasing number and incidence of low-trauma ankle fractures in elderly people: Finnish statistics during 1970–2000 and projections for the future. Bone. 2002 Sep 1;31(3):430-3.
- ↑ 2.0 2.1 Tidy N, Porter S. Tidy's physiotherapy. 13th ed. Edinburgh: Elsevier; 2013.
- ↑ Edwards WB, Taylor D, Rudolphi TJ, Gillette JC, Derrick TR. Effects of running speed on a probabilistic stress fracture model. Clinical Biomechanics. 2010 May 1;25(4):372-7.
- ↑ 4.0 4.1 4.2 Maffulli N, Longo UG, Denaro V. Femoral Neck Stress Fractures. Operative Techniques in Sports Medicine. 2009;17:90-93.
- ↑ 5.0 5.1 5.2 5.3 5.4 5.5 Goost H, Wimmer MD, Barg A, Kabir K, Valderrabano V, Burger C. Fractures of the ankle joint: investigation and treatment options. Deutsches Ärzteblatt International. 2014 May;111(21):377.
- ↑ 6.0 6.1 6.2 6.3 6.4 6.5 Daly PJ, Fitzgerald RH, Melton LJ, Llstrup DM. Epidemiology of ankle fractures in Rochester, Minnesota. Acta Orthopaedica Scandinavica. 1987 Jan 1;58(5):539-44.
- ↑ 7.0 7.1 7.2 7.3 Holloway KL et al. Foot and Ankle Fracture Incidence in South-Eastern Australia: An Epidemiological Study. Clin Res Foot Ankle 2014, 2:4
- ↑ 8.0 8.1 8.2 Tartaglione JP, Rosenbaum AJ, Abousayed M, DiPreta JA. Classifications in brief: Lauge-Hansen classification of ankle fractures.
- ↑ 9.0 9.1 Yin MC, Yuan XF, Ma JM, Xia Y, Wang T, Xu XL, Yan YJ, Xu JH, Ye J, Tong ZY, Feng YQ. Evaluating the reliability and reproducibility of the AO and Lauge-Hansen classification systems for ankle injuries. Orthopedics. 2015 Jul 1;38(7):e626-30.
- ↑ Judd D, Kim D. Foot Fractures That Are Frequently Misdiagnosed As Ankle Sprains. American family physician. 2002 Sep 1;66(5):785.
- ↑ Dancocks A, Rouse A, Hiscox J. A pilot study to assess the sensitivity and specificity of an intrasound device in the diagnosis of ankle fractures. Emergency Medicine Journal. 1997 Jul 1;14(4):230-2.
- ↑ Westphal T, Piatek S, Halm JP, Schubert S, Winckler S. Outcome of surgically treated intraarticular calcaneus fractures—SF-36 compared with AOFAS and MFS. Acta orthopaedica Scandinavica. 2004 Jan 1;75(6):750-5.
- ↑ Schie-Van der Weert V, Van Lieshout EM, De Vries MR, Van der Elst M, Schepers T. Determinants of outcome in operatively and non-operatively treated Weber-B ankle fractures. Archives of orthopaedic and trauma surgery. 2012 Feb;132(2):257-63.
- ↑ 14.0 14.1 14.2 Nilsson GM, Eneroth M, Ekdahl CS. The Swedish version of OMAS is a reliable and valid outcome measure for patients with ankle fractures. BMC musculoskeletal disorders. 2013 Dec;14(1):1-8.
- ↑ Huang Z, Liu L, Tu C, Zhang H, Fang Y, Yang T, Pei F. Comparison of three plate system for lateral malleolar fixation. BMC Musculoskeletal Disorders. 2014 Dec;15(1):1-9.
- ↑ Lin CC, Moseley AM, Refshauge KM, Haas M, Herbert RD. Effectiveness of joint mobilisation after cast immobilisation for ankle fracture: a protocol for a randomised controlled trial [ACTRN012605000143628]. BMC Musculoskeletal Disorders. 2006 Dec;7(1):1-0.
- ↑ Murdoch A, Taylor N, Dodd K. Physical therapists should consider including strength training as part of fracture rehabilitation. Physical therapy reviews. 2004 Mar 1;9(1):51-9.
- ↑ Bachmann LM, Kolb E, Koller MT, Steurer J, ter Riet G. Accuracy of Ottawa ankle rules to exclude fractures of the ankle and mid-foot: systematic review. Bmj. 2003 Feb 22;326(7386):417.