Diabetes Mellitus Type 1
Original Editors - Collen Nalley and Abbye Senn from Bellarmine University's Pathophysiology of Complex Patient Problems project.
Top Contributors - Abbye Senn, Colleen Nalley, Lucinda hampton, Rachael Lowe, Elaine Lonnemann, Vidya Acharya, Amanda Ager, Evan Thomas, WikiSysop, Fasuba Ayobami and Kim Jackson
Definition/Description[edit | edit source]
Type 1 diabetes mellitus (T1DM) is an autoimmune disease that leads to the destruction of insulin-producing pancreatic beta cells.
Insulin: is an essential anabolic hormone that exerts multiple effects on glucose, lipid, protein, and mineral metabolism, as well as growth; importantly, insulin allows glucose to enter muscle and adipose cells, stimulates the liver to store glucose as glycogen and synthesize fatty acids, stimulates the uptake of amino acids, inhibits the breakdown of fat in adipose tissue, and stimulates the uptake of potassium into cells.
Individuals with type 1 diabetes mellitus require life-long insulin replacement therapy. Without insulin, diabetic ketoacidosis (DKA) develops and is life-threatening[1].
(T1DM) can result in serious vascular complications and neuropathies and can be a major cause of cardiovascular disease and strokes. It is also the leading cause of end-stage renal (kidney) disease, non-traumatic amputations in the lower extremity, and new cases of blindness.[2].
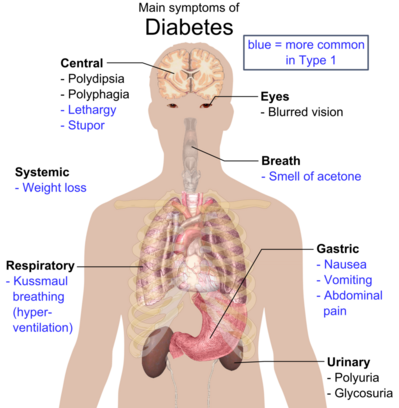
Image 1: Overview of possible symptoms of diabetes
Etiology[edit | edit source]
In T1DM, there is the immune destruction of the beta cells in the pancreatic islets over months or years, causing an absolute deficiency of insulin. Although the exact etiology of T1DM is still unknown, researchers believe there is a genetic predisposition.
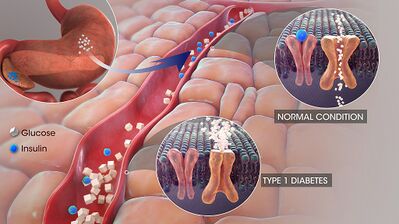
Image 2: 3D medical animation still of Type 1 Diabetes showing lower amount of insulin production in a diabetic patient.
- In those at risk, it is generally believed that a virus or other environmental factors trigger the autoimmune beta-cell destruction. Some studies have found an increased development of T1DM in children born to a mother that had Coxsackievirus or another Enterovirus during pregnancy.
- Environmental toxins have also been postulated to play a role. The hygiene hypothesis suggests that improved sanitation relates to the increased development of autoimmune-mediated disorders. It is proposed that the reduction of childhood exposure to infectious agents leads to the lack of proper immune system development.
- Dietary factors have also been examined as potential triggers[1].
Epidemiology[edit | edit source]
T1DM is one of the most frequent chronic diseases in children but can start at any age. There has been a steady increase in the incidence and prevalence of T1DM, representing approximately 5% to 10% of people with diabetes.
- In the United States, there are an estimated 1.24 million people with T1DM, and that number is expected to grow to 5 million by 2050.
- Worldwide, there is also a considerable geographic variation in incidence. The highest reported incidences are in Finland and other Northern European nations with rates approximately 400-times greater than those seen in China and Venezuela[1].
Characteristics/Clinical Presentation[edit | edit source]
Symptoms for type 1 diabetes can include:
- Extreme thirst
- Frequent urination
- Sudden unexplained weight loss
- Extreme fatigue and weakness
- Blurred vision
- Nausea and vomiting
- Constant hunger
Image 3: Overview of the most significant possible symptoms of diabetes
The 4 T’s: A simple way to remember the four main symptoms of type 1 diabetes.
- Tiredness
- Toilet
- Thinner
- Thirsty[3]
Associated Co-morbidities[edit | edit source]
- Neuropathy
- Nephropathy
- Retinopathy
- Cardiomyopathy
- Hypoglycemia
- Diabetic ketoacidosis
- Diabetic foot disease[1]
- Amputation
Diagnostic Tests[edit | edit source]
- Fasting plasma glucose (FPG) ≥ 126 mg/dl on two different days
- A1C Levels≥ 6.5 % on two separate occasions (but must be confirmed by FPG)
- Oral glucose tolerance test ≥ 200 mg/dl
Other Information: [2]
- FPG >100mg/dl is a risk factor for future diabetes
- A1C is a measure of how diet, exercise, and/or medication/insulin have been controlling glucose over a period of time
- Normal FPG= 80-120 mg/dl
- Want to keep A1C levels below 7%
- If A1C is >10%=medical attention immediately
Management[edit | edit source]
Type 1 diabetes is a life threatening condition which needs to be closely managed with daily care. Type 1 diabetes is managed with:
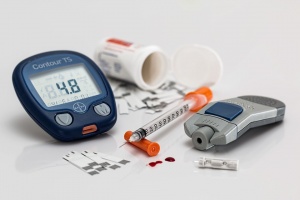
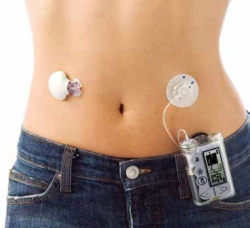
- Insulin replacement through lifelong insulin injections (up to 6 every day) or use of an insulin pump
- Monitoring of blood glucose levels regularly (up to 6 times every day or as directed by a doctor or Credentialled Diabetes Educator)
- Following a healthy diet and eating plan
- Taking regular exercise
The aim diabetes management is to keep blood glucose levels as close to the target range as possible, between 4 to 6 mmol/L (fasting). However, the ranges will vary depending on the individual and an individual’s circumstances.
Keeping blood glucose level at the optimum range is a careful balance between what food is eaten, physical activity and medication. Blood glucose levels which are too high, could result in hyperglycaemia or ketoacidosis. Blood glucose levels which are too low, could result in hypoglycaemia.
Monitoring of blood glucose levels should occur throughout the day and even at night. Keeping blood glucose levels on target will help prevent both short-term and long-term complications.[5]
Physical Therapy Management[edit | edit source]
Physiotherapists should play a role in education re exercise
Regular exercise is an important part of diabetes management. It helps insulin to work more efficiently and assist with blood glucose control. If client has fluctuating or high blood glucose levels (i.e. fasting blood glucose levels greater than 14 mmol/L and urinary ketones), it is best to avoid exercise until blood glucose has settled. Exercise in these circumstances can actually elevate blood glucose and increase ketone production[5].
If client has any diabetes complications (eg retinopathy, nephropathy) you should assess individually and advise appropriately re exercise. Screen for reflexes, sensation in feet, questions about neuropathic symptoms, foot ulcers, calluses, etc[2]
Exercise Specific Education
- Amount of exercise: For good health, you should be doing about 30 minutes of exercise every day. If this is not possible, then this time can be divided in 3 x 10 minutes sessions. You can break up exercise throughout the day. If you need to lose weight, 45-60 minutes everyday.
- Intensity of exercise: Aim for moderate intensity. This means you should still be able to talk as you exercise without becoming breathless.
- Taking care of feet: Ulcers or other lesions on the feet are a serious danger for people with diabetes. It is important to avoid foot damage especially for middle-aged and elderly people. Always inspect your feet before and after exercise. Avoid exercise that causes stress to the feet (e.g. running). Exercise which poses minimal weight or stress on the feet is ideal such as riding an exercise bike or brisk walking in good footwear. Wear comfortable and well-fitting shoes.
Exercise tips
- Drink extra fluid before, during (only if prolonged exercise) and after exercise to avoid dehydration. The fluid may be water or a sweetened drink if extra carbohydrate is required. 250 ml every 15 minutes or one litre of fluid per hour is recommended.
- Take extra carbohydrate before and during exercise to prevent hypoglycaemia. Extra carbohydrate is often needed after exercise. Discuss adjusting carbohydrate intake with your doctor or dietitian.
- Monitor your blood glucose levels before, if possible during (at least initially), and after exercise to assess your requirements for extra food.
- It may be necessary to reduce your insulin dose prior to exercise. Insulin adjustment varies with each individual. Discuss appropriate adjustments to suit your exercise schedule with your doctor or Credentialed Diabetes Educator.
- Wear sun block when exercising outdoors.
People with diabetes are discouraged from strenuous physical activity if they feel unwell or have ketones present in their blood or urine[5].
Important considerations:[edit | edit source]
- Type 1 diabetics may need to decrease insulin dose or pump activity during exercise, as well as increase food intake, with prolonged activities (10-15g CHO with every 30 min. of exercise).[6]
- Exercise increases insulin, which can drop glucose levels to low dangerous ranges, especially with high intensity or prolonged duration exercise. Monitor glucose levels before, during, and after exercise. A randomized controlled trial[7] shows that the 6-week high-intensity interval training (HIIT) program was safe in people with T1DM as no severe hypoglycemia was reported. And it was effective in improving well-being and exercise adherence in the previously inactive T1DM population as the health-related quality of life, sleep quality, exercise motivation, and enjoyment showed better results in the study.
- Watch for confused, lethargic state or change in mental status in DM patient - have patient do finger stick check for glucose levels if available and immediately refer to physician. If patient has an insulin pump, diabetic ketoacidosis (DK) can occur quicker if there is an interruption in insulin delivery. Monitor patient carefully for excess perspiration, increased motion at pump site, and temperature during exercise.
Watch for signs and symptoms of life threatening conditions: Hyperglycemia, Diabetic Ketoacidosis; Hypoglycemia.
Blood glucose levels in relation to exercise that a PT should be aware of:
- <100 mg/dL= give 10-15 g CHO snack and retest glucose levels 15 minutes later
- 100-250 mg/dL= safe exercise levels; proceed with treatment
- 250-300 mg/dL @ start of exercise="caution zone"; postpone exercise until stable levels are achieved; ketones in urine are checked for at these levels
- >300 mg/dL= stop exercise immediately!!!! (NOT SAFE)
Prognosis[edit | edit source]
Type 1 DM is associated with high morbidity and mortality. Close to 50% of patients will develop a serious complication over the lifetime. Some will lose eyesight, and others will develop end-stage renal disease. For those who make it past the first 20 years, the prognosis is good. However, the disease has no cure, and with time, the patient may develop premature coronary artery disease, neuropathy, foot ulcers, and vision loss.
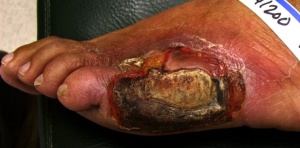
Image: Diabetic foot ulcer
Maintaining euglycemia for a lifetime is associated with severe anxiety and depression; for many patients with type 1 diabetes, the quality of life is poor.[1]See Diabetes HRQOL
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 Lucier J, Weinstock RS, Doerr C. Diabetes Mellitus Type 1 (Nursing).2021 Available: https://www.ncbi.nlm.nih.gov/books/NBK507713/ (accessed 28.9.2021)
- ↑ 2.0 2.1 2.2 2.3 Goodman CC, Snyder TEK. Differential Diagnosis for Physical Therapists: Screening for Referral. 5th ed. St. Louis, MO: Saunders/Elsevier; 2013: 425-432.
- ↑ Diabetes SA Diabetes type 1 Available: https://www.diabetessa.com.au/Web/Signs_and_Symptoms/Type_1_Diabetes/Web/Signs_and_Symptoms/Type_1_Diabetes.aspx?hkey=d13c6e40-3678-4d80-b99d-2be4bba77188 (accessed 28.9.2021)
- ↑ American Diabetes Association. Type 1 Diabetes. Available from: http://www.diabetes.org/diabetes-basics/type-1/?loc=util-header_type1 (accessed 8 April 2016).
- ↑ 5.0 5.1 5.2 Diabetes aus. Diabetes type 1 Available:https://www.diabetesaustralia.com.au/living-with-diabetes/managing-your-diabetes/managing-type-1/ (accessed 28.9.2021)
- ↑ Franc S, et al. Insulin-based strategies to prevent hypoglycaemia during and after exercise in adult patients with type 1 diabetes on pump therapy: the DIABRASPORT randomized study. Diabetes, Obesity, and Metabolism 2016; 12. http://www.ncbi.nlm.nih.gov/pubmed/26264812 (accessed 7 April 2016).
- ↑ Alarcón-Gómez J, Chulvi-Medrano I, Martin-Rivera F, Calatayud J. Effect of High-Intensity Interval Training on Quality of Life, Sleep Quality, Exercise Motivation and Enjoyment in Sedentary People with Type 1 Diabetes Mellitus. International Journal of Environmental Research and Public Health. 2021 Jan;18(23):12612.