Classification of Traumatic Brain Injury
Original Editor - Anna Ziemer
Top Contributors - Naomi O'Reilly, Kim Jackson, Simisola Ajeyalemi, Lucinda hampton, Stacy Schiurring, Wendy Walker, Uchechukwu Chukwuemeka, Nicole Hills, Olajumoke Ogunleye and Nupur Smit Shah
Introduction[edit | edit source]
There are various classification determinants utilized to classify traumatic brain injury (TBI). The clinical presentation and prognosis depend on the individual nature of the injury with often coexisting types of traumatic brain injury. The classification is important for acute management, treatment, and prognosis as well as neurorehabilitation requirements. [1]
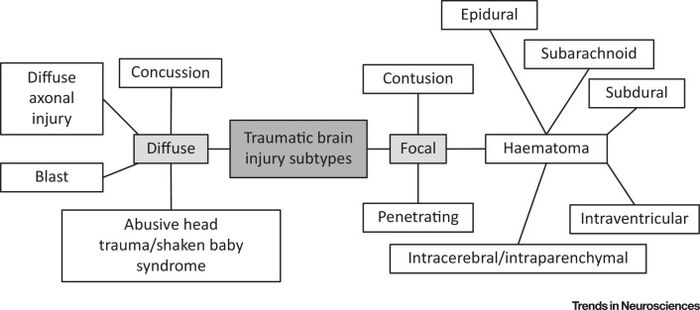
5 Classification determinants are detailed below.
1.Primary v Secondary Injuries[edit | edit source]
Dependant on the timing and impact nature, ie. mechanical or non-mechanical, and accompanying pathophysiological processes.
Primary Injury[edit | edit source]
Occurs at the time of injury and is induced by mechanical forces. Two main mechanisms that cause primary injury are:
- Contact i.e. an object striking the head or the brain striking the inside of the skull
- Acceleration - Deceleration.
Primary injury due to acceleration-deceleration results from unrestricted movement of the head and leads to shear, tensile, and compressive strains. These forces can cause intran acranial hematoma, diffuse vascular injury, and injury to cranial nerves and the pituitary stalk. [5]
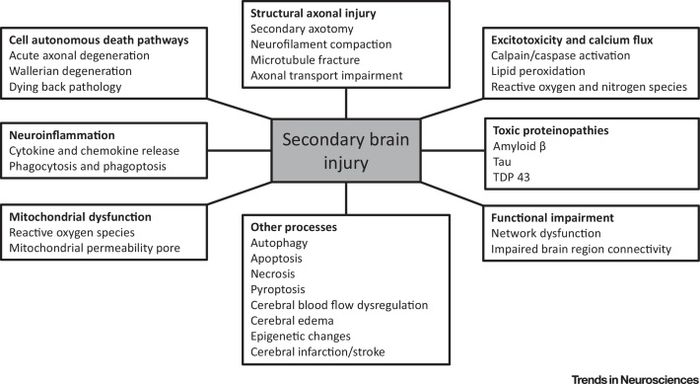
Secondary Injury[edit | edit source]
A secondary injury is not mechanically induced. It may be delayed from the moment of impact, and it may superimpose injury on a brain already affected by a mechanical injury. [5] The secondary damage is caused by casa cade of processes impacting “cerebral blood flow (hyper or hypoperfusion), impaired cerebrovascular autoregulation, cerebral metabolic dysfunction an,d impaired cerebral oxygenation.” [6] The ischemia and oedema are secondary injury types. See Pathophysiology
The outcome of a head injury is determined by the above types, with primary injury extent being only sensitive to preventative measures, and secondary injury extend being susceptible to neuroprotective therapeutic interventions.
2.Focal v Diffuse Injuries[edit | edit source]
Focal Injury[edit | edit source]
Usually due to contact and causing scalp injury, it might present as skull fracture, contusions and/or intracranial haemorrhage. Those injuries are detectable by CT, MRI or PET scans. Contusions are the bleeding on the brain and include fracture contusion, coup contusion (at the site of the impact) and contrecoup contusion (directly opposite to the impact site). This mechanism is related to the moving of intracranial content in the skull and impinging on in the internal surface of the skull. Commonly observed injury is coup-contrecoup injury presenting with a contusion on opposite sides of the brain.
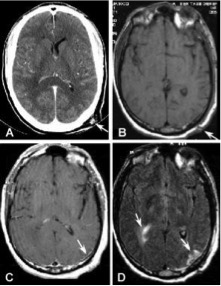
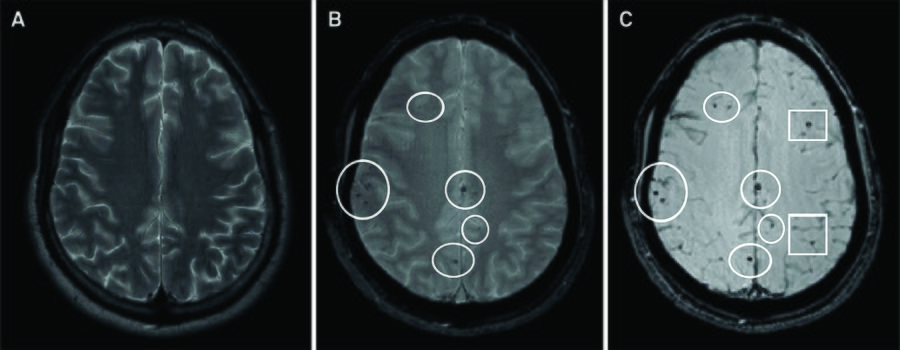
Diffuse Injury[edit | edit source]
Usually due to acceleration/deceleration injury and concussion resulting in diffuse axonal injury (DAI) and brain swelling. A diffuse axonal injury is difficult to diagnose with commonly available CT or MRI scans, and is demonstrated by histological white matter injury of the cerebral hemispheres, the corpus callosum, the brain stem and, less commonly, the cerebellum. A diffuse axonal injury might be accompanied by some focal lesions, but again only diagnosable microscopically. The tearing of the nerve tissue disrupts the brain’s regular communication metabolic processes. This disturbance in the brain can produce temporary or permanent widespread brain damage, coma, or death. The shaken baby syndrome is a type of diffuse axonal injury. These injuries are commonly found together.
3. Opened v Closed Injuries[edit | edit source]
Open / Penetrating Injury[edit | edit source]
Open/ Penetrating Injury occurs from the impact of a bullet, knife, or other sharp object that forces hair, skin, bone, and fragments from the object into the brain and dura mater is breached. The area of damage is determined by the trajectory of the object and possible ricocheting when travelling through different density tissues (i.e., skull compared to the brain). A "through-and-through" injury occurs when an object enters the skull, goes through the brain, and exits the skull and has a complex impact on the brain tissue with penetration injuries, additional shearing, stretching, and rupture of brain tissue.
Closed / Non-Penetrating Injury[edit | edit source]
A closed injury is an injury to the brain caused by an outside force without any penetration of the skull. The most serious complication is the brain oedema within constrained space of the skull and resultant increase in the intracranial pressure and compression of brain structures and cranial nerves.
4. Degree of Severity[edit | edit source]
TBI degree of severity assessment can be context dependent, subjective, and are influenced by the point-of-view and experience of the clinical assessor. This situation is not unique to the TBI diagnosis. However, the assessed degree of severity can effect a person with TBI's available rehabilitation and assistance resources[10].
Examples of differing viewpoints of TBI severity:[10]
- acute risk of death
- quantifying brain biomarker efflux
- risk/need for neurosurgical measures
- level of treatment/care needed (home, emergency department, intensive care unit, etc)
- duration of hospital stay
- outcome at the end of hospital stay
- quantification of brain tissue injury
- functional/vocational recovery
- person's level of independence as an outcome
- subjective symptoms as an outcome
- quality of life as an outcome
Mild, Moderate, or Severe Traumatic Brain Injury depending on degrees of severity. Mild traumatic brain injury may affect the brain cells temporarily, but more serious injuries can result in long-term complications or death.
A study published in 2021 investigated the classification of assessment and management of concussion and mild TBI and found that these diagnoses present on a spectrum and cannot be applied in a binary way. Further study and research into new classification methods involving dynamic risk profiles may provide more precise treatment targets[11]. A 2020 study states that the term ‘concussion’ is commonly used to describe a patient's clinical presentation, but does not identify the underlying pathological process. Based on this line of reasoning, concussion cannot be considered a true diagnosis. However, there is growing evidence of diffuse axonal injury as a likely pathological substrate for concussion, thereby providing a framework to develop true diagnostic criteria. Further research is indicated[12].
Measures of Severity[edit | edit source]
The main measures of severity used to classify the injury include:
- Glasgow Coma Scale (GCS): is a point scale used to assess a patient's level of consciousness and neurological functioning after brain injury. The scoring is based on the best eye-opening response (1-4 points), best motor response (1-6points) and best verbal response (1-5 points) with the cutoff point for coma at 8 points. For more in-depth information see GCS student’s guide
Duration of Loss of Consciousness[edit | edit source]
Describing alteration in consciousness duration:
- Mild (mental status change or loss of consciousness [LOC] < 30 min),
- Moderate (mental status change or LOC 30 min to 6 hr),
- Severe (mental status change or LOC > 6 hr)
Post-traumatic Amnesia (PTA)[edit | edit source]
Post-traumatic Amnesia is described by the time elapsed from injury to the moment when patient presents with continuous memory of what is happening around them.
Overview of Classification Criteria for traumatic brain injury severity based on Glasgow Coma Scale, Loss of Consciousness, Post-traumatic Amnesia and structural imaging:
| Severity | GCS | Loss of Consciousness | Structural Imaging |
|---|---|---|---|
| Mild | 13 - 15 | < 20 min to 1 Hour | Definition Dependant |
| Moderate | 9 - 12 | 1 hour to 24 Hours | Normal or Abnormal |
| Severe | 3 - 8 | > 24 Hours | Normal or Abnormal |
5. Symptoms[edit | edit source]
Traumatic brain injury can have wide-ranging physical, cognitive, psychological and physiological effects occurring immediately or elapsed. The symptoms might differ depending on the severity of TBI, but some are not specific to the type of injury.
Mild Traumatic Brain Injury[edit | edit source]
| Physical Symptoms | Sensory Symptoms | Cognitive Symptoms |
|---|---|---|
| With or without loss of consciousness. If loss of consciousness: a few seconds to a few minutes | Blurred Vision | State of being dazed, confused or disoriented |
| Headache | Ringing in the Ears | Memory or concentration deficits |
| Nausea or Vomiting | Bad taste in the mouth or changes in the ability to smell | Mood changes or mood swings |
| Fatigue or Drowsiness | Sensitivity to light or sound | Irritability |
| Problems with speech | Feeling depressed or anxious | |
| Difficulty sleeping or sleeping more than usually | Fatiguability | |
| Dizziness or loss of balance |
Moderate to Severe Traumatic Brain Injury[edit | edit source]
| Physical Symptoms | Sensory Symptoms | Cognitive Symptoms |
|---|---|---|
| Loss of consciousness from several minutes to hours or days | Blurred vision | Coma and other disorders of consciousness |
| Persistent headache or headache that worsens | Double vision | Profound confusion |
| Repeated vomiting or nausea | Ringing in the ears | Irritability |
| Convulsions or seizures | Bad taste in the mouth or changes in the ability to smell | Agitation, combativeness or other unusual behaviour |
| Dilation of one or both pupils of the eyes | Sensitivity to light or sound | Sad or depressed mood |
| Clear fluid or blood draining from the nose or ears | Fatiguability | |
| Sudden swelling or bruises behind the ears or around eyes | ||
| Inability to awaken from sleep | ||
| Weakness or numbness | ||
| Loss of coordination or balance | ||
| Irregular breathing | ||
| Difficulty speaking |
Resources[edit | edit source]
References[edit | edit source]
- ↑ Hill CS, Coleman MP, Menon DK. Traumatic Axonal Injury: Mechanisms and Translational Opportunities. Trends in Neuroscience. 2016;39(5):311-324. doi.org/10.1016/j.tins.2016.03.002
- ↑ Hill CS, Coleman MP, Menon DK. Traumatic Axonal Injury: Mechanisms and Translational Opportunities. Trends in Neuroscience. 2016;39,5:311-324. doi.org/10.1016/j.tins.2016.03.002
- ↑ Dr John Campbell. Head Injuries 5, Primary Brain Injuries. Available from: https://youtu.be/Qe4Udri6JNo[last accessed 30/08/19]
- ↑ Dr John Campbell. Head Injuries 7, Secondary Brain Injury. Available from: https://youtu.be/bZZLMO_0EOs[last accessed 30/08/19]
- ↑ 5.0 5.1 Silver JM, McAllister TW, Yodofsky SC, editors. Textbook of Traumatic Brain Injury. Arlington, Va: American Psychiatric Publishing; 2005. p27-39.
- ↑ Werner C, Engelhard K. Pathophysiology of traumatic brain injury. British Journal of Anaesthesia. 2007;99(1):4-9. DOI: 10.1093/bja/aem131
- ↑ Hill CS, Coleman MP, Menon DK. Traumatic Axonal Injury: Mechanisms and Translational Opportunities. Trends in Neuroscience. 2016;39(5):311-324. doi.org/10.1016/j.tins.2016.03.002
- ↑ Morales DL at al. Brain Contusion Imaging. Medscape 2018. Available from: https://emedicine.medscape.com/article/337782-overview (accessed 15 June 2019)
- ↑ Centola Grassi D, Macedo da Conceição D, da Costa Leite C, Santos Andrade C. Current contribution of diffusion tensor imaging in the evaluation of diffuse axonal injury. Arq. Neuro-Psiquiatr. 2018;76(3):189-199. doi.org/10.1590/0004-282x20180007
- ↑ 10.0 10.1 Tenovuo O, Diaz-Arrastia R, Goldstein LE, Sharp DJ, van der Naalt J, Zasler ND. Assessing the severity of traumatic brain injury—time for a change?. Journal of clinical medicine. 2021 Jan 4;10(1):148.
- ↑ Karaliute M, Saksvik SB, Smevik H, Follestad T, Einarsen C, Vik A, Håberg AK, Iverson GL, Skandsen T, Olsen A. Methodology Matters: Comparing Approaches for Defining Persistent Symptoms after Mild Traumatic Brain Injury. Neurotrauma Reports. 2021 Dec 1;2(1):603-17.
- ↑ Smith DH, Stewart W. ‘Concussion’is not a true diagnosis. Nature Reviews Neurology. 2020 Sep;16(9):457-8.







