Cervical Spine Fractures in Contact Sports
Top Contributors - Grace Cooper, Kaya Simon, Chin Cheng Chan, Angeliki Chorti, Khloud Shreif, Naomi O'Reilly, Vidya Acharya and Cindy John-Chu
Introduction[edit | edit source]
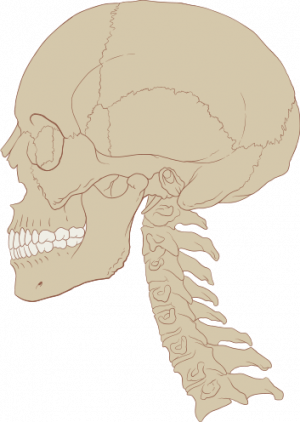
The cervical spine is a dynamic structure that protects nervous innervation to the entire body while maintaining the range of motion for the head and neck. It contains seven vertebrae, which provide support to the head while allowing for side flexion, rotation, flexion, and extension. [1]
Cervical spine fractures are a primary cause of mobility loss and mortality in trauma patients, with a bone fracture accounting for 56% of cervical spinal cord injuries. Damage to the spinal cord could have serious consequences as it is where the central nervous system connects between the brain and the body. A spinal cord injury at the cervical spine can lead to temporary or permanent paralysis of the entire body from the neck down. Fractures of the cervical spine are classified into three groups based on the level of involvement: C1, C2, and the sub-axial spine (C3 to C7). [2]
The most common causes of cervical fractures are motor vehicle accidents, falls, violence, and sports activities. On this page, we will be focusing on fractures in the cervical vertebrae in sports that involve physical contact. Although cervical spine injuries and patterns vary by sport and gender, [3] contact sports, e.g. American football, ice hockey, football, and rugby, carry a particular risk of cervical injuries as a cervical fracture could occur in actions like spearing an opponent with the head in contact sports.
Pathophysiology[edit | edit source]
A fracture to the cervical spine could result from compression (frequently caused by minor trauma in people with osteoporosis), burst fractures (vertebrae crushed in all directions) or a fracture-dislocation (from car collisions or falls from heights). C1 fractures typically occur due to axial loading. A combination of compression, hyperflexion, and hyperextension are the most common cause of C2 fractures. High-impact accidents are known to commonly cause sub-axial cervical spine fractures. [4]
Epidemiology[edit | edit source]
The literature suggests that cervical fractures are most commonly seen in association with trauma, [5] often in young males participating in contact sports. However, there is some divide between the prevalence rates and the specifics of certain risk factors. This may be due to the fact that studies often used populations who were already exposed to trauma and were done on spinal injuries as a whole instead of specifically cervical fractures.
Much of the literature agrees motor vehicle accidents to be the most common cause, with prevalence ranging from 48%-66%. [6] Contact sports injuries and falling from heights followed, ranging from 14%-21% and cases from assault ranged from 10-15%.[6] Despite not being as common, the literature also acknowledged the occurrence of specifically atlas fractures in the elderly, with this being primarily alongside other head and neck injuries. [7] A study by Khanpara et al. [8] suggested fractures to C1 and C2 to be the most prevalent across all causes and specifically closed fractures to C2 and C7 to be the most frequent. It was also supported that the incidence of cervical fractures increased between 2005 and 2013 from 62.3% to 67.6%.[8]
[edit | edit source]
Although cervical fractures are particularly common in contact sports, more recent studies are suggesting athletes participating in non-contact sports such as diving, horse riding, and cycling are also at significant risk. A study by DePasse et al. [9] identified cycling to be the most common cause of a cervical fracture after diving and football in males. The peak in the prevalence of cervical fractures in cycling between 2000-2015 was said to be partly responsible for the overall inrease in incidence of sport-related cervical fractures by 35% during this period. The study identified horse riding to be the most common for females and then followed by cycling. This more recent evidence suggests a shift in the prevalence of cervical fractures from certain sports.
Aetiology/ Mechanism of Injury[edit | edit source]
The mechanism of injury for a cervical fracture is complex and much is still unexplored with regards to mechanisms specific to certain sports. The literature seems to identify axial loading, buckling, the influence of padding and whiplash to be some of the key injury biomechanics involved in cervical fractures in contact sports. [10] The importance of those involved in pitch side was emphasised in the recognition of the mechanisms of injury for a cervical fracture during play.
Axial loading[edit | edit source]
The mechanism of axial loading arises when the head and neck are flexed to around 30 degrees; this causes the normal lordotic curve to disappear which means that the spine is not able to absorb the impact, resulting in a fracture. [11] A study by Swartz et al. [10] identified axial loading as a mechanism of injury for 27% of tackling injuries. A key factor in this was players tackling with their heads down or using the crown of their head as the initial point of contact during a tackle. As a result of the collision, the head stops but the trunk continues to move. The study recommended the use of the shoulder for blocking and tackling instead to reduce the chances of axial loading occurring. [12]
Buckling[edit | edit source]
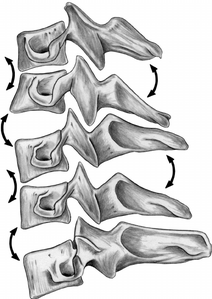
Buckling can occur during axial loading due to the compressive forces resulting in angulations within the cervical spine as an attempt to release the energy caused by the axial loading. [10] During buckling, the players' head and neck may not go through a noticeable observable motion yet but the cervical spine often goes into an extreme position of hyperflexion or hyperextension which suggests that head and neck movement is not always a reliable indication for the severity of the potential injury.
Influence of padded surfaces[edit | edit source]
Padded surfaces are needed in contact sports for protection against blunt trauma; however, there is some uncertainty as to whether they provide any protection to the cervical spine itself and could in fact act as a mechanism of injury for cervical fractures. The padding allows the impact force of the trauma to last longer meaning the head is in axial compression for longer, being depressed further into the padded surface. This phenomenon has been referred to ‘pocketing’ in studies as the padding forms a pocket for the head during the trauma making it near to impossible for the cervical spine to not be put under axial load and increasing the time it is under this load. [13]
Whiplash[edit | edit source]
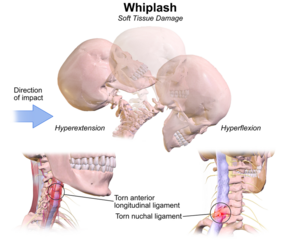
Whiplash can occur in contact sports, most often when a player is tackled from behind when they are not expecting it. In this situation the hips, back and trunk are the first areas to be moved by the force of the tackle. The trunk moves upwards and forwards to compress the cervical spine. This causes the neck to extend resulting in tension being created through buckling as the lower cervical vertebrae extend and upper vertebrae flex. It is not the extension which is the ultimate mechanism of injury but the combination of the forward trunk movement, compression and buckling that rotate to force the vertebrae into extension, putting extreme pressure on the facet joints. [10]
Risk factors for sustaining cervical fractures in contact sports[edit | edit source]
Participation in contact sports to any level increases the risks of attaining a cervical fracture, yet the research suggests that within this, males may be at greater risk than females with a male: female ratio of 2:1 suggested. [8] Age was probably the most emphasised risk factor across all studies with much of the literature attempting to identify a specific ‘red zone’ although there appeared to be great variability in this. The overall range varied between 15-35 years, with some studies suggesting this to be narrower of 20-29. [14] One of the more recent studies suggested an age of 18-25 with 80% of all cervical fractures in the study falling into that age group. [15] Osteoporosis and osteoarthritis were also identified as less common risk factors alongside chronic conditions such as congenital stenosis. [15]
Pitch-side Management[edit | edit source]
Management of cervical spine injuries in sport starts from the moment the player goes down on the pitch. Until a cervical spine injury can be definitively ruled out, players need to be handled with care to prevent exacerbating the injury and causing permanent harm.
Assessing on the Pitch[edit | edit source]
Prompt identification of any potentially catastrophic injuries is vital. The mechanism of injury is an important sign since pitch-side practitioners do not have the tools nor the time to accurately determine whether a player has a C-Spine injury. Crosby et al. [16] estimates that 2-5% of blunt trauma patients have a cervical spine injury.
If the practitioner witnessed trauma to the head or neck, or if their view was restricted and they could not see, then they must immediately perform manual inline stabilisation (MILS) to take control of the head. MILS is a manoeuvre used when a patient has suspected C-Spine trauma to provide a degree of stability to the cervical spine, prior to the application of a cervical collar. This will help minimise excessive movement and thereby reduce the chance of further injury. To perform MILS the practitioner or assistant should:
- Crouch/kneel/lie beside or behind the player, the clinician should attempt to stabilise their elbows/arms on the ground, against another stable object or on their knees to prevent swaying as they become fatigued
- Place both hands on the patient’s mastoid processes or cradle the occiput
- Apply equal pressure so not to move the head or let it fall
Primary Survey[edit | edit source]
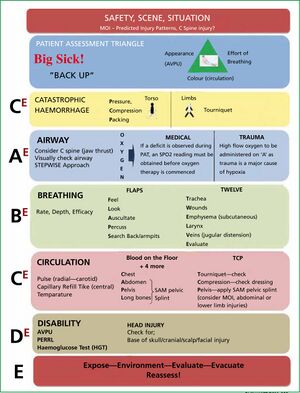
To assess a patient on the field, the clinician must first perform a primary survey. The first part involves assessing the players' alertness and then includes checking the players airways, breathing, and circulation to identify any life-threatening injuries. This survey will immediately identify if the player is breathing normally. It will ensure that the medical practitioner is fully aware if they have to carry out immediate interventions that could save the players life. If no immediate life-threatening injuries are present, then the clinician should determine the level of consciousness and conduct a neurological screening.
Secondary Survey[edit | edit source]
The secondary survey is a detailed head-to-toe examination with the purpose of determining whether the player has suffered any other injuries. This on-field evaluation should include an examination of the level of consciousness, cognitive and memory processes, and cranial nerve function, with an awareness that significant brain injury is possible. This is determined with the help of an A-E assessment. Maddocks questions are also used to investigate the suspicion of a head injury. [17] These 5 questions that take less than a minute are utilised to evaluate orientation as well as assessing short- and long-term memory function. However, their sensitivity range from 32-75%. [17] The Sports Concussion Assessment Tool 5 (SCAT5) is a standardised concussion screening tool used by medical practitioners as an effective pitch-side assessment mechanism and has been shown to have moderate to high test-retest reliability. [18]
The neurological evaluation of a conscious player can be used to further investigate potential C-Spine trauma and begins with questions about extremity numbness, painful dysesthesias or paraesthesia, weakness, and neck pain. A physical examination is limited to asking if the patient can move all of their limbs. If there is any gross weakness, numbness, or significant pain to the cervical region, then this could be indicative of a serious neurological deficit. If the athlete is unconscious or presents with any of the below symptoms, then they will need to be extracted off the pitch using a spinal motion-restriction device, such as a spinal board or cervical collar. [19]
- Blunt trauma and altered level of consciousness
- Spinal pain or tenderness
- Loss of cervical range of motion
- Neurologic complaint or findings (e.g., numbness or motor weakness in more than 1 limb)
- Anatomic deformity of the spine
Neck Immobilisation and Spinal Board Extraction[edit | edit source]
The gold standard for neck immobilization is the combined use of a hardboard, collar, sandbags, and tape or straps. This is used primarily during prehospital transfers and can limit movement to 5% of the normal range.[20] It should be noted that this type of immobilisation carries a high risk of pressure injury as there is literature to suggest that collars can cause increases in cerebrospinal fluid pressure, skin ulceration, reduced tidal volume and dysphagia. [21] Additionally, a 2011 study [22] observed that cervical collars are insufficient for immobilizing an unstable spine during passive range of motion tests. Numerous other studies also revealed that cervical collars fail to provide a significant reduction in motion during any transfer procedure. [23][24]
Once the collar is secured, the player can be moved onto a spinal board using the log roll technique. The use of the log roll will be applied in 2 scenarios. This will be at matchday or training where there may be a number of experienced and relevantly trained helpers. The other scenario could be where there are no trained helpers, and the medical practitioner will be required to ‘coach’ any assistance. As a note of caution, the best practice could be to not attempt a log roll and to manage the player where they are. [26] It may be the case that the initial care given is to keep them warm and to apply oxygen to the player using a non-rebreathe mask with high flow oxygen (15L/ Min).
- To perform a log roll safely, a minimum of 5 people is required
- The leader will be in charge of the head, keeping it MILS and preventing excessive rotation of the neck. The leader will also be the one giving commands to the rest of the group
- Three assistants should be kneeling beside the player, and one will be in charge of moving the spinal board
- The three assistants will place their hands on the opposite side of the player’s body, interlocking their arms.
- On the leader’s command, the assistants will roll the injured player to 90degrees and the spinal board will be slid underneath them
- Once the spinal board is in place, the player will be rolled back down on, again on the leader’s command
- From here, the leader remains in place and another assistant will help place head blocks and straps on.
Although it conveniently only requires 4 people, the log roll does not promise motion stability. Due to different dimensions in the head, torso, hips and lower extremities, it can be hard to maintain spinal alignment when the body is rolled. It is also incredibly difficult to ensure that the neck is rotated at the same pace as the rest of the body as the motion is carried out by four different people. [26] The log roll manoeuvre continues to be used due to a lack of training in alternative methods.
Whilst waiting for an ambulance, the Canadian C-Spine Rule can be used to determine whether a patient will need a scan. It is applicable to patients who are alert (Glasgow Coma Scale score of 15) and stable conditions following trauma where cervical spine injury is a concern. Based on a systematic review from 2012, [27] the Canadian-C spine rule has a high sensitivity and thus the potential to reduce imaging rates. However, there is also a moderate incidence of false-negatives which contributes to unnecessary imaging.
Further Management and Treatment[edit | edit source]
Management of cervical spine fractures may be surgical and/or conservative. Interventions for C-spine fractures are typically guided by the severity of the fracture. The urgency of treatment is dependent on a number of different factors including: life-threatening airway, respiratory or circulatory compromise, neurological lesions, and spinal instability. Therefore, appropriate initial management is deemed to play a crucial role in dictating long term prognosis of C-spine fracture patients.
Initial Management[edit | edit source]
Early and effective analgesia[edit | edit source]
This should be used within an acute setting to help control pain. NICE guidelines support the use of intravenous morphine as the first-line analgesic, where appropriate, or intra-nasal diamorphine or ketamine if intravenous access cannot be achieved or established. [28]
Stabilisation of the Cervical spine[edit | edit source]
This becomes the focus of the initial management of a suspected C-spine fracture and is achieved by following the ATLS protocol to protect the spinal cord via immobilisation of all neck movements using a cervical collar. This is known as the 3-point C-spine immobilisation.
As previously mentioned, it is important to recognise that the application of these collars is not without complications. Therefore, more recent evidence suggests that cervicothoracic orthoses such as halo-thoracic bracing can be considered more appropriate for the initial management of a c-spine fractures as they provide greater stabilisation through restricting flexion and extension by 70-80%, rotation by 60-70% and lateral flexion by 60%. [29]
The next stage in the management of C-spine fractures is primarily guided by the grade of instability caused by the injury. [30] The grade of cervical spine instability is paramount in the decision-making process to guide definitive management. [31] A traumatic spinal injury, such as a C-spine fracture, can disrupt the biomechanical stability of the spine – therefore causing both neurological and musculoskeletal injuries that can detrimentally impact a patient’s functional status. [32] Therefore, a principal aim in the management of C-spine fractures is to reduce and prevent further disability in our patients functional status.
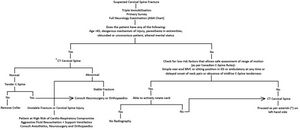
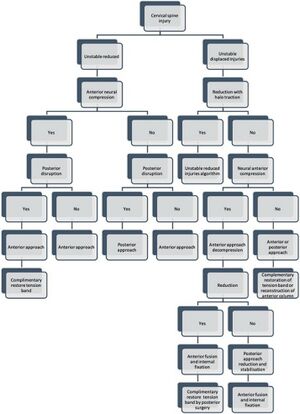
Surgical Treatment[edit | edit source]
Algorithm for the management of suspected cervical spine fractures in the emergency department:
- Progressive neurological deterioration
- Patients with high incidence of late complications e.g.: kyphosis of 30 degrees.
Aims of Surgery:
- Re-align the cervical spine to achieve mechanical stability.
- Reduce pain and discomfort.
- Preserve and improve neurological function.
- Facilitate early movement in the rehabilitation process.
Surgical approaches for treating sub axial cervical injuries include anterior decompression and fusion, posterior stabilisation with or without decompression and a circumferential approach that combines both anterior and posterior approaches to the spine (Zaveri, 2017). Surgical stabilisation should also be considered with patients who are unable to mobilise with cervical collar bracing (O’Dowd, 2010).
However, the benefits of surgery must be weighed up against the potential risks, which should be considered on an individual case-by-case basis [33]
- Risk of hemorrhage
- Damage to the carotid or vertebral artery
- Damage to the superior or recurrent laryngeal nerve
- Damage to the trachea or oesophagus leading to infection
- Surgical wound infection
- Potential damage to the spinal cord causing neurological deficits
It is important to consider these risks when weighing up the effectiveness of surgical intervention. In the general population, anterior cervical discectomy and fusion (a common type of C-spine surgery) has been found to be successful in approximately 89% of patients. [34] However, it is important to recognise that there are some key differences in the management of C-spine fractures in athletes compared to the general population.
- Athletes tend to be in good health and therefore are more likely to respond positively to surgery and post-surgical rehabilitation.
- But, on the other hand, athletes are more likely to engage in activities with high levels of physical demands that therefore put the spine at greater risk of a further or new injury.
As a result, the decision-making process surrounding surgical intervention must be taken on an individual case-by-case basis with the goal to achieve the best possible return-to-play outcomes for your athlete.
Return to Play and Long-Term Management for Different Types of Fractures[edit | edit source]
Taking into consideration the potential devastating complications associated with cervical spine fractures, return to play decisions are generally contentious and variable between different cases and classifications of injury. Despite no randomised controlled trials being carried out, decision making is largely guided by expert opinion. There is an overwhelming consensus that the athlete must be: asymptomatic, have full strength, full active range of motion and be psychologically prepared to return to training and competitive play.
Cervical Spine Fracture[edit | edit source]
The decision making regarding RTP is largely indicated by the degree of instability at the cervical spine. Some fractures, including fractures of the spinous process or unilateral laminar fractures, do not cause instability and may require no treatment or only short-term immobilisation in a cervical collar. Minimally displaced bilateral pars interarticularis fractures of C2 (Hangman’s fracture) can be treated with a cervical collar (conservative management).
Unstable Cervical Spine Fracture[edit | edit source]
These types of fractures should be reduced quickly and stabilized temporarily with cervical traction using Gardner-Wells tongs or a halo ring device. A contrast-enhanced CT scan or MRI of the cervical spine may be obtained before fracture reduction to rule out the presence of retro pulsed intervertebral disk material. An unrecognized retro pulsed disk material has been implicated in the sudden neurological deterioration of patients undergoing a reduction of their cervical fractures. Therefore, surgical treatment is typically indicated for unstable cervical fractures.
Stable Fractures[edit | edit source]
In the case of a stable fracture that has completely healed according to radiological confirmation, players are allowed to return within approximately 12 months, providing they are asymptomatic, have regained full strength, range of motion and are psychologically prepared to return to play. Currently, there is no experimental or clinical data to help physicians predict the stability of healed spinal fractures or fusions when they are placed under extreme degrees of mechanical stress. There is increased mechanical stress above and below fused spinal segments, and repetitive microtrauma to a stiff spine exacerbates the stress. At present, there is no conclusive evidence that the injured cervical spine is made stronger than normal by fusion. Thus, in the absence of any objective ability to measure the degree of dynamic stress stability of the spine, any healed fracture (except for chip, minor wedge/compression, isolated laminar, or spinous process fractures) and any injury that has required internal stabilization must be dealt with caution. Where there are multilevel fusions or a fusion involving C1–C2 or C2–C3, return to contact collision sports is contraindicated, but the athlete could participate in a noncontact sport with low risk of neck injury, such as tennis or golf.
Associated Neurological Injuries[edit | edit source]
Guidelines state that any athlete with a neurological injury should be prohibited from further competition/practice until asymptomatic. [35] Those without cord injury (i.e., a normal neurological exam), who have stable fractures as evidenced by flexion-extension radiographs can be allowed to return to their normal daily activities. Those whose fractures require a halo vest or surgical stabilization are considered to have insufficient spinal strength to safely return to contact sports unless bony fusion and the neurological exam are shown to be normal. Even after the fracture has healed, the altered biomechanics in surrounding spinal segments and loss of normal motion may produce high risk of future sports-related injury.
Return To Play: An example of the Physical Management of a Stable Cervical Spine Fracture with no Contraindications[edit | edit source]
Early-Stage Management[edit | edit source]
The decision to begin a rehabilitation protocol must be determined by the athlete and an multi-disciplinary team consisting of the medical professionals, therapist, coaches. The key goals of the initial stage are to reduce pain, reduce muscle spasm and begin to restore normal range of motion and quality of movement'. Empirical evidence supports the combination of multiple treatment modalities including range of motion exercises, massage, electrical stimulation, heat, and analgesics. Initial rehabilitation should be carried out with the cervical spine in neutral alignment and in a position where gravity is eliminated to prevent any nerve root, disc or facet joint irritation and limit the involvement of overactive superficial muscles.
Early-stage range of motion exercises should commence as soon as possible and have been shown to have good analgesic effects. [36] If active range of motion is limited, a progression from passive to active should be carried out. It is important to avoid intense stretching of spasmed muscles, as research has shown it can reduce the stability of the neck. Simple exercises in all planes of movement should be carried out without the provocation of pain and reproduction of symptoms.
Research has shown the importance of retraining the deep neck flexor’s (DNF’s) as they are the key stabilisers for the cervical spine. Isometric strengthening of the deep neck flexors (DNF’s) can commence immediately. The ‘Cranio-Cervical Flexion Test’ may give objective feedback which is helpful for monitoring purposes throughout the rehabilitation process. [37]D epending on access to equipment, ideally, a pressure cuff should be used for feedback. Progressive overload should be achieved through increasing pressure, number of repetitions and the length of holds.
In order to move on to the next phase, there should be a significant reduction in acute painful symptoms, full asymptomatic, active range of motion in all planes should be achieved, and activation of the DNF’s.
Initial Rehabilitation[edit | edit source]
The aim of this stage is to increase the strength of the neck mobilisers without exposing them to excessive forces. Range of motion exercises and DNF strengthening should continue during this phase.
Initial programming should be set at a moderate volume and low intensity and then gradually increased with more repetitions, length of contraction and the number of sets. Throughout the phase, the athlete and therapist should monitor any reproduction of symptoms, loss of range of motion and any change in biomechanics (especially any compensatory shoulder kinematics).
In terms of positioning, the athlete should begin strengthening in a gravity-eliminated position before progressing to standing and then finally any sport-specific positions.
Rehabilitation Progression[edit | edit source]
Once full range of motion is achieved and isometric contraction is asymptomatic and 100% of maximum voluntary contraction, the progression is to move on to concentric and eccentric strengthening through the range.
This isotonic strengthening should be done at a higher volume and a medium intensity, initially using manual or dynamometry resistance. Cable machines can also be used with a head harness. Exercises should begin in the sagittal plane (flexion and extension) and then progress to transverse and coronal plane strength.
Once strength in all planes is back to baseline, sport specific neck training can begin in a controlled manner. For example, in rugby, tackle bags can be used to reintroduce contact and in racing, drivers can use simulation equipment.
Return To Play[edit | edit source]
The final stage to the rehabilitation programme is combining the previous neck strengthening regime with an emphasis returning to sport specific skills, along with psychological preparation to be exposed to forces on the cervical spine.
A study by Eckner et al. [38] demonstrated how the pre-activation of muscles around the cervical spine has the potential to decrease the likelihood of head and neck injuries in sport. An example of this in rugby is a pre-activation routine using a resistance band, working the muscles around the cervical spine in all planes prior to training or a match. This has been shown to increase the chance of adapting neural elements resulting in optimal motor skill, muscular control and co-ordination.
Like in any case, the decision to return to play is injury and athlete specific. The decision should involve all members of the MDT but should remain centred around the athlete. In order to reduce the risk of further injury and optimise performance, the athlete should be confident that they are both physically and psychologically prepared to return to competitive play.
References[edit | edit source]
- ↑ Frost BA, Camarero-Espinosa S, Foster EJ. Materials for the spine: anatomy, problems, and solutions. Materials. 2019 Jan 14;12(2):253.
- ↑ Van Eck CF, Fourman MS, Abtahi AM, Alarcon L, Donaldson WF, Lee JY. Risk factors for failure of nonoperative treatment for unilateral cervical facet fractures. Asian Spine Journal. 2017 Jun;11(3):356-64.
- ↑ Meron A, McMullen C, Laker S, Currie J, Comstock D. Epidemiology of Cervical Spine Injuries in High School Athletes Over a Ten-Year Period. PM&R 2018 April; 10(4):365-72.
- ↑ Fehlings MG, Tetreault L, Nater A, Choma T, Harrop J, Mroz T, Santaguida C, Smith JS. The aging of the global population: the changing epidemiology of disease and spinal disorders. Neurosurgery. 2015 Oct 1;77(suppl_1):S1-5.
- ↑ MarconI RM, CristanteI AF, Jacobsen TeixeiraII W, NarasakiII DK, OliveiraI RP, Pessoa de Barros Filho TE. Fractures of the cervical spine. Clinics 2013 Jan; 68(11):1455-61.
- ↑ 6.0 6.1 Hauwe LV, Sundgren PC, Flanders AE. Spinal trauma and spinal cord injury (SCI). Diseases of the Brain, Head and Neck, Spine 2020–2023. Cham, Springer. 2020:231-40.
- ↑ Fiedler N, Spiegl UJ, Jarvers JS, Josten C, Heyde CE, Osterhoff G. Epidemiology and management of atlas fractures. Eur Spine J. 2020 Oct;29(10):2477-83.
- ↑ 8.0 8.1 8.2 Khanpara S, Ruiz-Pardo D, Spence SC, West OC, Riascos R. Incidence of cervical spine fractures on CT: a study in a large level I trauma center. Emergency Radiology. 2020 Feb;27(1):1-8.
- ↑ DePasse JM, Durand W, Palumbo MA, Daniels AH. Sex-and sport-specific epidemiology of cervical spine injuries sustained during sporting activities. World neurosurgery. 2019 Feb 1;122:e540-5.
- ↑ 10.0 10.1 10.2 10.3 Swartz EE, Floyd RT, Cendoma M. Cervical spine functional anatomy and the biomechanics of injury due to compressive loading. Journal of athletic training. 2005 Jul;40(3):155.
- ↑ Torg JS. Athletic injuries to the head. neck and face. Mosby 1991:345-50.
- ↑ Cantu RC, Mueller FO. Catastrophic football injuries: 1977–1998. Neurosurgery. 2000 Sep 1;47(3):673-7.
- ↑ Nightingale RW, McElhaney JH, Richardson WJ, Myers BS. Dynamic responses of the head and cervical spine to axial impact loading. J Biomech. 1996 Mar 1;29(3):307-18.
- ↑ Schoenfeld AJ, Sielski B, Rivera KP, Bader JO, Harris MB. Epidemiology of cervical spine fractures in the US military. Spine J. 2012 Sep 1;12(9):777-83.
- ↑ 15.0 15.1 Schroeder GD, Vaccaro AR. Cervical spine injuries in the athlete. J Am Acad Orthop Surg. 2016 Sep 1;24(9):e122-33.
- ↑ Crosby ET, Lui A. The adult cervical spine: implications for airway management. Canadian Journal of Anesthesia/Journal canadien d'anesthésie. 1990 Jan;37(1):77-93.
- ↑ 17.0 17.1 Brown J, Viljoen W, Hendricks S, Abrahams S, Burger N, McFie S, Patricios J, On-field identification and management of concussion in amateur rugby union. S Afr J Sports Med 2016;28(1):6-10.
- ↑ Echemendia RJ, Meeuwisse W, McCrory P, Davis GA, Putukian M, Leddy J, Makdissi M, Sullivan SJ, Broglio SP, Raftery M, Schneider K. The sports concussion assessment tool 5th edition (SCAT5): background and rationale. Br J Sports Med. 2017 Jun 1;51(11):848-50.
- ↑ Fischer PE, Perina DG, Delbridge TR, Fallat ME, Salomone JP, Dodd J, Bulger EM, Gestring ML. Spinal motion restriction in the trauma patient–a joint position statement. Prehosp Emerg Care. 2018 Nov 2;22(6):659-61.
- ↑ Crosby ET, Lui A. The adult cervical spine: implications for airway management. Can J Anesth.1990 Jan;37(1):77-93.
- ↑ Papadopoulos MC, Chakraborty A, Waldron G, Bell BA. Exacerbating cervical spine injury by applying a hard collar. BMJ. 1999 Jul 17;319(7203):171-2.
- ↑ Horodyski M, DiPaola CP, Conrad BP, Rechtine II GR. Cervical collars are insufficient for immobilizing an unstable cervical spine injury. J Emerg Med. 2011 Nov 1;41(5):513-9.
- ↑ Conrad BP, Horodyski M, Wright J, Ruetz P, Rechtine GR. Log-rolling technique producing unacceptable motion during body position changes in patients with traumatic spinal cord injury. J Neurosurg Spine 2007;6:540-3
- ↑ DiPaola MJ, DiPaola CP, Conrad BP, Horodyski M, Del Rossi G, Sawers A, Bloch D, Rechtine GR. Cervical spine motion in manual versus Jackson table turning methods in a cadaveric global instability model. J Spinal Disord Tech. 2008 Jun 1;21(4):273-80.
- ↑ Interior Health. Hard Collar Application. Available from: http://www.youtube.com/watch?v=ydljBEN2RU8 [accessed 5/5/2023]
- ↑ 26.0 26.1 Conrad BP, Del Rossi G, Horodyski MB, Prasarn ML, Alemi Y, Rechtine GR. Eliminating log rolling as a spine trauma order. Surg Neurol Int. 2012;3(Suppl 3):S188-97.
- ↑ Michaleff ZA, Maher CG, Verhagen AP, Rebbeck T, Lin C.-W. Accuracy of the Canadian C-spine rule and NEXUS to screen for clinically important cervical spine injury in patients following blunt trauma: a systematic review. CMAJ. 2012; 184(16):E867–76.
- ↑ National Institute for Health and Care Excellence. Spinal Injury: Assessment and Initial Management. Available from: https://www.nice.org.uk/guidance/ng41/evidence/full-guideline-2358425776 [accessed 7/5/2023]
- ↑ Aresti N, Grewal I, Montgomery A. The initial management of spinal injuries. Orthop Trauma. 2014; 28(1):63-9.
- ↑ O’Dowd J. Basic principles of management of cervical spine trauma. Eur Spinal J. 2010; 19(1):18-22.
- ↑ Beeharry MW, Moqeem K, Rohilla MU. Management of Cervical Spine Fractures: A Literature Review. Cureus. 2021 Apr; 13(4): e14418.
- ↑ Niazi T, Daubs M, Dailey A. Principles of Surgical Management of Spinal Trauma Associated with Spinal Cord Injury. Musculoskeletal Key. Available from: https://musculoskeletalkey.com/principles-of-surgical-management-of-spinal-trauma-associated-with-spinal-cord-injury/ [accessed 7/5/2023]
- ↑ Wascher T. Potential Risks and Complications of ACDF Surgery. Available from: https://www.spine-health.com/treatment/spinal-fusion/potential-risks-and-complications-acdf-surgery [accessed 7/5/2023]
- ↑ Haghnegahdar A, Sedighi M. An Outcome Study of Anterior Cervical Discectomy and Fusion among Iranian Population. Neurosci J. 2016;1(1): 1-7.
- ↑ Cockerell OC, Iino Hayes N, Sylvester R. The neurological risks of playing association football. JRSM open. 2021 Nov;12(11):20542704211055558.
- ↑ Yesil H, Hepguler S, Dundar U, Taravati S, Isleten B. Does the Use of Electrotherapies Increase the Effectiveness of Neck Stabilization Exercises for Improving Pain, Disability, Mood, and Quality of Life in Chronic Neck Pain?. Spine. 2018 Oct 15; 43(20):E1174-83.
- ↑ Hudswell S, von Mengersen M, Lucas N. The cranio-cervical flexion test using pressure biofeedback: A useful measure of cervical dysfunction in the clinical setting?. Int J Osteopath Med. 2005; 8(3):98-105.
- ↑ Eckner JT, Oh YK, Joshi MS, Richardson JK, Ashton-Miller JA. Effect of neck muscle strength and anticipatory cervical muscle activation on the kinematic response of the head to impulsive loads. Am J Sports Med. 2014 Mar;42(3):566-76.