Assessment of Spinal Cord Injury
Original Editor - Naomi O'Reilly
Top Contributors - Naomi O'Reilly, Kim Jackson, Admin, Tarina van der Stockt, Eugenie Lamprecht, Tony Lowe, Rucha Gadgil, Lucinda hampton and Olajumoke Ogunleye
Introduction[edit | edit source]
Assessment in neurological physiotherapy is a process of collecting information about disordered movement patterns, underlying impairments, activity restrictions, and societal participation for the purpose of intervention planning and to help the therapist determine the best intervention. [1][2] Assessment is arguably the most important step in the rehabilitation process, as our clinical reasoning is based on the information it provides and provides the basis for our decision making throughout the rehabilitation process. Treatment can only be as good as the assessment on which it was based, so in order for us to progress and manage our treatment plan and ensure we are identifying our patients' problems, assessment should be an ongoing and continuous, and should allow us to develop individualised, patient-centred goals and ultimately a tailor-made treatment plan for the individual.
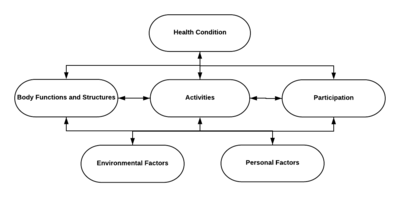
We can use the framework of the International Classification of Functioning, Disability and Health (ICF) to define the role and purpose of physiotherapy for individuals with spinal cord injury. The ICF was introduced by the World Health Organization (WHO) in 2011 and is a revised version of the International Classification of Impairment, Disability and Handicap. The ICF defines components of health from the perspective of the body, the individual and society. One of its primary purposes is to provide a unified and standard language for those working in the area disability, which enhances clarity of communication and understanding of team roles with a spinal cord injury multidisciplinary team and challenges clinicians to think holistically. [3][4]
The assessment of an individual with a spinal cord injury is an important initial step in physiotherapy management. This step is not only important for setting realistic goals, but also for identifying key problems. We can use the ICF to articulate the goals and purpose of physiotherapy for individuals with a spinal cord injury. For example, the health condition is a spinal cord injury. An associated impairment is decreased muscle strength, which directly impacts on the ability to perform activities such as walking and moving. This in turn has implications for participation, such as working, engaging in family life and participating in community activities. Standardised assessments of impairments are similar to those used across all areas of physiotherapy, although there are some that are specific to spinal cord injury. Assessments of impairments are of limited interest to a physiotherapist without accompanying assessments of activity limitations to quantify a person's ability to move and complete purposeful motor tasks. Impairments, activity limitations and participation restrictions are also all affected by environmental and personal factors, such as support from family and employers, access to appropriate equipment, financial situation and coping mechanisms. In the ICF framework, such environmental and personal influences are termed contextual factors. Ensure you are familiar with the ICF, its general use in Clinical Practice and its use within the Neurorehabilitation Process as it should provide the framework for your assessment and treatment throughout the rehabilitation process. [4][5]
Database[edit | edit source]
Reviewing the individual's medical chart and liaising with the medical team forms the initial element of any assessment, providing background data about the individual to assist us to determine if they are medically stable and ready for physiotherapy. [1]
Presenting Condition[edit | edit source]
Diagnosis[edit | edit source]
- Type of Spinal Cord Injury e.g. Complete or Incomplete, Specific Syndrome
- Level of Spinal Cord Injury e.g. C5
- AIS Level e.g AIS A
History of Presenting Condition[edit | edit source]
Date of Spinal Cord Injury[edit | edit source]
- When did the spinal cord injury occur?
- How long ago was the spinal cord injury?
Cause of Spinal Cord Injury[edit | edit source]
- Traumatic or Non-traumatic. When did initial symptoms appear, were they sudden or did they come on gradually. This can have a bearing on what type of medical treatment options may be available to the patient.
Progression of the Condition[edit | edit source]
- Look for changes in the initial symptoms, which may provide some information about the behaviour of the condition and some prediction of prognosis.
- What was the initial AIS Level? e.g. has there been a change in their AIS Scale since admission? Following treatment?
Results of Specific Investigations[edit | edit source]
- Results of these investigations assist us in having an overall understanding of the patient's condition and provide us with specific information, which allows us to predict the signs and symptoms that are likely to be present and assist us in planning our objective assessment e.g.
Medical Management[edit | edit source]
- How has the condition been managed by the medical team?
- Did they require surgery or other medical interventions? e.g.ventilatory supports, nutritional supports, etc.
Medical Observations[edit | edit source]
- Provides information on how medically stable the patient is and on their suitability for physiotherapy assessment
Other Management[edit | edit source]
- What other management is in place for the individual that your assessment may need to be scheduled around e.g. bladder and bowel management, nutritional needs - if a patient has not got adequate intake this could affect your assessment
- What other multidisciplinary team members are involved with treatment?
Previous Therapy[edit | edit source]
Has the individual previously been involved in Physiotherapy?[edit | edit source]
- What are their expectations of physiotherapy?
Surgical History and Precautions[edit | edit source]
- Type of Procedure
- Date of Surgery
- Any Complications?
- Any contraindication?
Past Medical History and Medications[edit | edit source]
Co-morbidities[edit | edit source]
- Consider the impact of other co-morbidities on treatment and management
Previous Neurological Conditions[edit | edit source]
- Has the individual had previous neurological conditions, which had an impact on their functional abilities and may be useful in predicting future outcomes
Special Equipment[edit | edit source]
- Does the individual require the use of specialized equipment for their management e.g. Suction Units, Special Seating, Orthotics, Mobility Aids
Technology Dependency[edit | edit source]
Is the individual dependent on certain technologies either prior to this admission or new since this admission that you need to be aware of? e.g. Nasal Gastric Tube, Wheelchair, AFO's
Previous Surgery[edit | edit source]
- Has the individual had previous surgery separate to any spinal stabilization that could impact on your assessment and has impacted on their function? e.g. Joint Replacements, Abdominal Surgery
Risk Factors[edit | edit source]
- Does the individual have specific risk factors that could be related to further Neurological Incident e.g. Atrial Fibrillation, Hypertension, Hypotension, High Cholesterol, Diabetes Mellitus
Medication History[edit | edit source]
- Name, dosage, frequency of any medication
- Recognize any contraindications for Physiotherapy Treatment
- Impact of Related Side Effects on Treatment e.g. Dantrolene can cause Nausea
Subjective Assessment[edit | edit source]
The subjective assessment is used to provide a detailed picture of how the spinal cord injury affects the individual and is particular to each individual. Much of the database information might also be collected during the subjective assessment when not in a formal hospital or healthcare environment where detailed records are available. Always consider your verbal and non-verbal communication as this will influence your interaction, as will the environment. Understanding what the individual was able to do pre spinal cord injury is vital in order to guide your objective assessment, set appropriate, realistic goals to guide treatment and maintain motivation.[6];
Social History[edit | edit source]
Having an understanding of the individual's social situation will allow you to plan for discharge and to ensure adequate supports are in place both during and after their treatment.
Social Situation
- What is the individual's background e.g. Occupation, Family, Hobbies / Recreation
Support Structures
- What support structures does the individual have from family, friends, colleagues or dependents?
- Having an understanding of these structures is key when looking at your discharge plans.
- It may assist with determining what may be needed for that individual when their inpatient treatment is complete.
Accommodation
- What type of accommodation are they living in? e.g. Two Storey, Bungalow, Apartment, Access such as Stairs, Steps Elevators
- Who are they living with? Family, Friends, Alone
- This is key information for goal setting and when planning for discharge options.
Social Service Support
- Was the individual previously linked in with any social service supports? e.g. Public Health Nurse, Home Care Supports, Meals on Wheels etc.
Patient Goals and Expectations[edit | edit source]
Goal setting is used to direct rehabilitation interventions towards a specific outcome or outcomes. Therapists should always involve patients in setting goals for their therapy. Goals that are of value to patients will optimize their motivation for and participation in the therapy and enable them to achieve the highest possible level of independence, autonomy, and control.
Objective Assessment[edit | edit source]
The functional consequences of an acute spinal cord are variable; therefore, the initial clinical presentation of an individual with an acute spinal cord injury is a key factor in determining triage, defining therapy, and predicting prognosis. The individual must be assessed with an accurate, consistent, and reproducible neurological assessment scale to define the neurological deficits and to facilitate communication. The comprehensive clinical assessment of the individual with a spinal cord injury should both accurately describe the individual’s neurological function (motor and sensory examinations) and generally predict the future relative abilities and/or impairment given the neurological status.
Assessment of Impairments[edit | edit source]
Objectively it is essential to first assess impairments including weakness, sensation, tone, range of movement and then the impact that these impairments have at the activity and participation level for the individual with a spinal cord injury. Only impairments which are amenable to physiotherapy interventions are of real interest. Key impairments need to be linked to specific activity restrictions and participation limitations. Identification and treatment of impairments without linking them to activity limitations and participation restrictions risks wasting time, money and resources on impairments which are of little consequence.
Muscle Strength[edit | edit source]
An assessment of muscle strength is typically performed as part of a patient's objective assessment to assist the physiotherapist's clinical reasoning and enable them to reason an appropriate point to begin strengthening rehabilitation from. Muscle strength can be assessed by a number of methods: manually, functionally or mechanically including the following; [7]
- Manual Muscle Testing (MMT) is a standardized set of assessments that measure muscle strength and function
- Repetition Maximum Testing is defined as the weight that can be lifted through an entire range of motion a set number of times. Most commonly one repetition maximum (1 RM) or ten repetition maximum (10 RM) are used.
- Hand-held Myometry are small devices that measure isometric force
- Dynamometry measures torque during dynamic contractions at a constant angular velocity
Muscle strength is assessed early in the acute phase following a spinal cord injury using the motor assessment of the International Standards for Neurological Classification of Spinal Cord Injury. Read more about Muscle Strength Assessment and Manual Muscle Testing
Sensation[edit | edit source]
According to Jones [6] sensation is complex consisting of several modalities including our four special senses including Vision, Hearing, Smell and Taste and our Somatosensory Senses including tactile - light touch and pressure, proprioception, temperature and pain. Injury to the Spinothalamic Tracts and/or Posterior Column following a spinal cord injury result in sensory deficits. Pain and temperature are transmitted by the lateral spinothalamic tracts. Light touch is transmitted by the anterior spinothalamic tract. Proprioception is transmitted by the posterior column. Spontaneous abnormal sensations may be noted early after injury and increase in severity to a sharper, burning character (dysesthesia) with chronic spinal cord changes. There may be associated with hyperesthesia, hyperalgesia, or numbness.
The evaluation of sensation, or any sensory modality for that matter, is highly dependent on the ability and desire of the patient to cooperate. Sensation belongs to the patient (i.e. is subjective) and the examiner must, therefore,e depend almost entirely on their reliability. Sensory changes that are unassociated with any other abnormalities (i.e., motor, reflex, cranial, hemispheric dysfunctions) must be considered weak evidence of disease unless a pattern of loss in a classical sensory pattern is elicited e.g. in a typical pattern of peripheral nerve or nerve root distribution. Therefore, one of the principle goals of the sensory exam is to identify meaningful patterns of sensory loss.
The sensation is assessed early in the acute phase following a spinal cord injury using the sensory assessment of the International Standards for Neurological Classification of Spinal Cord Injury. Read more about Sensory Assessment
Muscle Tone[edit | edit source]
According to Jones (2011) muscle tone is the state of readiness in a muscle at rest which provides us with a background level of tone from which we can function efficiently, defined by the resistance to passive movement. Normal tone should be high enough to maintain our position upright against gravity but low enough to allow voluntary movement. [6] Muscle tone is dependent on two physiological factors;
- Neural factors relate to the degree of activation of the contractile apparatus of the muscle which is a result of output from the alpha motor neuron in the ventral horn of the spinal cord. [6]
- Non-Neural factors relate to mechanical-elastic properties of the soft tissue incorporating the viscosity of the muscle and muscle length, which can be influenced by age, temperature and exercise. [6]
Damage to the Central Nervous System following may cause an individual to lose the ability to control muscle tone which can lead to either an increase or decrease in muscle resting tone. [8] An Upper Motor Neuron Lesion may be characterized by increased tone, while a Lower Motor Neuron Lesion results in hypotonia. Depending on the level of the lesion individuals with a spinal cord injury may present with either increased or decreased muscle tone.
Decreased Tone[edit | edit source]
The terms hypotonicity and flaccidity are general with no truly objective measures available. Generally, hypotonia or low tone is considered to be an abnormal decrease in skeletal muscle tone, a reduced level of muscle stiffness, providing little to no resistance to passive movement and present with heavy limbs when handled and have difficulty maintaining an upright position against gravity. Flaccidity is considered to be the total absence of muscle tone.
Increased Tone[edit | edit source]
Spasticity is a velocity-dependent increase in tonic stretch reflexes with exaggerated tendon jerks, resulting from hyperexcitability of the stretch reflex that develops in individuals with an upper motor neuron lesions and has three main characteristics; [9]
- Velocity-Dependence. The amount of muscle tone depends on the velocity of movement: the more rapid the movement, the greater the resistance; the slower the movement, the less the resistance.
- Differing Tone in Flexors and Extensors. The tone in the flexors and extensors of a limb is not balanced, which commonly causes characteristic resting postures of that limb. Some individuals with a complete spinal cord injury have excess tone in the flexors of the legs, which causes the legs to flex up onto the abdomen
- Associated Weakness. The muscle with spasticity is also often weak. If left untreated, muscles shortened by spasticity may eventually develop fixed contractures.
Spasticity can be assessed through observation and measurement tools such as the Modified Ashworth Scale or Tardieu Scale. Read more about Assessment of Spasticity
Reflexes[edit | edit source]
Reflex testing, which incorporates an assessment of the function and interplay of both the sensory and motor pathways, is simple, informative and can give important insights into the integrity of the nervous system across many different levels.
Deep Tendon Reflexes[edit | edit source]
The stretch reflex (myotatic reflex) is a muscle contraction in response to stretching within the muscle. It is a monosynaptic reflex which provides automatic regulation of skeletal muscle length. When a muscle lengthens, the muscle spindle is stretched and its nerve activity increases. This increases alpha motor neuron activity, causing the muscle fibers to contract and thus resist the stretching. A secondary set of neurons also causes the opposing muscle to relax. The reflex functions to maintain the muscle at a constant length. [6]
- Biceps (C5/6)
- Triceps (C7/8)
- Brachioradialis (C6/7)
- Patellar / Knee (L3/4)
- Achilles / Ankle (S1/2)
Plantar Reflex (Babinski's Sign)[edit | edit source]
The Plantar Reflex (Babinski Sign) refers to the dorsiflexion of the great toe with or without fanning of the other toes and withdrawal of the leg, on plantar stimulation in patients with pyramidal tract dysfunction. Read more about the Plantar Reflex.
Hoffmanns Reflex (Finger Flexor Test)[edit | edit source]
Hoffmann's Reflex (Finger Flexor Test), named for Johann Hoffmann, is a finding elicited by a reflex test which verifies the presence or absence of problems in the corticospinal tract. The test involves tapping the nail or flicking the terminal phalanx of the middle or ring finger. A positive response is seen with flexion of the terminal phalanx of the thumb.
Babinski sign video provided by Clinically Relevant
Hoffman's sign video provided by Clinically Relevant
Joint Range of Motion[edit | edit source]
Range of Motion is the measurement of movement around a specific joint or body part or is the distance or amount of freedom your joint can be moved in a certain direction. Range of motion is measured in angle degrees normally with a Goniometer. There are three primary elements related to the range of motion.
- Passive Range of Motion is typically practised on a joint that is inactive.
- Active-assistive Range of Motion is movement completed with some manual assistance from the physiotherapist.
- Active Range of Motion are movements performed solely by the patient.
Loss of joint range of movement and joint mobility, is a common complication of spinal cord injury often leading to contracture. Reduced joint range of movement or contracture can be neurally mediated secondary to spasticity and non-neurally mediated as a result of structural changes in soft tissues overlying the joints. Measurements of passive joint range of motion are used to determine baseline movement and quantify the severity of contracture where present. Read more about Goniometry
Balance[edit | edit source]
Balance, [12]especially sitting balance, is essential for individuals with SCI as many individuals are wheelchair-bound. Balance is required in order to remain upright posture and prevent falls while using the upper limbs to assist ambulation when using a wheelchair. However, the complete/ partial loss of sensation and muscle strength in the lower limbs and trunk may affect the individual's ability to maintain balance.
Balance control is determined by;
- Static Balance: maintaining an upright posture.
- Proactive Balance: maintaining balance during voluntary movement.
- Reactive Balance: regaining balance after a loss of balance occurred.
Physiotherapists should assess all 3 these aspects of balance throughout different functional activities due to its task-specific nature. 3 Outcome measures used to assess unsupported sitting balance include;
Sitting Balance Score (SBS)
| Score | Assess |
|---|---|
| 1 (poor) | Unable to maintain a static position |
| 2 (fair) | Able to maintain a static position without difficulty
but requiring assistance in all righting tasks |
| 3 (good) | Able to maintain a static position without difficulty,
but requiring assistance in righting from the hemiplegic side |
| 4 (normal) | Able to perform the testing without any physical assistance |
Motor Assessment Scale (MAS) item 3 ‘Balanced Sitting’
| Score | Assess |
|---|---|
| 1 | Sits with support only |
| 2 | Sits unsupported for 10 s |
| 3 | Sits unsupported with weight well forward and evenly distributed |
| 4 | Sits unsupported, turns head and trunk to look behind |
| 5 | Sits unsupported, reaches forward to touch the floor and returns to the starting position |
| 6 | Sits on stool unsupported, reaches sideways to touch floor |
Functional Reach Test
The Functional Reach Test can also be modified from standing to sitting position.
Respiratory Function[edit | edit source]
Spinal cord injury can result in paralysis of the respiratory muscles of inspiration and expiration, which may then affect both the passive resistance of the lungs and chest wall to expansion and the active components of inspiration and expiration. With traumatic spinal cord injuries, other injuries may also be present which may impact on respiratory function including rib fractures, pneumothorax and /or haemothorax.
Respiratory function needs to be assessed with a comprehensive respiratory examination, paying particular attention to other associated thorax injuries which should include:
- Observation of the Individual
- Ventilation Method
- Type of Ventilation
- History of Ventilation
- History of Weaning
- Pattern of Breathing
- Observation of patterns of breathing is very important.
- Paradoxical Breathing. Commonly seen with diaphragmatic paralysis. The abdominal wall retracts during inspiration and protrudes during the expiration phase. This pattern, more frequent in cervical than thoracic SCI, is the result of a lack of spinal motor activation of the external intercostals combined with the excessive compliance of the abdominal wall due to weak muscle contraction. Alterations in the chest wall, lung and abdominal compliance in tetraplegia are associated with an increase in the work of breathing and may contribute to respiratory muscle fatigue[13].
- Lack of Intercostal results in ribs being drawn inwards by negative pressure in the thoracic cavity instead of Rib Elevation during Inspiration.
- Asymmetrical expansion, often associated with the effects of chest trauma or asymmetrical residual innervation of the semi-diaphragms may also be observed.
- Respiratory Rate
- Oxygen Saturation
- Heart Rate
- Temperature
- Blood Pressure
- Fluid Balance
- Auscultation
- Arterial Blood Gases
- Chest X-Ray
- Monitor for signs of Basal Collapse and Consolidation
- Altered heights of the hemi-diaphragms can be associated with partial de-innervation in high cervical lesions.
- Effectiveness of Cough
- Assessing the effectiveness of the individual's cough is essential as the ability to clear secretions can be reduced secondary to the combination of loss of abdominal generated active expiration and volume of air.
- Cough peak expiratory flow rate can be evaluated using a Peak Flow Meter and Face Mask.
- <280L/Min = Cough May Not be Effective
- 160L/Min = Ineffective Cough
- Spirometry (VC and FEV1)
- Microspirometer can be used to evaluate Forced Vital Capacity (FVC), which gives an indication of the extent of respiratory impairment by the restrictive presentation post spinal cord injury.
- Where volumes are reduced below 500ml ventilator support, either invasive or non-invasive, are generally required to reduce the risk of atelectasis, collapse and consolidation.
Cardiovascular Fitness[edit | edit source]
Assessment of cardiovascular fitness in spinal cord injury is important for the appropriate prescription of exercise programs and monitoring improvements in cardiovascular fitness. Cardiovascular fitness is assessed using standardised assessments including;
- Peak Oxygen Consumption Tests
- i.e. VO2 Peak Tests, measure expired gas while undergoing exercise that is gradually increased to the maximal intensity and is considered the Gold Standard and most accurate method of measuring cardiovascular fitness in individuals with a spinal cord injury. Equipment for Peak Oxygen Consumption Testing is expensive and generally not readily available in spinal cord injury units but are more frequently used in sports performance testing.
- Sub-maximal Arm Tests
- i.e. Coopers Test, as the name suggests, do not require an individual to exercise to exhaustion but is a method of estimating VO2 Max or "Cardiovascular Fitness" where the intensity or workload is increased at a steady rate, but only up to 85%of your maximum heart rate. Portable gas analysis, heart rate and perceived exertion using the Borg Scale can be used to quantify response to exercise.
- Field Tests
- i.e. 6 Minute Walk Test Field are simple tests that require minimal equipment. Fitness can be assessed by measuring the distance covered in a set time or the time taken to complete a set distance.
Pain[edit | edit source]
Pain, which can limit the ability to perform movement tasks and activities of daily living, is a common complication of spinal cord injury, and also has important implications for quality of life, and general feelings of happiness and well- being. There are many different types of pain which occur in association with spinal cord injury, and the characteristics, patterns of presentation, intensity and location are highly variable with some presenting at the time of the spinal cord injury while others have a more insidious onset and can present years later and involve many different areas of the body. can be assessed by a detailed subjective and objective assessment.
Assessment of Activity[edit | edit source]
Impairment in an individual with a spinal cord injury ultimately are associated with activity limitations. As with the assessment of impairments, there are many different standardised assessments of activity and activity limitations, some that are generic assessments while others are specific to spinal cord injury. The most commonly used assessments specific to spinal cord injury include the Spinal Cord Independence Measure (SCIM) and The Walking Index for Spinal Cord Injury (WISCI). Commonly assessed activity limitation domains in spinal cord injury include:
General Mobility (including Bed Mobility and Transfers)[edit | edit source]
Outcome measures that include items such as bed mobility and transfers are the Functional Independence Measure (and 5 additional mobility and locomotor items), Spinal Cord Independence Measure, Quadriplegic Index of Function and the Clinical Outcomes Variable Scale.
Wheelchair Mobility[edit | edit source]
Outcome measures that assess wheelchair mobility are the Wheelchair Skills Test, the Wheelchair Circuit and the Quebec User Evaluation of Satisfaction with Assistive Technology.
Gait[edit | edit source]
Outcome measures that assess gait are the 10 Metre Walk Test, 6 Minute Walk Test, Walking Index for Spinal Cord Injury and the Spinal Cord Injury Functional Ambulation Inventory.
Upper Limb and Hand Function[edit | edit source]
Outcome measures that assess upper limb and hand function are the Sollerman Hand Function Test, Jebsen Hand Function Test, Common Object Test, Tetraplegia Hand Activity Questionnaire, Grasp and Release Test, the Capabilities of Upper Extremity Instrument and the AuSpinal.
Assessment of Participation[edit | edit source]
Understanding the individual's involvement in activities of daily life prior to the spinal cord injury will give an indication of what their level of participation and assist in goal setting and treatment planning. It can also provide motivation for the individual during treatment if the treatment plan incorporates activities of interest to the patient. It is most useful to assess the participation domains that the patient is interested in. Commonly assessed participation domains include:
Family[edit | edit source]
Normal Daily Routine - What would the patients daily routine be? Do they do their own cooking, cleaning and other domestic tasks? What time do they tend to get up, go to bed etc.
Education[edit | edit source]
Is the individual in education? Part-Time or Full Time? School, College, University? What is the subject area? What type of activities are involved?
Work[edit | edit source]
Is the individual Employed? Unemployed? Retired? Work in the Home? What type of activities are involved?
Leisure[edit | edit source]
How does the individual normally spend their free time? What activities do they like to be involved in? Can these be incorporated into their Treatment? Sport, Art, Music, Reading, Outdoors
Environmental Factors[edit | edit source]
Environmental factors are external factors which include the physical, social and attitudinal environment in which the individual lives, which can have a positive or negative influence on their participation as a member of society, on performance of activities or on body function or structure.
Resources[edit | edit source]
Brogardh, C. & Lexell, J., The Use of ICF in the Neurorehabilitation Process , NeuroRehabilitation 36 (2015) 5–9
References[edit | edit source]
- ↑ 1.0 1.1 Ryerson S, Neurological Assessment: The Basis of Clinical Decision Making. In: Lennon S, Stokes M, editors. Pocketbook of Neurological Physiotherapy. Elsevier Health Sciences; 2008 Oct 10.
- ↑ Bernhardt J, Hill K. We Only Treat What It Occurs to us to Assess: The Importance of Knowledge-based Assessment. Science-based Rehabilitation: Theories into Practice. 2005:15-48.
- ↑ Sykes C. Health Classifications 1 - An Introduction to the ICF. WCPT Keynotes. World Confederation for Physical Therapy. 2006.
- ↑ 4.0 4.1 Rauch A, Cieza A, Stucki G. How to Apply the International Classification of Functioning, Disability and Health (ICF) for Rehabilitation Management in Clinical Practice. Eur J Phys Rehabil. 2008;44(3):329-42.
- ↑ Harvey L. Management of Spinal Cord Injuries: A Guide for Physiotherapists. Elsevier Health Sciences; 2008 Jan 10.
- ↑ 6.0 6.1 6.2 6.3 6.4 6.5 Jones K. Neurological Assessment: A Clinician's Guide. Elsevier Health Sciences; 2011 Nov 29.
- ↑ Porter S. Tidy's Physiotherapy. Edinburgh: Churchill Livingstone, 2013.
- ↑ Brodal P. The central nervous system: structure and function. Oxford University Press; 2004.
- ↑ Lance JW. Symposium synopsis. In: Feldman RG,fckLRYoung RR, Koella WP (eds). Spasticity: Disordered Motor Control. Chicago, IL: Year Book 1980:485–94.
- ↑ PT14. Goniometry for the Upper Extremity, Part 1. Available from: https://youtu.be/C86dDCYjmR8[last accessed 30/10/18]
- ↑ PT14. Goniometry for the Upper Extremity, Part 2. Available from: https://youtu.be/JkOqO1imNPg[last accessed 30/10/18]
- ↑ Jørgensen V, Elfving B, Opheim A. Assessment of unsupported sitting in patients with spinal cord injury. Spinal cord. 2011 Jul;49(7):838-43.
- ↑ Galeiras Vázquez R, Rascado Sedes P, Mourelo Fariña M, Montoto Marqués A, Ferreiro Velasco ME. Respiratory management in the patient with spinal cord injury. BioMed research international. 2013;2013. Available from: https://www.hindawi.com/journals/bmri/2013/168757/ (last accessed 28.10.2019)