Standing Flexion Test
Original Editors - Merlin Roggeman
Top Contributors - Merlin Roggeman, Rachael Lowe, Shaimaa Eldib, Admin, Kai A. Sigel, WikiSysop, Kim Jackson, Wanda van Niekerk, Lucinda hampton, 127.0.0.1, Tony Lowe and George Prudden
Definition/description[edit | edit source]
The standing flexion test is a test that can be used to assess sacroiliac joint dysfunction. It is best used in combination with other specific tests. A synonym is the Vorlauf test.
Clinically relevant anatomy[edit | edit source]
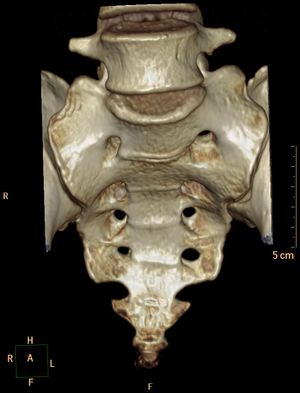
This test involves the sacroiliac joint (SIJ). It is the joint between the iliac bones of the pelvis and the sacrum (figure 1), a joint in which very little movement occurs (nutation and contranutation). It is a strong synovial joint, with both hyaline (on the sacral surface) and fibrous cartilage (on the ilial surface). Furthermore, the SIJ is reinforced by many ligaments connecting sacrum and ilium, and which tend to relax in pregnancy. “The sacroiliac joint has been implicated as a possible cause of low back pain by many authors (Grieve 1976; Erhard & Bowling 1977; Weismantel 1978; Mitchell et al. 1979; DonTigny 1985; Bernard & Kirkaldy 1987; Bourdillon et al. 1995; Schwarzer et al. 1995; Shaw 1992, Maigne et al. 1996).”[1] Some authors claim it to be a major cause of low back pain, others rather think it is an uncommon source of low back pain.[1] Therefore, the SIJ is often evaluated by clinicians who examine patients with lumbosacral pain. Assessing SIJ dysfunction is important.[1][2]
Purpose[edit | edit source]
The purpose of the standing flexion test is to assess sacroiliac joint dysfunction. This condition can result from a variety of causes, including osteoarthritis, gout, rheumatoid arthritis, pregnancy, ankylosing spondylitis, … It is a state of altered mobility within the sacroiliac joint’s range of motion, causing changes in the structural relationship between the sacrum, the ilium and one or both legs. It is characterized by:
- Reduced mobility in the affected joint, which will be noticeable when performing the standing flexion test. However, the standing flexion test alone is not enough to diagnose SIJD. Additional testing is preferable.[1][2][3][4][5]
Technique[edit | edit source]
- The patient stands erect, with his feet at shoulder width.
- The therapist stands or squats behind the patient and places his thumbs directly under each posterior superior iliac spine (PSIS).[2]
- The patient bends forward, starting with flexing the neck, then the upper thoracic spine to the lumbar spine, and as far as possible while keeping the knees extended. The therapist will observe each PSIS and their movement. Each PSIS should move an equal amount in a superior direction.[1][2]If one PSIS moves further cranial than the other, the test is positive.
- The side with the greater movement is the affected side, because an articular restriction between the ilium and sacrum occurs. The sacrum will bend forward along with the lumbar spine, and if there is an articular restriction in the SIJ, nutation will occur less in that joint than on the other side.[1][6]
Because similar findings may occur in case of contralateral hamstrings tightness, this condition should be examined too to rule out any effect of tightness. [1][2][6]
Evidence[edit | edit source]
- Little evidence has been found about the reliability and validity of the standing flexion test.
- Most studies have even found the reliability and the validity of the test to be rather low for diagnosis of sacroiliac joint dysfunction.
- In 1999 a study with a level of evidence C made by Vincent-Smith and Gibbons concerning the inter-examiner and intra-examiner reliability of the standing flexion test led to the conclusion that there is poor significant reliability both inter-examiner and intra-examiner. This means that its use for indication of sacroiliac joint syndrome remains questionable and that it must undergo further research.
- In order to investigate SIJD, a combination of different tests, such as seated flexion test, Gillett test, Rücklauf, Faber test, scral thrust, compression test [7] … is preferable.[1][2][8]
- “Cibulka et al. (1988) investigated the reliability of a combination of four palpation tests for the detection of SIJ dysfunction. This is one of the only studies in the field to report a high level of reliability (k=0.88) for such tests. The authors conclude that combining the standing flexion test, the prone knee flexion test, the supine long sitting test and palpation of the posterior superior iliac spine heights when sitting, allows an examiner to detect the presence of SIJ dysfunction.” [1]
- All articles found that the reliability of this test is questionable, and that additional tests are necessary to provide conclusive evidence. [1][2][3][8]
Clinical bottom line[edit | edit source]
- This test is indicative for sacroiliac joint dysfunction (SIJD), but only when combined with other specific tests with the same outcome.
- Medical imaging (CT-scan, MRI) may be needed to provide further evidence of SIJD[9].
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 1.7 1.8 1.9 B. Vincent-Smith, P. Gibbons. Inter-examiner and intra-examiner reliability of the standing flexion test. Manual Therapy (1999); 4(2), 87-93fckLRLevel of evidence: C
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 Nancy A. Potter, Jules M. Rothstein. Intertester Reliability for Selected Clinical Tests of the Sacroiliac Joint. Physical Therapy. 1985; 65: 1671-1675fckLRLevel of evidence: C
- ↑ 3.0 3.1 Michael T Cibulka, Anthony Delitto and Rhonda M Koldehoff. Changes in Innominate Tilt After Manipulation of the Sacroiliac Joint in Patients with Low Back Pain An Experimental Study. Physical Therapy. 1988; 68: 1359-1363fckLRLevel of evidence: C
- ↑ http://www.medicinenet.com/sacroiliac_joint_pain/page2.htm
- ↑ Kent E. Timm et al. Sacroiliac Joint Dysfunction in Elite Rowers. Journal of Orthopaedic & Sports Physical Therapy. 1999; 29(5): 288-293fckLRLevel of evidence: C
- ↑ 6.0 6.1 http://therapyprotocols.webs.com/sijdysfunctionprotocols.htm
- ↑ Hilal Telli MD, Serkan Telli MD, Murat Topal MD. The validity and reliability of provocation tests in the diagnosis of sacroiliac joint dysfunction. Pain Physician. 2018 Jul;21:E367-76.
- ↑ 8.0 8.1 P. van der Wurff, W. Meyne, R.H.M. Hagmeijer. Clinical tests of the sacroiliac joint, A systematic methodological review. Part 2: Validity. Manual Therapy (2000); 5(2): 89-96fckLRLevel of evidence: B
- ↑ Weber U, Zubler V, Zhao Z, Lambert RG, Chan SM, Pedersen SJ, Østergaard M, Rufibach K, Maksymowych WP. Does spinal MRI add incremental diagnostic value to MRI of the sacroiliac joints alone in patients with non-radiographic axial spondyloarthritis?. Annals of the rheumatic diseases. 2015 Jun 1;74(6):985-92.