Rehabilitation of Acquired Brain Injury in Disasters and Conflicts: Difference between revisions
Wendy Walker (talk | contribs) No edit summary |
No edit summary |
||
| Line 207: | Line 207: | ||
== Resources == | == Resources == | ||
[https://humanity-inclusion.org.uk/sn_uploads/uk/document/responding-disasters-dos-and-donts-guide-rehabilitation-professionals-april-2016.pdf Responding Internationally to Disasters: Do’s and Don’ts] | * [https://www.who.int/publications/i/item/emergency-medical-teams Minimum Technical Standards and Recommendations for Rehabilitation in Emergency Medical Teams] | ||
* [https://humanity-inclusion.org.uk/sn_uploads/uk/document/responding-disasters-dos-and-donts-guide-rehabilitation-professionals-april-2016.pdf Responding Internationally to Disasters: Do’s and Don’ts] | |||
* [https://hi.org/en/early-rehabilitation-in-conflicts-and-disasters Early Rehabilitation in Conflict and Disasters: A Field Handbook] | |||
* [https://get.disasterready.org/rehabilitation-treatment-planning/ Rehabilitation Treatment Planning Tool for Common Conflict and Emergency Related Injuries] | |||
* [https://www.physio-pedia.com/images/a/ae/Chapter_8_Acquired_Brain_Injury.pdf Rehabilitation in Sudden Onset Disasters] | |||
=== Profession Specific Guidelines === | |||
* [https://world.physio/sites/default/files/2020-06/Disaster-Management-Report-201603.pdf The Role of Physical Therapists in Disaster Management] | |||
* [https://wfot.org/resources/occupational-therapy-in-disaster-preparedness-and-response-dp-r Occupational Therapy in Disaster Preparedness and Response] | |||
* [https://learning.wfot.org/ Disaster Management for Occupational Therapists Online Learning Module] | |||
* [https://www.who.int/mental_health/emergencies/guidelines_iasc_mental_health_psychosocial_june_2007.pdf Iasc Guidelines on Mental Health and Psychosocial Support in Emergency Settings] | |||
[https://world.physio/sites/default/files/2020-06/Disaster-Management-Report-201603.pdf The Role of Physical Therapists in Disaster Management] | |||
[https://wfot.org/resources/occupational-therapy-in-disaster-preparedness-and-response-dp-r Occupational Therapy in Disaster Preparedness and Response] | |||
== References == | == References == | ||
Revision as of 01:27, 1 March 2022
Original Editors - Naomi O'Reilly
Top Contributors - Naomi O'Reilly, Wendy Walker, Kim Jackson, Tarina van der Stockt and Jess Bell
Introduction[edit | edit source]
While accurate data is scarce, traumatic brain injury remains a common neurological consequence of disasters and conflicts. A wide range of mild, moderate, and severe traumatic brain injury occur as a result of overpressure, gun shot wounds, a blow to the head or penetrating injury, and crush injuries following the huge kinetic energy released by rapid-onset natural disasters and armed conflict. Shockwaves from blasts, e.g. bombs or exploding debris, can cause damage to the brain as well as open or closed head injuries, with children more vulnerable due to their size and relative frailty e.g. thinner skin and softer skull bones. Non-traumatic causes of brain injury including cerebral malaria, meningitis, stroke related to cardiovascular or sickle cell disease, tumour causing pressure on the brain or near drowning, also continue to be seen in conflict and disaster settings.
Given the many potential sources of acquired brain injury, disaster preparedness planners and emergency medical personnel face a major challenge in preventing and managing neurotrauma within this context. [1] In settings of conflict or natural disaster, acquired brain injury management is particularly complex, as it is frequently complicated by the presence of poly-trauma, such as associated skull (and other) fractures, open wounds and internal injuries when in disaster and conflict settings. Individuals with acquired brain injury may face long-term physical, cognitive and behavioural impairments with residual neurological deficits, as well as medical complications, all resulting in lifestyle consequences; these necessitate comprehensive interdisciplinary management, including medical, surgical and rehabilitation. [2] All rehabilitation professionals working in disasters and conflicts should be able to provide aftercare information to patients with mild brain injury or suspected brain injury, including how to recognise signs of deterioration. [1]
Immediate Emergency Care[edit | edit source]
Early diagnosis and treatment of traumatic acquired brain injuries can be challenging under normal circumstances, and these challenges are exacerbated in the aftermath of disaster and conflicts due to to the chaotic environment including damaged infrastructure, poor communication and shortages of relevant health and rehabilitation workers, particularly neurotrauma specialists. [3]
During this early stage, immediate diagnosis and treatment is key to minimising the development of secondary brain injuries; this is a massive challenge, particularly in low resource countries where medical infrastructure and availability of state-of-the-art neurological care is already scare and may be further limited as a result of disaster or conflict. Family members are often separated, and symptoms of post traumatic stress disorder can be common during the post acute phase.
As a result, early deployment of specialised emergency medical teams to meet the immediate needs of disaster victims is a key element of the immediate emergency response, and is guided by a range of World Health Organization initiatives, including Emergency Response Frameworks (Standards and Guidelines); Coordination Mechanisms, and the Emergency Medical Team Accreditation Process ensuring that rehabilitation professionals form part of the Emergency Medical Teams. [3][4]
Specialised care teams are defined by the World Health Organization as “National or International teams embedded into Emergency Medical Teams or a National Facility to provide specialist care”, which may include rehabilitation teams; they are deployed based on the response required to meet specific needs at the request of the host health authorities. These teams should be multidisciplinary and need to be integrated into a disaster or conflict response and management plan and their skills need to be shared with local rehabilitation and health-care providers through mentoring and educating/training." [2]
A specialised care team that is focused on traumatic brain injury rehabilitation in a disaster or conflict setting should include: [2][4]
| Rehabilitation Interventions | General Applicability of Recommendations in Disaster Settings | |
|---|---|---|
| Weak | ||
| Team Composition | Minimum Technical Standard;
A traumatic brian injury specialised rehabilitation team should be led by a rehabilitation physician and comprise of at least three other professionals from different disciplines, including rehabilitation medicine, nursing, physiotherapy, occupational therapy, speech and language therapy, and psychology. In addition, a team lead is required to represent the care team at health coordination level | |
| Qualification and Experience | Minimum Technical Standard;
Rehabilitation professionals in a traumatic brian injury specialised care team should have at least 6 months’ experience working in a traumatic brain injury unit or with traumatic brain injury patients in a major trauma center and at least 3 years of postqualifying clinical experience At least one team member, preferable the team leader, should have experience in emergency response and all team members should have undergone training in working in austere environments | |
| Rehabilitation Equipment | Minimum Technical Standard;
Specialized care teams for rehabilitation should have capability to rapidly provide the equipment here. | |
| Length of Stay | Minimum Technical Standard;
A team that embeds into a local facility should plan to stay for at least 1 month with evidence of a exit strategy and release mechanism. | |
Early Rehabilitation[edit | edit source]
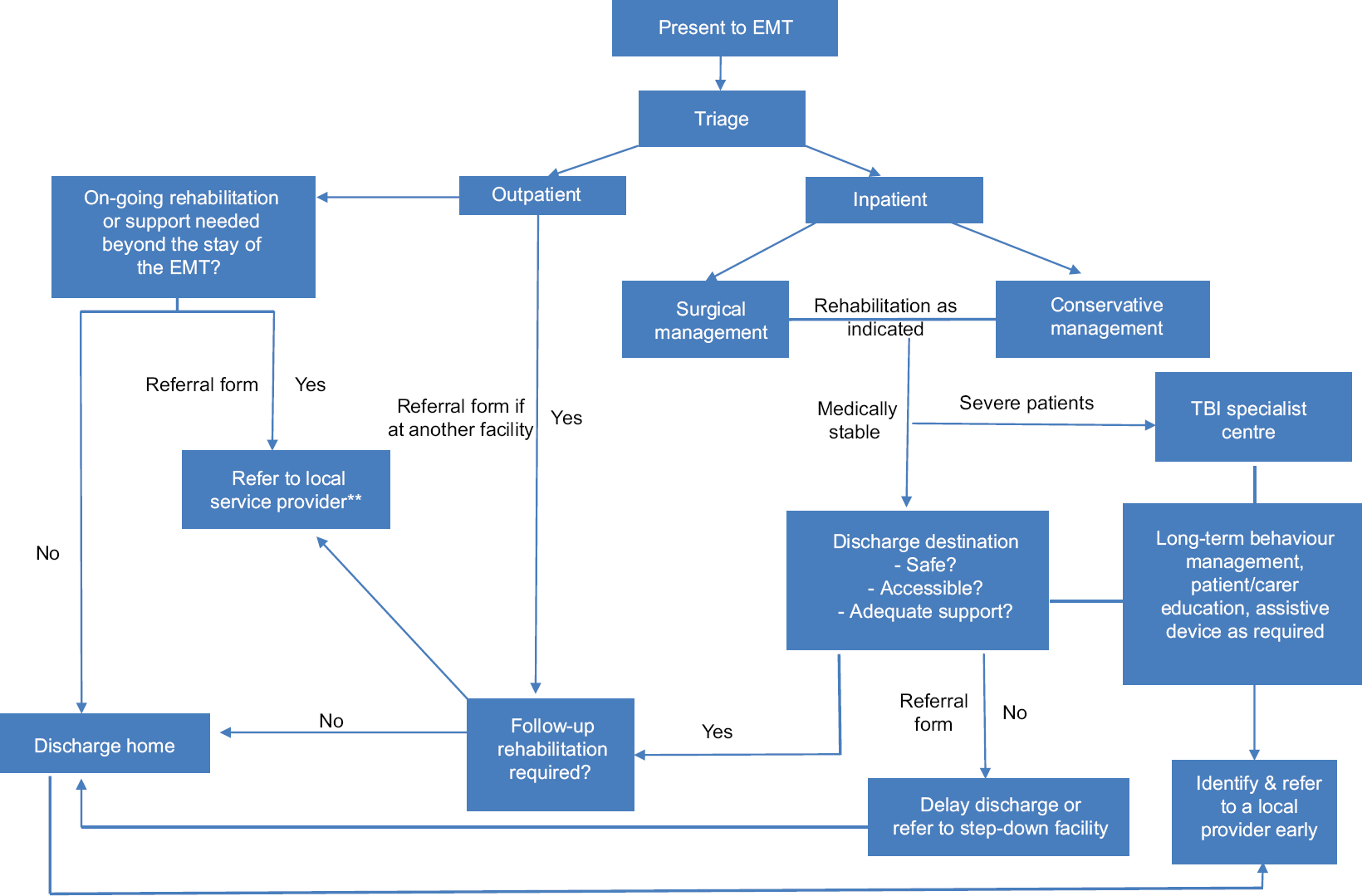
The overriding objective of acquired brain injury care in disaster settings has now extended well beyond survival and acute management to include implementation of rehabilitation structures which work towards reintegration of the individual with an acquired brain injury back into home and community. The World Health Organization's minimum standards for rehabilitation recommendations for managing patients with traumatic brain injury following a disasters include: [2][5]
- Cognitive and neurological changes should be monitored and regularly assessed
- Early referral to a step-down facility using local rehabilitation providers and support networks, as required
- Appropriate mobility aids prescribed for mobility deficits using local service provider
- Patients with long term or permanent nerve injury considered for orthotic device, sought from a local provider
- Referral pathways identified for microsurgery for appropriate patients
Rehabilitation is a vital element of the treatment and management process post traumatic brain injury in a disaster setting and should prepare individuals with long-term impairment, their care providers and local rehabilitation personnel to manage their ongoing needs over a longer term and should be started early following any disaster.[5] Early rehabilitation should focus on comprehensive assessment for neurological and functional limitations and individualised treatment programs for specific functional goals with ongoing monitoring of outcomes. The goal of early rehabilitation in a disaster setting is to improve functional outcomes and restore as much independence in the patient as possible, while minimising secondary complications, with an emphasis on patient and care giver education about realistic expectations and self-management strategies. Survivors of traumatic brain injury need support for acquisition of essential skills for maximum return to their previous level of functional independence, regardless of whether specific impairments can be eliminated. [2]
Guidelines[edit | edit source]
Independently extracted, compared, and categorised evidence-based rehabilitation intervention recommendations for rehabilitation interventions were synthesised from currently published traumatic brain injury Clinical Practice Guidelines, developed by the Department of Labor and Employment (DLE); Scottish Intercollegiate Guidelines Network (SIGN); Department of Veterans Affairs/Department of Defence (DVA/DOD); and American Occupational Therapy Association (AOTA) for applicability in disaster settings. [5] As a result of the complexities related to the environment, resources, service provision, and workforce in disaster and conflict settings many recommendations for traumatic brain injury care are challenging to implement, and more advanced interventions are generally not applicable due to limited access to services, trained staff/resources, equipment, funding, and operational issues.[5]
Patient/carer education, general physical therapy, practice in daily living activities and safe equipment use, direct cognitive/behavioural feedback, basic compensatory memory/visual strategies, basic swallowing/communication, and psychological input are the key recommendations from a rehabilitation perspective that have been found to be most applicable for survivors of acquired brain injury in disaster and conflict settings. The following table outlines the general applicability of clinical practice guidelines for acquired brain injury in disaster and conflict settings.[5]
| Rehabilitation Interventions | General Applicability of Recommendations in Disaster Settings | ||
|---|---|---|---|
| Weak | Moderate | Strong | |
| Patient Education |
| ||
| Gait, Balance and Mobility |
|
Task-Specific Training
Repetitive Training |
|
| Spasticity and Muscle Tone |
|
|
|
| Sleep Disturbance Management |
| ||
| Cognitive Rehabilitation |
|
|
|
| Behavioural and Emotional Disorders |
|
Comprehensive Neurobehavioural Program
|
|
| Activities of Daily Living |
|
|
|
| Post-Traumatic Headache Management |
|
| |
| Service Delivery |
|
|
|
Summary[edit | edit source]
“Early rehabilitation can greatly increase survival and enhance the quality of life for injured survivors.”[6]
Current advances in disaster and conflict response and management have improved survival rates for those with acquired brain injury, resulting in increased number of survivors. Traumatic brain injury is one of the more common complex injuries post sudden onset disaster and survivors often have long-term physical, cognitive and behavioural disabilities, residual neurological deficits, medical complications and lifestyle consequences, which necessitate comprehensive interdisciplinary management, including medical, surgical and rehabilitation. The goal of early rehabilitation in disaster and conflict settings is to improve functional independence and successful reintegration into the community, with an emphasis on patient education about realistic expectations and self-management strategies. [2][1]
Rehabilitation professionals are now considered key health care members and as such are involved in all phases following disasters and conflicts, including early involvement with emergency medical teams. Several unique areas of skill are offered by rehabilitation professionals, including those of assessing and treating casualties with acute injuries, and possibly preventing or lessening the burden of chronic dysfunction amongst patients after the emergency phase, with a major strength being our focus on functional outcomes combined with the ability to carry out thorough assessments, often with limited resources. [2][1]
Resources[edit | edit source]
- Minimum Technical Standards and Recommendations for Rehabilitation in Emergency Medical Teams
- Responding Internationally to Disasters: Do’s and Don’ts
- Early Rehabilitation in Conflict and Disasters: A Field Handbook
- Rehabilitation Treatment Planning Tool for Common Conflict and Emergency Related Injuries
- Rehabilitation in Sudden Onset Disasters
Profession Specific Guidelines[edit | edit source]
- The Role of Physical Therapists in Disaster Management
- Occupational Therapy in Disaster Preparedness and Response
- Disaster Management for Occupational Therapists Online Learning Module
- Iasc Guidelines on Mental Health and Psychosocial Support in Emergency Settings
References [edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 Lathia C, Skelton P, Clift Z. Early rehabilitation in conflicts and disasters. Handicap International: London, UK. 2020.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 Amatya B, Vasudevan V, Zhang N, Chopra S, Astrakhantseva I, Khan F. Minimum technical standards and recommendations for traumatic brain injury rehabilitation teams in sudden-onset disasters. The Journal of the International Society of Physical and Rehabilitation Medicine. [serial online] 2018 [cited 2019 Oct 19];1:72-94. Available from: http://www.jisprm.org/text.asp?2018/1/2/72/249854
- ↑ 3.0 3.1 Regens JL, Mould N. Prevention and treatment of traumatic brain injury due to rapid-onset natural disasters. Frontiers in public health. 2014 Apr 14;2:28.
- ↑ 4.0 4.1 Vasudevan V, Amatya B, Chopra S, Zhang N, Astrakhantseva I, Khan F. Minimum technical standards and recommendations for traumatic brain injury specialist rehabilitation teams in sudden-onset disasters (for Disaster Rehabilitation Committee special session). Annals of Physical and Rehabilitation Medicine. 2018 Jul 1;61:e120.
- ↑ 5.0 5.1 5.2 5.3 5.4 Lee SY, Amatya B, Judson R, Truesdale M, Reinhardt JD, Uddin T, Xiong XH, Khan F. Applicability of traumatic brain injury rehabilitation interventions in natural disaster settings. Brain injury. 2019 Aug 24;33(10):1293-8. DOI: 10.1080/02699052.2019.1641748
- ↑ Sphere. The Sphere Handbook 2018 Humanitarian Charter and Minimum Standards for Humanitarian Response. 2018 Available form: https://www.spherestandards.org/handbook-2018/