Swan-Neck Deformity
Original Editor - Boaz Telfort
Top Contributors - Beverly Klinger, Shaimaa Eldib, Boaz Telfort, Kim Jackson, Chrysolite Jyothi Kommu, Nikhil Benhur Abburi, Wanda van Niekerk and Anas Mohamed
Definition/Description[edit | edit source]
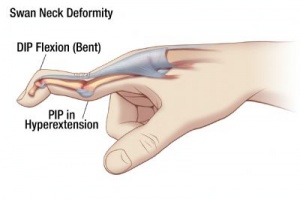
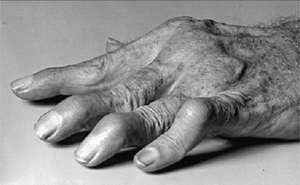
Swan-Neck Deformity (SND) is a deformity of the finger characterized by hyperextension of the proximal interphalangeal joint (PIP) and flexion of the distal interphalangeal joint (DIP). Reciprocal flexion of the metacarpal phalangeal joint (MCP) can also be present. A Swan-Neck Deformity is caused by an imbalance to the extensor mechanism of the digit. The deformity develops when there is a loss of extension at the distal phalanx or tightening of the extensor mechanism at the proximal phalanx,both intrinsic and extrinsic, at the PIP joint.[1]
Etiology/Epidemiology[edit | edit source]
Swan-Neck Deformity is initially caused by damage to the attachment of the extensor tendon.[2] Injury to the extensor tendon can be caused by a traumatic laceration, a closed avulsion from a direct blow to the DIP while digit is extended, or by weakening at the DIP from chronic inflammation as well as extensor tendon subluxation due to an inflammatory disease most commonly rheumatoid arthritis.[1]
Damage to the extensor mechanism results in laxity at the volar plate and tightness at the triangular ligament around the proximal interphalangeal (PIP). [1] The resulting shape looks similar to a swan’s neck, which is how the condition got its name.[2]
Swan-Neck Deformity can be caused by a variety of conditions such as rheumatoid arthritis[3][4], untreated mallet finger, various disorders such as cerebral palsy[5], stroke, Parkinson’s disease, traumatic brain injury, psoriatic arthritis, scleroderma, and hand trauma.[1]
Characteristics/Clinical Presentation[edit | edit source]
A patient with Swan-Neck Deformity may present with a history of inflammatory diseases such as rheumatoid arthritis or trauma to the extensor mechanism of the digit.[1] Upon examination, the patient may present with inflammation of the joints, stiffness in the fingers, and a gradual difficulty in flexion at the PIP. A snapping sensation may also occur during flexion.[6]
Staging[edit | edit source]
The Nalebuff classification system is most commonly used to classify the severity of a Swan-Neck Deformity. This classification system is based on the PIP joint stiffness with associated MCP joint positions.[1]
- Type 1: PIP joint is flexible in all positions of the MCP joint.
- Type 2: PIP joint flexion is limited in certain positions of the MCP joint.
- Type 3: PIP joint flexion is limited irrespective of the position of the MCP joint.
- Type 4: PIP joints are stiff and have a poor radiographic appearance.
Evaluation[edit | edit source]
Active and passive Range of Motion should be assessed at the MCP, PIP, and DIP independently. In the early stages it is possible for the PIP joint to maintain flexibility, however will return to deformity when the full digital extension is performed. In the later stages, the PIP will present with increased stiffness and could possibly be fixed into hyperextension. Along with manual testing, a patient should be screened for rheumatoid arthritis and x-rays should be ordered to evaluate for articular disruption, severe arthritis in the later stages, or even carpal collapse.[1]
In order to determine whether a patient is presenting with a capsular restriction or intrinsic tightness, a Bunnell-Littler Test (Finochietto-Bunnell test) is performed. The Bunnell-Littler test is performed by holding the MCP in an extended position while passively flexing the PIP, noting the available ROM. The test is then repeated with the MCP flexed. If there is no change in motion between the two tests, then capsular restriction at the PIP joint is suggested. If the motion increases when the MCP is flexed, then intrinsic muscle tightness is suggested.[1]
Treatment/Management[edit | edit source]
There are many treatments available for this deformity, depending on the condition’s severity. There are two categories of treatment: surgical and non-surgical.
Non-Surgical/Conservative[edit | edit source]
Hand therapy for passive stretching combined with corrective splinting may benefit even chronic conditions. This combination of treatment may increase mobility and flexibility at both the DIP and the PIP joints. Extension block splints may help correct the hyperextension at the PIP joint. Progressive extension splinting can help improve the DIP flexion deformity. Although stretching and splinting may increase mobility. Severe or long-standing deformities will not likely achieve true correction without surgery[8]. An oval 8 splint can be used to correct deformity in the initial stages
Thermoplastic materials with a width of 0.5mm and length of 10cm can be used to fabricate custom made splints. making can be viewed here
Surgical[edit | edit source]
If a patient presents in the early stages of a swan neck deformity, a volar restraint must be developed during surgery to recreate the action of the volar plate. Flexor Digitorum Superficialis Tenodesis (FDS) is a common procedure to help prevent hyperextension. If a DIP joint mallet deformity is present, however, and a lateral band laxity has already formed then a conjoint lateral band tenodesis can be performed to correct both deformities as long as the anatomy is intact. [1]
PIP joint hyperextension can be corrected by lengthening the central slip, by tethering the joint in flexion using an FDS tenodesis or by performing a dermodesis (removing an ellipse of skin on the volar aspect of the joint). A release of the intrinsic muscle contributing to the central slip can also be performed if intrinsic tightness is also evident.[1]
In the later stages of a swan neck deformity when PIP arthrosis is evident, a joint fusion or replacement may be indicated along with soft tissue procedures that will still be necessary. Arthroplasty of the MCP joints can also be performed if a subluxation is occurring due to severe degenerative arthritis. [1]
Postoperative and Rehabilitation Care[edit | edit source]
The hand should be immobilised in a plaster splint with the MCP joints in full extension and PIP joints flexed. Active flexion exercises should begin within the first 4 to 5 days if flexor tenosynovectomy has been performed. Dorsal extension blocking should be placed until 4 to 6 weeks postoperatively[8].
This video details how to use an Oval-8 Finger Splint for Swan Neck Deformity injuries.
Differential Diagnosis[edit | edit source]
The boutonniere deformity can be mistaken for a swan-neck deformity. It is important to recognize that boutonniere deformity consists of hyperextension of the DIP and flexion of the PIP.[11]
References[edit | edit source]
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 Lane R, Nallamothu SV. Swan-Neck Deformity. InStatPearls [Internet] 2019 Feb 4. StatPearls Publishing.
- ↑ 2.0 2.1 MedicalNewsToday. What's to know about swan neck deformity. Available from: https://www.medicalnewstoday.com/articles/318642.php (accessed 15 February 2019)
- ↑ Brulard C, Sauvage A, Mares O, Wavreille G, Fontaine C. Treatment of rheumatoid swan neck deformity by tenodesis of proximal interphalangeal joint with a half flexor digitorum superficialis tendon. About 23 fingers at 61 months follow-up. Chirurgie de la main. 2012 Jun;31(3):118-27.
- ↑ Chinchalkar SJ, Lanting BA, Ross D. Swan neck deformity after distal interphalangeal joint flexion contractures: a biomechanical analysis. Journal of Hand Therapy. 2010 Oct 1;23(4):420-5.
- ↑ Carlson EJ, Carlson MG. Treatment of swan neck deformity in cerebral palsy. The Journal of hand surgery. 2014 Apr 1;39(4):768-72.
- ↑ ASSH. Swan Neck Deformity. Available from: http://www.assh.org/handcare/hand-arm-conditions/swan-neck-deformity (accessed 15 February 2019)
- ↑ Dr. Donald Ozello. Bunnell-Littler Test AKA Finochietto-Bunnell Test. Available from: https://www.youtube.com/watch?v=GpBrc5CIEVk [Last accessed 19/10/2020]
- ↑ 8.0 8.1 Lane R, Nallamothu SV. Swan-Neck Deformity. InStatPearls [Internet] 2018 Sep 10. StatPearls Publishing.
- ↑ Orfit Industries. Anti swan neck orthosis (Orfit Strips) - Splinting techniques 7/10. Available from: https://www.youtube.com/watch?v=9Gx5W_Ux6oE [last accessed 31/5/2021]
- ↑ 3 Point Products. How to Treat Swan Neck Deformity with an Oval-8 Finger Splint. Available from: https://youtu.be/Dv_fTqEeFGQ
- ↑ McKeon KE, Lee DH. Posttraumatic boutonniere and swan neck deformities. JAAOS-Journal of the American Academy of Orthopaedic Surgeons. 2015 Oct 1;23(10):623-32.