Orthoses for Management of Neuromuscular Impairment
Original Editors - Rucha Gadgil
Top Contributors - Rucha Gadgil, Naomi O'Reilly and Kim Jackson
Introduction[edit | edit source]
The neuromuscular system can be called as the biomechanical apparatus through which the CNS executes postural actions[1]. It includes all the muscles in the body and the nerves serving them.
The term ‘neuromuscular disorders' encompasses conditions which affect either the muscles, such as those in the arms and legs or heart and lungs, or the nerves which control the muscles[2]. Common examples may include: Cerebral palsy, Stroke, Spinal cord injury, Post-polio syndrome, Muscular dystrophies, Spinal muscular atrophy,etc.
Impairments in these diseases may vary widely by person and condition, in type and severity, and may include:
- increased or decreased tone,
- atrophied muscle mass, weakness,
- muscle twitching, shaking, cramping,
- stiff or tight muscles (spasticity),
- walking on the toes,
- a crouched gait,
- drop foot, numbness and tingling
- balance problems, loss of postural control
These impairments often cause mobility problems and affect the quality of life of the individual adversely. They have to rely on assistive devices like orthoses to improve function and mobility. Recommendations for orthoses can be made by a physiotherapist, an orthotist, or a doctor[3].
Types of orthoses[edit | edit source]
The main aim of using orthoses for neuromuscular impairments is:
- improving the quality of life
- independence
- maintaining optimal functioning of muscles
The orthoses should fulfill the following criteria for an individual:
- Optimal Alignment
- Stability
- Prevent contractures
- Flexibility
The orthoses used can be divided into:
- Lower limb orthoses[4]:
- shoe inserts
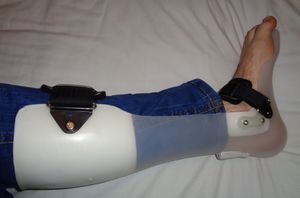
- ankle-foot orthoses (AFO): AFOs are the most common and vary greatly in the design and the types of materials used. AFOs may be solid or hinged at the ankle and may have a removable foot plate.
- knee-ankle-foot orthoses (KAFO) and
- hip-knee-ankle-foot-orthoses (HKAFO).
- Cervical orthoses: to assist in positioning head and neck in case of muscle weakness. eg. in ALS patients
- Thoracolumbosacral orthoses (TLSOs) correct spinal curvatures, scoliosis, and can improve balance and stability as well as control of the extremities, head, neck and trunk.
- Upper limb orthoses:
- Wilmington Robotic Exoskeleton (WREX): a functional upper limb orthosis designed to enhance movement for individuals with neuromuscular disabilities.[5]
- Hand Splints
- Functional electric stimulation (FES) devices: alternative to traditional orthoses. They generate an electrical current stimulating a muscle causing muscle contraction in a predictable movement pattern creating a physiological bracing[6].These have shown gait improvements when compared to traditional AFO.
Assessment[edit | edit source]
The clinician has to identify the impairments and functional limitations, understand the prognosis, take into account the lifestyle and risk factors before selecting the most appropriate treatment method and/or assistive device.
It is important to assess the body holistically when planning a rehabilitation programme. This may include evaluation of[3]
- muscle testing, normal joint movement,
- evaluation of flexibility,
- evaluation of motor and sensory functions, and functional capacities,
- functional posture, and gait analysis
- respiratory functions.
Orthotic prescription has to be preceded by a complete biomechanical assessment, gait analysis (for lower limb), functional assessment and patient counselling and education. Each orthosis has to be custom made and proper fitting to avoid complications.
Fitting and Measurements[edit | edit source]
It is important to consider the fitting of the orthoses for the individual. Weight of the material of the device also has to be taken into account. The measurements of the limb can be taken by:
- measuring tape
- plaster cast
- computer scanner
- foam prints/ ink prints
- 3D scanner[7]
For measuring for an AFO:
Complications and Barriers[edit | edit source]
There are some complications can arise with orthotic management:
- pressure sores and broken skin[9]
- infection, and
- pain
- inadequate support/stabilization
Thus, it is important to evaluate the skin, neurological function, vascular status, and musculoskeletal system regularly in patients who will be using an orthosis.
It is also important to re-evaluate a device fitting regularly and alter the dimensions of the orthosis as required.
There may be several barriers to device utilization, such as:
- appearance,
- weight,
- ability to don and doff the orthoses
- incorrect understanding of environmental needs and requirements.
It is important for the entire medical team to work in conjunction with the patient to overcome them[10].
Evidence[edit | edit source]
Lower Limb Orthoses[edit | edit source]
A study eliciting users’ perspectives regarding fitting, acceptability, effectiveness and use of orthoses, in adults with knee instability related to neuromuscular disorders or central nervous conditions found that effectiveness, reliability, comfort and durability were the most valued features of orthoses, and the participants' relied on orthotic devices to enable engagement in daily activities. However, obtaining suitable footwear alongside orthotic devices was notified as a significant concern[11].
Research evidence supporting clinical recommendations for ankle-foot orthotic (AFO) prescription in neuromuscular impairments demonstrated demonstrated improvement in walking speed and ankle dorsiflexion, and highlighted future research needs to provide detailed information on type and severity of lower limb impairment of participants and design features of the AFO intervention[12]. The literature supports the use of AFO in neuromuscular impairments by demonstrating improved gait, functional mobility, and energy efficiency[13].
Spinal Orthoses[edit | edit source]
The use of spinal braces/orthoses for neuromuscular impairments is still an under-studied field. The use of dynamic spinal brace for neuromuscular scoliosis found positive results. The study showed improved sitting stability and caregiver satisfaction[14].
In children with cerebral palsy, studies have reported that spinal orthoses can provide functional benefits such as stability, head control ,and hand control, improving the child's functional abilities that are vital to their quality of life[15]. The main indication for spinal orthoses in these patients is to stabilize and delay the progression of the spinal curvature[16].
Upper Limb Orthoses[edit | edit source]
In individuals with Upper Limb impairments a novel, articulated upper-extremity orthosis, the Wilmington Robotic Exoskeleton (WREX), has shown good results in regards to improved function and usage of the arm[17]. Another study rated a child's performance and satisfaction while partaking in important activities both with and without the exoskeleton device (WREX). The results showed a statistically significant improvement in arm function for everyday tasks, both in performance and satisfaction with the WREX[18].
FES[edit | edit source]
These devices act through circuitry and programming to substitute for a deficit in the neural system to restore function. A systematic review on stroke patients provided moderate-quality evidence that both ankle-foot orthoses and continuous functional electrical stimulation improved walking speed after stroke, but the effects on balance remained unclear. The authors also underlined the need for further long-term, high-quality RCTs[19].
Conclusion[edit | edit source]
There have been innumerable advances in materials, 3-D printing, and robotic exoskeletons that are changing manufacturing, overall function, and level of assistance provided by orthotic devices[20]. The picture of orthotic management is constantly changing with advent of newer technological advances, and this demands indepth study and research to keep pace with the advances.
References [edit | edit source]
- ↑ Alghwiri A, Whitney S; Guccione's Geriatric Physical Therapy, (Fourth Edition), Mosby,2020.
- ↑ Potikanond, S., et al. Muscular Dystrophy Model. Adv Exp Med Biol, 2018; 1076: 147-172.
- ↑ 3.0 3.1 Demir Y. Neuromuscular Diseases and Rehabilitation, Neurological Physical Therapy, Toshiaki Suzuki, IntechOpen, 2017. DOI: 10.5772/67722. Available from: https://www.intechopen.com/books/neurological-physical-therapy/neuromuscular-diseases-and-rehabilitation
- ↑ Webster J, Murphy D. Atlas of Orthoses and Assistive Devices. 5th Edition. Elsevier. 2017
- ↑ Rahman T, Sample W, Jayakumar S, King MM, Wee JY, Seliktar R, Alexander M, Scavina M, Clark A. Passive exoskeletons for assisting limb movement. J Rehabil Res Dev. 2006 Aug-Sep;43(5):583-90. doi: 10.1682/jrrd.2005.04.0070. PMID: 17123200.
- ↑ Prenton S, Hollands K, Kenney L, Onmanee P. Functional electrical stimulation and ankle foot orthoses provide equivalent therapeutic effects on foot drop: A meta-analysis providing direction for future research. J Rehabil Med. 2018;50(2):129-139. doi:10.2340/16501977-2289
- ↑ Telfer, S., Woodburn, J. The use of 3D surface scanning for the measurement and assessment of the human foot. J Foot Ankle Res 3, 19 (2010). https://doi.org/10.1186/1757-1146-3-19
- ↑ Foot and Ankle Associates of North Texas. AFO - Measuring Leg Size. Available from: https://www.youtube.com/watch?v=gwVl_LipyGg [Last accessed: 16 June 2021]
- ↑ Witherow E, Peiris C. Custom-Made Finger Orthoses Have Fewer Skin Complications Than Prefabricated Finger Orthoses in the Management of Mallet Injury: A Systematic Review and Meta-Analysis; Archives of Physical Medicine and Rehabilitation, 2015; 96(10):1913-1915. https://doi.org/10.1016/j.apmr.2015.04.026.
- ↑ Boyce SH, Quigley MA, Campbell S. Management of ankle sprains: A randomised controlled trial of the treatment of inversion injuries using an elastic support bandage or an aircast ankle brace. Br J Sports Med. 2005. doi:10.1136/bjsm.2003.009233
- ↑ McCaughan D, Booth A, Jackson C, et alOrthotic management of instability of the knee related to neuromuscular and central nervous system disorders: qualitative interview study of patient perspectivesBMJ Open 2019;9:e029313. doi: 10.1136/bmjopen-2019-029313
- ↑ Chisholm AE, Perry SD. Ankle-foot orthotic management in neuromuscular disorders: recommendations for future research. Disabil Rehabil Assist Technol. 2012 Nov;7(6):437-49. doi: 10.3109/17483107.2012.680940. Epub 2012 Apr 25. PMID: 22533384.
- ↑ Betancourt JP, Eleeh P, Stark S, Jain NB. Impact of Ankle-Foot Orthosis on Gait efficiency in Ambulatory Children with Cerebral Palsy. Am J Phys Med Rehabil. March 2019:1. doi:10.1097/PHM.0000000000001185
- ↑ Nakamura N, Uesugi M, Inaba Y, Machida J, Okuzumi S, Saito T. Use of dynamic spinal brace in the management of neuromuscular scoliosis: a preliminary report. J Pediatr Orthop B. 2014 May;23(3):291-8. doi: 10.1097/BPB.0000000000000034. PMID: 24476687.
- ↑ Pettersson, Katina and Rodby-Bousquet, Elisabet. ‘Prevalence and Goal Attainment with Spinal Orthoses for Children with Cerebral Palsy’. 1 Jan. 2019 : 197 – 203.
- ↑ Olafsson Y, Saraste H, Al-Dabbagh Z. Brace treatment in neuromuscular spine deformity. J Pediatr Orthop. 1999; 19: 376-379.
- ↑ Haumont T, Rahman T, Sample W, M King M, Church C, Henley J, Jayakumar S. Wilmington robotic exoskeleton: a novel device to maintain arm improvement in muscular disease. J Pediatr Orthop. 2011 Jul-Aug;31(5):e44-9. doi: 10.1097/BPO.0b013e31821f50b5. PMID: 21654447.
- ↑ Shank TM, Wee J, Ty J, Rahman T. Quantitative measures with WREX usage. IEEE Int Conf Rehabil Robot. 2017 Jul;2017:1375-1380. doi: 10.1109/ICORR.2017.8009440. PMID: 28814012.
- ↑ Nascimento LR, da Silva LA, Araújo Barcellos JVM, Teixeira-Salmela LF. Ankle-foot orthoses and continuous functional electrical stimulation improve walking speed after stroke: a systematic review and meta-analyses of randomized controlled trials. Physiotherapy. 2020 Dec;109:43-53. doi: 10.1016/j.physio.2020.08.002. Epub 2020 Aug 20. PMID: 33120054.
- ↑ Ford C, Grotz R, Kope Shamp J. The Neurophysiological Ankle-Foot Orthosis. Clin Prosthes Orthot. 1986;10:15-23.