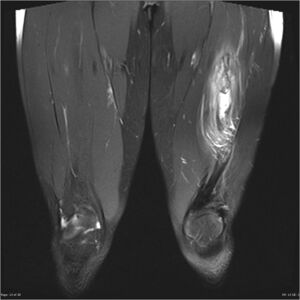
Myositis Ossificans
Original Editor - Lucinda hampton
Top Contributors - Lucinda hampton, Kim Jackson and Ahmed M Diab
Introduction[edit | edit source]
Myositis ossificans (MO) is the most common form of heterotopic ossification (HO), usually within large muscles.[1]
- Some doctors view MO and HO as two points on the same line. They are similar problems that cause pain, local signs of inflammation, and loss of motion.
- In both cases, bone forms in and around soft tissue (usually muscle).
- Myositis ossificans (MO) occurs after trauma to the muscle or a broken bone. New bone cells form between the torn muscle fibers. This happens most often around the elbow or thigh. Children and young adults are affected most often[2].
- Severe muscle contusions can trigger the myositis ossificans, causing bone to form within the injured muscle tissue. [3]
Epidemiology[edit | edit source]
Most cases of myositis ossificans occur as a result of trauma, and thus, the primary demographic is young adults. Another group which is especially prone to myositis ossificans are paraplegics, usually without evidence of trauma.[1]
Clinical presentation[edit | edit source]
Typically presents as a painful, tender, enlarging mass, which in 80% of cases is located in large muscles of the extremities, often following recognized local trauma, although a definite traumatic event is not always recalled.
- In the case of paraplegics, recognized episodes of trauma are often absent, and the disease occurs particularly around the knees and hips[1].
- Myositis ossificans is a rare condition that may develop following a quadriceps contusion, see MO of the Quadriceps. Quadriceps contusions occur following a direct impact to the quadriceps muscle from an object or person. This most commonly occurs due to a collision with another player during contact sports such as football or rugby, or from an impact from a ball in sports such as hockey or cricket.[4]
Pathology[edit | edit source]
Myositis ossificans is essentially metaplasia of the intramuscular connective tissue resulting in extraosseous bone formation (without inflammation).
Unfortunately, the histologically of myositis ossificans can appear similar to osteosarcoma, and thus, can lead to inappropriate management.[1]
Diagnosis[edit | edit source]
A thorough subjective and objective examination from a physiotherapist can usually predict the likelihood of the presence of myositis ossificans.
An X-ray approximately three weeks after the injury is usually required to confirm diagnosis. Further investigations such as an MRI scan or Ultrasound may be required, in some cases, to assist with diagnosis.[4]
- Advanced cross-sectional imaging alone can be nonspecific and may appear to be similar to more sinister etiologies. Therefore, the evaluation of a suspicious soft-tissue mass often necessitates multiple imaging modalities for accurate diagnosis.
- When imaging is indeterminate, biopsy may be required for a histologic diagnosis. However, histopathology varies based on stage of evolution. [5]
Physiotherapy[edit | edit source]
The best strategy to manage this condition is to prevent its occurrence. Once myositis ossificans is established, there is very little that can be done to accelerate the resorptive process (i.e. the process of removing bone from the bruised region). Treatment will usually focus on rest from aggravating activities and the implementation of gentle pain-free range of movement exercises.
See Physiotherapy section in
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 Radiopedia MO Available:https://radiopaedia.org/articles/myositis-ossificans-1 (accessed 24.10.2021)
- ↑ eOrthopod.com What’s the difference between myositis ossificans and heterotopic ossification? Available:https://eorthopod.com/faq/whats-the-difference-between-myositis-ossificans-and-heterotopic-ossification/ (accessed24.10.2021)
- ↑ Larson CM, Almekinders LC, Karas SG, Garrett WE. Evaluating and managing muscle contusions and myositis ossificans. The Physician and Sportsmedicine. 2002 Feb 1;30(2):41-50. [1]
- ↑ 4.0 4.1 Physio advisor Myositis Ossificans Available: https://www.physioadvisor.com.au/injuries/thigh/myositis-ossificans/ (accessed 24.10.2021)
- ↑ Walczak BE, Johnson CN, Howe BM. Myositis ossificans. JAAOS-Journal of the American Academy of Orthopaedic Surgeons. 2015 Oct 1;23(10):612-22. Available:https://pubmed.ncbi.nlm.nih.gov/26320160/ (accessed 24.10.2021)