ICF and Application in Clinical Practice
Original Editor - Ewa Jaraczewska based on the course by Patricia Saleeby
Top Contributors - Ewa Jaraczewska, Jess Bell and Tarina van der Stockt
Introduction[edit | edit source]
The comprehensive and holistic nature of the International Classification of Functioning, Disability and Health (ICF) makes it extremely useful in clinical practice.[1] The primary purpose of applying the ICF in clinical practice is to establish a common language for defining health and health-related states between providers.[2] It can enhance decision-making among healthcare and social care professionals. The ICF's holistic approach is essential for making more informed assessments, developing more effective interventions, and achieving good patient outcomes.[1]
Overview of ICF[edit | edit source]
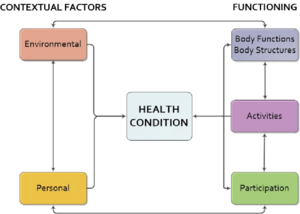
The ICF defines the interaction between health conditions, personal and social factors, daily activities, and social life.[3] The relationship between these various domains and components is reciprocal, which explains how they interact by mutually influencing one another. [1]
The following are characteristics of the ICF:[4]
- The ICF is universal: it applies to all people regardless of age, gender, socioeconomic status and health condition.
- The ICF is neutral: it does not relate a person's functioning to the cause of their health status.
- The ICF uses neutral language when describing health and health-related states.
- The ICF provides a continuum between functioning and disability.
Framework[edit | edit source]
The ICF is a biopsychosocial model of functioning, health and disability. Using standard language to define and measure disability, the ICF helps to explain how a person's body problems and social circumstances affect their functioning.
Definitions for the ICF Domains/Components[edit | edit source]
In the ICF model, a person is viewed in terms of their health conditions, body functions and structures, activities and participation, and environmental and personal factors.[1]
- Health Condition: "an umbrella term for the disease, disorder, injury, trauma"[4]
- Body Functions: "physiological functions of the body system, including psychological functions"[4]
- Body Structures: "anatomical parts of the body, such as organ, limbs and their components"[4]
- Activity: "execution of a task or action by an individual".[4] Activity limitations describe the problems or issues at the level of the individual.[1]
- Participation: "involvement in a life situation".[4] Participation restrictions are problems the individual may experience in their life situation or within an environmental context.[1]
- Environmental Factors: the "physical, social and attitudinal environment in which people live".[4]
- Personal Factors: the "particular background of an individual's life and living".[4]
You can learn more about the ICF components and ICF qualifiers here.
Case Study[edit | edit source]
Case study: A patient sustained a third degree burn injury to the hand causing damage to the integrity of the skin structure.[1]
Goal: To define ICF codes that correspond to this patient's injury for the purpose of assessment
Health condition (ICD-11): Burn injury to the hand
- ND95: Burn of wrist or hand
- ND95.3: Burn of wrist or hand, full thickness burn
Body structure codes (s codes) according to specificity :
- s810: structures of the area of skin
- s8102: skin of the upper extremity
Body functions (b codes) following the skin healing process:
- b810: protective functions of the skin may be impaired temporarily
- b820: functions of the skin for repairing breaks and other damage to the skin (from wound stage to scar formation)
- The body functions domain can include inclusion and exclusion criteria:
- Inclusion: function of scab formation, healing, scaring; bruising and keloid formation
- Exclusion: the skin's protective function and other skin functions
- The body functions domain can include inclusion and exclusion criteria:
Activities and Participation (d codes) can be restricted due to nerve damage or poor healing, which can affect long-term mobility and hand function, including:
- d445: hand and arm use
- d440: fine use of the hand
- d4401: use one or both hands to seize or hold something (example: grasping a tool or a door knob)
- d550: eating (example: "carrying out the coordinated tasks and actions of eating food that has been served, bringing it to the mouth and consuming it in culturally accepted ways, cutting or breaking food into pieces, opening bottles and cans, using eating implements, having meals, feasting, or dining")
- d750: limited or lack of informal social relationships, including meeting with a neighbour or participating in happy hour with co-workers due to cosmetic concerns and body image distress
- d845: inability to maintain a job due to anxiety and perceived stigma related to scarring in the hand area
Environment (e codes)
- e460: not comfortable going out shopping due to societal attitude towards visible scars, which causes anxiety
ICF Core Sets[edit | edit source]
ICF Core Sets (ICFCS) are a " selection of essential categories from the full ICF classification that are considered most relevant to describe the functioning of a person with a specific health condition or in a specific healthcare context"[5] Their purpose is to facilitate assessment in clinical practice and research.[6]
The ICF Core Sets are shortlisted from over 1400 ICF categories describing functioning, disability and health. They are developed for acute, early post-acute and long-term conditions. They are also categorised as neurological, musculoskeletal, cardiopulmonary conditions, spinal cord injury and vocational rehabilitation.[5] Each ICFCS has comprehensive and brief versions. The brief version of an ICFCS contains categories that describe functioning at its minimum standard.[5]
The process of ICF Core Set creation is complex and includes three phases:[5]
- Phase 1: Collecting evidence that contains an empirical multi-centre study, a systematic literature review, a qualitative study and an expert survey. Expert surveys capture the perspective of health professionals who work with patients with a specific health condition.[1]
- Phase 2: There is an international consensus conference where experts and health professionals look at the "candidate" ICF categories and decide which ICF categories should be included in the ICFCS.
- Phase 3: The ICFCS is implemented and introduced into practice.
Using the ICF Core Sets in clinical practice has several purposes, including:[7]
- To help with selecting an appropriate combination of outcome measures.
- To assist with selecting a tool in developing comprehensive outcome measures.
- To describe patterns of disability.
- To inform about the magnitude, the location and the nature of any functioning problem.
- To highlight the strengths and weaknesses of an individual patient.
- To describe changes in a patient’s functional profiles over time.
Clinical Forms[edit | edit source]
The development of clinical forms allows health professionals to focus on specific patient problems and "relate the disabilities to relevant and modifiable variables."[8] The following is the summary by Levesque and Thoomes of the advantages of using clinical forms in practice:[9]
- They encourage a biopsychosocial perspective.
- They allow the clinician to identify all factors within the ICF model.
- They direct the healthcare professional to use the most appropriate objective tests and outcome measures.
- They highlight contextual factors – personal and environmental which may affect prognosis and a patient's recovery
- They enable the clinician to identify factors which can be modifiable.
Rehabilitation Problem-Solving Form (RPS-Form)[edit | edit source]
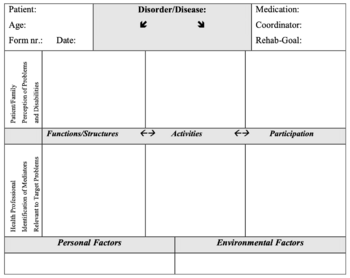
The Rehabilitation Problem-Solving Form (RPS-Form) facilitates the assessment of a patient by various health professionals as it addresses all components of human functioning, and environmental and personal factors. Additionally, the RPS-Form incorporates patients' perspectives and enhances their participation in the decision-making process of rehabilitation.[10] It is a tool in clinical practice,[8] which collects information from the ICF to enhance the patient-centred approach and the decision-making process. The RPS-Form contains areas designated for the ICF domains, categories, and codes.
This form can:[1]
- Help identify target problems and factors that contribute to these problems.
- Identify the most appropriate plan in terms of the treatments and interventions needed for a particular patient.
- Facilitate interprofessional communication.
- Help to provide information, including the views of the patient, professionals, clinicians.
- Help to improve communication between health professionals and their clients by recording their views.
You can find out more about the application of the RPS form for a specific condition here.
Physical Therapy Clinical Reasoning and Reflection Tool (PTCRT)[edit | edit source]
Clinical reasoning is a core skill needed for solving clinical problems and establishing rapport with patients. It allows healthcare providers, including physiotherapists, to integrate the patient's needs and experiences with their reasoning and decision-making in practice.[11]
The Physical Therapy Clinical Reasoning and Reflection Tool (PTCRT) uses the ICF framework to guide a physical therapist's practice and facilitate clinical reflection.[1] Achieving favourable outcomes in collaboration with the patient defines the success of the clinical reasoning process.[12] This form has designated areas which are aligned with ICF domains. This allows the clinician to record relevant categories and codes when working with a patient. The environmental section of this tool includes internal and external environmental factors which can become barriers and facilitators. The barriers are indicated by a minus sign and the facilitators by a positive sign.[1]
Sections of the Physical Therapy Clinical Reasoning and Reflection Tool (PTCRT) can be used to guide critical thinking, or the physiotherapist can complete the entire worksheet to "identify further potential inquiries to explore, either by a review of the evidence or by designing a new and important clinical question".[12]
You can find The Physical Therapy Clinical Reasoning and Reflection Tool (PT-CRT) here.
Cross-Walking of the ICF[edit | edit source]
Several clinical professional associations have integrated the ICF into their respective scope of practice.[1] But, perhaps more commonly in practice, there has been a "cross-walking" of the ICF to existing clinical instruments.[1] This enables ICF categories to be included in rehabilitation practice.
Cross-walking has specific linking rules developed by a group of individuals involved in the WHO development and maintenance activities.[1] The main rule is described in work by Cieza et al.[13] and states the following: "Before one links meaningful concepts to the ICF categories, one should have acquired a good knowledge of the conceptual and taxonomical fundaments of the ICF, as well as of the chapters, domains, and categories of the detailed classification, including definitions".[13]
It is worth noting that more work must be done to ensure the ICF is incorporated into practice. A study by Pongpipatpaiboon et al.[14] found that less than 50% of the ICF categories were present in the clinical assessment tools for individuals with a spinal cord injury.[14] This phenomenon was observed primarily in the acute and late long-term phases of spinal cord injury rehabilitation. Activities, participation, and environmental factors were the least covered in these phases. However, more ICF categories were included in the assessment after the patient's interview identified them.[14] The results of this study highlighted the underrepresentation of the environmental factors across the spinal cord injury continuum of care.[14]
Resources[edit | edit source]
- International Classification of Functioning, Disability and Health (ICF)
- A Tool for Clinical Reasoning and Reflection Using the International Classification of Functioning, Disability and Health (ICF) Framework and Patient Management Model
- Amatya B, Elmalik A, Song K, Lee SY, Galea MP, Khan F. Responsiveness of the International Classification of Functioning, Disability And Health (ICF) Clinical Functioning Information Tool (ClinFIT) in Routine Clinical Practice in an Australian Inpatient Rehabilitation Setting. J Rehabil Med. 2022 Apr 20;54:jrm00268.
References[edit | edit source]
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 Saleeby P. ICF and Application in Clinical Practice Course. Plus 2022
- ↑ Aims of the ICF. Available from https://www.icf-elearning.com/wp-content/uploads/ [last access 9.09.2022]
- ↑ Pasqualotto L, Lascioli A. ICF-based functional profile in education and rehabilitation: a multidisciplinary pilot experience. Journal of advanced health care, 2020; 2(1)
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 4.6 4.7 The ICF model. Available from https://www.icf-elearning.com/wp-content/uploads/articulate_uploads/ [last access 9.09.2022]
- ↑ 5.0 5.1 5.2 5.3 Selb M, Escorpizo R, Kostanjsek N, Stucki G, Üstün B, Cieza A. A guide on how to develop an International Classification of Functioning, Disability and Health Core Set. Eur J Phys Rehabil Med. 2015 Feb;51(1):105-17.
- ↑ Karlsson E, Gustafsson J. Validation of the international classification of functioning, disability and health (ICF) core sets from 2001 to 2019–a scoping review. Disability and rehabilitation. 2022 Jul 3;44(14):3736-48.
- ↑ Perin C, Bolis M, Limonta M, Meroni R, Ostasiewicz K, Cornaggia CM, Alouche SR, da Silva Matuti G, Cerri CG, Piscitelli D. Differences in rehabilitation needs after stroke: a similarity analysis on the ICF core set for stroke. International Journal of Environmental Research and Public Health. 2020 Jan;17(12):4291.
- ↑ 8.0 8.1 Steiner WA, Ryser L, Huber E, Uebelhart D, Aeschlimann A, Stucki G. Use of the ICF model as a clinical problem-solving tool in physical therapy and rehabilitation medicine. Phys Ther. 2002 Nov;82(11):1098-107.
- ↑ Levesque L,Thoomes E. Use of the RPS-Form as a Teaching Aid. Available from https://www.ifompt.org/site/ifompt/files/pdf/ [last access 10.09.2022]
- ↑ Eberhardt B, Greiner J. The clinical use of the RPS-Form is based on the ICF Model. Implementation of the RPS-Form in two centres in Indonesia and Nepal. 2008. Available from https://www.rehabnet.ch/files/categories/Downloads/Publikation_BEberhardt_Clinical_use_RPS_Form_Indonesia_Nepal_2008_RehabNET_EN.pdf [last access 11.09.2022]
- ↑ Abrandt Dahlgren M, Valeskog K, Johansson K, Edelbring S. Understanding clinical reasoning: A phenomenographic study with entry-level physiotherapy students. Physiotherapy Theory and Practice. 2021 Sep 23:1-0.
- ↑ 12.0 12.1 Atkinson HL, Nixon-Cave K. A tool for clinical reasoning and reflection using the international classification of functioning, disability and health (ICF) framework and patient management model. Phys Ther. 2011 Mar;91(3):416-30.
- ↑ 13.0 13.1 Cieza A, Geyh S, Chatterji S, Kostanjsek N, Ustün B, Stucki G. ICF linking rules: an update based on lessons learned. J Rehabil Med. 2005 Jul;37(4):212-8.
- ↑ 14.0 14.1 14.2 14.3 Pongpipatpaiboon K, Selb M, Kovindha A, Prodinger B. Toward a framework for developing an ICF-based documentation system in spinal cord injury-specific rehabilitation based on routine clinical practice: a case study approach. Spinal cord series and cases. 2020 May 5;6(1):1-9.