Clinical Reasoning
Original Editor - Rachael Lowe
Top Contributors - Admin, Kris Porter, Rachael Lowe, Olajumoke Ogunleye, Oyemi Sillo, Shreya Pavaskar, 127.0.0.1, WikiSysop, Uchechukwu Chukwuemeka, Claire Knott, Rucha Gadgil, Lucinda hampton, Mariam Hashem, Kim Jackson and Vidya Acharya -
Introduction[edit | edit source]
Clinical Reasoning is the process by which a therapist interacts with a patient, collecting information, generating and testing hypotheses, and determining optimal diagnosis and treatment based on the information obtained. It has been defined as “an inferential process used by practitioners to collect and evaluate data and to make judgments about the diagnosis and management of patient problems"[1]. This clinical reasoning process sensitizes healthcare professionals to make the best judgment under specific circumstances, in relation to the patient and context.[2]
Clinical reasoning is “the sum of the thinking and decision-making processes associated with clinical practice”[3][1]. During this process, the therapist analyses multiple variables contributing to the patient’s limited physical capacity (the ability to execute a task or action in a specific environment) and performance (what the patient can do in his or her own current environment). The key elements of the process include the generation of hypotheses of factors assumed to underlie the limitations of physical capacity and performance and the postulation of the magnitude of those factors. The therapist interacts with the patient and other persons involved in the patient's care (family, other health care professionals) and guides the patient in finding meaningful goals and health management strategies[4].
All decisions and actions need to be made in line with professional ethics and community expectations[4].
The below 7-minute video is a good introduction to clinical reasoning
Clinical Reasoning[edit | edit source]
Clinical Reasoning is integral to physiotherapy practice. As a concept, clinical reasoning is quite a simple one; however in practice, it is difficult and fraught with errors. The aim of clinical reasoning is to prevent misdirection [6] A robust clinical reasoning process is vital so the threshold of suspicion of serious pathology is at an appropriate level[7]. The way a therapist clinically reasons their findings can strongly influence how the case is interpreted. This has implications as to how the clinician views the red flags and gives weight to any red herrings presented therein [8]. It is done knowingly or unknowingly and is basically a cognitive process.
The most common form of clinical reasoning within the physiotherapy profession is hypothetico-deductive reasoning[9]. Within hypothetico-deductive reasoning, the clinician gains initial clues in regard to the patient's problem (from the subjective assessment), which forms the initial hypotheses in the therapist's mind. Further data is collected in the objective assessment, which may confirm or negate the hypotheses. Continual hypothesis generation may occur during management and reassessment[3]. Identification and prioritization of pertinent clinical data to either support or negate the hypotheses form the basis of clinical reasoning.[10]
Clinical reasoning consists of the following five dimensions:
• cognition
• a discipline-specific knowledge base
• metacognition, which means the individual’s awareness of his/her way of thinking
• the role of the patient in the decision-making process
• contextual interaction[1]
Reflection after the initial assessment and also after the subsequent sessions will help the therapist to recognise patterns and their clinical reasoning process will improve[6][7].
Process of Clinical Reasoning[edit | edit source]
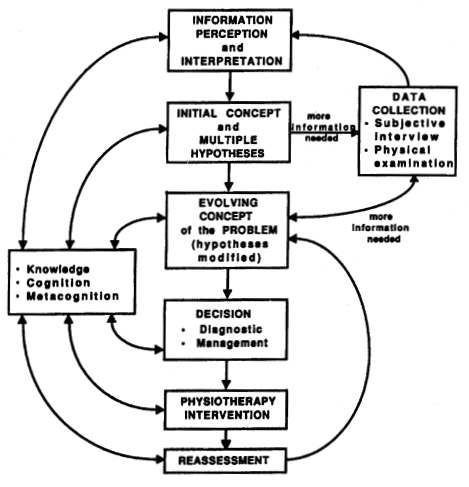
Clinical reasoning should begin as soon as the therapist meets the patient, as their behaviour can inform the therapist's clinical reasoning[7]. There should be ongoing data collection which should not stop at the end of the assessment to aid this process. A hypothetico-deductive model of clinical reasoning can be seen in Figure 1.
Figure 1: A Hypothetico-deductive model of Clinical Reasoning[6]
The therapist may be able to ascertain quickly that something is wrong with the patient due to the subjective and objective assessment along wither their subsequent clinical reasoning. The data gathered over sessions should be collated to best inform the therapist. This will contribute to the therapist's evolving concept of the patient's problem[7][6]. The decision made at each step will influence the decision at the next step.
Another model used for clinical reasoning is the Dual process theory, i.e., the ability to balance intuition and analytical reasoning for a particular situation.[11]It uses the concepts of deduction, induction and abduction for coming to a conclusion; however, developing this type of decision-making requires significant experience and exposure.[11]
Pattern Recognition[edit | edit source]
Pattern recognition is an important part of clinical reasoning however, this will be limited in students and newly qualified physiotherapists[6][9].
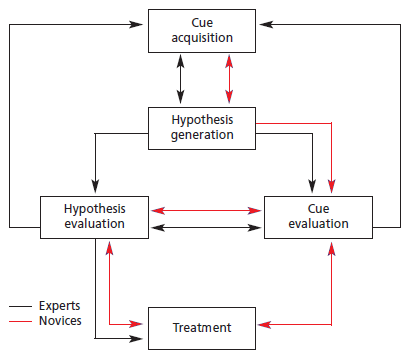
Knowledge is also an important consideration. The newly qualified therapist is expected to have many more potential hypotheses in comparison to an experienced therapist[6]. There are suggested to be differences between novice and expert therapists in the process of clinical reasoning[9]. Although broadly similar, novice physiotherapists have to go through a long process of clinical reasoning compared to expert therapists due to a lack of knowledge comparison and less experience in pattern recognition. Figure 2 demonstrates the clinical reasoning process of expert therapists (with at least 3 years of experience) and novice therapists (with under three years of experience or students)[9].
Figure 2: Difference in clinical reasoning between expert and novice therapists[9].
Problem solving[edit | edit source]
This approach is a content-specific process requiring rules and knowledge related to the text and context. The types vary according to different clinical cases or problems. It involves comparing, testing and analysing the case to determine what will be next in protocol and this keeps on going in a cycle till a desired result is achieved.
Patient Involvement in the Clinical Reasoning Process[edit | edit source]
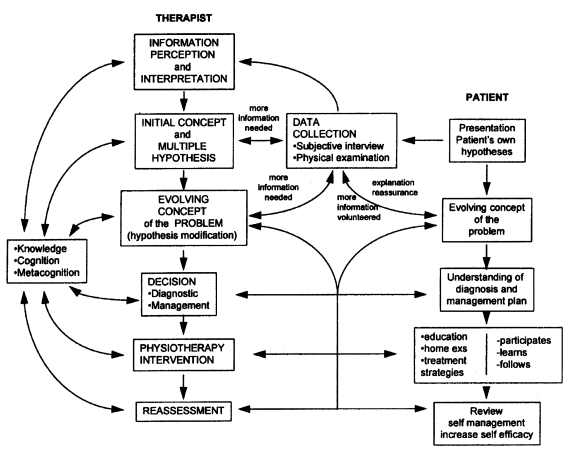
The patient should be an integral part of the clinical reasoning process, as this can help the clinician to form hypotheses and lead towards the review of the outcome post physiotherapy intervention[6](See Figure 3).
Figure 3: Patient involvement in the clinical reasoning process[6].
Despite the desire of the physiotherapist to find logical connections between signs and symptoms that lead to specific functional diagnoses, this is not always readily achieved. In such instances, failure to get the pieces that will solve the puzzle may prove troubling and discomforting. But clear answers and ready explanations will not often be at hand, and becoming comfortable in the grey areas of clinical practice may be a prerequisite for compassionate and pathic practice in physiotherapy[12].
Approaches[edit | edit source]
Hypothesis-Oriented Algorithm for Clinicians II (HOAC II)
International Classification of Functioning, Disability and Health (ICF)
Resources[edit | edit source]
Physical Therapy Clinical Reasoning and Reflection Tool - aims to integrate the ICF framework into the patient management model while incorporating the hypothesis-driven basis of CDM models
getPTsmart - Tool to engage in the teaching and learning of clinical reasoning in a contemporary, time-independent environment that serves as a link between the classroom and clinical practice.
References[edit | edit source]
- ↑ 1.0 1.1 1.2 Higgs J, Jones M. Clinical decision making and multiple problem spaces. In: Higgs J, Jones MA, Loftus S, Christensen N. Clinical reasoning in health professions. Amsterdam: Elsevier;2008. p. 4-19.
- ↑ Gummesson C, Sundén A, Fex A. Clinical reasoning as a conceptual framework for interprofessional learning: a literature review and a case study. Physical Therapy Reviews. 2018 Jan 2;23(1):29-34.
- ↑ 3.0 3.1 Edwards I, Jones M, Carr J, Braunack-Mayer A, Jensen GM. Clinical reasoning strategies in physical therapy. Physical therapy. 2004;84(4):312-30.
- ↑ 4.0 4.1 Atkinson HL, Nixon-Cave K. A tool for clinical reasoning and reflection using the International Classification of Functioning, Disability and Health (ICF) framework and patient management model. Physical therapy. 2011;91(3):416-30.
- ↑ Rahul Patwari Clinical reasoning Available from:https://www.youtube.com/watch?v=6DzeF8hCNb8&app=desktop (last accessed 3.3.2020)
- ↑ 6.0 6.1 6.2 6.3 6.4 6.5 6.6 6.7 Jones, M. Clinical reasoning and pain. Manual Therapy. 1995; 1:17-24.
- ↑ 7.0 7.1 7.2 7.3 Greenhalgh, S. Red Flags, and clinical Presentation Mapping. Available from: https://macpweb.org/home/index.php?m=file&f=873. (accessed 21 October 2008)
- ↑ Greenhalgh, S. and Selfe, J. Margaret: a tragic case of spinal Red Flags and Red Herrings. Physiotherapy. 2004; 90:73-76.
- ↑ 9.0 9.1 9.2 9.3 9.4 Doody C, McAteer M. Clinical reasoning of expert and novice physiotherapists in an outpatient orthopaedic setting. Physiotherapy. 2002;88 (5): 258-268.
- ↑ Richards JB, Hayes MM, Schwartzstein RM. Teaching clinical reasoning and critical thinking: from cognitive theory to practical application. Chest. 2020 Oct 1;158(4):1617-28.
- ↑ 11.0 11.1 Croskerry, P. (2015). Clinical Decision Making. In: Barach, P., Jacobs, J., Lipshultz, S., Laussen, P. (eds) Pediatric and Congenital Cardiac Care. Springer, London. https://doi.org/10.1007/978-1-4471-6566-8_33
- ↑ Chowdhury A, Bjorbækmo WS. Clinical reasoning—embodied meaning-making in physiotherapy. Physiotherapy Theory and Practice. 2017 Jul 3;33(7):550-9.