How to Write a Case Study
Original Editor - Mariam Hashem
Top Contributors - Mariam Hashem, Kim Jackson and Admin
Introduction[edit | edit source]
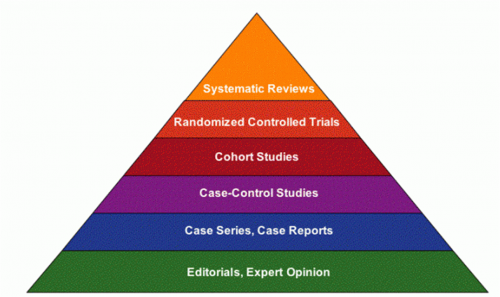
In evidence-based hierarchy, case studies come in the in the fifth level. Although they cannot be considered as guidelines, case studies are powerful material to share clinical experience and knowledge. You could write a case study to represent a typical or an unusual case presentation and share your successful program with your colleagues.
There are general guidelines for case studies but if you are writing for publication you have to be aware of the journal's specific requirements. If you're writing a case study as part of Plus program assignment the following instructions will take you a step by step into the writing process.
The Anatomy of a case study article[edit | edit source]
- Title
- Abstract
- Introduction
- Client Characteristics
- Examination Findings
- Clinical Hypothesis
- Intervention
- Outcome
- Discussion
- References
Instructions[edit | edit source]
A case study should be limited to clinical relevant information. In order to eliminate unnecessary details begin by asking yourself a set of questions: what is my purpose of writing this article? what is my message? Then gather all needed information and search similar cases in literature to make relations. Try to keep interpretations on the development of the pathology and disease development as simple as possible and keep your article limited to proven facts[1].
Throughout the whole writing process, you should support your case with evidence by citing information properly.
Title[edit | edit source]
Expressive and concise titles attract readers. Highlight the most essential keywords in your topic.
You may chose either of these suggested formulas:
'' A case study of cervicogenic headache responding to mobilisation with movement technique'' or ''Mobilisation with movement technique in cervicogenic headache: a case study''
Example of an expressive title:
| Case study of a transfemoral amputee semi-professional cyclist |
Abstract[edit | edit source]
A narrative abstract includes a summary of the purpose, case presentation, intervention and outcomes.
Write your abstract after finishing the article.
Example:
| This case presentation is a semi-professional cyclist who incurred a transfemoral amputation as a result of a road traffic accident. The case study documents from initial assessment until discharge and highlights the main problems encountered by the patient, the goals, the rehabilitation programme and the outcome. |
Introduction[edit | edit source]
In the introduction, you give your readers an idea on the background of the case. Then discuss relevant cases and similar literature briefly. However, the most important aim of the introduction is driving your readers' attention to the purpose of your report. They should have a clear vision of your objectives.
If there is anything interesting or challenging you met when diagnosing or managing this case, it's worth mentioning in the introduction.
Client Characteristics[edit | edit source]
Here is where you mention the demographic data, nature of the condition and answer this question: why the patient sought your help? Try to use the patient's own words in describing the chief complaint.
History-taking usually gives us lots of information but in client characteristics it's better to eliminate non relevant data. Inform your readers about the information that guided your diagnosis and directed your hypothesis.
Example:
| The patient is a 24 year old man who was previously very fit and well with no medical history. He was a semi-professional cyclist who also worked in a very physical job in a bicycle shop. Previously he would train for many months training for the race season and cycling was the centre of his life. He was knocked off his bike whilst cycling by a truck driver who was drunk. He incurred an emergency transfemoral amputation three weeks prior to the initial assessment with the author. |
Examination Findings[edit | edit source]
What tests have you utilised to guide your decision and reach your final diagnosis? What results have you obtained from your examination? Were there any related observations?
Give details on the tests and examination you have used and make sure they are valid and cited. You may want to describe the test application and response. Again, restrict yourself to relevant information and eliminate unnecessary details.
If you are writing your case study on Physiopedia, you may want to link the test to a relevant page or add a video or an image of the test. If you are using an image for your patient(s), please respect their privacy and make sure to ask for permission before publishing.
Example:
| On examination, subjectively he spoke about the pain that he was experiencing. He explained the pain as shooting pain into the absent limb 7/10 on the VAS scale. This was intermittent pain during sleep and was affecting his rehabilitation and use of prosthesis. It also became apparent that he was working through the grieving process recognized as; denial, anger, bargaining, depression, and acceptance[1].He was very angry that the truck driver that had caused the accident had been drunk and he felt like his life would never be the same again.
He had been a highly functioning young man previously, a semi professional cyclist and worked in a bike shop which was a very physically demanding job. His main objective was to return to the life he had.He was managing to independently clean, toilet and dress himself and was ambulating using crutches. He was not having any problems with transfers. Objectively, his transfemoral stump and wound were in good condition. He had no contractures and he had full range of movement at the hip and trunk. He had reduced strength of the hip, especially extension, adduction and internal rotation. His core muscles were weak and bridging was difficult. His sitting balance was very good, as were his pelvic movements but his standing balance was poor. He was able to transfer his weight side to side and forwards and backwards. His gait was very asymmetrical, with poor hip extension, hip hitching and trunk side flexion. |
Clinical Hypothesis/Impression[edit | edit source]
From your findings on the physical examination, what decision have you reached? What helped you in clinical reasoning?
Remember, your hypothesis should be supported with evidence.
Example:
| A major problem that the patient faced during rehabilitation was phantom limb pain, a neuropathic pain perceived by the region of the body that is no longer present[2]. This was affecting his sleep and his rehabilitation programme and having negative psychological effects, adding to already altered psychological state as he was working through the grieving process[1]. The pain he described as tingling, cramping and shooting pains in the portion of the limb that was removed. He found this pain, not only disabling but also unnerving, as he could not understand why he would continue to get pain where he no longer had a limb. |
Intervention[edit | edit source]
Mention your treatment goals and discuss your management program. Name your techniques, describe them in details and make sure to cite them properly. If you had to apply certain modifications to your treatment, write about them.
Example:
| It was important to work with the consultant to prescribe the relevant medication to initially ease the symptoms but there were also other approaches that could help. It was important for the patient to understand that this pain was real and he was not imagining it. It was explained to him that although the limb is no longer there, the nerve endings at the site of the amputation continue to send pain signals to the brain that make the brain think the limb is still there.
A TENS machine was initially used to try to ease the pain. It was also important to massage the stump, continue the rehabilitation programme and to wear an elastic stump sock to minimize the volume changes. It has also been shown that there is a significant reduction in the intensity of phantom limb pain using mental imagery[3] and mirror therapy can help to resolve the visual-proprioceptive disassociation in the brain[2]. Therefore mirror therapy was also initiated with graded motor imagery. This is where the patient views a reflection of the intact limb through a mirror positioned where the amputated limb would have been. Gradually, movements of the intact leg were introduced. |
Outcome[edit | edit source]
Report the degree of response and the tools/methods you've used to measure improvement or worsening. Also, here you tell your readers about your discharge plan or referrals to another healthcare specialist.
Example:
| The anti-neuropathic medication, amitriptyline, and TENS reduced the patient’s symptoms initially but the pain continued to impair function of the limb when doing exercises and gait re-education and was still affecting his sleep. The patient felt more in control of his pain, once he understood why it was occurring. When the patient started massaging the stump he felt that the pain diminished more but did not stay away.
It was the mirror therapy that seemed to have the greatest effect. As the patient used the mirror therapy more and gradually introduced movements of the intact limb, he felt a decrease in the amount of pain he was experiencing. After a while, he was able to visualize the limb without the mirror, which he could do more regularly. The pain went from a 7/10 on the Visual Analogue Scale to 2/10 and it no longer disturbed the patient's sleep. |
Discussion[edit | edit source]
In the discussion, you summarise the whole experience and share you you have learnt.
Discuss your hypothesis and support your theories with evidence. However, it's better to keep it simple and concise with regards to theoretical aspects.
Example:
| There are many cases, such as this, with previously healthy and very fit amputees who have suffered traumatic amputation and wish to return to high level competitive sports, especially since the increase of war conflicts in the past twenty years, considering there were 1,221 US Service members who sustained an amputation from 2001-2011[4].
It is therefore imperative that, as physiotherapists, we strive to rehabilitate all patients to the best of their ability. It is so important to have shared, realistic goals with the patient and to be aware not only of the physical issues, but also social, emotional, psychological and economic problems that they will encounter on the way[5]. It is imperative that at each step of rehabilitation the patient remains at the centre of the inter-disciplinary team. The rehabilitation is an ever-evolving situation with constantly revised training programmes and communication and education is key. |
References[edit | edit source]
Your writing should end with a reference list. Only include references that you have used in your case.
Resources[edit | edit source]
See the Physiopedia case studies category:
See these examples of case studies in Physiopedia:
- Case study of a transfemoral amputee semi-professional cyclist: Amputatee Case Study
- Management of Neck Pain: a case study
- Merging stratification approaches in physical therapy management of a case of subacute low back pain
- Amputation secondary to Diabetes Mellitus: Amputee Case Study
- Manual Therapy and Exercise Intervention in the Treatment of Shoulder and Neck Pain in a Patient with Mental Health Comorbidities: A Case Report
- Effectiveness of thoracic manipulations on shoulder pain: A Case Report
References[edit | edit source]
- ↑ Budgell B. Guidelines to the writing of case studies. The Journal of the Canadian Chiropractic Association. 2008 Dec;52(4):199.